
UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
Washington, D.C. 20549
FORM 10-K
(Mark One)
☒ ANNUAL REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934
For the fiscal year ended December 31, 2020
OR
☐ TRANSITION REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934
Lantern Pharma Inc.
(Exact name of registrant as specified in its charter)
| Delaware | 001-39318 | 46-3973463 | ||
| (State or Other Jurisdiction of Incorporation) |
(Commission File Number) |
(IRS Employer Identification No.) |
| 1920
McKinney Avenue, 7th Floor Dallas, Texas |
75201 | |
| (Address of Principal Executive Offices) | (Zip Code) |
(972) 277-1136
(Registrant’s telephone number, including area code)
Securities registered pursuant to Section 12(b) of the Act: Common Stock
| Title of each class | Trading Symbol | Name of each exchange on which registered | ||
| Common Stock, $0.0001 par value | LTRN | The Nasdaq Stock Market |
Indicate by check mark if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes ☐ No ☑
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or Section 15(d) of the Act. Yes ☐ No ☑
Indicate by check mark whether the registrant (1) has filed all reports required to be filed by Section 13 or 15(d) of the Securities Exchange Act of 1934 during the preceding 12 months (or for such shorter period that the registrant was required to file such reports), and (2) has been subject to such filing requirements for the past 90 days. Yes ☑ No ☐
Indicate by check mark whether the registrant has submitted electronically every Interactive Data File required to be submitted pursuant to Rule 405 of Regulation S-T (§232.405 of this chapter) during the preceding 12 months (or for such shorter period that the registrant was required to submit such files). Yes ☑ No ☐
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, a non-accelerated filer, a smaller reporting company, or an emerging growth company. See the definitions of “large accelerated filer,” “accelerated filer,” “smaller reporting company,” and “emerging growth company” in Rule 12b-2 of the Exchange Act.
| Large accelerated filer | ☐ | Accelerated filer | ☐ |
| Non-accelerated filer | ☑ | Smaller reporting company | ☑ |
| Emerging growth company | ☑ |
If an emerging growth company, indicate by check mark if the registrant has elected not to use the extended transition period for complying with any new or revised financial accounting standards provided pursuant to Section 13(a) of the Exchange Act. ☐
Indicate by check mark whether the registrant has filed a report on and attestation to its management’s assessment of the effectiveness of its internal control over financial reporting under Section 404(b) of the Sarbanes-Oxley Act (15 U.S.C. 7262(b)) by the registered public accounting firm that prepared or issued its audit report. ☐
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Exchange Act). Yes ☐ No ☑
State the aggregate market value of the voting and non-voting common equity held by non-affiliates computed by reference to the price at which the common equity was last sold, or the average bid and asked price of such common equity, as of the last business day of the registrant’s most recently completed second fiscal quarter: $34,733,370.
As of March 8, 2021, the registrant had 11,169,665 shares of common stock, $0.0001 par value per share outstanding.
DOCUMENTS INCORPORATED BY REFERENCE
Portions of the registrant’s definitive proxy statement for the registrant’s 2021 Annual Meeting of Stockholders to be filed pursuant to Regulation 14A within 120 days of the registrant’s year ended December 31, 2020 are incorporated herein by reference into Part III of this Annual Report on Form 10-K.
Table of Contents
i
SPECIAL NOTE CONCERNING FORWARD-LOOKING STATEMENTS AND RISK FACTORS
This Annual Report on Form 10-K contains forward-looking statements that involve substantial risks and uncertainties. We make such forward-looking statements pursuant to the safe harbor provisions of the U.S. Private Securities Litigation Reform Act, Section 21E of the Securities Exchange Act of 1934, as amended, and other federal securities laws. All statements, other than statements of historical fact, contained in this Annual Report on Form 10-K, including statements regarding our strategy, future preclinical studies and clinical trials, future financial position, projected costs, prospects, plans and objectives of management, are forward-looking statements. The words “anticipate,” “believe,” “contemplate,” “could,” “estimate,” “expect,” “intend,” “seek,” “may,” “might,” “plan,” “potential,” “predict,” “project,” “target,” “aim,” “should,” ‘will” “would,” or the negative of these words or other similar expressions are intended to identify forward-looking statements, although not all forward-looking statements contain these words. Forward-looking statements reflect our current views with respect to future events and are based on assumptions and subject to risks and uncertainties.
The forward-looking statements in this Annual Report on Form 10-K include, among other things, statements relating to:
| ● | the potential advantages of our RADR® platform in identifying drug candidates and patient populations that are likely to respond to a drug candidate; |
| ● | our strategic plans to advance the development of any of our drug candidates; |
| ● | our strategic plans to expand the number of data points that our RADR® platform can access and analyze; |
| ● | our research and development efforts of our internal drug discovery programs and the utilization of our RADR® platform to streamline the drug development process; |
| ● | the initiation, timing, progress, and results of our preclinical studies or clinical trials on any of our drug candidates; |
| ● | our intention to leverage artificial intelligence, machine learning and genomic data to streamline the drug development process and to identify patient populations that would likely respond to a drug candidate; |
| ● | our plans to discover and develop drug candidates and to maximize their commercial potential by advancing such drug candidates ourselves or in collaboration with others; |
| ● | our expectations regarding our ability to fund our operating expenses and capital expenditure requirements with our existing cash and cash equivalents; |
| ● | our ability to secure sufficient funding and alternative source of funding to support our existing and proposed preclinical studies and clinical trials; |
| ● | our estimates regarding the potential market opportunity for our drug candidates we or any of our collaborators may in the future develop; |
| ● | our anticipated growth strategies and our ability to manage the expansion of our business operations effectively; |
| ● | our expectations related to future expenses and expenditures; |
| ● | our ability to keep up with rapidly changing technologies and evolving industry standards, including our ability to achieve technological advances; |
| ● | the potential impact that COVID-19 may have on our business plans; |
ii
| ● | our ability to source our needs for skilled labor in the fields of artificial intelligence, genomics, biology, oncology and drug development; and |
| ● | the impact of government laws and regulations on the development and commercialization of our drug candidates. |
We may not actually achieve the plans, intentions, or expectations disclosed in our forward-looking statements, and you should not place undue reliance on our forward-looking statements. Actual results or events could differ materially from the plans, intentions, and expectations disclosed in the forward-looking statements we make. Factors that may cause actual results or events to differ materially from current plans, intentions, and expectations include, among other things:
| ● | We have a limited operating history and have never generated any revenues other than from a prior research grant, which may make it difficult to evaluate the success of our business to date and to assess our future viability; |
| ● | We have incurred significant operating losses since inception and anticipate that we will continue to incur substantial operating losses for the foreseeable future and may never achieve or maintain profitability; |
| ● | We will need substantial additional funding, and if we are unable to raise capital when needed, we could be forced to delay, reduce or eliminate our drug development programs or commercialization efforts; |
| ● | Our RADR® platform may fail to help us discover and develop additional potential drug candidates; |
| ● | We have limited experience in drug discovery and drug development and may not receive regulatory approval to market our drug candidates; |
| ● | Even if we are successful in completing all preclinical studies and clinical trials, we may not be successful in commercializing one or more of our drug candidates; and |
| ● | Those other risk factors listed under Part I, Item 1A. “Risk Factors,” Part II, Item 7. “Management’s Discussion and Analysis of Financial Condition and Results of Operations” and elsewhere in this Annual Report on Form 10-K. |
These factors could cause actual results or events to differ materially from the forward-statements that we make. Furthermore, we operate in a competitive and rapidly changing environment. New risks and uncertainties emerge from time to time, and it is not possible for us to predict all risks and uncertainties that could have an impact on the forward-looking statements contained in this Annual Report on Form 10-K.
You should read this Annual Report on Form 10-K and the documents that we file with the Securities and Exchange Commission, or the SEC, with the understanding that our actual future results may be materially different from what we expect. These forward-looking statements are based on management’s current expectations. These statements are neither promises nor guarantees, but involve known and unknown risks, uncertainties and other important factors that may cause our actual results, performance or achievements to be materially different from any future results, performance or achievements expressed or implied by the forward-looking statements. Factors that may cause actual results or events to differ materially from current plans, intentions, and expectations include, among other things, those listed under Part I, Item 1A. “Risk Factors,” Part II, Item 7. “Management’s Discussion and Analysis of Financial Condition and Results of Operations” and elsewhere in this Annual Report on Form 10-K. Given these uncertainties, you should not rely on these forward-looking statements as predictions of future events. The forward-looking statements contained in this Annual Report on Form 10-K are made as of the date of this Annual Report on Form 10-K, and we do not assume any obligation to update any forward-looking statements, whether as a result of new information, future events or otherwise, except as required by applicable law.
In addition, statements that “we believe” and similar statements reflect our beliefs and opinions on the relevant subject. These statements are based upon information available to us as of the date of this Annual Report on Form 10-K, and while we believe such information forms a reasonable basis for such statements, such information may be limited or incomplete. Our statements should not be read to indicate that we have conducted an exhaustive inquiry into, or review of, all potentially available relevant information. These statements are inherently uncertain and investors are cautioned not to unduly rely upon these statements.
Unless the context requires otherwise, references to the “Company,” “Lantern,” “we,” “us,” and “our” in this Annual Report on Form 10-K refer to Lantern Pharma Inc., a Delaware corporation, and, where appropriate, its wholly-owned subsidiary.
iii
Overview
We are a clinical stage biotechnology company, focused on leveraging artificial intelligence (“A.I.”), machine learning and genomic data to streamline the drug development process and to identify the patients that will benefit from our targeted oncology therapies. Our portfolio of therapies consists of small molecules that others have tried, but failed, to develop into an approved commercialized drug, as well as new compounds that we are developing with the assistance of our proprietary A.I. platform and our biomarker driven approach. Our A.I. platform, known as RADR®, currently includes more than 1.2 billion data points, and uses big data analytics (combining molecular data, drug efficacy data, data from historical studies, data from scientific literature, phenotypic data from trials and publications, and mechanistic pathway data) and machine learning to rapidly uncover biologically relevant genomic signatures correlated to drug response, and then identify the cancer patients that we believe may benefit most from our compounds. This data-driven, genomically-targeted and biomarker-driven approach allows us to pursue a transformational drug development strategy that identifies, rescues or develops, and advances potential small molecule drug candidates at what we believe is a fraction of the time and cost associated with traditional cancer drug development.
Our strategy is to both develop new drug candidates using our RADR® platform and other machine learning driven methodologies, and to pursue the development of drug candidates that have undergone previous clinical trial testing or that may have been halted in development or deprioritized because of insufficient clinical trial efficacy (i.e., a meaningful treatment benefit relevant for the disease or condition under study as measured against the comparator treatment used in the relevant clinical testing) or for strategic reasons by the owner or development team responsible for the compound. Importantly, these historical drug candidates appear to have been well-tolerated in many instances, and often have considerable data from previous toxicity, tolerability and ADME (absorption, distribution, metabolism, and excretion) studies that have been completed. Additionally, these drug candidates may also have a body of existing data supporting the potential mechanism(s) by which they achieve their intended biologic effect, but often require more targeted trials in a stratified group of patients to demonstrate statistically meaningful results. Our dual approach to both develop de-novo, biomarker-guided drug candidates and “rescue” historical drug candidates by leveraging A.I., recent advances in genomics, computational biology and cloud computing is emblematic of a new era in drug development that is being driven by data-intensive approaches meant to de-risk development and accelerate the clinical trial process. In this context, we intend to create a diverse portfolio of oncology drug candidates for further development towards regulatory and marketing approval with the objective of establishing a leading A.I.-driven, methodology for treating the right patient with the right oncology therapy.
A key component of our strategy is to target specific cancer patient populations and treatment indications identified by leveraging our RADR® platform, a proprietary A.I. enabled engine created and owned by us. We believe the combination of our therapeutic area expertise, our A.I. expertise, and our ability to identify and develop promising drug candidates through our collaborative relationships with research institutions in selected areas of oncology gives us a significant competitive advantage. Our RADR® platform was developed and refined over the last four years and integrates millions of data points immediately relevant for oncology drug development and patient response prediction using artificial intelligence and proprietary machine learning algorithms. By identifying clinical candidates, together with relevant genomic and phenotypic data, we believe our approach will help us design more efficient preclinical studies, and more targeted clinical trials, thereby accelerating our drug candidates’ time to approval and eventually to market. Although we have not yet applied for or received regulatory or marketing approval for any of our drug candidates, we believe our RADR® platform has the ability to reduce the cost and time to bring drug candidates to specifically targeted patient groups. We believe we have developed a sustainable and scalable biopharma business model by combining a unique, oncology-focused big-data platform that leverages artificial intelligence along with active clinical and preclinical programs that are being advanced in targeted cancer therapeutic areas to address today’s treatment needs.
1
Scientific literature offers a definition for “drug rescue” as research involving abandoned small molecules and biologics that have not been approved by the U.S. Food and Drug Administration (“FDA”). These rescued molecular compounds are often abandoned by pharmaceutical companies in the drug discovery or preclinical testing phase, typically because they do not prove effective for the specific use for which they were developed. Some of these compounds may be useful in treating other diseases for which they have not been tested. See, Hemphill, Thomas A., “The NIH Promotes Drug Repurposing and Rescue,” Research Technology Management, v. 5, no. 5, pp. 6-8 (2012). Our use of the term “rescue”, “drug rescue”, or “drug rescuing” refers to, “…a system of developing new uses for chemical and biological entities that previously were investigated in clinical studies but not further developed or submitted for regulatory approval, or had to be removed from the market for safety reasons.”, which is a definition we believe is recognized in the drug discovery, drug development and pharmaceutical and biotechnology industries. See, Naylor, S. and Schonfeld J., “Therapeutic Drug Repurposing, Repositioning and Rescue,” DDW (Drug Discovery World) Winter 2014, and Mucke, HAM, A New Journal for the Drug Repurposing Community. Drug Repurposing, Rescue & Repositioning 1, 3-4 (2014). The use of the term “drug rescue,” “rescuing,” or words of similar meaning in this report should not be construed to mean that our RADR® platform has resolved all issues of safety and/or efficacy for any of our drug candidates. Issues of safety and efficacy for any drug candidate may only be determined by the U.S. FDA or other applicable regulatory authorities in jurisdictions outside the United States.
Our current portfolio consists of four compounds in active development: two drug candidates in clinical phases, one in preclinical studies, and one in research optimization. All of these drug candidates are leveraging precision oncology, A.I. and genomic driven approaches to accelerate and direct development efforts. We currently have two drug candidates in clinical development, LP-100 and LP-300, where we are leveraging data from prior preclinical studies and clinical trials, along with insights generated from our A.I. platform, to target the types of tumors and patient groups that would be most responsive to the drug. Both LP-100 and LP-300 showed promise in important patient subgroups, but failed pivotal Phase III trials when the overall results did not meet the predefined clinical endpoints. We believe that this was due to a lack of biomarker-driven patient stratification. Additionally, we have one new drug candidate, LP-184, in preclinical development for two potentially distinct indications where we are leveraging machine learning and genomic data to streamline the drug development process and to identify the patients and cancer subtypes that will best benefit from the drug, if approved. As part of our antibody drug conjugate (ADC) program commenced in early 2021, we have initiated the optimization and evaluation of an antibody drug conjugate aimed at leveraging our LP-184 molecule in combination with an antibody for select solid tumors.
Our development strategy is to pursue an increasing number of oncology focused, molecularly targeted therapies where artificial intelligence and genomic data can help us provide biological insights, reduce the risk associated with development efforts and help clarify potential patient response. We plan on strategically evaluating these on a program-by-program basis as they advance into clinical development, either to be done entirely by us or with out-licensing partners to maximize the commercial opportunity and reduce the time it takes to bring the right drug to the right patient.
We have out-licensed our drug-candidate LP-100 to Allarity Therapeutics A/S (“Allarity Therapeutics”), a European biotechnology company. LP-100 is in a Phase II clinical trial in metastatic, castration-resistant, prostate cancer (mCRPC) that is managed by Allarity Therapeutics. Our second clinical-stage drug candidate in the rescue process is LP-300. LP-300 is a small molecule with cysteine modifying activity on select proteins, which has an existing investigational new drug application (“IND”). We are in the process of initiating discussions with the U.S. FDA to launch a future phase II clinical trial for LP-300 with a stratified patient population of approximately 40 to 75 patients. Our new drug candidate, LP-184, is in a preclinical translational ex vivo study using fresh human biopsies. LP-184 is a next generation alkylating agent with nanomolar potency that preferentially damages DNA in cancer cells that overexpress certain biomarkers. LP-184 is in the fulvene class of compounds and has shown preliminary preclinical indications of lower toxicity, longer half-life, and increased antitumor activity as compared to other compounds in this drug class. Subject to regulatory clearance to move forward under a future IND application, we are planning a Phase I clinical trial for LP-184 across multiple solid tumors that express a certain biomarker profile, and in glioblastoma to begin in late 2021 or early 2022. Our antibody drug conjugate (ADC) program is in early stage development and compound optimization for solid tumors.
LP-100 (Irofulven) is showing promise in solid tumors, primarily prostate cancer, where it is being advanced in an out-licensing transaction with Allarity Therapeutics, after being in-licensed and developed by us. LP-100 has been well-tolerated, based on initial observations from a phase II clinical trial in Europe in mCRPC. Continuing enrollment for this Phase II clinical trial has slowed during the COVID-19 pandemic. Allarity Therapeutics has also stated that it is focusing its existing resources on other programs that are currently higher priority for Allarity than LP-100. As of the date of this report, we are unable to forecast the timeline for the completion of the Phase II clinical trial. Recently published data (also supported by prior publications on Irofulven) indicates that tumors carrying mutations in ERCC2 and ERCC3 genes are likely to be sensitive to LP-100, and that the drug will be synthetically lethal in these tumors, in a fashion similar to the activity of PARP inhibitors in BRCA deficient tumors. These observations expand the potential treatment indications for LP-100 to include urothelial tumors, including bladder cancers, since as many as 10% of bladder cancers carry ERCC2/ERCC3 mutations. These indications may represent a more rapid and efficient path to potential approval of LP-100, and we are evaluating possibilities aimed at maximizing the value of these additional observations.
2
Most patients with metastatic prostate cancer present with localized cancer, for which the standard of care may include active observation, radiation, surgery, and androgen deprivation/suppression therapy. Responses to such therapy can be transient and many patients will develop a castration resistant prostate cancer (CRPC) and develop, or are at risk to develop, mCRPC which accumulates genomic alterations including DNA repair deficits. Chemotherapeutic agents play a critical role in the management of both metastatic castration sensitive and mCRPC. The frequent use of the chemotherapy drug docetaxel in treating metastatic androgen sensitive prostate cancers exemplifies this role. Historical observations of potential anticancer activity of LP-100 in clinical studies with prostate cancer, and evidence of sensitivity to LP-184 in prostate cancer cell lines along with the development of computational methods that integrate gene expression signatures, support LP-184 as a drug candidate with potential for use in combination with androgen deprivation therapy for metastatic prostate cancer that is castration sensitive as well as metastatic prostate cancer that is castration resistant.
LP-184 is a new small molecule drug candidate that in preliminary preclinical studies has demonstrated increased plasma stability, reduced total body clearance, significantly longer half-life, and potentially greater tumor regression than other studied fulvene based compounds. We estimate that a substantial number of patients each year who suffer from metastatic prostate cancer globally could be eligible for potential treatment with LP-184, if approved. In addition, the observed nanomolar potency of LP-184 suggests that it may have anticancer properties in a wide range of solid tumors as an alkylating agent that works by causing DNA damage in tumor cells. Other indications for LP-184 in solid tumors are emerging as a result of early developmental and biomarker studies, including ovarian, breast, liver, kidney, pancreatic and thyroid cancers, as well as certain glioblastomas.
| ● | Based on increased sensitivity in cell-lines and PDx models exhibiting DNA repair deficient genetic backgrounds, we believe that LP-184 could have potential for targeted treatment of DNA repair deficient hereditary breast and ovarian cancers, from which more than 2.3 million patients suffer globally according to the Global Cancer Observatory. |
| ● | Based on recent observations, we also believe that LP-184 could have potential as treatment (alone or in combination with other treatments) for glioblastoma, which is an aggressive type of cancer that accounts for more than half of all primary brain tumors. The American Association of Neurological Surgeons estimates that glioblastoma has an incidence of two to three per 100,000 adults per year and accounts for about 17% of all tumors of the brain (primary and metastatic). |
| ● | Our A.I. platform RADR® helped uncover genomic biomarkers that we believe indicate certain patients could be more responsive to therapy with LP-184. |
Further work on these biomarkers both in-silico and in preclinical studies will help to establish a genomic signature that may accelerate our time to a clinical trial and help guide patient selection. We believe that the market for LP-184 as a molecularly-targeted drug candidate could be significant.
LP-300 (disodium 2,2’-dithio-bis-ethane sulfonate or dimesna) is a late-stage clinical drug candidate that was in-licensed by us from BioNumerik Pharmaceuticals, Inc. (“BioNumerik”) in May 2016, and subsequently acquired by us in January of 2018. Using our RADR®platform as part of the drug rescue process, we have identified LP-300 for use in a more targeted set of cancer patients who exhibit a biomarker profile that we believe correlates with non-or never smoking status but still have a form of non-small cell lung cancer (NSCLC). LP-300, originally branded as Tavocept®, is a molecular entity that we believe may be capable of ameliorating the toxic side effects of chemotherapeutic drugs such as cisplatin, and it also appears to act as a potential chemoenhancer. LP-300 has been studied in multiple randomized, controlled, multi-center non-small cell lung cancer (NSCLC) trials that included administration of either paclitaxel and cisplatin and/or docetaxel and cisplatin. Since acquiring LP-300 from BioNumerik, we have not yet conducted further clinical testing of LP-300. We are currently evaluating LP-300 for the launch of a targeted phase II trial, in non or never smoking patients with NSCLC in combination with chemotherapy, under an existing IND.
3
Prior clinical trials conducted by BioNumerik for LP-300 did not meet their primary clinical endpoints and at least one or more future clinical trials that meet their pre-specified primary endpoints with statistical significance will be required before we can obtain a regulatory marketing approval, if any, to commercialize LP-300. Prior clinical trial observations are not necessarily predictive of the outcome of any future clinical trials we may conduct.
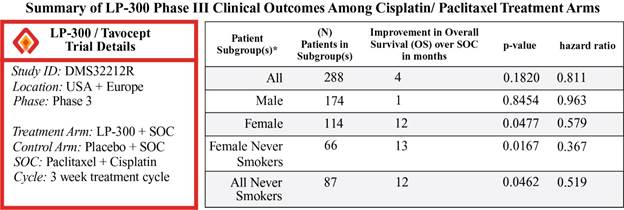
Retrospective analyses of the results of a multi-country phase III lung cancer trial conducted by BioNumerik in subgroups of NSCLC adenocarcinoma patients receiving LP-300, paclitaxel and cisplatin demonstrated substantial improvement in overall survival, particularly among female never smokers, where a 13.6 month improvement in overall survival (p-value 0.0167, hazard ratio 0.367) in favor of LP-300 was observed, as compared to placebo in the subgroup of paclitaxel/cisplatin-treated patients. Similar retrospective findings of increased overall survival in the subgroup of LP-300/paclitaxel/cisplatin treated female Asian patients with adenocarcinoma of the lung were observed in a randomized, double-blind, placebo-controlled trial in Japan. We plan on advancing this drug candidate for the never or non-smoker population of patients due to the following important market and clinical need factors:
| ● | As many as 40% of lung cancers either do not carry currently known targetable proteins or will progress despite initial therapy resulting in a dependence upon chemotherapeutic drug regimens in their treatment, and according to the Global Cancer Observatory, lung cancer is the second most common cancer with over 2 million cases globally. |
| ● | Approximately 40% of all lung cancers are adenocarcinomas, with more than half of such lung adenocarcinomas occurring in women. |
| ● | As many as 20% of people who die from lung cancer in the United States every year have never smoked or used any other form of tobacco. |
| ● | With declining rates of smoking, especially in North America and Europe, the relative proportion of lung cancer patients who are never-smokers is increasing, and this does not appear to be confounded by passive smoking or misreported smoking status. |
| ● | Women who have never smoked have a higher proportion of lung cancer than men who are lifelong never-smokers. |
| ● | In the clinical research community, a greater focus is being placed on lung cancers that occur in the never-smoking population along with the recognition that such lung cancers might be a genetically distinct type of cancer with a different molecular profile than smoking-based lung cancers. |
| ● | Mechanistic studies indicate that LP-300 may work by disruption at binding sites of oncoproteins such as ALK, MET, ROS1 and EGFR which are more commonly altered in female non-smokers and Asian females than in any other groups. |
| ● | Never-smokers have also been observed to be less responsive to therapies that stimulate or leverage the immune system such as checkpoint inhibitors or PD-1 and PL-L1 inhibitors. In a meta-analysis research publication of 1,981 patients by Drs. Li, Huang and Fu published in OncoTargets and Therapy, June 26, 2018 which spanned 3 Phase III randomized, controlled clinical trials the authors observed that, “…PD-1 inhibitors were more efficacious in smoking NSCLC patients compared with chemotherapy. No better survival of nonsmoking patients was observed in the treatment of PD-1 inhibitors than chemotherapy.” |
We are focused on advancing the development of LP-300 as a combination therapy for non or never-smokers with NSCLC adenocarcinoma and potentially among non or never-smokers with a genomic signature that correlates with a higher potential of response to this drug compound. We selected NSCLC in non- or never smokers as our lead proposed indication because it is a cancer with a growing patient population, without effective treatment options, and LP-300 has shown an improvement in overall survival in this targeted sub-group population in prior clinical studies.
4
In vitro studies indicate that the target-specific effects of LP-300 potentially correlate to the covalent modification of accessible cysteine residues important in protein function/structure. These could be involved in disruption/ blocking of cofactor binding sites resulting in blocking of oncoproteins such as ALK, MET, ROS1, and EGFR that are more commonly altered in female non-smokers than in any other group. Other potential mechanisms of action of LP-300 could include impact on stress induced oxidoreductases thereby allowing LP-300 to exert its potential chemo-enhancing effects in the presence of chemotherapeutic agents such as cisplatin. LP-300 is postulated to potentiate antitumor cytotoxicity of standard of care chemotherapy agents such as cisplatin. We believe a key LP-300 related mechanism is likely to occur through the increase of tumor cell sensitivity to oxidative stress. Additionally, via induction of NRF2 (also known as NFE2L2), LP-300 has the potential to provide protection of healthy cells against chemotherapy-associated toxicity, and such protection potential was observed with LP-300 combination therapy in both prior nonclinical studies and clinical trials
A differential gene expression analysis of whole transcriptome profiling data from LP-300 treated versus untreated NSCLC adenocarcinoma cells has been performed. Using a threshold of fold change > 2 out of a set of 51 curated NRF2 (NFE2L2) target genes as well as NRF2 itself, we observed the top significantly upregulated genes in response to LP-300 exposure. Based on our observations, we believe these genes could include NFE2L2, NQO1, PHGDH, HMOX1, SLC7A11, SRXN1, SOX2, GPX2, GPX3, GPX4, GPX7, G6PD, SIRT1, ITGB2 and BCL2. Our analysis indicates that these genes preferentially map to the following biological signaling pathways: (i) detoxification of reactive oxygen species; (ii) glutathione metabolism; and (iii) inflammatory response. We filed a patent application in March of 2020 on this discovery.
The interaction network of selected genes along with the associated biological pathways is shown in the figure below.

5
As part of our overall growth strategy, we plan to grow our pipeline by identifying new drug candidates and pursuing potential indications for both LP-184 and LP-300 while leveraging our RADR® platform. We are also pursuing the identification and design of potential combination therapies in cancer for our compounds by leveraging our RADR® platform to analyze synergistic genomic networks and biological pathways with other currently approved drugs. We intend to select our next clinical program in the next twelve months.
We have an extensive multi-national portfolio of intellectual property directed to our drug candidates, and to protect the targeted use and development of our portfolio of compounds in specific patient populations and in specific therapeutic indications. In addition, as our RADR® platform and other machine learning driven methodologies progress and mature, we will continue to evaluate additional ways to further protect these assets.
As of March 2021, we own or control over 70 active patents and patent applications across 14 patent families whose claims are directed to our drug candidates and what we plan to do with our drug candidates. We have in-licensed or acquired patents from AF Chemicals, and BioNumerik that are directed to the compounds, LP-100, LP-184 and LP-300. Additionally, we have also filed patent applications to further enhance, and extend the use of these in-licensed compounds. Our 14 patent families are directed to our drug candidates, their usage, manufacturing and other matters. These matters are essential to precision oncology and relate to: (a) uniquely powerful, data-driven, biologically relevant biomarker signatures, (b) patient selection and stratification approaches that rely on prediction of response derived from these signatures and, (c) the ability to develop novel, combination therapy approaches with existing therapeutics.
Our Drug Candidate Pipeline
One of the ways we are building our drug candidate pipeline is by in-licensing clinical stage drug candidates that may have been discontinued for development. We use our RADR® platform to assist in analyzing prior clinical research conducted by others to identify small-molecule oncology drug candidates that have (i) a well-tolerated profile evidenced by completion of phase I clinical trials, and (ii) demonstrated at least limited antitumor or anticancer activity in clinical trials. We intend to implement an efficient and thorough workflow to advance the drug candidates in our pipeline as potential precision medicine treatments for cancer. Our targeted development workflow includes preclinical studies where drug activity and associated gene signatures are identified, in part through strategic collaborations with some of the top academic institutions and clinical translational centers in the world. Using this collaborative approach, together with innovative observations from our RADR® platform, we intend to develop and add drug candidates to our pipeline with the objective of treating the right patient populations with the right oncology therapies.
We use our RADR® platform to identify potential biomarkers for patient response to a drug candidate and we further intend to validate the selected drug candidate and potential associated biomarkers by conducting small, focused early phase clinical trials. We intend to create various exit opportunities between one to three years for each drug candidate that progresses successfully. For each drug candidate that progresses, along with its newly identified biomarker diagnostic potential for drug response, we intend to partner, out-license, or internally develop the drug.
6
Our current pipeline of development programs involves three small molecule drug candidates: LP-100, LP-184 and LP-300.

| ● | LP-100 (6-Hydroxymethylacylfulvene or irofulven) LP-100 has been out-licensed to Allarity Therapeutics and is in a phase II clinical trial in AR-targeted and Docetaxel-Pretreated mCRPC Patients. |
| ● | LP-300 (Sodium 2,2’-disulfanediyldiethanesulfonate) (Tavocept®) We are currently evaluating LP-300 for the launch of a phase II clinical trial, in combination with chemotherapy in non-smokers or never-smokers with NSCLC adenocarcinoma that have a unique biomarker profile. |
| ● | LP-184. (hydroxyureamethylacylfulvene) LP-184 is a next generation alkylating agent with nanomolar potency that preferentially damages DNA in cancer cells that overexpress certain biomarkers. LP-184 is in preclinical development and is in the planning stages for a phase I clinical trial. |
LP-100 is currently being advanced by our licensee, Allarity Therapeutics. LP-184 and LP-300 are being advanced solely by us. There is currently no active IND in the U.S. for LP-100 and LP-184. We currently have an existing IND in the U.S. for LP-300 that was transferred to us as part of our in-licensing and agreement with BioNumerik to acquire the rights to the compound.
Additional Portfolio Opportunities
Based on the recognition of antibody drug conjugates (ADCs) as a promising therapeutic approach for cancer treatment, and one that has growing interest due to the potential to increase targeted cancer cell death, we have started reviewing our portfolio of small molecules for their potential to be used as part of an ADC approach. ADCs can increase selectivity and maximize tumor cell death and also minimize collateral toxicity. Our compounds LP-100 and LP-184 have the potential to be linked to antibodies (or peptides) and used in potential additional indications or alongside other small molecules or immuno-oncology agents. We believe that LP-300 can also play a role in developing ADC constructs and increasing the potential to deliver targeted therapies. We are actively researching and reviewing potential development pathways and partnerships that would enable us to develop an ADC complement to our portfolio.
The last two years have seen five FDA approvals in the growing class of ADCs for therapeutic use. This has driven increased deal-making and portfolio additions by large pharma companies. In addition to the acquisition of Immunomedics by Gilead, Merck acquired Velos Bio in November of 2020 and NBE Therapeutics was acquired by Boehringer Ingelheim in December of 2020. It is notable that both NBE and Velos, at the time of their acquisition, had just successfully completed Phase 1 trials using their ADC approach in specific cancer subtypes.
7
On December 30, 2020, we entered into an Evaluation and Limited Use Agreement (the “Evaluation Agreement”) with Califia Pharma, Inc. (“Califia”). Califia’s founder, Michael J. Kelner, M.D., is a widely published researcher with recognized expertise in the areas of illudofulvene chemistry and antibody drug conjugates. Califia has developed novel transcriptional-coupled repair inhibitors that have demonstrated potential for an improved therapeutic index compared to traditional ADC payloads.
The Evaluation Agreement provides for Lantern and Califia to collaborate on the in vitro and in vivo testing and evaluation of novel Califia payloads conjugated to a Lantern targeting entity. The Evaluation Agreement also provides us with the right to negotiate with Califia for exclusive license rights to use LP-184 and related analogs as the payload with an affinity drug conjugate or small molecule drug conjugate targeting entity supplied by Lantern. We also have the right under the Evaluation Agreement to negotiate for non-exclusive license rights to use a Lantern targeting entity with a payload and linker combination selected from novel specified Califia payloads and linkers.
We plan on increasing our focus on CNS (Central Nervous System) cancers based on the promising data that has been generated in experiments conducted with LP-184. LP-184 has shown that it can cross the blood brain barrier (BBB) while leaving neuronal cells intact. This unique profile has been validated in neuronal cell-plate assays, neuronal spheroids, and also in xenograft models and is now undergoing further validation in a collaboration with an affiliate of the Johns Hopkins School of Medicine. We have launched a program in GBM, and have uncovered several additional CNS cancers we believe will be sensitive to LP-184 based on genomic profiling and biomarker analysis conducted with our A.I. platform, RADR. We expect to focus additional resources on developing LP-184 as both monotherapy and combination therapy in several rare and ultra-rate CNS and brain cancers.
Based on the positive data regarding the blood brain barrier permeability for LP-184, we reviewed and analyzed a range of CNS cancers, beyond GBM, that we believe to have the potential to be responsive to LP-184 and make an improvement in patient survival. One of the CNS tumor types that was identified by RADR was ATRT, Atypical Teratoid Rhabdoid Tumor, which is a very rare, fast-growing tumor of the brain and spinal cord. It usually occurs in children aged three years and younger, but can also occur in older children and sometimes adults. However, the younger the patient the poorer the prognosis for survival. ATRT has no known approved targeted therapies and there is no standard chemotherapy regimen. According to the NCI, approximately 90 percent of ATRTs are characterized by a SMARCB1 mutation, which significantly reduces the ability of the surrounding cells to suppress the tumor. ATRT occurs in about 50 to 60 children per year and less than 10 adults per year, although recent diagnosis has increased due to improved access to cancer care and improved diagnostic methods. We believe that we can target this genetically defined subset of ultra-rare ATRT cancers, and plan on pursuing this indication in collaborations with academic cancer centers and potentially pursuing orphan or fast-track status if the additional data we obtain supports that this has the potential for changing the clinical outcome for patients.
We have obtained initial cell line data regarding LP-184 and ATRT that we believe supports the potential for LP-184 to qualify in the future for possible grant of a Rare Pediatric Disease Designation for use of LP-184 for ATRT. Additionally, we believe that subject to LP-184 successfully completing required clinical trials and regulatory requirements, LP-184 for the rare disease indication of ATRT may also potentially qualify for grant of a Rare Pediatric Disease Priority Review Voucher ("PRV"). Under Section 529 of the Federal Food, Drug, and Cosmetic Act, FDA will award a PRV to sponsors of rare pediatric disease product applications that meet certain criteria. Under this program, a sponsor that receives approval for a drug or biologic for a rare pediatric disease may qualify for a PRV that can be redeemed to receive expedited review of a subsequent product marketing application. A PRV may be redeemed by the company that initially receives it, or the PRV can be sold to another company.
Our Precision Cancer Therapy Development Using Our Innovative RADR® Platform
Historically, cancer treatment protocols include surgery, chemotherapy and radiation therapy. Treatments have been selected based on histologic type and disease spread, irrespective of genetic differences among patients. With the advent of precision therapies, cancer treatments increasingly target specific genes or mechanisms of action for a more personalized approach to patient care. This trend represents a substantial advance in cancer treatment because tumor growth is highly dependent on genetic changes and the genetic profile of the individual and the progression of the disease is highly variable amongst patients.
Our RADR® platform is core to our drug development approach for identifying the desired candidates to in-license and develop. According to a recent article in JAMA (Estimated Research and Development Investment Needed to Bring a New Medicine to Market, 2009-18, JAMA, March 3, 2020) oncology drug development is costly, risky, and highly competitive with an average success rate of 4% to 8% and average developmental costs of over $1 billion per successful drug. There is a critical need to rescue clinical research on drugs that have failed clinical trials in order to provide additional possible therapies for patients while reducing the overall cost of therapeutic development. Many drug failures within oncology may be attributed to the heterogeneity of the tested patient population, even though there may be a strongly positive therapeutic impact on certain patient subgroups within that population.
8
As data-centric and machine learning approaches begin to change the pace and scale of drug discovery and development, research and development (“R&D”) we believe efforts in large biopharma companies will begin to shift away from traditional approaches towards new data and A.I.-centric approaches. According to Deloitte Consulting, in Ten Years On | Measuring the return from pharmaceutical innovation 2019, “decades of advances in science and technology have driven improvements in health care outcomes and influenced stakeholder expectations of the role of the biopharmaceutical industry (biopharma). However, the past decade has seen increasing pressures undermine the productivity of biopharma R&D, leading to a decade of decline in the return on investment. At the same time, innovative new treatments are changing the face of disease management. New treatment modalities and an increasing understanding of precision medicine have led to the need for new R&D models...” The Deloitte Consulting report further describes that R&D costs will, “shift from traditional discovery and trial execution to a process driven by large datasets, advanced computing power and cloud storage”.
Analysts estimate that this shift from traditional screening, and trial-based studies to leveraging in silico, data and A.I. methodologies will drive a significant increase in the spending on A.I. by the biopharma and drug discovery community to approximately $4 billion by 2021, increasing by about 40% annually from $730 Million in 2019 according to PMLive and Global Market Insights. As a result of these trends and changes in the R&D model in biopharma, we believe that we, and companies that are using data-centric and A.I. centric approaches to drug discovery and development, are in an ideal position to benefit from this industry shift that has the potential to help deliver drugs to the right patients faster, with a higher degree of personalization and a potentially lower amount of average costs in the development cycle.
Our drug rescue approach leverages substantial prior research and development investments in candidates that were withdrawn from development prior to submission for FDA approval. The large volume of failed compounds, recent developments that permit increased access to validated genomic and biomarker data, and the rapid evolution of AI technology creates an opportunity to efficiently capitalize on these investments.
Our RADR® platform is rapidly emerging as a robust and scalable platform for targeted cancer therapy development. Through the use of AI and machine learning, RADR® is designed to quickly identify and guide the development of compounds that we can develop as potential oncology agents through either a process of drug rescue, drug repositioning or de-novo development. RADR® is being developed on a routine basis through an accumulation and curation of genomic and biomarker data that is directly relevant to the measurement and classification drug-tumor interaction, and clinical datapoints related to patient response and patient stratification.
Predicting optimal drug responses in cancer patients requires the identification and validation of predictive biomarkers. Our RADR® platform seeks to identify biomarkers to assist in selecting patients who have the highest likelihood to respond to our drug candidates. For example, the targeted indications for our drug candidate LP-184 were chosen in part because they are known to highly express the protein coding gene PTGR1. Our preclinical “PRostate cancer Artificial Intelligence Study using Ex vivo models” or “PRAISE” trial and our planned clinical trial for LP-184 are intended to examine biomarkers related to LP-184’s molecular and cellular targets to identify those that may correlate with clinical observed anticancer activity. This method of using and validating targeted biomarkers during development and then using these biomarkers during clinical trials can lead to shortening of the development timeline and compression of costs associated with oncology drug development.
Similarly, we believe LP-300 targets molecular pathways that are more common in female non- or never smokers than in any other group and also targets kinases involved in key signaling pathways involving enzymes critical for DNA synthesis and repair, such as Excision Repair Cross-Complementation Group 1 (ERCC1), Ribonucleotide Reductase 1 (RNR1), Ribonucleotide Reductase 2 (RNR2), as well as enzymes and proteins important in regulating cell redox status, such as Thioredoxin (TRX), Peroxiredoxin (PRX), Glutaredoxin (GRX), and Protein Disulfide Isomerase (PDI). Our plan is to bring LP-300 into a targeted phase 2 clinical trial within the non- or never-smoker sub-group that are identified with the adenocarcinoma sub-type of NSCLC.
9
Our RADR® Platform
The human genome consists of 19,000 to 20,000 protein coding genes. One input record derived from available data bases and analyzed by our RADR® platform consists of datapoints (expression values) from approximately 20,000 genes, another input record type is drug sensitivity data (IC20, IC50), and other sets include key clinical parameters from HIPAA compliant patient data and clinical histories. Our RADR® platform uses a data-driven gene feature selection methodology that is a combination of biology, informatics, and statistics – computational biology. The architecture and modules of our platform are depicted in the image below.

RADR® Platform Architecture and Modules
Our platform uses AI and machine learning to identify genes and genomic signatures believed to be highly correlated with drug sensitivity. These statistically significant genes are furthered filtered in the pathway network and interaction analysis to identify genes believed to be biologically relevant. Genes that make up this layer are either related to the molecule’s mechanism of action or heavily connected to each other in gene networks. Lastly, another inductive learning algorithm ranks these filtered genes based on drug sensitivity by calculating the half maximal inhibiting concentration (IC50) of the correlated relationship. In this way, our platform has the potential to predict drug sensitivity, classify a patient as responder or non-responder and identify biomarkers for each drug-tumor combination.
We developed our platform using primarily open-source third party supervised algorithms such as Neural Networks, Support Vector Machine, Random Forest, K-Nearest Neighbors, Logistic Regression and Penalized Multivariate Regression. Each algorithm is trained with input data to predict drug sensitivity (regressor models) and stratify patient response as responder or non-responder (classifier models). Model tuning and optimization is then performed using a hyperparameter search algorithm in order to produce the predicted lowest cross validation error. The models are then evaluated using traditional performance metrics such as accuracy, area under the curve, sensitivity, specificity, precision, root mean square error and mean absolute error calculations.
10
A feature reduction algorithm is then used to reduce the number of genes under analysis to a biomarker gene panel of less than approximately 50 genes. This set of genes is intended to carry the highest coefficient to predict drug sensitivity and the highest variable importance in classifying a responder from a non-responder. Genes that do not help in predicting the output variable are eliminated sequentially.

Our RADR® Platform Workflow
Our RADR® platform’s proprietary workflow involves preliminary statistical analysis on approximately 18,000 features typically from whole transcriptomic datasets reducing the set to approximately 2,000 features. This is followed by gene filtering via biological and statistical methodologies yielding approximately 200 significant genes. Feature selection ensures that genes that do not contribute to response prediction are excluded from the output dataset. The prediction component subsequently applies an A.I.-driven reduction algorithm to the previously filtered genes generating a targeted set of typically less than 50 candidate biomarkers predictive of response to a particular molecule.
A distinct and unique benefit of the RADR® platform is its ability to integrate biological knowledge and data-driven feature selection to generate hypothesis-free biomarker signatures. This can then aid in identifying novel targets for predictive screening and drug development.
Our RADR® platform is enabled through access to, and analysis of, a number of key datasets: (i) publicly available databases (ii) data from commercial clinical studies and trials and (iii) our proprietary data generated from ex vivo 3D tumor models specific to drug-tumor interactions. We incorporate automated supervised machine learning strategies along with big data analytics, statistics and systems biology to facilitate identification of new correlations of genetic biomarkers with drug activity. The value of the platform architecture is derived from its validation through the analysis of over 1.2 billion oncology-specific clinical and preclinical data points, more than 140 drug-cancer interactions, and over 55,000 patient records from five data bases, one of which is our internal data base. Our long-term objective is to collect and analyze over ten billion oncology-specific clinical and preclinical data points to further enhance the prediction power of our RADR® platform. We use cancer cell line gene expression profiles and drug sensitivity data (IC50) as one of its input types. In a population of 10 case studies our platform was able to distinguish responders from non-responders with an average historical accuracy of over 80%. We have also used our platform to generate genetic signatures that we believe to have applicability for the majority of FDA approved drug-tumor indications. External validation, through retrospective data analysis, of patient datasets from 10 independent clinical studies achieved an average response prediction accuracy greater than 80%, and internal analysis of 120 drug-tumor interactions in cell lines achieved an accuracy of greater than 85%.
11


We have developed our platform in a cloud environment that efficiently uses parallel processing to analyze patient stratification and biomarker selection. Best software engineering practices are followed while designing and developing our platform’s architecture. Each component of the platform’s architecture is unit tested and then integration tested to ensure functions and programs are working as designed. In order to track modifications in the software, a version control system is in place. Detailed documentation has been created to record the design and architecture of our platform.
Our platform uses a simple user input and GUI based AI architecture that can be used in many pharmaceutical research areas such as biomarker identification, patient stratification, drug rescue and reposition by bioinformaticians, clinicians and trained wet-lab scientists.
12

13
Our Strategy
Our mission is to bring the right cancer drugs to the right patients by transforming the drug development process through the use of artificial intelligence and data-driven development approaches. Our proprietary A.I.-enabled, and precision oncology approach, which focuses on developing our own pipeline of compounds by rescuing drug candidates that have previously failed and developing new compounds that are targeted to specific biological activity and genomic pathways, has the potential, we believe, to bring drugs to market faster, with lower costs, and with reduced risk, thereby enabling a change in the cost and availability of precision cancer therapy. We work with leading research laboratories, translational medicine and cancer centers to develop our studies and clinical trials for our portfolio, and actively update and improve our RADR® platform to incorporate additional biomarker data, patient outcome data, cancer drug efficacy studies and computational models that relate to oncology drug development and prediction of patient response.

As part of our growth strategy, we plan to:
| ● | Pursue existing indications for both LP-184 and LP-300, leveraging our RADR® platform to refine and optimize our trial design and biomarker signatures that correlate to potential patient response. |
| ● | Expand our pipeline by identifying new drug candidates that have either been abandoned or have failed in late stage clinical trials, and have the potential to benefit from a precision medicine approach that leverages our expertise and A.I. platform. |
| ● | Identify and design potential combination therapy approaches to use our compounds in conjunction with currently approved drugs by leveraging our RADR® platform to analyze and uncover synergistic mechanisms and biological pathways using genomics and machine learning. |
| ● | Increase the number of data points powering our RADR® A.I. platform from more than the current 1.2 billion to approximately three billion by the end of 2021. |
14
| ● | Advance the algorithms, methodologies and models that underlie our computational and machine learning platform to improve the predictive power, and to develop additional capabilities that are focused on accelerating or de-risking oncology drug development. |
| ● | Pursue collaborations and partnerships with other biotech and pharma companies where our A.I. and precision oncology expertise can be used to de-risk or accelerate development programs and where our stockholders can receive a significant economic benefit. |
| ● | Continue to develop and patent intellectual property and advance our intellectual property portfolio associated with both fundamental patents and patents associated with precision, patient stratified, targeted therapies and genomic or biomarker signatures. |
| ● | Select and launch our next clinical development program in the coming twelve months. |
LP-300
General Overview
LP-300 is a cysteine-modifying molecular entity that works to modulate multiple cellular pathways simultaneously and is a potential combination agent for targeted indications in NSCLC. LP-300 is a small molecule (molecular weight 326.4 Da) that was in-licensed from BioNumerik Pharmaceuticals, Inc. in May 2016, and subsequently acquired by us in 2018. We are focused on repositioning LP-300 as a potential combination therapy for non-smoking (or never-smoker) NSCLC patients with histologically defined adenocarcinoma. Since obtaining LP-300 rights from BioNumerik, we have not yet conducted further clinical testing of LP-300. We are currently evaluating LP-300 for the launch of a phase II trial, in combination with chemotherapy under an existing IND. Prior clinical trials conducted by BioNumerik for LP-300 did not meet their primary clinical endpoints, and at least one or more future clinical trials that meet their pre-specified primary endpoints with statistical significance will be required before we can obtain a regulatory marketing approval, if any, to commercialize LP-300. Safety and efficacy determinations are solely within the authority of the FDA in the U.S. or other regulatory agencies in other jurisdictions. Currently there is no approved therapy specifically for the growing indication of non-smokers (or never-smokers) with NSCLC, and female non- or never smokers appear to be uniquely responsive to LP-300. With both chemosensitizing and chemoprotective activity, LP-300 has potential as a combination agent or adjuvant in front line, second line or salvage therapy in newly diagnosed, relapsed, metastatic or advanced NSCLC for overall survival enhancement and toxicity alleviation from primary chemotherapy or standard of care. We are currently in the early stages of defining a specific biomarker signature that correlates with heightened sensitivity to LP-300. We believe that this signature may help accelerate the clinical development of LP-300 and has the potential to guide patient selection for targeted clinical trials.
LP-300 has been administered in multiple clinical trials to more than 1,000 patients and has been generally well-tolerated. Retrospective analyses of the results of a multi-country phase III lung cancer trial (study ID DMS32212R) in subgroups of adenocarcinoma patients receiving LP-300, paclitaxel and cisplatin demonstrated substantial improvement in overall survival, particularly among female never smokers, where a 13.6 month improvement in overall survival (p-value 0.0167, hazard ratio 0.367) in favor of LP-300 was observed, as compared to placebo in the subgroup of paclitaxel/cisplatin-treated patients. Similar retrospective findings of increased overall survival in the subgroup of LP-300/paclitaxel/cisplatin treated female Asian patients with adenocarcinoma of the lung were observed in a randomized, double-blind, placebo-controlled trial in Japan. Prior historical clinical trial observations are not necessarily predictive of the outcome of future trials. No assurances can be given that we will be successful in obtaining marketing approval for LP-300. The chemical structure of LP-300 is depicted below.
LP-300 Chemical Structure

15
Based on the subgroup observations of increased overall survival described above, we believe LP-300 has potential for an orphan indication designation in treating non- or never smokers with advanced NSCLC adenocarcinoma. Although orphan status has not previously been granted for non-smoking associated NSCLC, we believe pursuit of this designation is supported by the unique observations regarding LP-300 and the growing recognition that non-smoking associated NSCLC is a distinct disease type as compared to smoking associated NSCLC. Summarized below are some key findings from LP-300’s prior clinical trials:
| ● | LP-300 targets molecular pathways that are more common in female non-smokers than in any other group. Key mechanisms have been elucidated to support LP-300’s role in the observed treatment benefits for females and never smokers noted in the Phase III NSCLC adenocarcinoma trial. The rationale for these observations includes the following: (1) Met/ALK & EGFR alterations are more common in non-smokers, who are most commonly female and present with advanced stage adenocarcinoma; (2) laboratory data indicate that LP-300 targets both EGFR WT/mut+ and Met/ALK; and (3) a high percentage of adenocarcinoma patients are either EGFR mutants or Met/ALK positive. |
| ● | There are several key pathways in NSCLC adenocarcinoma whose targets are often overexpressed in females, and LP-300 modulates these pathways. LP-300 targets the following key pathways: (1) kinases involved in key signaling pathways (ALK, ROS, MET); (2) enzymes critical for DNA synthesis and repair (ERCC1, RNR1, RNR2); and (3) enzymes and proteins important in regulating cell redox status (TRX, PRX, GRX, PDI). The alterations that are targeted and modulated by LP-300 are more likely in women with lung adenocarcinoma, especially non-smokers. |
| ● | LP-300 showed that females had a survival increase from 13 months to 25 months, based on a retrospective subgroup analysis of a Phase III NSCLC adenocarcinoma trial. Results from a Phase III NSCLC adenocarcinoma trial exhibited an overall survival of 25.0 months, with a 2-year survival of 51.4%, in the subgroup of females with advanced adenocarcinoma of the lung receiving paclitaxel/cisplatin and LP-300. The observed results were statistically significant (p-value = 0.0477; HR=0.579) and were observed in a subgroup of 114 patients in retrospective analyses. Consistent statistically significant retrospective subgroup analysis results were observed in female NSCLC adenocarcinoma patients receiving paclitaxel/cisplatin and LP-300 in a prior LP-300 double-blind, placebo-controlled phase III trial conducted in Japan. |
| ● | LP-300 exhibits potential to reduce anemia and protect against chemotherapy-induced kidney toxicity, both of which are conditions that disproportionately affect females. The LP-300 arm of the Phase III NSCLC adenocarcinoma trial also demonstrated the potential for LP-300 to protect against chemotherapy-induced kidney toxicity and anemia. These findings complement earlier clinical observations regarding LP-300’s potential to protect against neuropathy and other chemotherapy-induced toxicities. |
Background-Scope of Prior Phase III NSCLC Adenocarcinoma Trial (LP-300)
LP-300 was studied in a randomized, multi-center (trial locations in four US states and five European countries), double-blind and placebo-controlled Phase III trial from 2010 to 2013 in patients with adenocarcinoma of the lung (the “Phase III NSCLC adenocarcinoma trial”). The aim of the trial was to determine whether LP-300, combined with a standard combination of chemotherapy drugs, would increase survival in patients with advanced NSCLC adenocarcinoma. The secondary aim of the trial was to determine if the chemoprotective properties of LP-300 were effective in preventing or reducing common side-effects of cancer treatment, including kidney damage, anemia, nausea and vomiting that can occur with these drug combinations. The trial enrolled NSCLC patients with newly diagnosed or recurrent advanced (stage IIIB/IV) primary adenocarcinoma of the lung. Patients with confirmed histopathological diagnosis of inoperable and measurable advanced primary adenocarcinoma (including bronchioalveolar cell carcinoma) of the lung, and no prior systemic treatment for NSCLC including chemotherapy, immunotherapy, hormonal therapy, targeted therapies or investigational drugs, were included in the trial. Overall survival was the primary outcome measure. Patients in the control arm received standard of care (cisplatin and either paclitaxel or docetaxel) plus placebo, whereas patients in the treatment arm received standard of care (cisplatin and either paclitaxel or docetaxel) plus LP-300. The primary results of the trial for patients receiving cisplatin and paclitaxel are outlined in the table below. While the overall results of the Phase III NSCLC adenocarcinoma trial did not meet the specified endpoint of the trial in increasing overall survival in all patients, when the data were retrospectively separated by gender and smoking status, the trial data demonstrated that all never smokers, especially female never smokers, saw increased survival with LP-300 combination treatment with paclitaxel and cisplatin. Furthermore, the LP-300 group in the phase III NSCLC adenocarcinoma trial exhibited well-tolerated advantages relating to the potential to protect against chemotherapy-induced nephrotoxicity, neuropathy and nausea along with reduced anemia.
16
The figure below depicts the survival curves for cisplatin/paclitaxel subgroups for the Phase III NSCLC adenocarcinoma trial that ended in 2013, as summarized. The Kaplan Meier curves maintain consistent separation between treatment arms for the never smokers, females, and female never smokers.

17
Rationale Behind LP-300 Rescue and Repositioning Efforts
Based on the results from the prior Phase III NSCL adenocarcinoma trial, we are in the process of designing a new Phase II clinical trial to target the population of non- or never smokers with adenocarcinoma that saw the greatest benefit in the previous Phase III trial. Although the incidence of non-smokers with NSCLC is rising currently there is no approved therapy specifically for the growing indication of non-smokers (or never-smokers) with NSCLC. Preclinical observations support that LP-300 preferentially modulates ALK and EGFR, two commonly mutated genes in non-smokers with adenocarcinoma. Based on the findings from the previous Phase III NSCL adenocarcinoma trial, it is possible that the benefits of combining LP-300 with standard of care chemotherapy could be further improved by identifying additional molecular biomarkers in patients who respond well to LP-300 combination treatment. We continue to seek additional opportunities for LP-300. Some of our considerations include a non- or never smoker population with a specific genetic signature that correlates to increased LP-300 sensitivity. We believe that this may also qualify as an orphan (rare disease) designation being a defined subset of NSCLC.
Clinical Translation Strategies
We have conducted discussions with more than ten key opinion leaders (KOLs) in the US, UK and India who recognized non-smokers with NSCLC adenocarcinoma as a unique population that could benefit from targeted precision oncology therapy. We intend to invite active participation and input from clinical and regulatory experts including KOLs and FDA authorities to facilitate evaluation of parameters important for repositioning our LP-300 program and conducting precision clinical trials.
Disease Background and Opportunity
Lung cancer remains one of the most common and deadly cancers worldwide. Lung cancer accounts for 13% of all new cancer diagnoses but 24% of all cancer deaths. Lung cancer kills more people annually than cancers of the breast, prostate, colon, liver, kidney, pancreatic, and melanoma combined. The American Cancer Society’s estimates for lung cancer in the US for 2019 are:
| ● | Approximately 228,150 new cases of lung cancer (116,440 in men and 111,710 in women) |
| ● | Approximately 142,670 deaths from lung cancer (76,650 in men and 66,020 in women) |
The most common type of lung cancer is called non-small cell lung cancer (“NSCLC”), which represents about 85% of all lung cancer.
Lung adenocarcinoma, a histological subtype of NSCLC that originates within the glands that line the lung, is the most common subtype of lung cancer in the world inflicting approximately 50% to 65% of non-Asians and approximately 70% to 85% of Asians diagnosed with lung cancer. According to the SEER Cancer Statistics Review (November 2018) published by the National Cancer Institute and other published literature, 60% to 65% of all new lung cancer diagnoses are among people who are former smokers or have never smoked, while 10-15% of new lung cancer cases are among never-smokers.
Over one-half of the patients diagnosed with NSCLC in any given year will present with inoperable advanced (stage IV) disease, for which there is no cure. Patients with stage IV NSCLC exhibit a median overall survival time of 8 to 10 months; approximately one-third of patients will survive for year, and only 10% to 21% of those patients will survive for two years.
Lung cancer is the most common cause of global cancer-related mortality, leading to over a million deaths each year and adenocarcinoma is its most common histological subtype. Worldwide, lung cancer occurred in approximately 2.1 million patients in 2018 and caused an estimated 1.8 million deaths. NSCLC is described as any type of epithelial lung cancer other than small cell lung cancer (“SCLC”). The 5-year survival rate for NSCLC is 16%. Rapid advances in understanding the molecular pathogenesis of NSCLC have demonstrated that NSCLC is a heterogeneous group of diseases. Although the initial treatment of localized disease is the same, the molecular characterization of tumor tissue in patients with NSCLC serves as a guide to treatment both in those who present with metastatic disease and in those who relapse after primary therapy. Molecularly targeted therapies have dramatically improved treatment for patients whose tumors harbor somatically activated oncogenes such as mutant EGFR1 or translocated ALK, RET, or ROS1. Mutant BRAF and ERBB2 are also investigational targets. Smoking is the major cause of lung adenocarcinoma but, as smoking rates decrease, proportionally more cases occur in never-smokers (defined as less than 100 cigarettes in a lifetime). KRAS mutations in lung cancer cases are nearly exclusive to smokers. KRAS, “Kristen rat sarcoma viral oncogene homolog,” is a protein involved in regulating cell division. KRAS mutation is a gain-of-function mutation (i.e. somatic mutation turns RAS, a benign gene “proto-oncogene” into KRAS, an oncogenic driver of many tumors). KRAS-mutated non-small cell lung cancer represents 20% to 25% of all NSCLC. There are no current KRAS-mutated NSCLC-targeted therapies but there are targeted therapies for the indication by targeting downstream pathways - for example mTOR inhibition. Tumor suppressor gene abnormalities, such as those in TP53, STK11, CDKN2A8, KEAP1, and SMARCA4 are also common but are not currently clinically actionable.
18
In reviewing lung cancer incidence and mortality rates among never-smokers in the Journal of Clinical Oncology, Wakelee, H.A. et al. have reported that the age-adjusted incidence rates of lung cancer among never-smokers aged 40 to 79 years from large population-based cohorts ranged from 14.4 to 20.8 per 100,000 person-years in women and 4.8 to 13.7 per 100,000 person-years in men, supporting earlier observations that women are more likely than men to have never smoking-associated lung cancer. The biology of lung cancer in never-smokers is apparent in differential responses to epidermal growth factor receptor inhibitors and an increased prevalence of adenocarcinoma histology in never-smokers. Lung cancer in never-smokers is an important public health issue needing further exploration of its incidence patterns, etiology, and biology. Due to the fact that there are no known therapy options for this group, we believe that aggressive development of therapy options is needed and is a high unmet clinical need.
The table below illustrates the growing concern of lung cancer in nonsmokers and never-smokers, and is a sample of the recent literature on the topic of never-smokers that the Company has used in assessing the potential patient and unmet clinical needs in this cancer.
|
Source |
Date of Study / Publication | Illustrative Quote | ||
| American Cancer Society | Oct. 31, 2019 | “As many as 20% of people who die from lung cancer in the United States every year have never smoked or used any other form of tobacco.” | ||
|
Journal of Royal Society of Medicine |
Aug. 25, 2019 | “Globally, there is wide variation in the proportion of lung cancers in never-smokers, in the range of 10% to 25%. With declining rates of smoking, the relative proportion of lung cancers in never-smokers are increasing and this does not appear to be confounded by passive smoking or misreported smoking status.” | ||
| Roswell Park | Apr. 3, 2019 | “…15% of lung cancers are found in people who have never smoked.” | ||
| Cancer Research U.K. | Nov. 16, 2018 | “Around 10-15% of the lung cancer patients I see have never smoked.” | ||
| ASCO – The Asco Post | Dec. 25, 2017 | “In the United States, about 20% of women with lung cancer are never-smokers, and about 7% of men with lung cancer are never-smokers.” | ||
|
Clinical Cancer Research September 2009
|
Sep. 15, 2009 | “The lung cancer death rates among never-smokers, although “rare” by conventional definitions (<40,000 US deaths per year), is similar to the death rates from leukemia, and endometrial cancer in women and cancers of the esophagus, kidney, and liver in men in the United States, and may be even more important in other populations, including Chinese women |
19
In 2019 in the US, 9,034 cases of NSCLC adenocarcinoma cases are estimated to be diagnosed in female non-smokers, accounting for approximately 3.9% of all lung cancer cases. With an estimated 120,000 globally projected adenocarcinoma cases of NSCLC in non-smoking females in 2019, this specific indication may possibly be classified as a rare disease. When attempting to explain some gender susceptibility differences, research has demonstrated that women with NSCLC tend to be:
| ● | Younger; |
| ● | Asian; |
| ● | 2-3 times more likely to be non-smokers; |
| ● | more likely to develop adenocarcinoma and; |
| ● | having metastatic disease. |
The high rate of adenocarcinomas in non-smoking women suggests the possible existence of other etiological factors in addition to smoking. Some factors that have been considered include gender-specific genetic alterations and predispositions, passive smoke effects, different nicotine metabolism in women, occupational exposure, diet, and chronic obstructive pulmonary disease. Based upon 2018 estimates published by Global Cancer Observatory and 2019 estimates published by the American Cancer Society, below is an overview of relevant potential patient population and market sizes that we believe LP-300 could address, if approved:
| Lung cancer | Global | US | ||||||
| Total 2019 lung cancer estimated incidence (new cases) | 2,000,000 | 228,150 | ||||||
| NSCLC adenocarcinoma incidence (~40% of all lung cancers) | 800,000 | 91,260 | ||||||
| Never-smokers estimate (~15% of adenocarcinoma) | 120,000 | 13,689 | ||||||
| Female never-smoker estimate (~66% of never-smokers with lung cancer are female) | 79,200 | 9,034 | ||||||
| Total Patient Segment in New Lung Cancer | 4.0 | % | 4.0 | % | ||||
Limitations on Current Treatment
Treatment of patients with advanced NSCLC in the first-line setting usually includes chemotherapy (including taxanes, vinorelbine, or gemcitabine) in combination with a platinum doublet (cisplatin or carboplatin). According to the clinical practice guidelines published by the National Comprehensive Cancer Network, many of these combinations have reached a plateau in terms of overall response (≥ 25% to 35%), time to progression (four to six months), median survival time (eight to ten months), one-year survival rate (30% to 40%), and two-year survival rate (10% to 15%) in patients with good performance status. Treatment remains palliative and is limited due to inherent toxicities that may affect the quality of life resulting from treatment. Toxicities can be life-threatening or cause treatment delays, thereby limiting the intensity of treatment delivered and affecting its efficacy. Common and serious chemotherapy-induced toxicities, such as anemia, emesis, and peripheral neurotoxicity resulting from treatment with platinum and taxanes, and nephrotoxicity due to cisplatin can result in treatment delays, dose modifications, and in severe cases, discontinuation of treatment. We believe it is important to pursue the development of novel therapies and combinations thereof that can substantially improve patient survival and quality of life by potentiating the antitumor activity of chemotherapy treatment while protecting against chemotherapy-induced toxicity.
Market Opportunity
Most non-smoker patients with lung cancer are women, and adenocarcinoma is the most common type. Non-smoker patients with non-small-cell lung cancer (“NSCLC”) generally have a better response to inhibitors of epidermal-growth-factor receptor (EGFR) tyrosine kinase, including without limitation gefitinib and erlotinib, than do those with a history of tobacco smoking. Studies have identified differences in chromosomal aberrations, genetic polymorphisms, gene mutations, and methylation status between lung cancer in non-smokers and tobacco-associated lung cancer. These clinical and biological differences suggest that the two cancers have overlapping but unique pathways of carcinogenesis. The EGFR mutation is one of the most important genetic change in lung cancer in people who have never smoked because it is more common in lung cancer in never-smokers than in tobacco associated lung cancer and is associated with greater therapeutic benefit from inhibitors of EGFR. Other alterations associated with never-smokers include mutations, fusions or amplifications in ALK, ROS1, RET and MET genes. Based upon published articles in CA: Cancer Journal for Clinicians and Nature Review Cancer, incidence in never-smokers is 10% to 15% of all lung cancers and globally, NSCLC in never-smokers comprises 15% to 20% of cases in men and greater than 50% in women. In Asia, never-smokers with NSCLC are 60% to 80% women and 20% to 40% men.
20
We are focused on advancing LP-300 as a potential combination therapy for non- or never smoking NSCLC patients with adenocarcinoma by leveraging our A.I. platform to help uncover the genomic and biomarker networks that are associated with response in the never-smoker and non-smoker groups. Additionally, through our early, preclinical work to define a gene signature that correlates with heightened sensitivity to LP-300, we believe there is potential to further expand the indication to include all NSCLC patients that have this identified genetic profile in their cancer. Currently there is no approved therapy specifically for the growing indication of non-smokers (or never-smokers) with NSCLC, and female non- or never smokers appear to be uniquely responsive to LP-300. If successful, LP-300 could provide improved patient benefit in terms of improved survival, and secondarily through the concurrent prevention and mitigation of common and serious chemotherapy-induced toxicities.
LP-300 Summary of Preclinical and Clinical Studies
Through partnerships and third-party outsourcing arrangements, we are conducting, or have conducted, the following preclinical studies on LP-300.
Cell line work with third party CROs
A study was conducted to assess whether LP-300 induces or suppresses specific biological pathways or functions that impact tumor cell proliferation, survival or apoptosis. In this study, NSCLC cell lines were exposed to selected concentrations of LP-300 alone and in combination with cisplatin, for defined duration. After exposure to the drugs in cell culture according to the chosen treatment conditions, RNA was obtained and transcriptomic analysis was performed using a NovaSeq 6000 next-generation sequencing platform. Overall, 1.26 million data points were generated and analyzed from this study yielding differential gene expression profiles between LP-300 untreated versus treated samples. Key pathways that emerged as being regulated by LP-300 include redox homeostasis and NRF2/Antioxidant Response Element signaling, among others.
We are working with a preclinical and discovery focused CRO to generate supporting preclinical data on LP-300 anticancer activity profiles in various molecular and demographic brackets of NSCLC cell line models. The goal of this study is to generate dose response curves and associated IC50 values for LP-300 alone as well as in combination with Cisplatin (standard of care agent) and selected targeted therapy agents on up to 20 different NSCLC cell lines. Genetic backgrounds of NSCLC drivers and related oncogenes in these cell lines are known, and will help to establish correlations between LP-300 cytotoxicity and specific markers. We intend to evaluate the status of LP-300 as a chemosensitizing agent, whether LP-300 triggers catastrophic oxidative stress, and understand specific transcriptional characteristics of tumors that are sensitive or resistant to LP-300 alone and in combination with other treatments. From this ongoing study, we hope to develop information to assist in further stratifying patients that would be key targets for future clinical trials. LP-300 could potentially be positioned to treat advanced NSCLC adenocarcinoma not just in never-smokers but also based upon genetic alterations.
Fox Chase Collaboration
We are engaged in discussions with Fox Chase Cancer Center (“FCCC”) to identify opportunities for collaborative research, both preclinically and clinically, for advancing LP-300. The objective is to develop studies to further elucidate the mechanism of action of LP-300, and to pursue a Phase II clinical trial in never-smokers with NSCLC. Regarding preclinical studies, we intend to discuss appropriate preclinical studies with cell lines, organoids or patient derived xenograft (PDX) models that are required to move forward to a clinical trial. In pursuing the areas of LP-300 related cysteine modification of EGFR / FGFR and other drivers commonly altered in never-smoking NSCLC, we plan on comparing LP-300 response in cell line models with EGFR exon 3 deletion, EGFR L858R/ T790M, exon 19 or 21 deletions, and EGFR wild type among other genetic backgrounds. We are interested in prioritizing studies that will progress towards a Phase II trial, including a PDX trial testing LP-300 in combination with selected tyrosine kinase inhibitors (TKIs) in addition to cisplatin / paclitaxel as standard of care agents in relevant models and comparing never-smokers and nonsmokers to smokers.
21
Prior Completed Trials of LP-300
Phase I. LP-300 has been evaluated in five Phase I studies (DMS10001, BioNumerik, 09/1997 through 04/2004; DMS10002, BioNumerik, 12/1997 through 08/2001; DMS12209, ASKA Pharmaceutical, 04/2000 through 12/2001; DMS10011, BioNumerik, 02/2006 through 07/2006; and DMS12307, Baxter, 07/2002 through 07/2005) to determine the maximum tolerated dose (“MTD”), and to evaluate the safety, tolerability, pharmacokinetics, and potential efficacy of LP-300 (alone or in combination with cisplatin, cisplatin/paclitaxel, or carboplatin/paclitaxel). An MTD for LP-300 was not reached in any of the Phase I studies at dose levels of up to 41 g/m2.
Phase II. In a U.S. multi-center, randomized, open-label trial (n=160 patients) with advanced (Stage IIIB and IV) NSCLC treated with LP-300 or no LP-300 (DMS22210/CALGB 30303, Cancer and Leukemia Group B, 08/2004 through 03/2007), although the overall population did not meet the pre-specified primary endpoint, an analysis of a subgroup of patients with adenocarcinoma revealed that the difference in the median overall survival period between the 2 treatment groups was statistically significant (LP-300 = 15.6 months, no LP-300 = 8.9 months; Log-rank p=0.0326), and the median overall survival for patients who received LP-300 was 6.7 months longer than that of those who did not receive LP-300.
Phase III. LP-300 has been evaluated in five Phase III studies: two in patients with metastatic breast cancer, with a primary endpoint examining the ability to reduce platinum/taxane induced peripheral neuropathy, and three in patients with NSCLC or advanced primary lung adenocarcinoma. (DMS32205R, ASKA Pharmaceutical, 08/2005 through 02/2008; DMS30203R, BioNumerik, 09/2001 through 10/2006; DMS30204R, ASKA Pharmaceutical, 04/2003 through 03/2006; DMS32206R, Baxter, 10/2002 through 04/2006; and DMS32212R, BioNumerik, 04/2010 through 06/2013) Although the overall population did not meet the pre-specified primary endpoints in any of the trials, analysis of subgroups of patients in one multi-country lung adenocarcinoma trial and one Japanese NSCLC trial revealed differences in the median overall survival between the two treatment arms (with or without LP-300 treatment). The results from the two key lung cancer trials obtained from retrospective analyses are described below:
| ● | Multi-country, double-blind, randomized, multi-center & placebo-controlled trial (n=540 patients) with advanced primary lung adenocarcinoma treated with LP-300 or Placebo & paclitaxel or docetaxel with cisplatin (DMS32212R). (the Phase III NSCLC adenocarcinoma trial) |
| Ø | Treatment with LP-300 nearly doubled the Overall Survival in women receiving paclitaxel/cisplatin (25.0-month median OS in LP-300 arm vs. 13.2-month OS in control arm) and the results in this subgroup were statistically significant (P-value = 0.0477; HR = 0.579) |
| Ø | For never smoking women with adenocarcinoma of the lung receiving paclitaxel/cisplatin, the Overall Survival in the LP-300 arm was more than double the control arm (27.0 months vs. 13.4 months, respectively) also being statistically significant in favor of LP-300 (P-value = 0.0167; HR = 0.367) and the 2-year survival was 72.4% in the LP-300 arm vs. 32.3% in the control arm. |
| ● | Statistically significant subgroup analyses and trends from this LP-300 Phase III NSCLC adenocarcinoma trial support repositioning LP-300 for non- or never smokers with adenocarcinoma of the lung. |
| ● | Randomized, double-blind, placebo-controlled and multi-center trial in patients with advanced NSCLC receiving paclitaxel & cisplatin (Japan Trial) (DMS32205R). The Japan Trial observations support and complement observations in the multi-country Phase III NSCLC adenocarcinoma trial. The observations for the female adenocarcinoma patient population in the LP-300 multi-country Phase III NSCLC adenocarcinoma trial are consistent with observations made for the subgroup of females with adenocarcinoma of the lung receiving paclitaxel/cisplatin and LP-300 or placebo in the Japan Trial. Although the overall population in the Japanese trial did not meet the pre-specified primary endpoint, a retrospective analysis of the subgroup consisting of female patients with adenocarcinoma revealed that the difference in the median overall survival period between the two treatment arms in this subgroup was significant (P-value = 0.0456, HR = 0.376). |
22
The LP-300 arm of the multi-country Phase III NSCLC adenocarcinoma trial also demonstrated safety profile advantages in terms of the potential to protect against chemotherapy-induced kidney toxicity and chemotherapy-induced anemia. These observations complemented earlier clinical observations regarding LP-300’s potential to protect against neuropathy and other chemotherapy-induced toxicities. Results from these trials indicate that treatment with LP-300 may, in further clinical testing, lead to improved survival in female and non- or never smoking patients with primary adenocarcinoma of the lung receiving cisplatin/paclitaxel combination chemotherapy.
Phase II and III LP-300 Adverse Events Summary
The following summarizes adverse events reported from a total of 1,712 patients enrolled in five randomized multi-center phase II and phase III studies with chemotherapy, with or without LP-300. A total of 1,712 patients were enrolled in these studies, of which 856 patients received LP-300 with chemotherapy.
| ● | All Adverse Events (AEs). The most frequently-occurring adverse events in patients receiving LP-300 with chemotherapy were generally similar to patients receiving placebo or chemotherapy alone. These events included blood and lymphatic system disorders (myelosuppression manifested as anemia, leukopenia, lymphopenia, neutropenia, and thrombocytopenia; also including decreased hematocrit, hemoglobin, lymphocyte count, neutrophil count, red blood cell count, platelet count, and white blood cell count), with an incidence ranging from 12% to 83%; gastrointestinal disorders including constipation, abdominal pain, diarrhea, nausea, stomatitis, and vomiting, with an incidence ranging from 22% to 83%; general disorders and administrative site conditions including fatigue (ranging from 17% to 85%); infusion/injection site pain/reactions (ranging from 12% to 18%); malaise (ranging from 16% to 28%); peripheral edema (ranging from 13% to 22%); pyrexia (ranging from 10% to 17%); infections and infestations disorders including nasopharyngitis (ranging from 11% to 16%); investigations including increased liver function tests including ALT, AST, and alkaline phosphatase (ranging from approximately 10% to 55%); increased blood lactate dehydrogenase (ranging from approximately 17% to 26%); increased blood urea or blood uric acid (ranging from approximately 11% to 32%); increased gamma-glutamyltransferase (ranging from approximately 23% to 33%); decreased total protein (ranging from approximately 12% to 21%); metabolic and nutritional disorders including weight decreased (ranging from 15% to 22%), anorexia (ranging from 14% to 82%), and hypomagnesemia (ranging from 22% to 30%); musculoskeletal and connective tissue disorders including arthralgia, back pain, and myalgia (ranging from 7% to 80%); nervous system disorders including dysgeusia (ranging from 12% to 22%), headache (ranging from 14% to 17%), and peripheral neuropathy (motor and sensory – ranging from 22% to 86%); psychiatric disorders including insomnia (ranging from 12% to 17%); respiratory, thoracic, and mediastinal disorders including dyspnea (ranging from 12% to 40%); skin and subcutaneous disorders including alopecia (ranging from 33% to 92%); rash (ranging from 22% to 29%); nail disorder/discoloration (10%); and vascular disorders including angiopathy (ranging from 64% to 69%) and flushing (ranging from 15% to 39%). |
| ● | Treatment-Related Adverse Events. Frequently occurring treatment-related AEs experienced by patients receiving LP-300 with chemotherapy included gastrointestinal disorders manifesting as nausea and vomiting (ranging from 12% to 67%, and 12% to 32%, respectively); fatigue (ranging from 22% to 82%); infusion/injection site pain/reactions (ranging from 11% to 18%); increased ALT (alanine aminotransferase) and gamma-glutamyltransferase (ranging from approximately 13% to 18%, and approximately 11% to 12%, respectively); peripheral neuropathy (motor and sensory – ranging from 14% to 54%); and vascular disorders including angiopathy (ranging from 60% to 69%), and flushing (ranging from 8% to 11%). |
| ● | Serious Adverse Events (SAEs). 11% to 49% of patients receiving LP-300 with chemotherapy, and 7% to 42% of patients in control groups receiving chemotherapy alone experienced SAEs during randomized multicenter studies. Frequently-occurring SAEs in patients receiving LP-300 with chemotherapy included pneumonia, hypersensitivity or drug hypersensitivity, dyspnea, pyrexia and dehydration, diarrhea, anaphylactic shock or anaphylactic reactions, vomiting, disease progression, infection, bronchospasm, pleural effusion, pulmonary embolism, thrombosis, hemolysis, nausea, chills, fatigue, sudden death, neutropenic infection, sepsis, anorexia, neutropenia, febrile neutropenia, pneumonitis, rash, and hypotension. Multiple allergic reactions have been reported in clinical trials of LP-300, and some of these reactions have been severe. It is possible that patients could experience an allergic reaction that is life-threatening. Five reports of grade 3 or 4 hemolysis events with three fatal outcomes were reported in patients receiving LP-300 with chemotherapy in a study involving the weekly drug administration schedule. Two events of hemolysis were reported in a study involving drug administration every two weeks. No events of hemolysis were reported in studies using the three weeks schedule of administration, which is the administration schedule used for the multi-country Phase III NSCLC adenocarcinoma trial. |
23
| ● | Treatment-Related Serious Adverse Events. Approximately 7% of patients receiving LP-300 with chemotherapy experienced treatment-related SAEs during randomized multicenter studies. The most frequently-occurring treatment-related SAEs experienced by patients receiving LP-300 with chemotherapy were hypersensitivity or drug hypersensitivity (five and two patients, respectively) and neutropenia (six patients). Other treatment-related SAEs experienced by patients receiving LP-300 with chemotherapy included hemolysis, bronchospasm, febrile neutropenia, anemia, nausea, and pulmonary edema (three patients, each); chills, diarrhea, pyrexia, neutropenic infection, hyperglycemia, acute respiratory distress syndrome, pulmonary embolism, sudden death, infection, and rash (two patients, each); and angina pectoris, cardiac arrest, tachycardia, sudden hearing loss, abdominal pain, vomiting, adverse drug reaction, anaphylactic shock, C. difficile colitis, pneumonia, sepsis, chemical cystitis, thrombosis in device, dehydration, leukopenia, anorexia, atrial fibrillation, fatigue, weight decrease, muscle disorder, pain in extremity, dizziness, peripheral sensory neuropathy, dyspnea, hypotension, and thrombosis (one patient, each). |
Clinical Evidence of Toxicity Protection by LP-300
The data from randomized multicenter studies of LP-300 and chemotherapy demonstrates objective evidence of several instances where treatment with LP-300 appears to provide potential benefit in terms of preventing and mitigating chemotherapy-induced toxicities, particularly in studies of LP-300 and chemotherapy in patients with advanced NSCLC. These data support that LP-300 has the potential to protect against chemotherapy-induced toxicities, including gastrointestinal, renal, electrolyte disturbances, and anemia; and there is data supporting the potential for LP-300 to protect against severe forms of these toxicities. In addition, treatment with LP-300 may protect against severe platinum-induced hearing loss and dehydration.
LP-300 Mechanism of Action
LP-300 is a water-soluble disulfide compound that lacks a free thiol or sulfate moiety. We postulate this unique structure of LP-300 may allow it to potentiate antitumor activity of certain types of cytotoxic chemotherapy, and exert chemoprotective effects, through distinct and interrelated mechanisms. In plasma, the lack of a free thiol prevents untoward reactivity and drug-drug interactions, and thereby may allow chemotherapeutic agents to retain their efficacy. Once inside the tumor cell, LP-300 is metabolized and may then potentiate antitumor activity of cytotoxic certain types of chemotherapy. A significant fraction of LP-300 is taken up by the kidneys, where LP-300’s metabolites can interact with chemotherapy drugs, such as cisplatin, and potentially diminish the chemotherapy drug’s ability to cause organ damage. We believe the postulated mechanisms that can enhance tumor directed chemosensitivity include restoration of apoptotic sensitivity thereby countering drug resistance; oxidative stress enhancement; anti-angiogenesis; decreased DNA synthesis and gene expression; and decreased glutathione and precursors (limiting glutathione tumor-mediated drug resistance). When LP-300 accumulates in the kidneys it appears to reduce the toxicity of certain drugs, such as cisplatin, that are excreted through the renal system.
As depicted in the model below, we believe LP-300 and its metabolites can modulate key components of the thioredoxin and glutaredoxin systems, which are believed to be involved as major mechanisms of the potentially enhanced antitumor effects of LP-300 with chemotherapy. The thioredoxin pathway is commonly upregulated in adenocarcinomas, and examination of primary lung tumors from non-smokers have shown significantly increased gene expression of thioredoxin. Overexpression of thioredoxin in cancer cells has been postulated to lead to resistance to apoptosis, increased cellular proliferation, increased gene expression, increased angiogenesis, increased conversion of DNA into RNA, and resistance to oxidative stress induction. We believe the modulation of thioredoxin expression is important for the observed increases in patient survival identified in retrospective analyses of certain subgroups of patients with primary adenocarcinoma of the lung receiving LP-300 in conjunction with cisplatin and paclitaxel chemotherapy. Different glutaredoxin transcript variants have been found to be elevated in transformed cells, and glutaredoxin isoforms (e.g., variants of glutaredoxin 2) have been found to be elevated in NSCLC cell lines, lending evidence for potential roles of glutaredoxin in tumor progression.
24
We believe LP-300 and its metabolites may potentiate the antitumor activity of chemotherapy by:
(1) shifting the redox balance and concentrations of reduced forms of thioredoxin and glutaredoxin to inactive oxidized forms of thioredoxin and glutaredoxin, thereby restoring apoptotic sensitivity, increasing sensitivity to oxidative stress, inhibiting cell growth and angiogenesis, RNA to DNA synthesis, and growth signaling, and
(2) forming thioredoxin or glutaredoxin adducts, which as inactive forms lead to thioredoxin- and glutaredoxin-mediated reduction of downstream targets in the cell that are important for tumor resistance to chemotherapy, angiogenesis and cell growth.

We believe that LP-300 may potentiate antitumor activity of certain types of cytotoxic chemotherapy, and exert chemoprotective effects through several distinct and interrelated mechanisms of action. LP-300 is a cysteine-modifying agent that appears to modulate multiple cellular pathways simultaneously. Experimental data indicate that LP-300 modifies and/or modulates the following key pathways:
| ● | Kinases involved in key signaling pathways (EGFR, ALK, ROS, MET) |
| ● | Enzymes critical for DNA synthesis and repair (ERCC1, RNR1, RNR2) |
| ● | Enzymes and proteins important in regulating cell redox status (TRX, PRX, GRX, PDI) |
25
The following key mechanisms have been observed to support our belief that LP-300 has potential to play an important role in the treatment of females and non- or never smokers with NSCLC adenocarcinoma. We believe these mechanisms help to explain the retrospective subgroup observations for females and never smokers receiving LP-300 together with cisplatin and paclitaxel in the Phase III NSCLC adenocarcinoma trial:
| ● | LP-300 targets cysteine residues. Computational and experimental data indicate that LP-300 demonstrates specificity towards cysteines. LP-300-mediated xenobiotic modulation of protein targets on cysteine results in distinct, (multi)target-specific effects correlated to the role of the cysteine residue(s) in the target. |
| ● | LP-300 alone inhibits human ALK and stimulates the inhibitory effect of crizotinib on human ALK. Alterations in ALK, along with MET, ROS1 & PDGFRA are thought to underlie nearly 10% of NSCLC adenocarcinoma cancers. Liquid Chromatography (LC), Mass Spectrometry (MS) and X-ray structural data demonstrate that LP-300 covalently modifies human ALK on Cys1156 and Cys1235. Enzyme assay data demonstrates that LP-300 inhibits human ALK’s kinase activity and stimulates the inhibitory effect of crizotinib on human ALK’s kinase activity. |
| ● | LP-300 inhibits human MET kinase activity and stimulates Staurosporine inhibition of human MET kinase activity. Mesenchymal Epithelial Transition Factor Kinase (MET) kinase mutations and amplification are an important, specific subset of NSCLC adenocarcinoma. Enzyme assays demonstrate that LP-300 inhibits human MET kinase activity and stimulates the inhibitory activity of staurosporine on human MET kinase. |
| ● | LP-300 inhibits EGFR kinase activity. EGFR mutations are an important, specific subset of NSCLC adenocarcinoma, particularly in non-smoker females. Enzyme assays demonstrate that LP-300 inhibits EGFR kinase activity and potentiates the inhibitory effect of eErlotinib on wild type as well as mutant EGFR kinase activity. |
| ● | LP-300 modestly inhibits retinal rod outer segment kinase (ROS1) activity. ROS1 chromosomal rearrangements are a recently identified class of mutations in NSCLC. Estimates of frequency of ROS1 rearrangements range from 1% to 2%. Experimental data are as follows: |
| Ø | Enzyme activity data demonstrates that LP-300 has an effect on Human ROS1 activity when ROS1 is preincubated with LP-300. We hypothesize that pre-incubation allows slower reacting cysteine residues to be modulated by LP-300. |
| Ø | Based on modeling studies, the cysteines on ROS1 appeared to be in less optimal orientations compared to cysteines in ALK. |
| Ø | LP-300 appears not to impact ROS1 activity unless ROS1 and LP-300 are pre-incubated prior to kinase assays. Therefore, to see an effect in vivo, it may be necessary to administer LP-300 prior to LP-300’s effects on ROS1 through preincubation of ROS1 and LP-300, suggesting slower xenobiotic modulation reactions. However, there are several possible explanations for the LP-300 effect on ROS1 and in the absence of an X-ray structure this remains a hypothesis. |
| ● | LP-300 modifies Ribonucleotide Reductase 1 and 2 (RNR1 and RNR2). Selective, elevated expression of the RNR1 subunit is associated with gemcitabine resistance in NSCLC. RNR1/RNR2 are essential for DNA synthesis, DNA repair & cell proliferation. RNR1/2 catalyzes the formation of deoxyribonucleotides needed for DNA synthesis, from ribonucleotides. |
| ● | LP-300 targets proteins that may result in protection against chemotherapy-induced nephrotoxicity and neuropathy. The LP-300 derivative-cisplatin/paclitaxel conjugate is inactive and this conjugate is not a substrate for aminopeptidase/γ-Glutamyl-transpeptidase (APN/GGT). These LP-300 heteroconjugates appear to cause potent inhibition of APN/GGT leading to suppression/bypass of renal APN/GGT xenobiotic metabolism pathways promoting protection against chemotherapy-induced nephrotoxicity. In addition, binding of the LP-300 derivative with reactive cisplatin/paclitaxel species, appears to inactivate the platinum-catalyzed microtubule hyper-polymerization. This action may serve to protect against chemotherapy-induced peripheral neuropathy. |
| ● | LP-300 modulates protein function in a way that may promote chemosensitization. LP-300 appears to promote covalent oxidation of redox proteins Thioredoxin (TRX), Peroxiredoxin1 (PRX1) and Glutaredoxin (GRX). This action may keep these redox proteins in an inactive non-signaling state, which could enhance sensitivity to oxidative stress and apoptosis induced by concomitant chemotherapy. |
26
Using various in vitro experimental approaches, LP-300 has been observed to form adducts on cysteines of various protein targets such as those listed below. For several of these targets, studies evaluating enzyme activity associated with the targets have demonstrated inhibition, modulation or impairment of such activity. In addition, X-ray crystallographic studies support LP-300 derived adducts at specific cysteines on these proteins.
Targeted Proteins Modified by LP-300
| Cellular Target of LP-300 | Cellular consequence of LP-300-modification and/or modulation | |
| Cellular thiol/disulfide balance | LP-300 and LP-300-derived mesna disulfide heteroconjugates are pharmacological surrogate/modulators of physiological thiols and disulfides (e.g., glutathione, cysteine, and homocysteine). | |
| Gamma-Glutamyltranspeptidase Aminopeptidase N | LP-300 and LP-300-derived mesna disulfide heteroconjugates can inhibit gamma-glutamyltranspeptidase and aminopeptidase N enzyme activity. | |
| Tubulin | LP-300 exerts direct and indirect protective interactions with tubulin. | |
| Anaplastic Lymphoma Kinase (ALK) | LP-300 disrupts/blocks ATP binding site resulting in inhibition of ALK kinase activity (vide infra). | |
|
Mesenchymal Epithelial Transition (MET) Factor Kinase |
Modification of non-active site cysteine(s) resulting in enzyme inhibition (MET). | |
| ROS1 kinase | LP-300 xenobiotically modifies ROS1 kinase in a time dependent manner. | |
| Redox Balance | LP-300 and LP-300-derived mesna disulfide heteroconjugates assist in the maintenance of cellular redox balance and support cellular defenses against oxidative insult. | |
| Thioredoxin (Trx) Glutaredoxin (Grx) | LP-300 modifies non-catalytic cysteines important in redox protein function/structure (Grx and Trx). | |
| Thioredoxin (Trx) Glutaredoxin (Grx) | LP-300 and/or LP-300-derived mesna disulfide heteroconjugates function as alternative substrates/inhibitors (Trx, Grx) resulting in impaired enzyme activity. | |
| Peroxiredoxin (Prx) | LP-300 disrupts active site structure (Prx) resulting in impaired enzyme activity. |
Mechanistic evaluation of LP-300 revealed that it has cysteine-modifying activity on select Receptor Tyrosine Kinases (RTKs) initiating proliferative signaling such as ALK, EGFR, MET and ROS1. LP-300 may also serve as a potential chemosensitizer for certain combination chemotherapies by inactivating proteins such as Thioredoxin (TRX), Glutaredoxin (GRX) and Peroxiredoxin (PRX) that are important in modulating cellular redox status and in turn drug resistance. Higher levels of PRX gene expression have been shown to correlate significantly with the absence of smoking history and with the female gender.
We believe well-tolerated profile advantages of LP-300 are imparted through its chemoprotective action via production of inactive LP-300-chemotherapeutic conjugates and preventing toxic taxane/platinum metabolites in the kidney, and targeting toxicity-inducing molecules and pathways (e.g. APN, GGT, and Tubulin).
We plan to conduct additional mechanism of action studies aimed at identifying and validating signaling molecules and pathways selectively triggered by or responding to LP-300, as well as identifying additional potential drug combinations for clinical applications. Using female non- or never smoker-derived lung adenocarcinoma cell lines that are sensitive to the combination of cisplatin, paclitaxel and LP-300, we intend to analyze the induction of expressed genes in a time and concentration-dependent manner. Identification of a pharmacodynamic biomarker that would be relevant at a lower dose of LP-300 could be a potentially valuable outcome of this investigation. We intend to employ established cell lines with known genetic backgrounds as well as fresh patient tumor specimens as in vitro or ex vivo model systems to perform drug response assays and genomic/ transcriptomic profiling. We believe these studies may assist with determination of correlations between frequently occurring known driver mutations or resistance-related alterations in ALK, EGFR, MET, ROS1 etc. and sensitivity to LP-300.
27
Planned Phase II Clinical Trial for LP-300
We intend to conduct a Phase II clinical trial of LP-300 in patients with adenocarcinoma NSCLC that are believed most likely to respond to treatment based on the characteristics of the tumor being treated and other preclinical studies being conducted with CROs and key collaborators. This proposed clinical trial will be subject to obtaining input from the FDA and other regulatory bodies, as well as approval by investigators and Institutional Review Boards. We anticipate employing a combination therapy approach that includes a doublet chemotherapy treatment. Our planned clinical trial of LP-300 may span over a two year period or more in either a single center or in multi-center locations involving approximately 40 to 75 patients diagnosed with adenocarcinoma NSCLC with little to no history of smoking and no prior chemotherapy treatment. We further anticipate that the primary objective of the study will be to investigate the response to treatment with a recommended Phase II dose of LP-300 in combination with chemotherapy in non- or never smoking patients with NSCLC. Secondary objectives may include (i) to assess the efficacy of LP-300 in combination with chemotherapy in patients with NSCLC and non- or never smoking status, (ii) to assess the efficacy of LP-300 in combination with chemotherapy in non-smoking females versus non-smoking males with NSCLC, (iii) to further investigate the safety and toxicity profile/tolerability of the LP-300 and chemotherapy combination, and (iv) to investigate biomarkers correlated with potential efficacy of LP-300 in paired tumor biopsies. We expect that the primary endpoint of the study will be overall survival with possible secondary endpoints of (i) progression-free survival, (ii) objective response rate, (iii) identification of gene signatures correlated with potential LP-300 efficacy from matched tumor tissue analysis, and (iv) protection against chemotherapy-induced nephrotoxicity. We have contracted with Patheon API Services, Inc., a division of Thermo Fisher Scientific, Inc., to manufacture a sufficient quantity of the active pharmaceutical ingredient for LP-300 to conduct a phase II trial.
Our RADR® Platform’s Approach to LP-300 Repositioning
Our RADR® platform is being implemented with the objective of uncovering insights from LP-300 rescued preclinical data as well as from lung cancer clinical trial data regarding actionable bioinformatics, biomarkers, target population demographics and smoking history. Differential expression analyses of RNAseq data on LP-300 pre- and post-exposure in selected NSCLC cell lines has revealed gene sets that could be upregulated and downregulated in response to LP-300 treatments involving the mapping of genes performing cellular redox functions, kinases involved in proliferating signaling, and apoptotic markers. We are currently in the early stages of defining a specific biomarker signature that correlates with heightened sensitivity to LP-300. We believe that this signature may help accelerate the clinical development of LP-300 and has the potential to guide patient selection for targeted clinical trials. We are also developing a list of approved cancer drugs that, when used in combination with LP-300, may have potential to improve the overall benefit to patients through either potentially greater anticancer properties or improved tolerability. We believe identifying such combinations would be attractive to established pharmaceutical and biotech companies.
Acquisition of Tavocept® (LP-300) Rights from BioNumerik
In January 2018, we entered into an Assignment Agreement (the “Assignment Agreement”) with BioNumerik Pharmaceuticals, Inc. (“BioNumerik”), pursuant to which we acquired rights to domestic and international patents, trademarks and related technology and data relating to LP-300 for human therapeutic treatment indications. Mr. Margrave, our Chief Financial Officer and Secretary, formerly served as the President, Chief Administrative Officer, General Counsel and Secretary of BioNumerik and has a minority ownership interest in BioNumerik. The Assignment Agreement replaced a License Agreement that was entered into between us and BioNumerik in May 2016. We made upfront payments totaling $25,000 in connection with entry into the Assignment Agreement.
28
If we commercialize LP-300 internally, we will be required to pay to the BioNumerik-related payment recipients designated in the Assignment Agreement a percentage royalty in the low double digits of cumulative net revenue up to $100 million, with incremental increases in the percentage royalty for net cumulative revenue between $100 million and $250 million, $250 million and $500 million, and $500 million and $1 billion, with a percentage royalty payment that could exceed $200 million for net cumulative revenue in excess of $1 billion. In addition, we have the right to first recover certain designated portions of patent costs and development and regulatory costs before the payment of royalties described above. We are obligated to make royalty payments under the Assignment Agreement during the “Agreement Term” that started on January 5, 2018 and continues (on a country-by-country and product-by-product basis) until the later to occur of (i) five (5) years after the expiration of the last to expire Patent Rights, as defined in the Assignment Agreement, in an applicable country in the Territory, as defined in the Assignment Agreement, and (ii) if no Patent Rights exist in such country, fifteen (15) years after May 31, 2016.
If we enter into a third party transaction for LP-300, we are required to pay the BioNumerik-related payment recipients a specified percentage of any upfront, milestone, and royalty amounts received by us from the transaction, after first recovering specified direct costs incurred by us for the development of LP-300 that are not otherwise reimbursed from such third party transaction. In addition, the Assignment Agreement provides that we will use commercially diligent efforts to develop LP-300 and make specified regulatory filings and pay specified development and regulatory costs related to LP-300. The Assignment Agreement also provides that we will provide TriviumVet DAC (“TriviumVet”) with (i) specified data and information generated by us with respect to LP-300, and (ii) an exclusive license to use specified LP-300-related patent rights, trademark rights and related intellectual property to support LP-300 development in non-human (animal) treatment indications. Under the Assignment Agreement, we are required to pay all patent costs on covered patents related to LP-300. Patent costs paid by us with respect to LP-300 related patents amounted to approximately $59,000 and $74,000 for the years ended December 31, 2018 and December 31, 2019, respectively. These patent costs are fully recoverable at the time of any net revenue from LP-300, with up to 50% of net revenue amounts to be applied towards repayment of patent costs until such costs are fully recovered. In addition to the recovery of patent costs, we have the right to recover the $25,000 upfront payments made in connection with entry into the Assignment Agreement, which payments are recoverable prior to making any royalty or third-party transaction sharing payments. We also have the right to recover all previously incurred LP-300 development and regulatory costs, with up to a mid-single digit percentage of net revenue amounts to be applied towards repayment of development and regulatory costs until such costs are fully recovered.
LP-184
General Overview
LP-184 (hydroxyureamethylacylfulvene) is currently in preclinical development. LP-184 is a small molecule drug candidate that is a next generation alkylating agent that preferentially damages DNA in cancer cells that overexpress certain biomarkers. It is from the fulvene class of compounds. LP-184 has nanomolar potency and it is a member of a new generation of acylfulvenes, a family of naturally-derived anticancer drug candidates. Earlier generations of acylfulvenes showed great promise in preclinical studies, but were hampered in human clinical studies because of the inability to deliver effective therapeutic doses due to unacceptable toxicities to normal cells. In preclinical studies, LP-184 has shown significantly enhanced antitumor activity and substantially reduced toxicity as compared to earlier generation acylfulvenes. In addition, we have used our RADR® platform, together with work of collaborators, to develop a patient-specific biomarker test we believe will be predictive of LP-184’s anticancer activity in targeted patient populations. We plan on using this test to facilitate patient selection in our planned Phase 1 clinical trial for LP-184. The chemical structure of LP-184 is depicted below.
29

LP-184 Chemical Structure
We have conducted LP-184 preclinical studies using fresh biopsy material from patients with advanced prostate cancer, which we see as a potential LP-184 indication. In addition, we are also evaluating LP-184 in a number of solid tumors that overexpress certain biomarkers that have been identified as correlating with potential response to LP-184. Preliminary analysis suggests that LP-184 is also expected to be a pro-drug likely activated by the enzyme Prostaglandin Reductase 1 (“PTGR1”). We believe LP-184’s mechanism of action is to alkylate DNA and protein macromolecules, form adducts, and arrest cells in the S-phase of the cell cycle.
In preclinical studies, LP-184 has demonstrated tumor regression in a xenograft mouse model of multi-drug resistant lung adenocarcinoma without dose-limiting toxicities. In mouse model studies, LP-184 further demonstrated favorable in vivo pharmacokinetic properties including increased half-life, plasma stability and bioavailability with reduced total body clearance. Further preliminary results from mouse studies reveal a better in vivo hematological profile for LP-184 with decreased neutropenia and thrombocytopenia events.
Using our RADR® platform, we have derived a 10-gene signature composed of candidate biomarkers determining sensitivity to LP-184. Genes from this signature, such as PTGR1, were found to be implicated in the potential induction of bioactivation of LP-184. We believe LP-184 may be well positioned as a new drug candidate for individual patient genetic profiles identified as having DNA repair complex deficiencies or other commonly prevalent gene signatures. LP-184 displayed less bone marrow toxicity in preclinical studies (dog and mouse), had an improved pharmacokinetic profile (increased bioavailability as reflected by increased AUC), was stable in plasma, and had an increased shelf life or stability in pharmaceutical grade material (sterile glass containers) for its class of compounds. LP-184 retained selective cytotoxicity towards solid tumor derived cell lines in vitro. LP-184 can be synthesized from original stock material (Illudin S) with additional steps.
30
We believe LP-184 is a non-hormone, non-chemotherapy, next generation alkylating agent with nanomolar potency that preferentially damages DNA in cancer cells that overexpress certain biomarkers indicated primarily in solid tumors such as those in prostate, pancreatic and ovarian cancers. LP-184 was developed using combinatorial chemistry approaches. Based on screening against conventional therapies both in vitro and in vivo, LP-184 cytotoxicity appears to be mediated through the Transcription Coupled Nucleotide Excision Repair (TC-NER) pathway, via alkylation of DNA leading to cell cycle arrest in S phase. Additional cytotoxic effects on tumors may include the generation of reactive oxygen species, chemical modification of various intracellular proteins, and induction of the Mitogen Activated Protein Kinase (“MAPK”) pathway followed by apoptosis. A proposed model for the mechanism of action of LP-184 is illustrated below.

We anticipate that the results from ongoing preclinical cell line studies will inform the targets for broader indications for LP-184 in solid tumors. Our RADR® platform has identified multiple solid tumor cancer indications that highly express PTGR1, including prostate, ovarian, kidney, liver, lung, pancreatic and thyroid cancers. Our RADR® platform will be employed to correlate results from ongoing preclinical studies with gene expression data to attempt to determine the likely anticancer activity of LP-184 in these cancer indications. Based on these results, we intend to conduct follow-up studies in patient derived xenografts (PDX) models to further elucidate precise targets and potential patient groups for future LP-184 clinical trials.
LP-184 Biomarker Background Using Our RADR® platform
LP-184 biomarker studies are being conducted by us to investigate the validity of relevant biomarkers. An NCI-60 cell line panel is being used to obtain gene expression data and sensitivity data (GI50). Determination of potential biomarkers for LP-184 target indications is performed by correlation analysis between normalized gene expression and GI50 values followed by biological and statistical filtering. For further testing, we intend to acquire biopsy tissues (from prostate and ovarian cancer patients) to perform gene expression analysis, predict potential drug response using Artificial Intelligence and machine learning and validate the results experimentally by preclinical drug sensitivity testing.
31
Our RADR® platform was used to analyze our dataset on preclinical LP-184 sensitivity to and baseline gene expression profiles of 57 cell lines from the NCI-60 panel. Panel A in the figure below highlights the comparison of LP-184 sensitivity prediction accuracy across a range of biomarker numbers. Starting from greater than 18,000 genes, our RADR® platform identified the 10 most significant genes as predictive of response to LP-184 treatment. As depicted in panel B below, out of 18 cell lines included in the blinded test set, our RADR® platform correctly predicted all 10 out of the actual 10 sensitive cell lines. Panels C and D show model performance metrics such as area under curve (AUC) and confusion matrix representation, respectively. Model training was performed using an initial set of 66 genes derived from 39 cell lines from the NCI-60 dataset. Model testing was conducted on 18 cell line records isolated as the blinded hold-out set.
We believe that genes from the 10 identified by our RADR® platform have been shown to be functionally involved in the postulated mechanism of action of LP-184, thereby reaffirming our belief in the utility and value of our RADR® platform. We intend to further extend and validate these cell line-derived preliminary biomarker analyses using LP-184 sensitivity and gene expression data derived from fresh tumor biopsy samples. Our goal is to determine the molecular profiles of patient tumors that predict potential drug response and to derive a diagnostic assay for stratifying patients. We believe that precision biomarker approaches increase the likelihood that a treatment will be found to be effective in a relatively small phase II cohort by eliminating the most likely non-responders and selecting the most likely responders. We anticipate that our RADR® platform driven determination of molecular profiles of tumor tissues that are sensitive to LP-184 will greatly assist with stratification of patients in a future phase II clinical trial.

As described above, analysis of LP-184 using our RADR® platform yielded a 10-gene pan-cancer signature of candidate biomarkers associated with LP-184 sensitivity. We intend to further validate these preliminary biomarker analyses using LP-184 sensitivity and pre-treatment gene expression data derived from ex vivo models of fresh tumor biopsy samples from selected cancer indications. Furthermore, gene weightage analysis was performed using Garson’s function to analyze the relative ranking of 10 genes in the LP-184 signature associated with anticancer sensitivity. We believe that PTGR1 stands out as the gene with the highest relative importance for purposes of determining LP-184 sensitivity.
32

The effect of gene expression on the response variable was also studied across the identified LP-184 signature genes using the Lek’s profile function as depicted below. We believe that the high expression of PTGR1 is significantly correlated to a possible positive anticancer response to LP-184. The Lek’s profile method explores the relationship of the outcome variable and a predictor of interest, while holding other predictors at constant values.
33

Numerous studies have determined that PTGR1 expression is elevated in several tumor types, including prostate. Our RADR® platform analyses indicate that tumor cells with high PTGR1 expression may be more sensitive to DNA damaging drugs like LP-184. Independent studies suggest that PTGR1 may be responsible for converting LP-184 to its active form. These two results support our belief that PTGR1 is the most prominent biomarker for predicting LP-184’s potential anticancer activity in targeted tumor types. Clinical mapping of PTGR1 expression profile was performed in independent historical datasets of unselected prostate cancer patients. Using our RADR® platform, we analyzed historical data from a total of 2,204 prostate cancer patients from 14 different studies and identified that on average 30% of the patient population showed high PTGR1 expression, and 39% of the patient population showed intermediate PTGR1 expression, representing a group of patients that has the potential to be at least partial responders to LP-184.
Disease Background for Prostate, Ovarian and Liver Cancer
Initial target patient populations for LP-184 include advanced cancers of the prostate and ovary. Based on computational analysis of in vitro cell line sensitivity data, we believe additional cancer types, including liver, kidney and thyroid, deserve further consideration as target indications in which LP-184 is predicted to have potential anticancer activity.
Prostate Cancer
Prostate cancer is the most commonly diagnosed cancer in men in the US and the second leading cause of cancer-related death in men in the US. The American Cancer Society’s estimates for prostate cancer in the United States for 2019 are:
| ● | Approximately 174,650 new cases of prostate cancer |
| ● | Approximately 31,620 deaths from prostate cancer |
34
Approximately 50% of patients who die from prostate cancer have metastases at diagnosis. The survival gains over the last decade have been modest with acceleration in life-extending drug development occurring in the last three years. Hormonal therapy works to reduce testosterone levels in the body to a level equal to that seen if physical castration were to occur. However, hormonal therapy can become refractory after one to three years and tumor growth may resume. This is referred to as Castration-Resistant Prostate Cancer (“CRPC”). About 10 - 20 % of prostate cancer patients develop CRPC within five years. According to JP Morgan, in 2011, approximately 136,000 men were treated for CRPC. Typically, standard hormonal therapy involving Androgen Deprivation Therapy (ADT) was prescribed in the past for all comer patients. Current prescribed regimens involve intensified therapy for most patients (docetaxel for high volume disease, and Zytiga for low and high volume disease) whereas upcoming molecularly selected agents in addition to hormonal therapy are used in an individualized approach to metastasis-directed or local therapy. Standard of care agents for prostate cancer include without limitation (i) Androgen production suppressors, such as Leuprolide (Lupron, Eligard), Goserelin (Zoladex), Triptorelin (Trelstar), Histrelin (Vantas), Abiraterone (Zytiga), (ii) Androgen signaling blockers, such as Flutamide (Eulexin), Bicalutamide (Casodex), Nilutamide (Nilandron), and Enzalutamide (Xtandi), and (iii) chemotherapeutics such as docetaxel and cabazitaxel. Drug classes of new small molecules in development include PARP inhibitors, PI3K inhibitors and DNA Damage Repair (DDR) inhibitors. The PARP inhibitor rucaparib (Rubraca) has recently been approved by the FDA. The identification and characterization of new molecular targets, agents exploiting new or non-parallel mechanisms of action, and the discovery of predictive biomarkers for mCRPC, are three of the major unmet needs in the prostate cancer space in the era of precision medicine that we believe LP-184 may address.
Ovarian Cancer
According to the American Cancer Society and other published sources, ovarian cancer is the second most common gynecologic cancer in the US. Ovarian cancer ranks fifth in cancer deaths among women, accounting for more deaths than any other cancer of the female reproductive system. Ovarian cancer is the second most common gynecologic malignancy in developed countries, with an incidence of 9.4 per 100,000 women and a mortality rate of 5.1 per 100,000. In developing countries, it is the third most common gynecologic malignancy, with an incidence of 5.0 per 100,000 and a mortality rate of 3.1 per 100,000. About 85% of ovarian cancer patients stop responding to or relapse within two years after first line therapy. The American Cancer Society estimates for ovarian cancer in the US for 2019 are:
| ● | Approximately 22,530 women will receive a new diagnosis of ovarian cancer. |
| ● | Approximately 13,980 women will die from ovarian cancer. |
A woman’s lifetime risk of developing ovarian cancer is 1 in 75, and her chance of dying of the disease is 1 in 1004. The disease typically presents at late stage when the 5-year relative survival rate is only 29%. Few cases (15%) are diagnosed with localized tumor (stage 1) when the five-year survival rate is 92%. The overall five-year relative survival rate generally ranges between 30%–40% across the globe and has seen only modest increases (2%–4%) since 1995.
Carboplatin in combination with paclitaxel has been the standard of care in the adjuvant and first-line settings for ovarian cancer, and, despite all relevant efforts, improving upon this standard in clinical practice has proven extremely hard. Attempts to improve survival and response rates using a triplet rather than the traditional doublet have failed to demonstrate any effective advantage. Prolonging antineoplastic therapy after the conventional 5 to 6 cycles also was not reported to provide significantly better outcomes. Intraperitoneal or dose-dense chemotherapy, and alternative platinum doublets, have been tested alongside targeted therapies such as bevacizumab, pazopanib, nintedanib and PARP inhibitors (olaparib/ rucaparib) with limited success to date. At present, alternatives to standard therapy do exist, but none has proven to be superior to conventional treatments, with the notable exception of carboplatin-paclitaxel plus bevacizumab. In light of available data, none of the other options can be considered a “new standard” that fits all. We believe that LP-184 has the potential to serve patient subgroups from multiple cancer types based on their gene signature status in a tissue-agnostic manner.
35
Liver Cancer
According to estimates published by the American Cancer Society and other published sources, liver cancer incidence has more than tripled since 1980. Liver cancer develops approximately three times more often in men than in women. Liver cancer death rates have increased over 2% per year since 2007. The American Cancer Society’s estimates for primary liver cancer (hepatocellular carcinoma) and intrahepatic bile duct cancer (cholangiocarcinoma) in the US for 2019 are:
| ● | Approximately 42,030 new cases (29,480 in men and 12,550 in women) will be diagnosed |
| ● | Approximately 31,780 people (21,600 men and 10,180 women) will die of these cancers |
Market Opportunity for LP-184
We are targeting a set of indications for LP-184 based on combining the factors of predicted response, unmet clinical need and market opportunity. These include prostate, ovarian and liver cancers. Below is an overview of relevant patient numbers and market sizes that we believe LP-184 may potentially address, if approved, based upon published estimates by the Global Cancer Observatory and other published sources:
| Prostate cancer | Global | US | ||||||
| Total 2019 prostate cancer estimated incidence (new cases) | 1,300,000 | 174,650 | ||||||
| CRPC incidence, ~20% of all prostate cancer | 260,000 | 34,930 | ||||||
| Metastatic CRPC incidence, ~80% of newly diagnosed CRPC | 208,000 | 27,944 | ||||||
| Patient fraction in target segment | 16 | % | 16 | % | ||||
| Ovarian cancer | Global | US | ||||||
| Total 2019 ovarian cancer estimated incidence (new cases) | 300,000 | 22,530 | ||||||
| Estimated patients not responding to or relapsing within 2 years after first line therapy (85% of all ovarian cancers) | 255,000 | 19,150 | ||||||
| Patient fraction in target segment | 85 | % | 85 | % | ||||
| Liver cancer | Global | US | ||||||
| Total 2019 liver cancer estimated incidence (new cases) | 841,000 | 42,030 | ||||||
| Estimated patients with hepatocellular carcinoma (75% of all liver cancers) | 630,750 | 31,522 | ||||||
| Patient fraction in target segment | 75 | % | 75 | % | ||||
Summary of LP-184 Preclinical Studies
Below is a summary of preclinical studies conducted on LP-184:
LP-184 screening studies using MV522 lung cancer line.
In cell line screening studies, LP-184 retained toxicity against the MV522 lung cancer line but displayed reduced toxicity against the normal 8392 B cell and CHRF 288-11 megakaryocyte lines (platelet precursors). From the NCI-60 cell line panel, LP-184 demonstrated increased tumor-killing activities against a variety of cancer cell lines, notably prostate, ovarian, lung and renal cancers. These observations are summarized below.
36
| Cell Line | LP-184 IC50 (nM) | |||
| 8392 Normal B Cells | >100,000 | |||
| CHRF 288-11 Megakaryocytic Cells | 8,800 | |||
| PC3 Prostate | 140 | |||
| DU145 Prostate | 14 | |||
| OVCAR3 Ovarian | 100 | |||
| OVCAR5 Ovarian | 45 | |||
| A549 Lung | 70 | |||
| A498 Renal | 25 | |||
| MV522 Lung (multi-drug resistant) | 210 | |||
In hematotoxicity studies, animals were treated 3 times per week for 3 weeks with control (sterile saline), or LP-100 at 10 mg/kg (MTD), or LP-184 at 10 mg/kg (80% MTD). N=6, mean + SD. LP-184 neutrophil and platelet results vs LP-100; p <0.02. Based on these studies, we believe LP-184 shows potential for an enhanced in vivo hematological safety profile. LP-184 appears less toxic to normal blood cells than LP-100. Studies in mice showing WBC differentials data indicated that LP-184 induces less thrombocytopenia and neutropenia than LP-100. The tables and figure below summarize these observations.
Groups of 6 mice treated 3X per week for 3 weeks with 10 mg/kg drug
| Analyte | Control | LP-100 | LP-184 | |||||||||
| White blood cell count* | 4.57±0.82 | 1.97±0.44 | 3.02±0.67 | |||||||||
| Neutrophil count* | 1.61±0.19 | 0.51±0.03 | 1.03±0.11 | |||||||||
| Hemoglobin (g/dL) | 9.9 | 8.2 | 10.6 | |||||||||
| Platelet count* | 574±127 | 384±64 | 587±149 | |||||||||
| * | Cells per microliter |
In both human plasma and in mice, LP-184 demonstrated a superior pharmacokinetic property profile compared to LP-100.
| Pharmacokinetic property | LP-100 | LP-184 | ||||||
| Half life (h) | 0.1 | 2.4 | ||||||
| AUC (ng*h) | 695 | 2200 | ||||||
| Cmax (ng/ml) | 5650 | 9730 | ||||||
37


Xenograft studies by Staake, et al. 2016
38
In a preclinical animal study by Staake MD, et al. of Hydroxyurea derivatives of irofulven with improved antitumor efficacy reported in Bioort Med Chem Lett. 2016: 26(7): 1836-1838, LP-184 treatment indicated a greater tumor regression in a mouse model with human cancer than LP-100.
LP-184 was tested in a variety of xenograft models including MV522 lung adenocarcinoma and was found to be superior to LP-100 in its ability to induce tumor regression or complete tumor remission. As described in the following figure, treatment with LP-184 demonstrated substantial regression of lung cancer tumors in mice treated with the 10 mg/kg and 20 mg/kg doses.

Glioblastoma
Glioblastoma is a fast-growing, aggressive type of CNS (Central Nervous System) tumor that forms on the supportive tissue of the brain. Glioblastoma is the most common grade IV brain cancer. The American Cancer Society estimates that approximately 23,890 brain and other nervous system cancers (13,590 men and 10,300 women) will occur in the U.S. in 2020. It also estimates that in 2020, approximately 18,020 deaths will occur from brain and other nervous system cancers. Approximately 240,000 new glioblastoma cases are estimated to occur each year worldwide, with approximately 11,000 to 13,000 new glioblastoma cases estimated to occur each year in the U.S. Glioblastomas usually affect adults. Treating glioblastoma is very difficult due to the brain-blood barrier and treatment often focuses primarily on relieving symptoms. The standard treatment for glioblastoma includes radiation and chemotherapy with temozolomide. Based on an article in the journal Genes and Diseases (Temozolomide resistance in glioblastoma multiforme, Genes Dis., 2016 May 11;3(3):198-210) and other publications, at least fifty percent of temozolomide treated patients do not respond to this treatment, and others often form resistance to temozolomide based regimens.
Based on recent observations and a preclinical study, we believe that LP-184 could have potential as treatment (alone or in combination with other treatments) for glioblastoma, which is an aggressive type of cancer that begins in the brain and accounts for more than half of all brain cancers. Our A.I. platform has helped to uncover biomarkers that may make a patient more responsive to LP-184 for the treatment of glioblastoma as well as LP-184 in combination with other approved therapies. We have filed a patent application on this discovery.
39
Ongoing and Planned Preclinical Studies for LP-184
For LP-184, we have conducted and planned the following preclinical studies:
Cell line sensitivity studies. We have partnered with a CRO to generate key preclinical data on LP-184 anticancer activity profiles in various cancer types. The goal of this study is to generate dose response curves and associated IC50 values for LP-184 as monotherapy on 41 different cancer cell lines representing prostate, NSCLC, ovarian, liver, kidney and thyroid cancer indications. PTGR1 transcript levels in these cell lines are generally known, and will help to determine correlations between LP-184 cytotoxicity and PTGR1 gene expression. LP-184 sensitivity profiles in cell lines from various cancer types, including liver, NSCLC and ovarian, were compared with publicly available data for standard of care chemotherapy agents cisplatin and pemetrexed that are commonly prescribed in NSCLC. In this cell line panel, LP-184 showed nanomolar potency whereas cisplatin and pemetrexed were less effective. A representative chart demonstrating the superior potency of LP-184 is depicted in the graph below. From this ongoing study, we hope to identify tumor types in addition to prostate that would be key potential targets for future clinical trials. LP-184 could potentially be positioned to treat tumors not just based upon tissue of origin or histology, but upon the PTGR1 expression status of the tumors.

We have now demonstrated LP184 activity in a panel of NSCLC cell lines. The data we have obtained support LP-184’s potential as a candidate for lung cancers that carry mutations in genes such as KEAP, which otherwise make such tumors refractory to alkylating agents.
By utilizing wet lab generated IC50 values across several tumor cell lines, including prostate, NSCLC, ovarian, liver, kidney and thyroid cancer, we reaffirmed and validated our RADR generated signature as a robust predictive tool to assess sensitivity in tumors.
We have now confirmed that the racemically pure negative isomer of LP-184 is several orders of magnitude superior to the positive enantiomer, while retaining differential toxicity between tumor cells and normal cells.
40
We are in the process of translating the leads generated by our A.I. based in silico analysis to confirm the most optimal drug combinations that would best enhance the efficacy of LP-184 and broaden potential indications of its utility.
The strong antitumor response of LP-184 observed in glioblastoma cell lines, prompted our further assessment of LP-184 as a candidate for glioblastoma and other CNS tumors. Since CNS tumor effective agents require the ability to cross the blood brain barrier (BBB), we used in silico analysis to determine the potential of LP-184 to penetrate BBB. Positive results from such analysis led us to partner with a CRO to validate the ability of LP-184 to cross the BBB in a multicellular in vitro model. Based on this research, we believe LP-184 is as efficacious as the standard of care Temozolomide in penetrating the BBB. These data have now led to a strategic collaboration with investigators at The Kennedy Krieger Institute, an affiliate of the Johns Hopkins School of Medicine.
Strategic Academic Collaborations for LP-184
We are or have been involved in the following academic collaborations for LP-184:
| ● | Georgetown University. We have entered into the second phase of our collaboration with Georgetown University. In the first phase, we confirmed the efficacy of LP-184 in a panel of prostate cancer organoid models. In the second phase, we will focus on wet lab validation of the leads generated by our A.I. models of the gene dependency of most sensitive prostate cancers. This project is intended to provide necessary experimental data for use of LP-184 in a personalized medicine approach to treating prostate cancer. Our gene correlation data has highlighted the deficiency of several pathways that hypothetically would allow LP-184 to be synthetically lethal in tumors with such disruptions. Our RADR analysis also indicates that as many as 20% of prostate cancers carry markers that will make these tumors highly sensitive to LP1-84. In Phase 2 or our collaboration with Georgetown, we are focusing on the development of gene specific isogenic engineered prostate cancer cell lines to dissect the pathways as well as extend the 2D and 3D prostate cancer studies to in vivo genomically defined prostate cancer PDXs. In addition, we have designed studies that will test LP-184 in combination with several other drugs that are known to inhibit pathways needed to repair damage to DNA caused by LP-184. The advantage of combining our DNA damaging agent along with a DNA damage repair inhibitor is that it is expected to substantially extend the tumor specific efficacy of LP-184, including prostate cancers that might otherwise not carry deficiencies in the DNA repair pathway. We expect that the drug sensitivity data and genomic data from these studies will further guide optimal positioning of LP-184. |
| ● | Memorial Sloan Kettering Cancer Center. We collaborated with the Memorial Sloan Kettering Cancer Center to evaluate LP-184 efficacy in preclinical models of cancer with defective DNA damage repair backgrounds, specifically ERCC3 mutations that are relatively common in hereditary breast and ovarian cancers. This study helped us in our efforts to (i) identify biomarkers (genomic, transcriptomic and/ or proteomic) associated with transcription-coupled nucleotide excision repair (TC-NER), the DNA repair pathway that acylfulvenes are known to target, and (ii) develop strategies for targeting vulnerabilities in this pathway during tumor growth (i.e. identify additional genetic backgrounds in this DNA repair pathway that can act with LP-184 in a synthetically lethal manner to inhibit tumor growth). Evidence from in vitro cell line work provided independent support for our belief in LP-184 anticancer activity in an engineered ERCC3 mutant breast cancer cell line model. The observed growth inhibition in this model fit well with the previously reported sensitivity range for LP-184 in the NCI-60 breast cancer cell line panel. This project provides a foundation to explore hereditary cancers with certain DNA damage repair deficiencies as potential indications for future LP-184 studies. An extrapolation of the results from this collaboration, when linked in the context of recent data and publications and other observations regarding acylfulvene mechanism of action, supports the potential for LP-184 to act as a synthetic lethal agent in tumors that carry mutations in ERCC3. |
41
| ● | The Research Institute of Fox Chase Cancer Center (“FCCC”). Our ongoing collaboration with FCCC has yielded results that strongly link LP-184 efficacy to the expression of PTGR1. PTGR1 was identified by our RADR analysis as the lead gene candidate, the expression of which is essential to LP-184 mediated cytotoxicity. Using CRISPR engineered cells, we have now demonstrated a total lack of activity in tumor cell lines where PTGR1 expression is artificially knocked out. These data continue to support our RADR based predictions and the strategies of using LP-184 for tumor indications based upon PTGR1 expression. Our RADR analysis has identified a multitude of tumors with a higher than required threshold of PTGR1 expression. We have further validated the activity of LP-184 in a panel of pancreatic cancer cell lines. Studies to evaluate the efficacy of LP-184 in pancreatic cancer PDX models and in xenografts are ongoing. Our intent is to use the results from these studies to support our filing for orphan drug designation for LP-184 for use in pancreatic cancers. |
| ● | Kennedy Krieger Institute and the Johns Hopkins Sidney Kimmel Comprehensive Cancer Center. We have initiated a new collaboration with Kennedy Krieger Institute and investigators at the Johns Hopkins School of Medicine. We sought this collaboration following multiple unique findings regarding LP-184, including: the efficacy of LP-184 in glioblastoma (GBM); a positive result suggesting the ability of LP-184 to penetrate the Blood Brain Barrier, in amounts similar to the GBM standard of care agent Temozolomide (TMZ); and LP-184’s special ability to kill GBM cells irrespective of the methylation status of MGMT promoter. We believe there is an urgent unmet need for an effective therapy to treat GBM with unmethylated MGMT. Both wet lab data and RADR based gene correlations highlighted sensitivity of tumor cells that carry unmethylated MGMT to LP-184. We will seek to obtain additional data in an expanded panel of GBM tumor cell lines, neurospheres obtained from patient biopsies and evaluation of LP-184 in GBM xenografts in order to support an orphan drug designation for LP-184 for GBM. Early results from this collaboration continue to support the cytotoxicity of LP-184 in both GBM cell lines and neurospheres. Additional GBM in vivo studies involving animal xenografts are expected to be completed in the first quarter of 2021. | |
| ● | Clinical Trials and Research Innovation Center in Northern Ireland. In 2019, we initiated a new collaboration with the Clinical Trials and Research Innovation Center in Northern Ireland (“C-TRIC”) on a novel preclinical ex-vivo study focused on determining gene signatures correlated with LP-184 anticancer activity in human fresh prostate tumor tissue biopsies. This study was paused due to the COVID-19 pandemic, including the impracticality of international travel and the reprioritization of projects due to the pandemic. We are collaborating with other studies in the U.S. and will evaluating recommencing the study with C-TRIC as more is learned following the end of the COVID-19 pandemic. |
Ongoing pre-IND Enabling and Planned IND Enabling Animal Studies
We intend to obtain toxicity data on fully synthetically produced (-) and (+) or R and S enantiomeric forms of LP-184 from cell line efficacy studies as well as non-GLP dose range finding studies in rats. We expect to select the enantiomer with the most favorable safety and antitumor profiles for continued analyses and further studies. Enantiomers are molecules that are non-superimposable mirror images of each other. We have planned an animal study to determine the selection of the desired LP-184 enantiomer involving non-GLP dose range finding in rats to compare toxicity of the enantiomers. Pursuant to the planned study, Sprague-Dawley rats will be given intravenous (over 30 min) doses of the two compounds in sterile saline on Days 1 and 8, using a syringe pump or infusion pump. We anticipate that the high dose will cause detectable toxicity to permit comparison between the two (+S) and (-R) enantiomers. Once an enantiomer selection decision is made, we intend to conduct further IND-enabling animal studies involving some or all of the following: (i) non-GLP dose range finding in rats, (ii) GLP analysis of toxicity in rats, (iii) non-GLP dose range finding in dogs, (iv) GLP analysis of toxicity in dogs, (v) LC-MS/MS Method development for the determination of LP-184 levels in Rat and Dog Plasma, (vi) HPLC Method development, (vii) Compatibility study of dose formulations and infusion systems (GLP), and (viii) Hemolytic potential (GLP).
Planned Phase I Clinical Trial for LP-184
Once regulatory clearance has been obtained to move forward under a future IND and subject to any changes or modifications in the IND in response to comments from the FDA, we intend to conduct a Phase I clinical trial to study LP-184 versus placebo in combination with neoadjuvant chemotherapy for the treatment of late stage solid tumors expected to include ovarian, prostate and liver cancer with high expression of the protein coding gene PTGR1 (Prostaglandin Reductase 1). We anticipate that the study will have a duration of 6 to 18 months and be located in a single center or multiple centers. We intend to conduct the study in two phases. In Phase 1A, we intend to perform a dose escalation using a standard 3 + 3 escalation strategy with a primary objective to assess the safety and toxicity profile of LP-184 in patients with solid tumors using the NCI CTCAE v.4.03 and to determine the maximum tolerated dose (MTD). In Phase IB we intend to perform a dose expansion involving treatment with LP-184 at the MTD in patients with metastatic solid tumors, with a primary objective to assess the safety and toxicity profile of LP-184 at the targeted MTD in patients with advanced solid tumors. Further planning and development of secondary objectives and primary and secondary endpoints are in process and will be subject to FDA review and comment.
42
LP-100
General Overview
LP-100 or 6-Hydroxymethylacylfulvene (or irofulven) exploits cancer cells’ deficiency in DNA repair mechanisms. We have out-licensed LP-100 to Allarity Therapeutics. LP-100 is in a phase II clinical trial in androgen receptor (AR)-targeted and Docetaxel-pretreated metastatic castration-resistant prostate cancer (mCRPC) patients. We hold an exclusive license for the development and commercialization of LP-100.
LP-100 shows multiple cytotoxic effects on tumor cell biology such as DNA adduct formation, RNA polymerase stalling and redox protein modification. It demonstrates enhanced sensitivity in DNA repair deficient (e.g. ERCC3 mutant or knockout) in vitro and in vivo models. In historical testing, clinical antitumor activity for LP-100 was observed in approximately 10-12% of patients with multidrug resistant advanced prostate cancer with notable resolution of bone metastases.
History of LP-100
LP-100 belongs to the family of compounds and small molecular entities (molecular weight <330) that represent a class of anticancer agents derived from fungal toxins called Illudins. Acylfulvenes were originally synthesized and developed by Drs. Michael J. Kelner and Trevor C. McMorris at University of California at San Diego (“UCSD”). In 1987, Professor McMorris published the first preclinical evaluation of the Illudins as anticancer agents and a library of hundreds of acylfulvene derivatives was created, many with significant in vitro and in vivo antitumor activity and potentially improved selectivity for tumor cells versus normal cells. The compound Illudin S was found to be highly cytotoxic against cancer cells, but demonstrated a poor therapeutic index. Better understanding of the mechanism of action led to the development of a novel family of semisynthetic antitumor agents, or next-generation acylfulvenes such as 6-hydroxymethylacylfulvene, now designated as LP-100. LP-100 is a semisynthetic derivative of Illudin S, one of a series of sesquiterpene natural products (Illudins) isolated from the Lantern mushroom Omphalotus illudens. LP-100 was selected for further study based on its potential to demonstrate promising antitumor activity while maintaining a more favorable therapeutic index, compared to previously studied Illudins. The chemical structure of LP-100 is depicted below.
LP-100 Chemical Structure

43
Mechanism of Action
LP-100 leads to rapid inhibition of DNA synthesis and induction of DNA damage. LP-100 is a monofunctional covalent DNA binder that inhibits DNA synthesis and replication, affects cell cycle and induces apoptosis. DNA repair of LP-100-induced lesions is mediated by components of the transcription-coupled nucleotide excision repair (TC-NER) pathway. LP-100 produces damage to DNA that can only be repaired by the TC-NER pathway. The DNA damage is unique, as two enzymes, RNA Polymerase III and Topoisomerase I (Topo 1), associated with the TC-NER are displaced leading to irreversible inactivation of the repair pathway. Other conventional DNA damaging chemotherapeutic agents, such as cisplatin, etoposide, doxorubicin and others, produce general damage that can be repaired by the Global Genome Nucleotide Excision Repair (GG-NER) pathway. Tumor cells often develop multidrug resistance (MDR) making them impossible to kill using conventional drugs. LP-100 appears to retain activity against MDR tumor cells regardless of the mechanism of resistance and tumor cells appear less likely to become resistant to LP-100. Killing of MDR tumor cells by LP-100 reflects its unique mechanism of disrupting the TC-NER pathway. Cell-based studies have demonstrated selective cytotoxicity of LP-100 towards a variety of solid tumor cell lines. The tumor cells cannot recover from this damage, undergo S-phase arrest, and then irreversibly initiate both caspase-dependent and –independent apoptosis pathways. LP-100 produces DNA damage and induces apoptotic DNA fragmentation in several tumor cell lines. Normal diploid cells, in contrast, do not normally need repair by the TC-NER pathway unless exposed to UV light. Treatment of mouse xenografts of human tumors with LP-100 results in tumor shrinkage. Synergistic or additive activity is observed when LP-100 is combined with various traditional anticancer agents.
LP-100 acts as a DNA damaging agent by causing alkylation of DNA and adduct formation. It modulates the TC-NER DNA repair pathway further activating the MAPK signaling cascade followed by apoptosis of target cells. Also, LP-100 induces RNA Polymerase II stalling in actively transcribed regions, triggering cell death possibly due to collisions between transcriptional machinery and the replication fork. LP-100 is not a substrate for drug efflux pumps, which helps to counteract chemoresistance to LP-100. Sensitivity to LP-100 is unlikely to be influenced by common resistance-inducing phenomena observed for other DNA damaging agents like cisplatin. Antitumor activity of LP-100 is independent of cellular p53 and p21 tumor suppressor gene status (such as loss of p53 or p21). LP-100 also produces redox protein modifications by targeting key redox-controlling proteins TrxR/ GrxR. Distortion of the redox status of cellular proteins serves as a pro-apoptotic stimulus in cancer cells.
LP-100 Clinical Profile
Clinical studies of LP-100 have been conducted in multiple solid tumor indications including prostate, ovarian, colorectal, pancreatic, thyroid, lung, breast and gastric cancers. More than 38 Phase I or Phase II trials involving > 1,300 patients have been conducted with LP-100. In prior clinical trials, LP-100 showed activity and produced regression in a variety of cancers, but failed to meet required endpoints for clinical trial success. Objective responses were reported for LP-100 single agent therapy in drug-resistant prostate (hormone and taxotere refractory), ovarian (platinum resistant), pancreatic, sarcoma, kidney, endometrial, and lung cancers. LP-100 also showed cancer treating potential when administered in combination with a variety of conventional chemotherapeutics including Camptosar, GemZar, Taxotere, Xeloda, Cisplatin, and Oxaliplatin. In a study of patients who failed prior conventional therapies, two rounds of LP-100 therapy led to rapid resolution of ovarian cancer metastasis. In a randomized Phase IIb study of patients with metastatic hormone refractory taxotere-resistant prostate cancer, LP-100 was compared to mitoxantrone. A total of 138 patients were enrolled and specified endpoints included overall survival, response rate, and safety assessment. The median one-year survival increased from 22% in the mitoxantrone-treated control group to 41% in the LP-100-treated group. Median overall survival was 10.1 months for treatment arm (LP-100 + Prednisone) and 7.4 months for control arm (Mitoxantrone + Prednisone), i.e. a 37% increase over standard of care. Treatment was well-tolerated in all arms. The most frequent Grade 3–4 toxicities (as % of patients in treatment/control arms) were asthenia (8%/0%), and vomiting (4%/0%). Grade 3–4 hematological events included neutropenia (22%/61%) and thrombocytopenia (23%/4%).
In 2001, LP-100 received FDA’s fast track status and a Phase III international clinical trial for LP-100 in refractory pancreatic patients was started. Clinical trials looked promising in shrinking tumors of drug-resistant pancreatic cancer. However, MGI Pharma stopped the Phase III clinical trial because it was unlikely for the trial to reach its objective due to a greater than expected survival benefit associated with the comparator agent (5-FU). In 2005, Phase II clinical trial results of LP-100 in women with recurrent and heavily pre-treated ovarian cancer revealed retinal toxicity. This retinal damage was associated with dose and administration of drug.
44
LP-100 has been well-tolerated, based on initial observations from the phase II clinical trial in Europe that is being managed by Allarity Therapeutics in patients with metastatic, castration-resistant, prostate cancer. This Phase II trial is aimed at evaluating the antitumor effect of LP-100 treatment in combination with Prednisolone in patients who have progressed on androgen receptor (AR)-targeted therapy and in docetaxel-pretreated metastatic Castration-Resistant Prostate Cancer (mCRPC) patients. In this protocol, patients are screened using a LP-100-specific response biomarker signature and eligible patients likely to respond to and benefit from treatment with LP-100 are recruited in the trial. Allarity Therapeutics dosed the first patient in the trial in the fourth quarter of 2018. Continuing enrollment for this Phase II clinical trial has slowed during the COVID-19 pandemic. Allarity Therapeutics has also stated that it is focusing its existing resources on other programs that are currently higher priority for Allarity than LP-100. As of the date of this report, we are unable to forecast the timeline for the completion of the Phase II clinical trial. Recently published data (also supported by prior publications on (Irofulven) indicates that tumors carrying mutations in ERCC2 and ERCC3 genes are likely to be sensitive to LP-100, and that the drug will be synthetically lethal in these tumors, in a fashion similar to the activity of PARP inhibitors in BRCA deficient tumors. These observations expand the potential treatment indications for LP-100 to include urothelial tumors, including bladder cancers, since as many as 10% of bladder cancers carry ERCC2/ERCC3 mutations. These indications may represent a more rapid and efficient path to potential approval of LP-100, and we are evaluating possibilities aimed at maximizing the value of these additional observations.
AF Chemicals
In January 2015, we entered into a Technology License Agreement to exclusively license global patent rights from AF Chemicals, LLC (“AF Chemicals”) for the treatment of cancer in humans for the compounds LP-100 (Irofulven) and LP-184. In February 2016, we and AF Chemicals entered into an Addendum (the “Addendum”) providing for additions and amendments to the Technology License Agreement. In December 2020, we and AF Chemicals entered into a Second Addendum (the “Second Addendum”) providing for further additions and amendments to the Technology License Agreement. The Technology License Agreement, Addendum and Second Addendum are collectively referred to as the “AFC License Agreement”.
The Second Addendum provides for us to make specified payments to AF Chemicals within 10 days after signing and by March 31, 2021. The Second Addendum also provides that, from December 30, 2020 until January 15, 2025, we will have no obligation to pay annual licensing fees, development diligence extension payments, or patent maintenance fee payments to AFC under the AFC License Agreement.
As part of the Second Addendum, we have agreed to apply for specified orphan drug designations for LP-184 in the US and EU. The Second Addendum also amends and clarifies other provisions of the Technology License Agreement, and provides us with the ability to recover a portion of initial payments made under the Second Addendum from sublicense fees or royalty payments that may be made to AFC by us or third parties prior to January 15, 2025.
Pursuant to the AFC License Agreement we made annual licensing fee payments relating to LP-184 to AF Chemicals in the amount of $30,000 during each of the years ended December 31, 2020 and 2019. In addition, we are obligated to make milestone payments to AF Chemicals at the time of an Investigational New Drug Application (“IND”) filing relating to LP-184 and also upon reaching additional specified milestones in connection with the development and potential marketing approval of LP-184 in the United States, specified countries in Europe, and other countries. We estimate that these payments could be as much as approximately $3,780,000 if all milestones were achieved and LP-184 obtained marketing approval in multiple countries and for multiple therapeutic indications.
In the event of a sublicense of the LP-184 rights, we are obligated to pay AF Chemicals (a) low double digit percentage of the gross income and fees received by us with respect to the United States in connection with such sublicense, and (b) a lower double digit percentage of the gross income and fees received by us with respect to Europe and Japan in connection with such sublicense. We are obligated to pay royalties under the AFC License Agreement for a term that expires upon the later of the expiration of the last patent licensed to us under the agreement, and the last to expire orphan drug designation, if any, relating to our product candidate LP-184 or other specified licensed technology under the agreement.
45
The AFC License Agreement also provides that we will pay AF Chemicals a royalty of at least very small single digit percentage of specified net sales of LP-184 and other analogs. In addition, the AFC License Agreement contains specified time requirements for us to file an IND, enroll patients in clinical trials, and file a potential NDA with respect to LP-184, with the ability for us to pay AF Chemicals additional amounts ranging up to an amount in the low hundreds of thousands of dollars for each one, two, three and four year extension to such development time requirements, with additional extensions beyond four years to be negotiated by us and AF Chemicals. Pursuant to the Second Addendum, no additional payments of annual licensing fees or development diligence extension payments are required to be made by us until January 15, 2025, at which time these obligations will resume. We will also be obligated to make annual licensing fee payments to AF Chemicals relating to LP-100 beginning January 15, 2025, as described below under Allarity Therapeutics.
The AFC License Agreement has a term that expires upon the later of the expiration of the last patent licensed to us under the agreement, and the last to expire orphan drug designation, if any, relating to our product candidate LP-184 or other specified licensed technology under the agreement, unless sooner terminated. The AFC License Agreement may be sooner terminated by AF Chemicals if we fail to make any payments required to be made under the agreement when due, upon a material breach of any other provision of the agreement that is not cured within the time period specified, and upon our bankruptcy or insolvency.
Allarity Therapeutics
Allarity Therapeutics has begun a Phase II trial of Irofulven in Denmark. With Allarity Therapeutics, we won a joint Massachusetts-Denmark grant to provide matching funds for production of LP-100 in Massachusetts and clinical studies in Denmark. The clinical studies utilize Allarity Therapeutics’ proprietary DRP® biomarker screening of potential patients to select those most likely to respond to the drug.
With our help, Allarity Therapeutics has had cGMP LP-100 produced at Albany Molecular Research Inc., PCI Synthesis, a division of SEQENS CDMO and Piramal Pharma Solutions (Lexington, KY USA). Allarity Therapeutics has used a proprietary DRP® bioinformatics approach to identify putative biomarkers that can predict which patients will respond based on gene expression profiles. Allarity Therapeutics started a Phase II clinical trial in Denmark for treatment of castration-resistant metastatic prostate cancer, with the first patient enrolled in the fourth quarter of 2018. The trial is over half way through enrollment for the first stage of the trial, although enrollment has slowed during the COVID-19 pandemic. The trial is estimated to enroll up to approximately 27 patients. If the study has a successful outcome, we anticipate that Allarity Therapeutics may out-license the drug.
Allarity Therapeutics Drug License and Development Agreement
In May 2015, we licensed various rights to LP-100 (Irofulven) to Allarity Therapeutics pursuant to a drug license and development agreement.
Pursuant to the agreement, Allarity Therapeutics is responsible for the development of LP-100 pursuant to a defined clinical development plan. The agreement also provides for a joint development committee, including representatives from Allarity Therapeutics and us, to regularly discuss, plan and inform the development of products under the agreement. In connection with the license under the agreement, Allarity Therapeutics also agreed to directly pay to AF Chemicals on our behalf various specified amounts owed to AF Chemicals with respect to LP-100 under the AFC License Agreement, which amounts will then be deducted from payments to be made by Allarity Therapeutics to us.
Development Milestone Payments
Pursuant to the agreement, Allarity Therapeutics has agreed to make milestone payments to us in connection with the development of LP-100 by Allarity Therapeutics or its affiliates, or by a third party (a “Program Acquirer”) that assumes control of the LP-100 development program from Allarity Therapeutics corresponding to: (i) initiation of treatment of first patient in a Phase III clinical trial; (ii) first filing for regulatory approval in the EU; (iii) first filing for regulatory approval in the US; (iv) first regulatory approval in the EU; and (v) first regulatory approval in the US. We and Allarity Therapeutics have also agreed that a portion of these milestone payments will be paid directly to AF Chemicals to satisfy our obligations under the AFC License Agreement.
46
The above milestones to be paid to us under the agreement are also subject to caps and floors providing that: the development milestones discussed above for initiation of Phase III treatment and for the first filing for regulatory approval in the EU and the US shall not be less than a specified percentage of the amount Allarity Therapeutics receives from a Program Acquirer upon the occurrence of a substantially similar milestone; and the development milestones discussed above for first regulatory approval in the EU and the US shall not be greater than a specified percentage of the amount Allarity Therapeutics receives from a Program Acquirer upon the occurrence of a substantially similar milestone. With certain exceptions, the maximum aggregate amount of development milestone payments described above to be paid by Allarity Therapeutics to us is $13,875,000 and to AF Chemicals is $7,125,000 for an aggregate total of $21,000,000.
In addition to the above milestones, Allarity Therapeutics has agreed to pay us a specified percentage of any milestone payments Allarity Therapeutics receives from a Program Acquirer that are different than the milestones described above, or a one-time payment in an amount in the low seven figures, whichever is higher. AF Chemicals would also receive a portion of any amounts to be received by us pursuant to this provision. The Allarity Therapeutics agreement also provides that development milestone payments (including the payments described above) will be paid not more than once even if additional indications are developed for LP-100.
Alternate Payment Structure in Event of Third Party Program Acquirer Agreement.
As an alternative to the development milestone payments to be paid as discussed above, and without the $21 million payment limitation, Allarity Therapeutics has agreed that we may select an alternate payment structure for all payments Allarity Therapeutics receives (other than royalty payments which are described below) in the event Allarity Therapeutics enters into an agreement for LP-100 with a Program Acquirer regarding a particular territory. We only have 15 days to make this selection from the date we receive notice from Allarity Therapeutics that they have entered into an agreement with a Program Acquirer.
If we select the alternate payment structure, then we would generally be entitled to receive a specified percentage of all amounts, other than royalty payments, received by or on behalf of Allarity Therapeutics from the Program Acquirer, after subtraction of amounts paid or payable by Allarity Therapeutics pursuant to the Program Acquirer agreement for taxes, other fees and payments to governmental authorities, and payments made by the Program Acquirer to reimburse Allarity Therapeutics’ regulatory and other costs. Selection of the alternate payment structure would not change our right to receive royalty payments from Allarity Therapeutics as described below. We have agreed to obtain the consent of AF Chemicals prior to electing to receive payments pursuant to the alternate payment structure and no assurances can be given that AF Chemicals would provide their consent.
Royalty Payments
In addition to the milestone payments described above, Allarity Therapeutics has agreed to pay us royalties based on annual incremental sales of product derived from LP-100 in an amount equal to a low single digit percentage of annual sales of between $0 and $50 million, a slightly higher single digit percentage of annual sales between $50 million and $150 million, a mid-level single digit percentage of annual sales between $150 million and $300 million, and a slightly higher mid-level single digit percentage of annual sales in excess of $300 million.
Royalties are subject to a cap of a specified percentage of any royalty payment Allarity Therapeutics receives from a Program Acquirer. The royalty amounts to be received by us may be subject to reduction in the event of generic competition, patent expiry, or if additional third-party licenses are required to be obtained for the development, use or commercialization of LP-100. Royalties will generally be received on a country by country basis until the later of: expiration of an applicable patent in a particular country; 10 years after the first commercial sale in the country; expiration of the last to expire valid claim of a relevant patent covering the LP-100 related product together with the use of the DRP® biomarker, provided the product is approved only for use with the DRP biomarker in the country; or expiration of any FDA (or any foreign equivalent) regulatory approval in each country that requires use of the DRP® biomarker as a companion diagnostic for the relevant product.
47
Allarity Therapeutics is obligated to pay royalties under the agreement on a country-by-country and product-by-product basis for a period that commences with the first commercial sale of a product until the later of (i) the expiration of the last valid claim on the patent that covers the product sold, or (ii) ten years after the first commercial sale of the covered product, or (iii) expiration of the last valid claim covered by a patent using a DRP® Biomarker as a companion diagnostic to the product sold, or (iv) on a country-by-country basis when the regulatory approval of the DRP® Biomarker as a companion diagnostic expires. However, the agreement may be sooner terminated without cause by Allarity Therapeutics upon 120 days prior written notice, or immediately upon certain regulatory actions that impede ongoing or future clinical trials, or upon written notice of a material breach of the agreement by us that we do not cure within 60 days. We also have the right to terminate the agreement upon written notice of a material breach of the agreement by Allarity Therapeutics that is not cured within 60 days.
Third Party Research and Development Programs for Our Drug Candidates
Virtually all of our developmental work is expected to be performed in contract labs in the near future, and most of it requires close collaboration with these groups. Our strategic collaborations have specialized focus areas tailored to advancing our pipeline drug candidates and provide expertise benefits.
| Collaborator | Focus Area | Drug Candidate | ||
| National Cancer Institute (NCI) | Gene signature development and drug sensitivity prediction | LP-184 | ||
| Georgetown University | Evaluation of drug efficacy and sensitivity in prostate and pancreatic cancer organoid models and engineered pancreatic cancer cell lines | LP-184 | ||
| Fox Chase Cancer Center (FCCC) | Determination of drug efficacy in PDX tumor models | LP-300 & LP-184 |
Manufacturing Overview
We do not currently own or operate any manufacturing facilities or have any manufacturing personnel. We currently rely, and expect to continue to rely, on third party contract manufacturing organizations (“CMOs”) for the manufacturing of our drug candidates for preclinical uses, clinical trials as well as for commercial manufacturing if our drug candidates receive marketing approval. We require that our CMOs produce bulk drug substances and finished drug products in accordance with current Good Manufacturing Practices (“cGMPs”) and all other applicable laws and regulations. We maintain agreements with our manufacturers that include confidentiality and intellectual property provisions to protect our proprietary rights related to our drug candidates. We have a CMO contracted to manufacture LP-184 for preclinical use. We obtain our supplies from these CMOs on a purchase order basis and do not have long-term supply arrangements in place. We do not currently have arrangements in place for redundant supply. For all of our drug candidates, we intend to identify and qualify additional manufacturers to provide the active pharmaceutical ingredient and fill-and-finish services prior to seeking regulatory approval.
LP-184 Manufacturing
We have contracted to Southwest Research Institute® (“SwRI®”) the development of a fully synthetic route to (-) and (+) LP-184. The synthesis process involves development and optimization of novel chemistry via multiple intermediates to produce (-) and (+) enantiomers of LP-184. We have contracted to SwRI® the production of pre-GMP batch of the desired enantiomer of fully synthetic LP-184. We intend to continue with the same supplier for manufacturing the GMP material intended for IND-enabling animal studies as well as phase I clinical trials.
LP-300 Manufacturing Plans
For the supply of LP-300 for our phase II and/or III clinical program, we have identified potential CMOs, and we believe GMP grade API material will be readily available. We have contracted with Patheon API Services, Inc., a division of Thermo Fisher Scientific, Inc., to manufacture a sufficient quantity of the active pharmaceutical ingredient for LP-300 to conduct a phase II trial. Our manufacturing process and protocol for LP-300 have been well established and substantial progress towards process validation has been made from previous campaigns that were undertaken by BioNumerik Pharmaceuticals, Inc.
48
Commercialization
We retain worldwide commercialization rights for our key candidates with the exception of LP-100, which we have out-licensed to Allarity Therapeutics. We plan to continue considering out-license and collaboration opportunities in order to maximize returns and pursue successful development of our key candidates. We currently have no sales, marketing or product distribution capabilities. However, once we have key candidates closer to FDA approval, we may build our own specialty sales force, partner with a larger pharmaceutical organization, or out-license our drug candidates.
We are continually evaluating out-license opportunities for our candidates at later stages of development in order to focus on identifying and licensing additional drug candidates for novel indications and/or patient subpopulations with an oncology focus for expansion of our pipeline.
Our commercial plans and strategy for each particular program may change as our programs advance, the markets change, we receive more clinical data, and depending on availability of capital.
Intellectual Property
We have an extensive multi-national portfolio of intellectual property rights directed to our drug candidates, and their targeted use and development in specific patient populations and in specific therapeutic indications.
As of the date of this report, we own or control rights in over 70 active patents and patent applications across over 14 patent families whose claims are directed to our drug candidates and what we plan to do with our drug candidates. We have in-licensed or acquired patents from AF Chemicals, and BioNumerik directed to the compounds, LP-100, LP-184 and LP-300. Additionally, we have also filed patent applications to further enhance and extend the use of these in-licensed compounds. Our patents are directed to our drug candidates, their usage, manufacturing, and other matters. These matters are essential to precision oncology and relate to: (a) uniquely powerful, data-driven, biologically relevant biomarker signatures, (b) patient selection and stratification approaches that rely on prediction of response deriving from these signatures and, (c) the ability to develop novel, combination therapy approaches with existing approved therapeutics. A recent application is directed to the use of LP-300 as a potential disulfide linker. We intend to pursue additional patent coverage relating to the use of LP-300 as a potential linker or linking technology.
We rely on a combination of patents, trade secrets, copyrights, trademarks, license agreements, nondisclosure and other contractual provisions and technical measures to protect our intellectual property rights in our novel drug candidates as well as our rescue drug candidates. Additionally, we also rely on the patent applications, trade secrets, and other contractual provisions and technical measures to protect the development of our genomic and biomarker signatures that help us in making predictions about the sensitivity to our drug candidates, patient stratification approaches, and the development of potential combination therapies with our drug candidates.
Intellectual Property Portfolio by the Numbers
As of March 2021, our intellectual property portfolio consisted of over 14 patent families covered by:
| ● | Over 50 issued patents across our portfolio of compounds in key, commercially important geographies; |
| ● | Over 20 pending patent applications, including three PCT applications; |
| ● | as well as two registered trademarks, two pending trademark registrations, and trademark applications in Japan, China, Europe, Canada and Australia. |
Our policy is to protect the proprietary technologies, inventions, and improvements that are commercially important to our business in the United States, Europe, Japan and other key jurisdictions important to our business. We fully expect that additional advances will come out of our ongoing work in developing biomarker signatures and patient stratification approaches and that these advances will form the basis of additional intellectual property protection through new patent filings, trademarks, trade secrets, and copyrights. We will continue to file patent applications and use trade secret laws to protect the uses of our genomic and biomarker signatures, response prediction and patient stratification discoveries. We plan to rely on these intellectual property advances to develop, strengthen, and maintain our proprietary position for novel therapeutics and novel formulations and uses of existing and new compounds across multiple therapeutic areas. We also plan to rely on data exclusivity, market exclusivity and patent term extensions when available.
49
Patent Portfolio
We have an extensive multi-national portfolio of intellectual property rights directed to our drug candidates, and their targeted use and development in specific patient populations and in specific therapeutic indications. Our portfolio consists of 14 patent families across issued patents and pending patent applications. For LP-100, we own and control two in-licensed patent families, including issued US Patents, Japan Patents, and various issued EU Patents directed to LP-100. We have also filed seven patent applications directed to our proprietary drug programs together with biomarkers and sensitivity parameters, two of which are being consolidated into one application, and one additional patent application directed to our RADR® platform. These filings include patent applications directed to LP-300 and additional patent applications directed to new manufacturing methods for novel, synthetic illudins, and gene signatures and biomarker profiles indicating sensitivity to LP-184 and use of LP-184 and novel synthetic illudins in glioblastoma and CNS cancers.
| ● | Our patent family directed to LP-100 has patents that expire in August 2026. |
| ● | Our patent family directed to LP-184 has patents that expire in August 2026, and patent applications, if granted, that would expire as late as May 2040. |
| ● | Our patent family directed to LP-300 has patents that expire in March 2028, and patent applications, if granted, that would expire as late as March 2040. |
We typically file a non-provisional patent application within 12 months of filing the corresponding provisional patent application. While we intend to timely file non-provisional patent applications relating to our provisional patent applications, we cannot predict whether any of our existing or future patent applications for our existing or future drug candidates will result in the issuance of patents that effectively protect these candidates, or if any of our issued patents or if any of our licensor’s issued patents will effectively prevent others from commercializing competitive products. Patent protection for the composition of matter of the LP-300 compound itself is unavailable because the compound was first identified many years ago. For more information regarding the risks related to our intellectual property, see “Risk Factors – Risks Related to Our Intellectual Property.”
RADR® Platform
We do not own or in-license any patents on our RADR® platform, but we have filed one patent application directed to our RADR® platform and rely on trade secrets and confidential procedures directed to protecting:
| ● | our A.I. and machine learning methodologies for our specific purposes in oncology drug development and drug rescue, |
| ● | our curation and normalization of select data from both public and proprietary data sources, and |
| ● | our developing insights that can be modeled to cover biological processes as algorithms inside our RADR® platform. |
LP-100
Our portfolio directed to LP-100 consists of two families of in-licensed patents that were filed in 2006. The patents include European, Japanese and US patents. US Patent No. 7655695 relates to acylfulvene analogs that are directed to tumor solid tumor growth inhibition. The nominal expiration for our patents directed to LP-100 is August 2026 and does not account for any applicable patent term adjustments or extensions.
50
LP-184& other Novel, Synthetic Illudin Derivatives
Our portfolio directed to LP-184 consists of six families of patents and patent applications and includes three PCT applications. US Patent No. 7655695 relates to acylfulvene analogs that are directed to solid tumor growth inhibition. The PCT applications filed in 2019 are related to synthetic preparation methods, additional indications, and treatment of cancers using genomic stratification. A provisional patent application filed in 2020 was directed to using LP-184 or other novel, synthetic illudin analogs or deriviatives to treat glioblastoma or other CNS cancers as either a mono or combination therapy. A provisional patent application filed in 2020 was directed to using LP-184 or other novel, synthetic illudin analogs or derivatives to treat pancreatic cancer also as either a mono or combination therapy. The nominal expiration for patents and patent applications directed to LP-184 ranges from 2026 to as late as 2040 and does not account for any applicable patent term adjustments or extensions. We intend to nationalize our patent applications in the US, Canada, EU, China, and Japan.
We have in-licensed patents from AF Chemicals related to the composition of matter of LP-184. We have also developed additional intellectual property for this class of compounds related to the development of novel synthetic routes and the preparation of certain illudin derivatives having therapeutic value. Additionally, in April of 2020, we filed a provisional patent on the use of LP-184 and these novel synthetic illudin derivatives in the treatment of glioblastoma and other CNS cancers.
LP-300
Our portfolio directed to LP-300 consists of seven families of owned patents. A more recent PCT patent application filed in 2020 is directed to treatment of non-small cell lung cancer (NSCLC) in nonsmokers and never smoking patients using disodium 2,2’-dithio-bis-ethane sulfonate (dimensa). The nominal expiration for NSCLC related patents and patent applications directed to LP-300 ranges from 2028 to as late as 2040 and does not account for any applicable patent term adjustments or extensions. We intend to nationalize our patent applications in the US, Canada, EU, China, and Japan.
We filed an additional PCT application in March 2020 directed to LP-300 and its application to NSCLC, as well as biomarkers that correlate to heightened response or sensitivity to LP-300. A recent application is directed to the use of LP-300 as a potential disulfide linker.
Confidentiality & Trade Secrecy
Although we enter into non-disclosure and confidentiality agreements with parties who have access to confidential or patentable aspects of our research and development output, such as our employees, collaborators, contract research organizations, contract manufacturers, consultants, advisors and other third parties, any of these parties may breach the agreements and disclose such output before a patent application is filed, thereby jeopardizing our ability to seek patent protection. These agreements provide that all confidential information developed or made known during the course of an individual or entities’ relationship with us must be kept confidential during and after the relationship. These agreements also provide that all inventions resulting from work performed for us or relating to our business and conceived or completed during the period of employment or assignment, as applicable, shall be our exclusive property. Third parties may also be able to develop substantially equivalent proprietary information, platforms or compounds, or otherwise gain access to our trade secret
Trademarks
We own various trademarks, applications and unregistered trademarks in the United States and other commercially important markets, including our company name, our A.I. platform, and certain compounds in development. Our trademark portfolio is designed to protect the brands for our Company, our A.I. platform and our portfolio of compounds.
51
Other Intellectual Property
We believe that our intellectual property rights on the RADR® platform are valuable and important to our business. We rely on a combination of trademarks, copyrights, trade secrets, license agreements, confidentiality procedures, non-disclosure agreements, employee disclosure, and invention assignment agreements, and other legal and contractual rights to establish and protect our proprietary rights.
Competition
We exist at the intersection of rapidly moving, global industries, namely, the biotechnology industry and the A.I. drug development industry. This is a unique and rapidly moving category with a variety of business models being developed globally. The pharmaceutical and biotechnology industries are characterized by rapidly advancing technologies, intense competition and a strong emphasis on intellectual property. A.I. is disrupting and changing all industries, including the biotechnology industry. Although these are competitive industries, we believe we are uniquely positioned due to our focus on oncology drug development, prediction of patient response, use of computational biology, and the ability to both rescue and develop compounds.
We face potential competition from many different sources, including major pharmaceutical and biotechnology companies, academic institutions and governmental agencies, and public and private research institutions.
Many of the companies against which we may compete have significantly greater financial resources and expertise in research and development, manufacturing, preclinical studies, conducting clinical trials, obtaining regulatory approvals and marketing approved products than we do. Smaller or early-stage companies may also prove to be significant competitors, particularly through collaborative arrangements with large and established companies. Mergers and acquisitions in the pharmaceutical, biotechnology and diagnostic industries may result in even more resources being concentrated among a smaller number of our competitors. These competitors also compete with us in recruiting and retaining qualified scientific and management personnel and establishing clinical trial sites and patient registration for clinical trials, as well as in acquiring technologies complementary to, or necessary for, our programs.
Our commercial opportunity could be reduced or eliminated if our competitors develop and commercialize medicines that are safer, more effective, have fewer or less severe side effects, and are more convenient or less expensive than any medicines we may develop. Our competitors also may obtain FDA or other regulatory approval for their medicines more rapidly than we may obtain approval for ours, which could result in our competitors establishing a strong market position before we are able to enter the market. In addition, our ability to compete may be affected in many cases by insurers or other third-party payors seeking to encourage the use of generic medicines.
Any drug candidates we successfully develop will compete with current and new therapies that may become available in the future. The key competitive factors affecting the success of all of our drug candidates, if approved, are likely to be their efficacy, combinability, safety profile, convenience, cost, the effectiveness of companion diagnostics in guiding the use of related therapeutics, if any, the level of generic competition, level of promotional activity, intellectual property protection, and the availability of reimbursement from government and other third-party payors. If any drug candidates under development are approved for the indications in which we are currently planning clinical trials, they will compete with the drugs discussed below and will likely compete with other drugs in development.
Artificial Intelligence and Drug Development
We believe our proprietary RADR® platform gives us a significant competitive advantage by using AI to select and license drugs with a well-tolerated safety profile to quickly and cost-effectively bring drugs to market. Recently, there has been an increase in the use of AI for drug development that we face competition in both for developing new drugs and in biomarker development. This includes competition to the pool of already existing drug candidates that may be eligible for patient stratification. Our competition in AI-driven drug development for oncology includes, but is not limited to, the following:
| ● | Development of drug candidates: A2A Pharmaceuticals, AI Therapeutics, Atomwise, Benevolent AI, Berg Health, BioXcel, Celsius Therapeutics, Exscientia, Gritstone Oncology, Deep Genomics; and |
| ● | Development of biomarkers and/or signatures for patient stratification and improved drug development: Adaptive Biotechnologies, Concerto HealthAI, Datavant, Envisagenics, Erasca, and Genialis,. |
52
Prostate Cancer
New agents are being actively developed to treat specific subtypes of prostate cancer. Our approach is to leverage A.I. and biomarker data to discover subtypes of prostate cancer and treatments for those subtypes of cancer. We believe our approach and our compounds take advantage of this improved characterization of prostate cancer.
There are approved standard of care agents for treating solid tumor prostate cancer, but there are a lack of approved therapeutic options for non-metastatic castration-resistant prostate cancer (“nmCRPC”) patients and castration-resistant disease in metastatic hormone-naïve prostate cancer (“mHNPC”). The competition we may face in regards to LP-100 and one of the indications of LP-184, specifically mCRPC, includes without limitation the following drugs:
| ● | Astellas/Pfizer’s Xtandi (enzalutamide) and Johnson & Johnson’s Zytiga (abiraterone acetate) and Clovis Oncology’s Rubraca (rucaparib) are approved for treatment of metastatic castration-resistant prostate cancer (mCRPC). |
| ● | Xtandi Zytiga and Androgen Deprivation Therapy (“ADT”) to treat mHNPC and nmCRPC, respectively. |
| ● | Pfizer has tested Talazoparib and Enzalutamide to treat mCRPC |
| ● | BeiGene has used Pamiparib treat mCRPC |
| ● | Millennium Pharmaceuticals has used ADT and TAK-700, a hormonal therapy that inhibits 17,20 lyase activity of the CYP17A1 enzyme, to treat Metastatic Prostate Cancer |
We believe LP-184 is unique and it has promise for use in an expanded set of proposed indications including ovarian cancer and hepatocellular carcinoma and other indications where specific biomarker profiles indicate likely sensitivity to the treatment. We are not aware of any drugs in development or approved that are specifically addressing this range of proposed biomarker profile targeted indications.
Non Small Cell Lung Cancer (NSCLC)
We believe LP-300 may have an advantage to approved drugs on the market by serving as a well-tolerated agent in combination with multiple existing standards of care drugs for the NSCLC patient population or female NSCLC patient population. LP-300 has shown potential to alleviate adverse events associated with approved chemotherapeutics such as cisplatin and paclitaxel while also potentiating their antitumor activities. LP-300 combined with cisplatin and/or paclitaxel has the potential to treat never-smoking NSCLC patients with advanced adenocarcinoma. Due to its multi-modal mechanism of action and tolerability, LP-300 has the potential to be combined with chemotherapy, targeted therapy and / or immunotherapy drugs. Beyond traditional chemotherapies, NSCLC treatments include targeted small molecules and biologics, which include, without limitation, afatinib, brigatinib, ceritinib, crizotinib, pembrolizumab, and ramucirumab that are used in specific NSCLC subtypes.
Government Regulation
Government authorities in the United States at the federal, state and local level and in other countries regulate, among other things, the research, development, testing, manufacture, quality control, approval, labeling, packaging, storage, record-keeping, promotion, advertising, distribution, post-approval monitoring and reporting, marketing and export and import of drug and biological products. Generally, before a new drug can be marketed, considerable data demonstrating its quality, safety and efficacy must be obtained, organized into a format specific for each regulatory authority, submitted for review and approved by the regulatory authority.
53
U.S. Drug Development
In the United States, the FDA regulates drugs under the Food, Drug, and Cosmetic Act (“FDCA”). Drugs also are subject to other federal, state and local statutes and regulations. The process of obtaining regulatory approvals and the subsequent compliance with appropriate federal, state, local and foreign statutes and regulations requires the expenditure of substantial time and financial resources. Failure to comply with the applicable U.S. requirements at any time during the product development process, approval process or post-market may subject an applicant to administrative or judicial sanctions. These sanctions could include, among other actions, the FDA’s refusal to approve pending applications, withdrawal of an approval, a clinical hold, untitled or warning letters, product recalls or market withdrawals, product seizures, total or partial suspension of production or distribution, injunctions, fines, refusals of government contracts, restitution, disgorgement and civil or criminal penalties. Any agency or judicial enforcement action could have a material adverse effect on us.
Our drug candidates are considered small molecule drugs and must be approved by the FDA through the NDA process before they may be legally marketed in the United States. The process generally involves the following:
| ● | completion of extensive preclinical studies in accordance with applicable regulations; |
| ● | submission to the FDA of an IND, which must become effective before human clinical trials may begin; |
| ● | approval by an independent institutional review board (“IRB”), or ethics committee at each clinical trial site before each trial may be initiated; |
| ● | performance of adequate and well-controlled human clinical trials in accordance with applicable IND regulations, good clinical practice (“GCP”), requirements and other clinical trial-related regulations to establish substantial evidence of the safety and efficacy of the investigational product for each proposed indication; |
| ● | submission to the FDA of an NDA; |
| ● | a determination by the FDA within 60 days of its receipt of an NDA to accept the filing for review; |
| ● | satisfactory completion of a FDA pre-approval inspection of the manufacturing facility or facilities where the drug will be produced to assess compliance with cGMP, requirements to assure that the facilities, methods and controls are adequate to preserve the drug or biologic’s identity, strength, quality and purity; | |
| ● | potential FDA audit of the preclinical study and/or clinical trial sites that generated the data in support of the NDA filing; | |
| ● | FDA review and approval of the NDA, including consideration of the views of any FDA advisory committee, prior to any commercial marketing or sale of the drug in the United States; and | |
| ● | compliance with any post-approval requirements, including the potential requirement to implement a Risk Evaluation and Mitigation Strategy (“REMS”), and the potential requirement to conduct post-approval studies. |
The data required to support an NDA are generated in two distinct developmental stages: preclinical studies and clinical trials. The preclinical and clinical testing and approval process requires substantial time, effort and financial resources, and we cannot be certain that any approvals for any future drug candidates will be granted on a timely basis, or at all.
Preclinical Studies and IND
Preclinical studies generally involve laboratory evaluations of drug chemistry, formulation and stability, as well as studies to evaluate toxicity in animals, which support subsequent clinical testing. The sponsor must submit the results of the preclinical studies, together with manufacturing information, analytical data, any available clinical data or literature and a proposed clinical protocol, to the FDA as part of the IND. An IND is a request for authorization from the FDA to administer an investigational product to humans, and must become effective before human clinical trials may begin.
54
Preclinical studies include laboratory evaluation of product chemistry and formulation, as well as in vitro and animal studies to assess the potential for adverse events and in some cases to establish a rationale for therapeutic use. The conduct of preclinical studies is subject to federal regulations and requirements, including GLP regulations for safety/toxicology studies. An IND sponsor must submit the results of the preclinical tests, together with manufacturing information, analytical data, any available clinical data or literature and plans for clinical studies, among other things, to the FDA as part of an IND. Some long-term preclinical testing, such as animal tests of reproductive adverse events and carcinogenicity, may continue after the IND is submitted. An IND automatically becomes effective 30 days after receipt by the FDA, unless before that time the FDA raises concerns or questions related to one or more proposed clinical trials and places the trial on clinical hold. In such a case, the IND sponsor and the FDA must resolve any outstanding concerns before the clinical trial can begin. As a result, submission of an IND may not result in the FDA allowing clinical trials to commence.
Clinical Trials
The clinical stage of development involves the administration of the investigational product to healthy volunteers or patients under the supervision of qualified investigators, generally physicians not employed by or under the trial sponsor’s control, in accordance with GCP requirements, which include the requirement that all research subjects provide their informed consent for their participation in any clinical trial. Clinical trials are conducted under protocols detailing, among other things, the objectives of the clinical trial, dosing procedures, subject selection and exclusion criteria and the parameters to be used to monitor subject safety and assess efficacy. Each protocol, and any subsequent amendments to the protocol, must be submitted to the FDA as part of the IND. Furthermore, each clinical trial must be reviewed and approved by an IRB for each institution at which the clinical trial will be conducted to ensure that the risks to individuals participating in the clinical trials are minimized and are reasonable in relation to anticipated benefits. The IRB also approves the informed consent form that must be provided to each clinical trial subject or his or her legal representative, and must monitor the clinical trial until completed. There also are requirements governing the reporting of ongoing clinical trials and completed clinical trial results to public registries.
A sponsor who wishes to conduct a clinical trial outside of the United States may, but need not, obtain FDA authorization to conduct the clinical trial under an IND. If a foreign clinical trial is not conducted under an IND, the sponsor may submit data from the clinical trial to the FDA in support of an NDA. The FDA will accept a well-designed and well-conducted foreign clinical trial not conducted under an IND if the trial was conducted in accordance with GCP requirements and the FDA is able to validate the data through an onsite inspection, if deemed necessary, and the practice of medicine in the foreign country is consistent with the United States.
Clinical trials in the United States generally are conducted in three sequential phases, known as Phase I, Phase II and Phase III, and may overlap.
| ● | Phase I clinical trials generally involve a small number of healthy volunteers or disease-affected patients who are initially exposed to a single dose and then multiple doses of the drug candidate. The primary purpose of these clinical trials is to assess the metabolism, pharmacologic action, tolerability and safety of the drug. |
| ● | Phase II clinical trials involve studies in disease-affected patients to determine the dose and dosing schedule required to produce the desired benefits. At the same time, safety and further pharmacokinetic and pharmacodynamic information is collected, possible adverse effects and safety risks are identified and a preliminary evaluation of efficacy is conducted. |
| ● | Phase III clinical trials generally involve a large number of patients at multiple sites and are designed to provide the data necessary to demonstrate the effectiveness of the product for its intended use, its safety in use and to establish the overall benefit/risk relationship of the product and provide an adequate basis for product approval. These trials may include comparisons with placebo and/or other comparator treatments. The duration of treatment is often extended to mimic the actual use of a product during marketing. |
55
Post-approval trials, sometimes referred to as Phase IV clinical trials, are conducted after initial marketing approval. These trials are used to gain additional experience from the treatment of patients in the intended therapeutic indication. In certain instances, the FDA may mandate the performance of Phase 4 clinical trials as a condition of approval of an NDA.
Progress reports detailing the results of the clinical trials, among other information, must be submitted at least annually to the FDA and written IND safety reports must be submitted to the FDA and the investigators for serious and unexpected suspected adverse events, findings from other studies suggesting a significant risk to humans exposed to the drug, findings from animal or in vitro testing that suggest a significant risk for human subjects and any clinically important increase in the rate of a serious suspected adverse reaction over that listed in the protocol or investigator brochure.
Phase I, Phase II and Phase III clinical trials may not be completed successfully within any specified period, if at all. The FDA or the sponsor may suspend or terminate a clinical trial at any time on various grounds, including a finding that the research subjects or patients are being exposed to an unacceptable health risk. Similarly, an IRB can suspend or terminate approval of a clinical trial at its institution if the clinical trial is not being conducted in accordance with the IRB’s requirements or if the drug has been associated with unexpected serious harm to patients. Additionally, some clinical trials are overseen by an independent group of qualified experts organized by the clinical trial sponsor, known as a data safety monitoring board or committee. This group provides authorization for whether a trial may move forward at designated check-points based on access to certain data from the trial. Concurrent with clinical trials, companies usually complete additional animal safety studies and also must develop additional information about the chemistry and physical characteristics of the drug as well as finalize a process for manufacturing the product in commercial quantities in accordance with cGMP requirements. The manufacturing process must be capable of consistently producing quality batches of our drug candidates. Additionally, appropriate packaging must be selected and tested and stability studies must be conducted to demonstrate that our drug candidates do not undergo unacceptable deterioration over their labeled shelf life.
NDA Review Process
Following completion of the clinical trials, data is analyzed to assess whether the investigational product is safe and effective for the proposed indicated use or uses. The results of preclinical studies and clinical trials are then submitted to the FDA as part of an NDA, along with proposed labeling, chemistry and manufacturing information to ensure product quality and other relevant data. In short, the NDA is a request for approval to market the drug for one or more specified indications and must contain proof of safety and efficacy for a drug.
The application must include both negative and ambiguous results of preclinical studies and clinical trials, as well as positive findings. Data may come from company-sponsored clinical trials intended to test the safety and efficacy of a product’s use or from a number of alternative sources, including studies initiated by investigators. To support marketing approval, the data submitted must be sufficient in quality and quantity to establish the safety and efficacy of the investigational product to the satisfaction of FDA. FDA approval of an NDA must be obtained before a drug may be marketed in the United States.
Under the Prescription Drug User Fee Act (“PDUFA”), as amended, each NDA must be accompanied by a user fee. The FDA adjusts the PDUFA user fees on an annual basis. According to the FDA’s fiscal year 2019 fee schedule, effective through September 30, 2020, the user fee for an application requiring clinical data, such as an NDA, was approximately $2.94 million. PDUFA also imposes an annual program fee for each marketed human drug ($325,424 in 2020) and an annual establishment fee on facilities used to manufacture prescription drugs. Fee waivers or reductions are available in certain circumstances, including a waiver of the application fee for the first application filed by a small business. Additionally, no user fees are assessed on NDAs for products designated as orphan drugs, unless the product also includes a non-orphan indication.
The FDA reviews all submitted NDAs before it accepts them for filing, and may request additional information rather than accepting the NDA for filing. The FDA must make a decision on accepting an NDA for filing within 60 days of receipt. Once the submission is accepted for filing, the FDA begins an in-depth review of the NDA. Under the goals and policies agreed to by the FDA under PDUFA, the FDA has 10 months, from the filing date, in which to complete its initial review of a new molecular-entity NDA and respond to the applicant, and six months from the filing date of a new molecular-entity NDA designated for priority review. The FDA does not always meet its PDUFA goal dates for standard and priority NDAs, and the review process is often extended by FDA requests for additional information or clarification.
56
Before approving an NDA, the FDA will conduct a pre-approval inspection of the manufacturing facilities for the new product to determine whether they comply with cGMP requirements. The FDA will not approve the product unless it determines that the manufacturing processes and facilities are in compliance with cGMP requirements and adequate to assure consistent production of the product within required specifications. The FDA also may audit data from clinical trials to ensure compliance with GCP requirements. Additionally, the FDA may refer applications for novel drug products or drug products which present difficult questions of safety or efficacy to an advisory committee, typically a panel that includes clinicians and other experts, for review, evaluation and a recommendation as to whether the application should be approved and under what conditions, if any. The FDA is not bound by recommendations of an advisory committee, but it considers such recommendations when making decisions on approval. The FDA likely will reanalyze the clinical trial data, which could result in extensive discussions between the FDA and the applicant during the review process. After the FDA evaluates an NDA, it will issue an approval letter or a Complete Response Letter. An approval letter authorizes commercial marketing of the drug with specific prescribing information for specific indications. A Complete Response Letter indicates that the review cycle of the application is complete and the application will not be approved in its present form. A Complete Response Letter usually describes all of the specific deficiencies in the NDA identified by the FDA. The Complete Response Letter may require additional clinical data, additional pivotal Phase 3 clinical trial(s) and/or other significant and time-consuming requirements related to clinical trials, preclinical studies or manufacturing. If a Complete Response Letter is issued, the applicant may either resubmit the NDA, addressing all of the deficiencies identified in the letter, or withdraw the application. Even if such data and information are submitted, the FDA may decide that the NDA does not satisfy the criteria for approval. Data obtained from clinical trials are not always conclusive and the FDA may interpret data differently than we interpret the same data.
Orphan Drugs
Under the Orphan Drug Act, the FDA may grant orphan designation to a drug or biological product intended to treat a rare disease or condition, which is generally a disease or condition that affects fewer than 200,000 individuals in the United States, or more than 200,000 individuals in the United States and for which there is no reasonable expectation that the cost of developing and making the product available in the United States for this type of disease or condition will be recovered from sales of the product.
Orphan drug designation must be requested before submitting an NDA. After the FDA grants orphan drug designation, the identity of the therapeutic agent and its potential orphan use are disclosed publicly by the FDA. Orphan drug designation does not convey any advantage in or shorten the duration of the regulatory review and approval process.
If a product that has orphan designation subsequently receives the first FDA approval for the disease or condition for which it has such designation, the product is entitled to orphan drug exclusivity, which means that the FDA may not approve any other applications to market the same drug for the same indication for seven years from the date of such approval, except in limited circumstances, such as a showing of clinical superiority to the product with orphan exclusivity by means of greater effectiveness, greater safety or providing a major contribution to patient care or in instances of drug supply issues. However, competitors may receive approval of either a different product for the same indication or the same product for a different indication but that could be used off-label in the orphan indication. Orphan drug exclusivity also could block the approval of one of our products for seven years if a competitor obtains approval before we do for the same product, as defined by the FDA, for the same indication we are seeking approval, or if a drug candidate is determined to be contained within the scope of the competitor’s product for the same indication or disease. If one of our products designated as an orphan drug receives marketing approval for an indication broader than that which is designated, it may not be entitled to orphan drug exclusivity. Orphan drug status in the European Union has similar, but not identical, requirements and benefits.
57
Expedited Development and Review Programs
The FDA has a fast track program that is intended to expedite or facilitate the process for reviewing new drugs that meet certain criteria. Specifically, new drugs are eligible for fast track designation if they are intended to treat a serious or life-threatening condition and preclinical or clinical data demonstrate the potential to address unmet medical needs for the condition. Fast track designation applies to both the product and the specific indication for which it is being studied. The sponsor can request the FDA to designate the product for fast track status any time before receiving NDA approval, but ideally no later than the pre-NDA meeting with the FDA.
Any product submitted to the FDA for marketing, including under a fast track program, may be eligible for other types of FDA programs intended to expedite development and review, such as priority review and accelerated approval. Any product is eligible for priority review if it treats a serious or life-threatening condition and, if approved, would provide a significant improvement in safety and effectiveness compared to available therapies.
A product may also be eligible for accelerated approval, if it treats a serious or life-threatening condition and generally provides a meaningful advantage over available therapies. In addition, it must demonstrate an effect on a surrogate endpoint that is reasonably likely to predict clinical benefit or on a clinical endpoint that can be measured earlier than irreversible morbidity or mortality (“IMM”), which is reasonably likely to predict an effect on IMM or other clinical benefit. As a condition of approval, the FDA may require that a sponsor of a drug or biologic receiving accelerated approval perform adequate and well-controlled post-marketing clinical trials. If the FDA concludes that a drug or biologic shown to be effective can be safely used only if distribution or use is restricted, it may require such post-marketing restrictions as it deems necessary to assure safe use of the product.
Additionally, a drug may be eligible for designation as a breakthrough therapy if the product is intended, alone or in combination with one or more other drugs or biologics, to treat a serious or life-threatening condition and preliminary clinical evidence indicates that the product may demonstrate substantial improvement over currently approved therapies on one or more clinically significant endpoints. The benefits of breakthrough therapy designation include the same benefits as fast track designation, plus intensive guidance from the FDA to ensure an efficient drug development program. Fast track designation, priority review, accelerated approval and breakthrough therapy designation do not change the standards for approval, but may expedite the development or approval process.
Post-Approval Requirements
Following approval of a new product, the manufacturer and the approved product are subject to continuing regulation by the FDA, including, among other things, monitoring and record-keeping requirements, requirements to report adverse experiences and comply with promotion and advertising requirements, which include restrictions on promoting drugs for unapproved uses or patient populations, known as “off-label use,” and limitations on industry-sponsored scientific and educational activities. Although physicians may prescribe legally available drugs for off-label uses, manufacturers may not market or promote such uses. Prescription drug promotional materials must be submitted to the FDA in conjunction with their first use. Further, if there are any modifications to the drug, including changes in indications, labeling or manufacturing processes or facilities, the applicant may be required to submit and obtain FDA approval of a new NDA or NDA supplement, which may require the development of additional data or preclinical studies and clinical trials.
The FDA may also place other conditions on approvals including the requirement for REMS, to assure the safe use of the product. A REMS could include medication guides, physician communication plans or elements to assure safe use, such as restricted distribution methods, patient registries and other risk minimization tools. Any of these limitations on approval or marketing could restrict the commercial promotion, distribution, prescription or dispensing of products. Product approvals may be withdrawn for non-compliance with regulatory standards or if problems occur following initial marketing.
58
The FDA may withdraw approval if compliance with regulatory requirements and standards is not maintained or if problems occur after the product reaches the market. Later discovery of previously unknown problems with a product, including adverse events of unanticipated severity or frequency, or with manufacturing processes, or failure to comply with regulatory requirements, may result in revisions to the approved labeling to add new safety information; imposition of post-market studies or clinical studies to assess new safety risks or imposition of distribution restrictions or other restrictions under a REMS program. Other potential consequences include, among other things:
| ● | restrictions on the marketing or manufacturing of the product, complete withdrawal of the product from the market, or product recalls; |
| ● | fines, warning letters, or holds on post-approval clinical studies; |
| ● | refusal of the FDA to approve pending applications or supplements to approved applications; |
| ● | applications, or suspension or revocation of product license approvals; |
| ● | product seizure or detention, or refusal to permit the import or export of products; or |
| ● | injunctions or the imposition of civil or criminal penalties. |
The FDA strictly regulates marketing, labeling, advertising and promotion of products that are placed on the market. Drugs may be promoted only for the approved indications and in accordance with the provisions of the approved label. The FDA and other agencies actively enforce the laws and regulations prohibiting the promotion of off-label uses, and a company that is found to have improperly promoted off-label uses may be subject to significant liability.
Other U.S. Regulatory Matters
Manufacturing, sales, promotion and other activities following product approval are also subject to regulation by numerous regulatory authorities in the United States in addition to the FDA, including the Centers for Medicare & Medicaid Services, other divisions of the Department of Health and Human Services, the Department of Justice, the Drug Enforcement Administration, the Consumer Product Safety Commission, the Federal Trade Commission, the Occupational Safety & Health Administration, the Environmental Protection Agency, and state and local governments.
For example, in the United States, sales, marketing and scientific and educational programs also must comply with state and federal fraud and abuse laws, false claims laws, transparency laws, government price reporting, and health information privacy and security laws. These laws include the following:
| ● | the federal Anti-Kickback Statute, which makes it illegal for any person, including a prescription drug manufacturer (or a party acting on its behalf), to knowingly and willfully solicit, receive, offer or pay any remuneration that is intended to induce or reward referrals, including the purchase, recommendation, order or prescription of a particular drug, for which payment may be made under a federal healthcare program, such as Medicare or Medicaid. Moreover, the ACA provides that the government may assert that a claim including items or services resulting from a violation of the federal Anti-Kickback Statute constitutes a false or fraudulent claim for purposes of the civil False Claims Act; |
| ● | the federal false claims and civil monetary penalties laws, including the civil False Claims Act that can be enforced by private citizens through civil whistleblower or qui tam actions, prohibit individuals or entities from, among other things, knowingly presenting, or causing to be presented, to the federal government, claims for payment that are false or fraudulent or making a false statement to avoid, decrease or conceal an obligation to pay money to the federal government; |
| ● | the Federal Health Insurance Portability and Accountability Act of 1996 (“HIPAA”), prohibits, among other things, executing or attempting to execute a scheme to defraud any healthcare benefit program or making false statements relating to healthcare matters; |
| ● | HIPAA, as amended by the Health Information Technology for Economic and Clinical Health Act and their implementing regulations, also imposes obligations, including mandatory contractual terms, with respect to safeguarding the privacy, security and transmission of individually identifiable health information; |
59
| ● | the federal Physician Payments Sunshine Act requires applicable manufacturers of covered drugs, devices, biologics and medical supplies for which payment is available under Medicare, Medicaid or the Children’s Health Insurance Program, with specific exceptions, to annually report to CMS information regarding payments and other transfers of value to physicians and teaching hospitals as well as information regarding ownership and investment interests held by physicians and their immediate family members; and |
| ● | analogous state and foreign laws and regulations, such as state anti-kickback and false claims laws which may apply to sales or marketing arrangements and claims involving healthcare items or services reimbursed by non-governmental third-party payors, including private insurers, state laws that require biotechnology companies to comply with the biotechnology industry’s voluntary compliance guidelines and the relevant compliance guidance promulgated by the federal government and may require drug manufacturers to report information related to payments and other transfers of value to physicians and other healthcare providers or marketing expenditures, state laws that require biotechnology companies to report information on the pricing of certain drug products, and state and foreign laws that govern the privacy and security of health information in some circumstances, many of which differ from each other in significant ways and often are not preempted by HIPAA, thus complicating compliance efforts. |
Pricing and rebate programs must also comply with the Medicaid rebate requirements of the U.S. Omnibus Budget Reconciliation Act of 1990 and more recent requirements in the ACA. If products are made available to authorized users of the Federal Supply Schedule of the General Services Administration, additional laws and requirements apply. Products must meet applicable child-resistant packaging requirements under the U.S. Poison Prevention Packaging Act. Manufacturing, sales, promotion and other activities also are potentially subject to federal and state consumer protection and unfair competition laws.
The distribution of pharmaceutical products is subject to additional requirements and regulations, including extensive record-keeping, licensing, storage and security requirements intended to prevent the unauthorized sale of pharmaceutical products.
The failure to comply with any of these laws or regulatory requirements subjects firms to possible legal or regulatory action. Depending on the circumstances, failure to meet applicable regulatory requirements can result in significant civil, criminal and administrative penalties, including damages, fines, disgorgement, individual imprisonment, exclusion from participation in government funded healthcare programs, such as Medicare and Medicaid, integrity oversight and reporting obligations, contractual damages, reputational harm, diminished profits and future earnings, injunctions, requests for recall, seizure of products, total or partial suspension of production, denial or withdrawal of product approvals or refusal to allow a firm to enter into supply contracts, including government contracts.
U.S. Patent-Term Restoration and Marketing Exclusivity
Depending upon the timing, duration and specifics of FDA approval of any future drug candidates, some of our U.S. patents may be eligible for limited patent term extension under the Hatch-Waxman Act. The Hatch-Waxman Act permits restoration of the patent term of up to five years as compensation for patent term lost during product development and FDA regulatory review process. Patent-term restoration, however, cannot extend the remaining term of a patent beyond a total of 14 years from the product’s approval date. The patent-term restoration period is generally one-half the time between the effective date of an IND or the issue date of the patent, whichever is later, and the submission date of an NDA plus the time between the submission date of an NDA or the issue date of the patent, whichever is later, and the approval of that application, except that the review period is reduced by any time during which the applicant failed to exercise due diligence. Only one patent applicable to an approved drug is eligible for the extension and the application for the extension must be submitted prior to the expiration of the patent. The USPTO, in consultation with the FDA, reviews and approves the application for any patent term extension or restoration. In the future, we may apply for restoration of patent term for our currently owned or licensed patents to add patent life beyond its current expiration date, depending on the expected length of the clinical trials and other factors involved in the filing of the relevant NDA.
60
Market exclusivity provisions under the FDCA also can delay the submission or the approval of certain applications. The FDCA provides a five-year period of non-patent marketing exclusivity within the United States to the first applicant to gain approval of an NDA for a new chemical entity. A drug is a new chemical entity if the FDA has not previously approved any other new drug containing the same active moiety, which is the molecule or ion responsible for the action of the drug substance. During the exclusivity period, the FDA may not accept for review an abbreviated new drug application (“ANDA”), or a 505(b)(2) NDA submitted by another company for another version of such drug where the applicant does not own or have a legal right of reference to all the data required for approval. However, an application may be submitted after four years if it contains a certification of patent invalidity or non-infringement. The FDCA also provides three years of marketing exclusivity for a NDA, 505(b)(2) NDA or supplement to an existing NDA if new clinical investigations, other than bioavailability studies, that were conducted or sponsored by the applicant are deemed by the FDA to be essential to the approval of the application, for example, new indications, dosages or strengths of an existing drug. This three-year exclusivity covers only the conditions of use associated with the new clinical investigations and does not prohibit the FDA from approving ANDAs for drugs containing the original active agent. Five-year and three-year exclusivity will not delay the submission or approval of a full NDA. However, an applicant submitting a full NDA would be required to conduct or obtain a right of reference to all of the preclinical studies and adequate and well-controlled clinical trials necessary to demonstrate safety and effectiveness.
European Union Drug Development
Similar to the United States, the various phases of preclinical and clinical research in the European Union are subject to significant regulatory controls. Although the EU Clinical Trials Directive 2001/20/EC has sought to harmonize the EU clinical trials regulatory framework, setting out common rules for the control and authorization of clinical trials in the EU, the EU Member States have transposed and applied the provisions of the Directive differently. This has led to significant variations in the member state regimes. Under the current regime, before a clinical trial can be initiated it must be approved in each of the EU countries where the trial is to be conducted by two distinct bodies: the National Competent Authority (“NCA”), and one or more Ethics Committees (“ECs”). Under the current regime all suspected unexpected serious adverse reactions to the investigated drug that occur during the clinical trial have to be reported to the NCA and ECs of the Member State where they occurred.
The EU clinical trials legislation currently is undergoing a transition process mainly aimed at harmonizing and streamlining clinical-trial authorization, simplifying adverse-event reporting procedures, improving the supervision of clinical trials and increasing their transparency. Recently enacted Clinical Trials Regulation EU No 536/2014 ensures that the rules for conducting clinical trials in the EU will be identical. In the meantime, Clinical Trials Directive 2001/20/EC continues to govern all clinical trials performed in the EU.
European Union Drug Review and Approval
In the European Economic Area (“EEA”), which is comprised of the 27 Member States of the European Union (including Norway and excluding Croatia), Iceland and Liechtenstein, medicinal products can only be commercialized after obtaining a Marketing Authorization (“MA”). There are two types of marketing authorizations.
| ● | The Community MA is issued by the European Commission through the Centralized Procedure, based on the opinion of the Committee for Medicinal Products for Human Use (“CHMP”), of the EMA, and is valid throughout the entire territory of the EEA. The Centralized Procedure is mandatory for certain types of products, such as biotechnology medicinal products, orphan medicinal products, advanced-therapy medicines such as gene-therapy, somatic cell-therapy or tissue-engineered medicines and medicinal products containing a new active substance indicated for the treatment of HIV, AIDS, cancer, neurodegenerative disorders, diabetes, auto-immune and other immune dysfunctions and viral diseases. The Centralized Procedure is optional for products containing a new active substance not yet authorized in the EEA, or for products that constitute a significant therapeutic, scientific or technical innovation or which are in the interest of public health in the EU. |
61
| ● | National MAs, which are issued by the competent authorities of the Member States of the EEA and only cover their respective territory, are available for products not falling within the mandatory scope of the Centralized Procedure. Where a product has already been authorized for marketing in a Member State of the EEA, this National MA can be recognized in another Member States through the Mutual Recognition Procedure. If the product has not received a National MA in any Member State at the time of application, it can be approved simultaneously in various Member States through the Decentralized Procedure. Under the Decentralized Procedure an identical dossier is submitted to the competent authorities of each of the Member States in which the MA is sought, one of which is selected by the applicant as the Reference Member State (“RMS”). The competent authority of the RMS prepares a draft assessment report, a draft summary of the product characteristics (“SPC”), and a draft of the labeling and package leaflet, which are sent to the other Member States (referred to as the Member States Concerned) for their approval. If the Member States Concerned raise no objections, based on a potential serious risk to public health, to the assessment, SPC, labeling or packaging proposed by the RMS, the product is subsequently granted a national MA in all the Member States (i.e., in the RMS and the Member States Concerned). |
Under the above described procedures, before granting the MA, EMA or the competent authorities of the Member States of the EEA make an assessment of the risk-benefit balance of the product on the basis of scientific criteria concerning its quality, safety and efficacy. Similar to the U.S. patent term-restoration, Supplementary Protection Certificates (“SPCs”) serve as an extension to a patent right in Europe for up to five years. SPCs apply to specific pharmaceutical products to offset the loss of patent protection due to the lengthy testing and clinical trials these products require prior to obtaining regulatory marketing approval.
Coverage and Reimbursement
Sales of our products will depend, in part, on the extent to which our products will be covered by third-party payors, such as government health programs, commercial insurance, and managed healthcare organizations. There is significant uncertainty related to third-party payor coverage and reimbursement of newly approved products. In the United States, for example, principal decisions about reimbursement for new products are typically made by CMS. CMS decides whether and to what extent a new product will be covered and reimbursed under Medicare, and private third-party payors often follow CMS’s decisions regarding coverage and reimbursement to a substantial degree. However, no uniform policy of coverage and reimbursement for drug products exists. Accordingly, decisions regarding the extent of coverage and amount of reimbursement to be provided for any of our products will be made on a payor-by-payor basis.
Increasingly, third-party payors are requiring that drug companies provide them with predetermined discounts from list prices and are challenging the prices charged for medical products. Further, such payors are increasingly challenging the price, examining the medical necessity and reviewing the cost effectiveness of medical drug candidates. There may be especially significant delays in obtaining coverage and reimbursement for newly approved drugs. Third-party payors may limit coverage to specific drug candidates on an approved list, known as a formulary, which might not include all FDA-approved drugs for a particular indication. We may need to conduct expensive pharmaco-economic studies to demonstrate the medical necessity and cost effectiveness of our products. As a result, the coverage determination process is often a time-consuming and costly process that will require us to provide scientific and clinical support for the use of our products to each payor separately, with no assurance that coverage and adequate reimbursement will be obtained.
In addition, in most foreign countries, the proposed pricing for a drug must be approved before it may be lawfully marketed. The requirements governing drug pricing and reimbursement vary widely from country to country. For example, the European Union provides options for its member states to restrict the range of medicinal products for which their national health insurance systems provide reimbursement and to control the prices of medicinal products for human use. A member state may approve a specific price for the medicinal product or it may instead adopt a system of direct or indirect controls on the profitability of the company placing the medicinal product on the market. There can be no assurance that any country that has price controls or reimbursement limitations for pharmaceutical products will allow favorable reimbursement and pricing arrangements for any of our products. Historically, products launched in the European Union do not follow price structures of the United States and generally prices tend to be significantly lower.
62
Healthcare Reform
The United States government, state legislatures, and foreign governments have shown significant interest in implementing cost containment programs to limit the growth of government-paid healthcare costs, including price-controls, restrictions on reimbursement, and requirements for substitution of generic products for branded prescription drugs. For example, in March 2010, the Patient Protection and Affordable Care Act of 2010, as amended by the Health Care and Education Reconciliation Act of 2010 (collectively, the “ACA”), was passed which substantially changed the way healthcare is financed by both the government and private insurers, and significantly impacts the U.S. pharmaceutical industry. The ACA contains provisions that may reduce the profitability of drug products through increased rebates for drugs reimbursed by Medicaid programs, extension of Medicaid rebates to Medicaid managed care plans, mandatory discounts for certain Medicare Part D beneficiaries and annual fees based on pharmaceutical companies’ share of sales to federal health care programs. The Medicaid Drug Rebate Program requires pharmaceutical manufacturers to enter into and have in effect a national rebate agreement with the HHS Secretary as a condition for states to receive federal matching funds for the manufacturer’s outpatient drugs furnished to Medicaid patients. The ACA made several changes to the Medicaid Drug Rebate Program, including increasing pharmaceutical manufacturers’ rebate liability by raising the minimum basic Medicaid rebate on most branded prescription drugs from 15.1% of average manufacturer price (“AMP”), to 23.1% of AMP and adding a new rebate calculation for “line extensions” (i.e., new formulations, such as extended release formulations) of solid oral dosage forms of branded products, as well as potentially impacting their rebate liability by modifying the statutory definition of AMP. The ACA also expanded the universe of Medicaid utilization subject to drug rebates by requiring pharmaceutical manufacturers to pay rebates on Medicaid managed care utilization and by enlarging the population potentially eligible for Medicaid drug benefits. The Centers for Medicare & Medicaid Services (“CMS”), have proposed to expand Medicaid rebate liability to the territories of the United States as well. Additionally, for a drug product to receive federal reimbursement under the Medicaid or Medicare Part B programs or to be sold directly to U.S. government agencies, the manufacturer must extend discounts to entities eligible to participate in the 340B drug pricing program. The required 340B discount on a given product is calculated based on the AMP and Medicaid rebate amounts reported by the manufacturer.
Some of the provisions of the ACA have yet to be implemented, and there have been judicial and Congressional challenges to certain aspects of the ACA Congress has recently considered legislation that would repeal or repeal and replace all or part of the ACA. While Congress has not passed comprehensive repeal legislation, two bills affecting the implementation of certain taxes under the ACA have passed. On December 22, 2017, the Tax Cuts and Jobs Act (the “Tax Act”) was enacted, which includes a provision repealing, effective January 1, 2019, the tax-based shared responsibility payment imposed by the ACA on certain individuals who fail to maintain qualifying health coverage for all or part of a year that is commonly referred to as the “individual mandate.” The Bipartisan Budget Act of 2018 (the “BBA”), among other things, amended the ACA, effective January 1, 2019, to close the coverage gap in most Medicare Part D drug plans. In July 2018, CMS published a final rule permitting further collections and payments to and from certain ACA-qualified health plans and health insurance issuers under the ACA risk adjustment program in response to the outcome of federal district court litigation regarding the method CMS uses to determine this risk adjustment. On December 14, 2018, a Texas U.S. District Court Judge ruled that the ACA is unconstitutional in its entirety because the “individual mandate” was repealed by Congress as part of the Tax Act. On December 18, 2019, the United States Court of Appeal for the Fifth Circuit ruled that the “individual mandate” of the ACA is unconstitutional, but remanded the case to the U.S. District Court to reconsider whether the entire ACA is unconstitutional. The remanded case is still pending in the U.S. District Court and other than on the application of the “individual mandate,” the ruling will have no immediate effect on the remaining provisions of the ACA pending a decision on remand by the U.S. District Court. Consequently, it is unclear how this decision, subsequent appeals, and other efforts to repeal and replace the ACA will impact the ACA.
63
Other legislative changes have been proposed and adopted in the United States since the ACA was enacted. These changes included aggregate reductions to Medicare payments to providers of up to 2% per fiscal year, effective April 1, 2013, which, due to subsequent legislative amendments, will stay in effect through 2027 unless additional congressional action is taken. In January 2013, President Obama signed into law the American Taxpayer Relief Act of 2012, which, among other things, reduced Medicare payments to several providers, and increased the statute of limitations period for the government to recover overpayments to providers from three to five years. These new laws may result in additional reductions in Medicare and other healthcare funding, which could have a material adverse effect on customers for our drugs, if approved, and accordingly, our financial operations.
Additionally, there has been heightened governmental scrutiny recently over the manner in which drug manufacturers set prices for their marketed products, which has resulted in several Congressional inquiries and proposed and enacted federal and state legislation designed to, among other things, bring more transparency to product pricing, review the relationship between pricing and manufacturer patient programs, and reform government program reimbursement methodologies for drug products. For example, At the state level, legislatures have increasingly passed legislation and implemented regulations designed to control pharmaceutical and biological product pricing, including price or patient reimbursement constraints, discounts, restrictions on certain product access and marketing cost disclosure and transparency measures, and, in some cases, designed to encourage importation from other countries and bulk purchasing.
Moreover, the Medicare Prescription Drug, Improvement, and Modernization Act of 2003 (“MMA”), established the Medicare Part D program to provide a voluntary prescription drug benefit to Medicare beneficiaries. Under Part D, Medicare beneficiaries may enroll in prescription drug plans offered by private entities that provide coverage of outpatient prescription drugs. Unlike Medicare Part A and B, Part D coverage is not standardized. While all Medicare drug plans must give at least a standard level of coverage set by Medicare, Part D prescription drug plan sponsors are not required to pay for all covered Part D drugs, and each drug plan can develop its own drug formulary that identifies which drugs it will cover and at what tier or level. However, Part D prescription drug formularies must include drugs within each therapeutic category and class of covered Part D drugs, though not necessarily all the drugs in each category or class. Any formulary used by a Part D prescription drug plan must be developed and reviewed by a pharmacy and therapeutic committee. Government payment for some of the costs of prescription drugs may increase demand for products for which we receive marketing approval. However, any negotiated prices for our products covered by a Part D prescription drug plan likely will be lower than the prices we might otherwise obtain. Moreover, while the MMA applies only to drug benefits for Medicare beneficiaries, private third-party payors often follow Medicare coverage policy and payment limitations in setting their own payment rates.
Employees
As of the date of this report, we employed a total of 15 professionals: 11 full-time and four part-time employees. None of our employees are represented by a labor union or covered under a collective bargaining agreement. We believe that we maintain strong relations with our employees.
We also engage outside consultants to assist with research and development, clinical development and regulatory matters, business development, operations and other functions from time to time.
64
Human Capital Resources.
Our employees drive our mission and we place a high level of importance on employee engagement and corporate culture. Fostering and maintaining a strong, healthy culture is a key strategic focus for us, and we regularly engage in independent third party surveys to gauge the satisfaction and engagement of our team.
Our compensation approach is aimed at attracting, retaining, motivating and rewarding superior employees who operate in a highly competitive and technologically challenging environment. The structure of our compensation aims to balance incentives for both short-term and long-term performance.
Some examples of the benefits we offer include medical insurance, dental insurance, vision insurance, and an unlimited paid-time off policy.
A substantial portion of our employees are focused on leading and advancing our drug development, biology and data science efforts. As we progress our product candidates and grow and expand our team, we intend to continue to place a significant focus on our human capital resources.
Available Information
We maintain a website at www.lanternpharma.com. The contents of our website are not incorporated in, or otherwise to be regarded as part of, this Annual Report on Form 10-K. We make available, free of charge on our website, access to our Annual Report on Form 10-K, our Quarterly Reports on Form 10-Q, our Current Reports on Form 8-K and amendments to those reports filed or furnished pursuant to Section 13(a) or 15(d) of the Securities Exchange Act of 1934, as amended (the “Exchange Act”), as soon as reasonably practicable after we file or furnish them electronically with the Securities and Exchange Commission (“SEC”).
Copies of our Annual Report on Form 10-K, our Quarterly Reports on Form 10-Q, our Current Reports on Form 8-K and other filings we make with the SEC are also available at the SEC’s Public Reference Room at 100 F Street, N.E., Washington, D.C. 20549. Please call the SEC at 1-800-SEC-0330 for further information on the Public Reference Room. Our SEC filings are also available on the SEC’s website at www.sec.gov. Statements contained in this Annual Report on Form 10-K concerning the contents of any contract or any other documents are not necessarily complete. If a contract or document has been filed as an exhibit to this Annual Report on Form 10-K, please see the copy of the contract or document that has been filed. Each statement in this this Annual Report on Form 10-K relating to a contract or document filed as an exhibit is qualified in all respects by the filed exhibit.
An investment in our common stock involves a high degree of risk. You should give careful consideration to the following risk factors, in addition to general economic and business risks and the other information included in this Annual Report on Form 10-K, including our financial statements and related notes, before deciding whether to invest in shares of our common stock. The occurrence of any of the adverse developments described in the following risk factors could materially and adversely harm our business, financial condition, results of operations or prospects. In that case, the trading price of our common stock could decline, and you may lose all or part of your investment. Additional risks or uncertainties not presently known to us or that we currently deem immaterial may also materially and adversely harm our business, financial condition, results of operations or prospects.
Risks Related to Financial Position and Need for Capital
We have a limited operating history and have never generated any revenues other than from research grants, which may make it difficult to evaluate the success of our business to date and to assess our future viability.
We were incorporated in November 7, 2013, and to date have been largely focused on organizing and staffing our company, raising capital, developing the RADR® platform and acquiring the rights to, and advancing the development of, our drug candidates, including conducting preclinical studies and early phase clinical trials on our drug candidates. We have not yet demonstrated an ability to successfully complete clinical trials, obtain marketing approvals, manufacture drugs on a commercial scale, or arrange for a third party to do so on our behalf, or conduct sales and marketing activities necessary for successful commercialization. Consequently, predictions about our future success or viability may not be as accurate as they could be if we had a longer operating history or a history of successfully developing and commercializing drugs.
65
We expect our financial condition and operating results to continue to fluctuate from quarter to quarter and year to year due to a variety of factors, many of which are beyond our control. We will need to eventually transition from a company with a research and development focus to a company capable of undertaking commercial activities. We may encounter unforeseen expenses, difficulties, complications and delays, and may not be successful in such a transition.
We have incurred significant operating losses since inception and anticipate that we will continue to incur substantial operating losses for the foreseeable future and may never achieve or maintain profitability.
Since our inception, we have incurred losses. Our net losses were $5,908,190 and $2,428,185 for the years ended December 31, 2020 and 2019, respectively. We expect to continue to incur significant expenses and increasing operating losses for the foreseeable future. None of our current drug candidates have been approved for marketing in the United States, or in any other jurisdiction, and may never receive such approval. It could be several years, if ever, before we have a commercialized drug that generates significant revenues. As a result, we are uncertain when or if we will achieve profitability and, if so, whether we will be able to sustain profitability. The net losses we incur may fluctuate significantly from quarter to quarter and year to year. We anticipate that our expenses will increase substantially as we:
| ● | continue the development of our drug candidates; |
| ● | initiate preclinical studies and clinical trials for any additional indications for our current drug candidates and any future drug candidates that we may pursue; |
| ● | continue to build our portfolio of drug candidates through the acquisition or in-license of additional drug candidates or technologies; |
| ● | continue to develop, maintain, expand and protect our intellectual property portfolio; |
| ● | continue to develop, maintain, and expand our RADR® platform; |
| ● | pursue regulatory approvals for our current and future drug candidates that successfully complete clinical trials; |
| ● | ultimately establish a sales, marketing, distribution and other commercial infrastructure to commercialize any drug candidate for which we may obtain marketing approval; |
| ● | hire additional clinical, regulatory, scientific and accounting personnel; and |
| ● | incur additional legal, accounting and other expenses in operating as a public company. |
To become and remain profitable, we must develop and eventually commercialize one or more drug candidates with significant market potential or license one or more of our drug candidates to an industry partner. This will require us to be successful in a range of challenging activities, including completing clinical trials of our drug candidates, publishing our data and findings on our drug candidates with peer reviewed publications, developing commercial scale manufacturing processes, obtaining marketing approval, manufacturing, marketing and selling any current and future drug candidates for which we may obtain marketing approval, and satisfying any post-marketing requirements. We are only in the preliminary stages of most of these activities and, in some cases, have not yet commenced certain of these activities. We may never succeed in any or all of these activities and, even if we do, we may never generate sufficient revenue to achieve profitability.
66
Because of the numerous risks and uncertainties associated with drug development, we are unable to accurately predict the timing or amount of expenses or when, or if, we will obtain marketing approval to commercialize any of our drug candidates. If we are required by the U.S. Food and Drug Administration, or FDA, or other regulatory authorities such as the European Medicines Agency, or EMA, to perform studies and trials in addition to those currently expected, or if there are any delays in the development, or in the completion of any planned or future preclinical studies or clinical trials of our current or future drug candidates, our expenses could increase and profitability could be further delayed.
Even if we do achieve profitability, we may not be able to sustain or increase profitability on a quarterly or annual basis. Our failure to become and remain profitable would decrease the value of our company and could impair our ability to raise capital, maintain our research and development efforts, expand our business or continue our operations. A decline in the value of our company also could cause investors to lose all or part of your investment.
We will need substantial additional funding, and if we are unable to raise capital when needed, we could be forced to delay, reduce or eliminate our drug development programs or commercialization efforts.
We anticipate that our expenses will increase substantially as we continue to develop and begin and continue clinical trials with respect to LP-184, LP-300 and our other drug candidates; seek to identify and develop additional drug candidates; acquire or in-license other drug candidates or technologies; seek regulatory and marketing approvals for our drug candidates that successfully complete clinical trials, if any; establish sales, marketing, distribution and other commercial infrastructure in the future to commercialize various drugs for which we may obtain marketing approval, if any; require the manufacture of larger quantities of drug candidates for clinical development and, potentially, commercialization; maintain, expand and protect our intellectual property portfolio; develop, maintain, and expand our RADR® platform; hire and retain additional personnel, such as clinical, quality control and scientific personnel; add operational, financial and management information systems and personnel, including personnel to support our drug development and help us comply with our obligations as a public company; and add equipment and physical infrastructure to support our research and development programs.
We will be required to expend significant funds in order to advance the development of LP-184, LP-300 and our other drug candidates. In addition, while we may seek one or more collaborators for future development of our current drug candidates or any future drug candidates that we may develop for one or more indications, we may not be able to enter into a partnership or out-license for any of our drug candidates for such indications on suitable terms, on a timely basis or at all. In any event, our existing cash, cash equivalents and other capital resources will not be sufficient to fund all of the efforts that we plan to undertake or to fund the completion of development of our drug candidates or our other preclinical studies. Accordingly, we will be required to obtain further funding through public or private equity offerings, debt financings, collaborations and licensing arrangements or other sources. We do not have any committed external source of funds. Further financing may not be available to us on acceptable terms, or at all. Our failure to raise capital as and when needed would have a negative impact on our financial condition and our ability to pursue our business strategy.
We believe our existing cash and cash equivalents as of December 31, 2020, plus approximately $64,200,000 of net proceeds from our public offering of common shares in January 2021, along with our anticipated expenditures and commitments for calendar year 2021, will enable us to fund our operating expenses and capital expenditure requirements for at least 12 months from the filing of this Form 10-K for the year ended December 31, 2020. Our estimate as to how long we expect our existing cash, cash equivalents and other capital resources to be able to continue to fund our operations is based on assumptions that may prove to be wrong, and we could use our available capital resources sooner than we currently expect. Further, changing circumstances, some of which may be beyond our control, could cause us to consume capital significantly faster than we currently anticipate, and we may need to seek additional funds sooner than planned. Our future funding requirements, both short-term and long-term, will depend on many factors, including:
| ● | the scope, progress, timing, costs and results of preclinical studies and clinical trials of LP-184, LP-300 and our other drug candidates; |
| ● | the costs associated with maintaining, expanding and updating our RADR® platform; |
| ● | the costs, timing and outcome of seeking regulatory approvals; |
67
| ● | our headcount growth and associated costs as we expand our research and development as well as potentially establish a commercial infrastructure; |
| ● | the costs of our licensing or commercialization activities for any of our drug candidates that receive marketing approval to the extent such costs are not the responsibility of any future collaborators, including the costs and timing of establishing drug sales, marketing, distribution and manufacturing capabilities; |
| ● | our ability to enter into and the terms and timing of any collaborations, licensing agreements or other arrangements; |
| ● | revenue received from commercial sales, if any, of our current and future drug candidates; |
| ● | the costs of preparing, filing and prosecuting patent applications, maintaining and protecting our intellectual property rights and defending against intellectual property related claims; |
| ● | the number of future drug candidates that we pursue and their development requirements; |
| ● | changes in regulatory policies or laws that may affect our operations; |
| ● | changes in physician acceptance or medical society recommendations that may affect commercial efforts; |
| ● | the costs of acquiring potential new drug candidates or technology; |
| ● | the costs associated with purchasing data for our RADR® platform; |
| ● | the costs associated with maintaining and expanding our cybersecurity systems; and |
| ● | the costs of operating as a public company. |
Risks Related to the Discovery and Development of Drug Candidates
We have limited experience in drug discovery and drug development and may not receive regulatory approval to market our drug candidates.
Prior to the acquisition of our drug candidates, we were not involved in and had no control over their preclinical and clinical development. In addition, we rely upon the parties from whom we have acquired our drug candidates from to have conducted such research and development in accordance with the applicable protocol, legal, regulatory and scientific standards, having accurately reported the results of all clinical trials conducted prior to our acquisition of the applicable drug candidate, and having correctly collected the data from these studies and trials. To the extent any of these has not occurred, our expected development time and costs may be increased, which could adversely affect our prospects for marketing approval of, and receiving any future revenue from, these drug candidates.
In the near term, we are dependent on our ability to advance the development of LP-184 and LP-300 and on the efforts of Allarity Therapeutics to advance LP-100. If we are unable to initiate or complete the clinical development of, obtain marketing approval for or successfully commercialize LP-184 and LP-300 and our other drug candidates, either alone or with a collaborator, or if we experience significant delays in doing so, our business could be substantially harmed.
We currently do not have any drugs that have received regulatory approval and may never be able to develop marketable drug candidates. We are investing a significant portion of our efforts and financial resources in the advancement of LP-184, LP-300 and our other drug candidates and in the development of our RADR® platform. Our prospects are substantially dependent on our ability, or those of any future collaborator, to develop, obtain marketing approval for and successfully commercialize drug candidates in one or more disease indications.
68
The success of LP-184, LP-300 and our other drug candidates will depend on several factors, including the following:
| ● | following submission of an Investigational New Drug Application, or IND, with the FDA or any comparable foreign regulatory authority, receiving clearance for the conduct of clinical trials of drug candidates and proposed design of future clinical trials; |
| ● | initiation, progress, timing, costs and results of clinical trials of our drug candidates and potential drug candidates; |
| ● | establishment of a safety, tolerability and efficacy profile that is satisfactory to the FDA or any comparable foreign regulatory authority for marketing approval; |
| ● | adequate ongoing availability of quality data sources for our RADR® platform and raw materials and drug product for clinical development and any commercial sales; |
| ● | obtaining and maintaining patent, trade secret protection and regulatory exclusivity, both in the United States and relevant global markets; |
| ● | the performance of our future collaborators, if any; |
| ● | the extent of any required post-marketing approval commitments to applicable regulatory authorities; |
| ● | establishment of supply arrangements with third-party raw materials suppliers and manufacturers; |
| ● | establishment of arrangements with third-party manufacturers to obtain finished drug product that is appropriately packaged for sale; |
| ● | protection of our rights in our intellectual property portfolio; |
| ● | successful launch of commercial sales following any marketing approval; |
| ● | a continued acceptable safety profile following any marketing approval; |
| ● | commercial acceptance by patients, the medical community and third-party payors; and |
| ● | our ability to compete with other therapies. |
Many of these factors are beyond our control, including the results of clinical trials, the time required for the FDA or any comparable foreign regulatory authorities to review any regulatory submissions we may make, potential threats to our intellectual property rights and the manufacturing, marketing and sales efforts of any future collaborator. If we are unable to develop, receive marketing approval for and successfully commercialize LP-300 and LP-184 our other drug candidates, on our own or with any future collaborator or experience delays as a result of any of these factors or otherwise, our business could be substantially harmed. The regulatory approval processes of the FDA and comparable foreign authorities are lengthy, time consuming, expensive and inherently unpredictable, and if we are ultimately unable to obtain regulatory approval for our drug candidates, our business will be substantially harmed.
The time required to obtain approval by the FDA and comparable foreign authorities is unpredictable but can take many years following the commencement of clinical trials and depends upon numerous factors, including the substantial discretion of the regulatory authorities. The results of preclinical studies and early clinical trials of our drug candidates may not be predictive of the results of later-stage clinical trials. Drug candidates in later stages of clinical trials may fail to show the desired safety and efficacy traits despite having progressed through preclinical studies and initial clinical trials. It is not uncommon for companies in the biotechnology and pharmaceutical industries to suffer significant setbacks in advanced clinical trials due to nonclinical findings made while clinical studies were underway and safety or efficacy observations made in clinical studies, including previously unreported adverse events. Our future clinical trial results may not be successful, and notwithstanding any potential promising results in earlier studies, we cannot be certain that we will not face similar setbacks. The historical failure rate for drug candidates in our industry is high. In addition, approval policies, regulations, or the type and amount of clinical data necessary to gain approval may change during the course of a drug candidate’s clinical development and may vary among jurisdictions. We have not obtained final regulatory approval for any drug candidate and it is possible that none of our existing drug candidates or any drug candidates we may seek to develop in the future will ever obtain regulatory approval.
69
Our drug candidates could fail to receive regulatory clearance or marketing approval for many reasons, including the following:
| ● | the FDA or comparable foreign regulatory authorities may disagree with the design or implementation of our clinical trials, including, but not limited to, the use of genomic or biomarker signatures to identify patients that may respond to drug efficacy; |
| ● | we may be unable to demonstrate to the satisfaction of the FDA or comparable foreign regulatory authorities that a drug candidate is safe and effective for its proposed indication; |
| ● | we may be unable to identify and recruit a sufficient number of patients with relevant genomic or biomarker signatures in order to conduct clinical trials on our drug candidates; |
| ● | the results of clinical trials may not meet the level of statistical significance required by the FDA or comparable foreign regulatory authorities for approval; |
| ● | the FDA or comparable foreign regulatory authorities may disagree with our interpretation of data from preclinical studies or clinical trials; |
| ● | the data collected from clinical trials of our drug candidates may not be sufficient to support the submission of a New Drug Application, or NDA, or other submission or to obtain regulatory approval in the United States or elsewhere; |
| ● | the FDA or comparable foreign regulatory authorities may fail to approve the manufacturing processes or facilities of third-party manufacturers with which we contract for clinical and commercial supplies; and |
| ● | the approval policies or regulations of the FDA or comparable foreign regulatory authorities may significantly change in a manner rendering our clinical data insufficient for approval. |
We have not previously completed all clinical trials for any of our drug candidates. Consequently, we may not have the necessary capabilities, including adequate staffing, to successfully manage the execution and completion of any clinical trials we initiate in a way that leads to our obtaining marketing approval for our drug candidates in a timely manner, or at all. This lengthy approval process as well as the unpredictability of future clinical trial results may result in our failing to obtain regulatory approval to market our drug candidates, which would significantly harm our business, results of operations and prospects.
In addition, even if we were to obtain approval, regulatory authorities may approve any of our drug candidates for fewer or more limited indications than we request, may not approve the price we intend to charge for our drugs, may grant approval contingent on the performance of costly post-marketing clinical trials, may approve a drug candidate with a label that does not include the labeling claims necessary or desirable for the successful commercialization of that drug candidate or may restrict its distribution. Any of the foregoing restrictions or requirements could materially harm the commercial prospects for our drug candidates.
We have not previously submitted a new drug application (an “NDA”) to the FDA or similar drug approval filings to comparable foreign authorities, for any drug candidate, and we cannot be certain that any of our drug candidates will be successful in clinical trials or receive regulatory approval. Further, our drug candidates may not receive regulatory approval even if they are successful in clinical trials. If we do not receive regulatory approvals for our drug candidates, we may not be able to continue our operations. Even if we successfully obtain regulatory approvals to market one or more of our drug candidates, our revenues will be dependent, in part, upon the size of the markets in the territories for which we gain regulatory approval and have commercial rights. If the markets for patients that we are targeting for our drug candidates are not as significant as we estimate, or if the price we charge for our drug candidate is too high, we may not generate significant revenues from sales of such drugs, if approved.
70
We plan to seek regulatory approval to commercialize our drug candidates both in the United States and the European Union and in additional foreign countries. While the scope of regulatory approval is similar in other countries, to obtain separate regulatory approval in many other countries we must comply with numerous and varying regulatory requirements of such countries regarding safety and efficacy and governing, among other things, clinical trials and possible limitations placed upon commercial sales, pricing and distribution of our drug candidates, and we cannot predict success in these jurisdictions.
Our business strategy to rescue previously failed drug candidates may not be successful, and important issues relating to safety and efficacy remain to be resolved for all of our drug candidates. Our strategy also involves risks and uncertainties that differ from other biotechnology companies that focus solely on new drug candidates that do not have a history of failed clinical trials.
Our drug candidate portfolio includes small molecules that others have tried, but failed, to develop into an approved commercialized drug. Our strategy to rescue previously failed drug candidates may not be successful, and the use of the term “drug rescue,” “rescuing,” or words of similar meaning in this report should not be construed to mean that our RADR® platform has resolved all issues of safety and/or efficacy for any of our drug candidates. Issues of safety and efficacy for any drug candidate may only be determined by the U.S. FDA or other applicable regulatory authorities in jurisdictions outside the United States.
Our business strategy includes a focus on leveraging A.I. to streamline the drug development process and to identify patients that will benefit from drug candidates that other biotechnology or pharmaceutical companies have abandoned or shelved after initiating clinical trials under an IND application filed with the FDA, including candidates that have failed to achieve statistical significance on the original endpoints established in the clinical trials. We use our RADR®platform to assess drug candidates together with big data sources of information to both target and evaluate sub-populations and identify new therapeutic indices and gene signatures that will potentially correlate with drug efficacy and patient response to treatment. While we have not yet successfully received regulatory or marketing approval for any of our drug candidates, and while we believe that our approach has the potential to reduce the cost and time of drug development through the identification and selection of patient populations more likely to respond to therapy, our strategy involves risks and uncertainties that differ from other biotechnology companies that focus solely on new drug candidates that do not have a history of failed clinical development. These risks and uncertainties include, but are not limited to, the following:
| ● | The remaining term of the initial patents filed with respect to a rescued and repositioned drug candidate may be significantly less than the patent term for a newly discovered drug candidate; |
| ● | Potential out-licensees, alliance partners and collaborators may view a rescued and repositioned drug candidate with more skepticism because of its history of failed clinical trials, thereby requiring a higher level of additional data and further explanations of mechanisms of action in order to overcome this skepticism and obtain commercially reasonable terms for future development or collaboration; |
| ● | Key personnel and institutional knowledge relating to a rescued and repositioned drug candidate may no longer be available for us; |
| ● | The current standard of care in the targeted therapeutic indication for the rescued and repositioned drug candidate may be different than the standard of care that existed during the candidate’s last clinical trial, which will require more time and resources from us to reassess and redesign the regulatory development path for the rescued and repositioned drug candidate; and |
| ● | The rescued and repositioned drug candidate may be perceived to be in an “older” therapeutic focus area of oncology, thereby generating less enthusiasm and support compared to therapeutic focus areas of oncology that may be perceived as more recent. |
71
We are dependent on Allarity Therapeutics for the development of LP-100.
We, with the consent of our licensor for LP-100, AF Chemicals, have entered into an agreement with Allarity Therapeutics in which we have granted an exclusive, royalty-bearing license, with the right to sublicense, to develop LP-100. Allarity Therapeutics will be solely responsible for the development of LP-100, including development of a comprehensive plan for a clinical trial program, but has the right to assign all or part of the agreement to a third-party program acquirer. Under the agreement, we and AF Chemicals, are entitled to receive certain specified milestone payments from Allarity Therapeutics subject to an overall aggregate maximum payment of $21 million U.S. dollars ($21,000,000) with certain exceptions. In addition to milestone payments, we are also entitled to receive royalty payments based on incremental levels of annual sales of LP-100 products by Allarity Therapeutics or any third-party program acquirer. As a result of the drug license and development agreement with Allarity Therapeutics, we are completely dependent on Allarity Therapeutics for the development of LP-100. Allarity Therapeutics is managing a Phase II clinical trial of LP-100 in patients with mCRPC. Continuing enrollment for this Phase II clinical trial has slowed during the COVID-19 pandemic. Allarity Therapeutics has also stated that it is focusing its existing resources on other programs that are currently higher priority for Allarity than LP-100. As of the date of this report, we are unable to forecast the timeline for the completion of the Phase II clinical trial.
We may depend on enrollment of patients with specific genomic or biomarker signatures in our clinical trials in order for us to continue development of our drug candidates. If we are unable to enroll patients with specific genomic or biomarker signatures in our clinical trials, our research, development and commercialization efforts could be adversely affected.
The timely completion of clinical trials in accordance with their protocols depends, among other things, on our ability to enroll a sufficient number of patients with genomic or biomarker signatures we have identified and who remain in the study until its conclusion. We may experience difficulties in patient enrollment in our clinical trials for a variety of reasons. Patient enrollment is affected by many factors including the size and nature of the patient population with the specific genomic or biomarker signature we have identified, the proximity of patients to clinical sites, the eligibility criteria for the trial, the design of the clinical trial, the size of the patient population required for analysis of the trial’s primary endpoints, the proximity of patients to study sites, our ability to recruit clinical trial investigators with the appropriate competencies and experience, our ability to obtain and maintain patient consents, the risk that patients enrolled in clinical trials will drop out of the trials before completion, and competing clinical trials and clinicians’ and patients’ perceptions as to the potential advantages of the drug being studied in relation to other available therapies, including any new drugs that may be approved for the indications we are investigating. We will compete with other pharmaceutical companies for clinical sites, physicians and the limited number of patients who fulfill the stringent requirements for participation in oncology clinical trials. Also, due to the confidential nature of clinical trials, we do not know how many of the eligible patients may be enrolled in competing studies and who are consequently not available to us for our clinical trials. Our clinical trials may be delayed or terminated due to the inability to enroll enough patients. The delay or inability to meet planned patient enrollment may result in increased costs and delay or termination of our trials, which could have a harmful effect on our ability to develop drugs.
Delays in clinical testing could result in increased costs to us and delay our ability to generate revenue.
Although we are planning for certain clinical trials relating to LP-300 and LP-184 and our other drug candidates, there can be no assurance that the FDA will accept our proposed trial designs. We may experience delays in our clinical trials and we do not know whether planned clinical trials will begin on time, need to be redesigned, enroll patients on time or be completed on schedule, if at all. Clinical trials can be delayed for a variety of reasons, including delays related to:
| ● | obtaining regulatory clearance to commence a trial; |
| ● | reaching agreement on acceptable terms with prospective contract research organizations, or CROs, and clinical trial sites, the terms of which can be subject to extensive negotiation and may vary significantly among different CROs and trial sites; |
| ● |
obtaining institutional review board, or IRB, approval at each site; | |
| ● | recruiting suitable patients to participate in a trial; |
72
| ● | identifying clinical sites with adequate infrastructure (including data collection) to conduct the trial; |
| ● | clinical sites deviating from trial protocol or dropping out of a trial; |
| ● | addressing patient safety concerns that arise during the course of a trial; |
| ● | having patients complete a trial or return for post-treatment follow-up; |
| ● | adding a sufficient number of clinical trial sites; or |
| ● | manufacturing sufficient quantities and quality of a drug candidate for use in clinical trials. |
We may also experience numerous unforeseen events during, or as a result of, clinical trials that could delay or prevent our ability to receive marketing approval or commercialize our drug candidates, including:
| ● | we may receive feedback from regulatory authorities that requires us to modify the design of our clinical trials; |
| ● | we may not have the ability to test patients for our clinical trials that require a specific genomic or biomarker signature in order to qualify for enrollment; |
| ● | clinical trials of our drug candidates may produce negative or inconclusive results, and we may decide, or regulators may require us, to conduct additional clinical trials or abandon drug development programs; |
| ● | the number of patients required for clinical trials of our drug candidates may be larger than we anticipate, enrollment in these clinical trials may be slower than we anticipate or participants may drop out of these clinical trials at a higher rate than we anticipate; |
| ● | our third-party contractors may fail to comply with regulatory requirements or meet their contractual obligations to us in a timely manner, or at all; |
| ● | the cost of clinical trials of our drug candidates may be greater than we anticipate; |
| ● | the supply or quality of our drug candidates or other materials necessary to conduct clinical trials of our drug candidates may be insufficient or inadequate; |
| ● | regulators may revise the requirements for approving our drug candidates, or such requirements may not be as we anticipate; and |
| ● | any future collaborators that conduct clinical trials may face any of the above issues, and may conduct clinical trials in ways they view as advantageous to themselves but that are suboptimal for us. |
If we are required to conduct additional clinical trials or other testing of our drug candidates beyond those that we currently contemplate, if we are unable to successfully complete clinical trials of our drug candidates or other testing, if the results of these trials or tests are not positive or are only modestly positive or if there are safety concerns, we may:
| ● | incur unplanned costs; |
| ● | be delayed in obtaining marketing approval for our drug candidates or not obtain marketing approval at all; |
| ● | obtain marketing approval in some countries and not in others; |
| ● | obtain marketing approval for indications or patient populations that are not as broad as intended or desired; |
| ● | obtain marketing approval with labeling that includes significant use or distribution restrictions or safety warnings, including boxed warnings; |
| ● | be subject to additional post-marketing testing requirements; or |
| ● | have the drug removed from the market after obtaining marketing approval. |
73
Furthermore, we intend to rely on CROs, cancer research centers and clinical trial sites to ensure the proper and timely conduct of our clinical trials and we intend to have agreements governing their committed activities. They may not perform as required or we may face competition from other clinical trials being conducted by other pharmaceutical companies.
We could encounter delays if a clinical trial is suspended or terminated by us, by the Institutional Review Board or IRB of the institutions in which such trials are being conducted, by the Data Safety Monitoring Board, or DSMB, for such trial or by the FDA or other regulatory authorities. Such authorities may impose such a suspension or termination due to a number of factors, including failure to conduct the clinical trial in accordance with regulatory requirements or our clinical protocols, inspection of the clinical trial operations or trial site by the FDA or other regulatory authorities resulting in the imposition of a clinical hold, unforeseen safety issues or adverse side effects, failure to demonstrate a benefit from using a drug, changes in governmental regulations or administrative actions or lack of adequate funding to continue the clinical trial.
Further, conducting clinical trials in foreign countries, as we may do for our current and future drug candidates, presents additional risks that may delay completion of our clinical trials. These risks include the failure of enrolled patients in foreign countries to adhere to clinical protocol as a result of differences in healthcare services or cultural customs, managing additional administrative burdens associated with foreign regulatory schemes, as well as political and economic risks relevant to such foreign countries.
If we experience delays in the completion of, or termination of, any clinical trial of our drug candidates, the commercial prospects of our drug candidates will be harmed, and our ability to generate revenues from any of these drug candidates will be delayed. In addition, any delays in completing our clinical trials will increase our costs, slow down our drug candidate development and approval process and jeopardize our ability to commence drug sales and generate revenues. Any of these occurrences may harm our business, financial condition and prospects significantly. In addition, many of the factors that cause, or lead to, a delay in the commencement or completion of clinical trials may also ultimately lead to the denial of regulatory approval of our drug candidates.
Our drug candidates may cause undesirable side effects or have other properties that could delay or prevent their regulatory approval, limit the commercial profile of an approved label, or result in significant negative consequences following marketing approval, if any.
Undesirable side effects caused by our drug candidates could cause us or regulatory authorities to interrupt, delay or halt clinical trials and could result in a more restrictive label or the delay or denial of regulatory approval by the FDA or other comparable foreign authorities. The clinical evaluation of LP-184 and our other drug candidates in patients is still in the early stages and it is possible that there may be side effects associated with their use. In such an event, we, the FDA, the IRBs at the institutions in which our studies are conducted, or the DSMB could suspend or terminate our clinical trials or the FDA or comparable foreign regulatory authorities could order us to cease clinical trials or deny approval of our drug candidates for any or all targeted indications. Treatment-related side effects could also affect patient recruitment or the ability of enrolled patients to complete the clinical trial or result in potential product liability claims. In addition, these side effects may not be appropriately recognized or managed by the treating medical staff. We expect to have to train medical personnel using our drug candidates to understand the side effect profiles for our clinical trials and upon any commercialization of any of our drug candidates. Inadequate training in recognizing or managing the potential side effects of our drug candidates could result in patient injury or death. Any of these occurrences may harm our business, financial condition and prospects significantly.
74
Additionally, if one or more of our drug candidates receives marketing approval, and we or others later identify undesirable side effects caused by such drugs, a number of potentially significant negative consequences could result, including:
| ● | regulatory authorities may withdraw approvals of such drugs; |
| ● | we may be required to recall a drug or change the way such a drug is administered to patients; |
| ● | additional restrictions may be imposed on the marketing or distribution of the particular drug or the manufacturing processes for the drug or any component thereof; |
| ● | regulatory authorities may require additional warnings on the label, such as a “black box” warning or contraindication; |
| ● | we may be required to implement Risk Evaluation and Mitigation Strategies, or REMS, or create a medication guide outlining the risks of such side effects for distribution to patients; |
| ● | we could be sued and held liable for harm caused to patients; |
| ● | our drug may become less competitive; and |
| ● | our reputation may suffer. |
Any of these events could prevent us from achieving or maintaining market acceptance of the particular drug candidate or for particular indications of a drug candidate, if approved, and could significantly harm our business, results of operations and prospects. Our approach to the discovery and development of drug candidates based on our RADR® platform is innovative and in the early stages of development; and we do not know whether we will be able to develop any drugs of commercial value.
We are leveraging our RADR® platform in an attempt to create a pipeline of drug candidates using biomarker identification and patient stratification for the development of oncology drugs. While we believe that applying our RADR® platform to drugs that have failed, been abandoned or otherwise failed to meet clinical endpoints and then developing a precision oncology approach that identifies the mechanism of action, potential combination drug usage and potentially responsive patient population is a powerful strategy, our approach is both innovative and in the early stages of development. Because our approach is both innovative and in the early stages of development, the cost and time needed to develop our drug candidates is difficult to predict, and our efforts may not result in the successful discovery and development of commercially viable medicines. We may also be incorrect about the effects of our drug candidates on the diseases of our defined patient populations, which may limit the utility of our approach or the perception of the utility of our approach. Furthermore, our estimates of our defined patient populations available for study and treatment may be lower than expected, which could adversely affect our ability to conduct clinical trials and may also adversely affect the size of any market for medicines we may successfully commercialize. Our approach may not result in time savings, higher success rates or reduced costs as we expect it to, and if not, we may not attract collaborators or develop new drugs as quickly or cost effectively as expected and therefore we may not be able to commercialize our approach as originally expected.
Our RADR® platform may fail to help us discover and develop additional potential drug candidates.
Any drug discovery or drug development that we are conducting using our RADR® platform may not be successful in identifying compounds that have commercial value or therapeutic utility. Our RADR® platform may initially show promise in identifying potential drug candidates, yet fail to yield viable drug candidates for clinical development or commercialization for a number of reasons, including:
| ● | research programs to identify new drug candidates will require substantial technical, financial and human resources, and we may be unsuccessful in our efforts to identify new drug candidates. If we are unable to identify suitable additional compounds for preclinical and clinical development, our ability to develop drug candidates and obtain product revenues in future periods could be compromised, which could result in significant harm to our financial position and adversely impact our stock price; |
| ● | compounds identified through our RADR® platform may not demonstrate efficacy, safety or tolerability; |
75
| ● | the data available for our RADR® platform that seeks to correlate genomic or biomarker signatures with certain cancers may be influenced by the race of the patient which may limit the efficacy of our drug candidates; |
| ● | potential drug candidates may, on further study, be shown to have harmful side effects or other characteristics that indicate that they are unlikely to receive marketing approval and achieve market acceptance; |
| ● | competitors may develop alternative therapies that render our potential drug candidates non-competitive or less attractive; or |
| ● | a potential drug candidate may not be capable of being produced at an acceptable cost. |
Any failure by us to comply with existing regulations could harm our reputation and operating results.
We will be subject to extensive regulation by U.S. federal and state and foreign governments in each of the markets where we intend to sell LP-300 and LP-184 if and after they are approved. For example, we will have to adhere to all regulatory requirements including the FDA’s current GCPs, Good Laboratory Practice, or GLP, and GMP requirements. If we fail to comply with applicable regulations, including FDA pre-or post- approval cGMP requirements, then the FDA or other foreign regulatory authorities could sanction us. Even if a drug is FDA-approved, regulatory authorities may impose significant restrictions on a drug’s indicated uses or marketing or impose ongoing requirements for potentially costly post-marketing studies.
Any action against us for violation of these laws, even if we successfully defend against it, could cause us to incur significant legal expenses, divert our management’s attention from the operation of our business and damage our reputation. We will need to expend significant resources on compliance efforts and such expenses are unpredictable and might adversely affect our results.
The FDA’s and other regulatory authorities’ policies may change and additional government regulations may be enacted that could prevent, limit or delay regulatory approval of our drug candidates. For example, in December 2016, the 21st Century Cures Act, or Cures Act, was signed into law. The Cures Act, among other things, is intended to modernize the regulation of drugs and spur innovation, but its ultimate implementation is unclear. If we are slow or unable to adapt to changes in existing requirements or the adoption of new requirements or policies, or if we are not able to maintain regulatory compliance, we may lose any marketing approval that we may have obtained and we may not achieve or sustain profitability, which would adversely affect our business, prospects, financial condition and results of operations.
In addition, we cannot predict the likelihood, nature or extent of government regulation that may arise from future legislation or administrative or executive action, either in the United States or abroad. If future legislation or administrative or executive actions impose restrictions on FDA’s ability to engage in oversight and implementation activities in the normal course, our business may be negatively impacted. In addition, if we are slow or unable to adapt to changes in existing requirements or the adoption of new requirements or policies, or if we are not able to maintain regulatory compliance, we may lose any marketing approval that we may have obtained and we may not achieve or sustain profitability.
76
We may be subject to extensive regulations outside the United States and may not obtain marketing approvals for drugs in Europe and other jurisdictions.
In addition to regulations in the United States, should we or our collaborators pursue marketing approvals for LP-184 and LP-300 and our other drug candidates internationally, we and our collaborators will be subject to a variety of regulations in other jurisdictions governing, among other things, clinical trials and any commercial sales and distribution of our drugs. Whether or not we, or our collaborators, obtain applicable FDA regulatory clearance and marketing approval for a drug, we must obtain the requisite approvals from regulatory authorities in foreign countries prior to the commencement of clinical trials or marketing of the drug in those countries. The requirements and process governing the conduct of clinical trials, drug licensing, pricing and reimbursement vary from country to country.
We expect to pursue marketing approvals for LP-184 and LP-300 and our other drug candidates in Europe and other jurisdictions outside the United States with collaborative partners. The time and process required to obtain regulatory approvals and reimbursement in Europe and other jurisdictions may be different from those in the United States regulatory and approval in one jurisdiction does not ensure approvals in any other jurisdiction; however, negative regulatory decisions in any jurisdiction may have a negative impact on the regulatory process in other jurisdictions.
Additionally, on June 23, 2016, the electorate in the United Kingdom voted in favor of leaving the European Union, commonly referred to as Brexit. On March 29, 2017, the country formally notified the European Union of its intention to withdraw pursuant to Article 50 of the Lisbon Treaty triggering a two-year period for the United Kingdom to formally leave the European Union. Following a series of extensions to leave the European Union, on January 31, 2020, the United Kingdom officially left the European Union commencing a transition period in which the United Kingdom is required to continue to follow all European Union rules and trading relationships, but will no longer be represented in the European Parliament. During the transition period, the United Kingdom and the European Union will engage in negotiations for new trade agreements and, among other things, the regulation of their pharmaceutical industries. Since a significant proportion of the regulatory framework in the United Kingdom is derived from European Union directives and regulations, the transition period could materially impact the regulatory regime with respect to the approval of our drug candidates in the United Kingdom or the European Union. Any delay in obtaining, or an inability to obtain, any marketing approvals, as a result of Brexit or otherwise, would prevent us from commercializing our drug candidates in the United Kingdom and/or the European Union and restrict our ability to generate revenue and achieve and sustain profitability. If any of these outcomes occur, we may be forced to restrict or delay efforts to seek regulatory approval in the United Kingdom and/or European Union for our drug candidates, which could materially and adversely affect our business.
If we are found in violation of federal or state “fraud and abuse” laws, we may be required to pay a penalty and/or be suspended from participation in federal or state health care programs, which may adversely affect our business, financial condition and results of operations.
In the United States, we will be subject to various federal and state health care “fraud and abuse” laws, including anti-kickback laws, false claims laws and other laws intended to reduce fraud and abuse in federal and state health care programs, which could affect us, particularly upon successful commercialization of our drugs in the United States. The federal Anti-Kickback Statute makes it illegal for any person, including a prescription drug manufacturer (or a party acting on its behalf), to knowingly and willfully solicit, receive, offer or pay any remuneration that is intended to induce the referral of business, including the purchase, order or prescription of a particular drug for which payment may be made under a federal health care program, such as Medicare or Medicaid. Under federal government regulations, some arrangements, known as safe harbors, are deemed not to violate the federal Anti-Kickback Statute. Although we seek to structure our business arrangements in compliance with all applicable requirements, these laws are broadly written, and it is often difficult to determine precisely how the law will be applied in specific circumstances. Accordingly, it is possible that our practices may be challenged under the federal Anti-Kickback Statute. False claims laws prohibit anyone from knowingly and willfully presenting or causing to be presented for payment to third-party payers, including government payers, claims for reimbursed drugs or services that are false or fraudulent, claims for items or services that were not provided as claimed, or claims for medically unnecessary items or services. Cases have been brought under false claims laws alleging that off-label promotion of pharmaceutical drugs or the provision of kickbacks has resulted in the submission of false claims to governmental health care programs. Under the Health Insurance Portability and Accountability Act of 1996, we are prohibited from knowingly and willfully executing a scheme to defraud any health care benefit program, including private payers, or knowingly and willfully falsifying, concealing or covering up a material fact or making any materially false, fictitious or fraudulent statement in connection with the delivery of or payment for health care benefits, items or services. Violations of fraud and abuse laws may be punishable by criminal and/or civil sanctions, including fines and/or exclusion or suspension from federal and state health care programs such as Medicare and Medicaid and debarment from contracting with the U.S. government. In addition, private individuals have the ability to bring actions on behalf of the government under the federal False Claims Act as well as under the false claims laws of several states.
77
Many states have adopted laws similar to the federal anti-kickback statute, some of which apply to the referral of patients for health care services reimbursed by any source, not just governmental payers. Neither the government nor the courts have provided definitive guidance on the application of fraud and abuse laws to our business. Law enforcement authorities are increasingly focused on enforcing these laws, and if we are found in violation of one of these laws, we could be required to pay a penalty and could be suspended or excluded from participation in federal or state health care programs, and our business, results of operations and financial condition may be adversely affected. We may be unable to maintain sufficient clinical trial liability insurance.
Our inability to obtain and retain sufficient clinical trial liability insurance at an acceptable cost to protect against potential liability claims could prevent or inhibit our ability to conduct clinical trials for drug candidates we develop.
We currently do not have clinical trial liability insurance and would need to secure coverage before commencing patient enrollment for our clinical trials in the United States or other jurisdictions. Any claim that may be brought against us could result in a court judgment or settlement in an amount that is not covered, in whole or in part, by our insurance or that is in excess of the limits of our insurance coverage. We expect we will supplement our clinical trial coverage with product liability coverage in connection with the commercial launch of LP-184 and LP-300 or other drug candidates we develop in the future; however, we may be unable to obtain such increased coverage on acceptable terms or at all. If we are found liable in a clinical trial lawsuit or a product liability lawsuit in the future, we will have to pay any amounts awarded by a court or negotiated in a settlement that exceed our coverage limitations or that are not covered by our insurance, and we may not have, or be able to obtain, sufficient capital to pay such amounts.
The FDA and other regulatory agencies actively enforce the laws and regulations prohibiting the promotion of off-label uses.
If we are found to have improperly promoted off-label uses of our drugs or drug candidates, if approved, we may become subject to significant liability. Such enforcement has become more common in the industry. The FDA and other regulatory agencies strictly regulate the promotional claims that may be made about prescription drug products, such as our drug candidates, if approved. In particular, a drug may not be promoted for uses that are not approved by the FDA or such other regulatory agencies as reflected in the drug’s approved labeling. If we receive marketing approval for our drug candidates for our proposed indications, physicians may nevertheless use our drugs for their patients in a manner that is inconsistent with the approved label, if the physicians personally believe in their professional medical judgment it could be used in such manner. However, if we are found to have promoted our drugs for any off-label uses, the federal government could levy civil, criminal and/or administrative penalties, and seek fines against us. The FDA or other regulatory authorities could also request that we enter into a consent decree or a corporate integrity agreement, or seek a permanent injunction against us under which specified promotional conduct is monitored, changed or curtailed. If we cannot successfully manage the promotion of our drug candidates, if approved, we could become subject to significant liability, which would materially adversely affect our business and financial condition.
78
We may not experience a faster development or regulatory review or approval process with potential Fast Track designation.
If a drug is intended for the treatment of a serious condition and nonclinical or clinical data demonstrate the potential to address unmet medical need for this condition, a drug sponsor may apply for FDA Fast Track designation. If we seek Fast Track designation for a drug candidate, we may not receive it from the FDA. However, even if we receive Fast Track designation, Fast Track designation does not ensure that we will receive marketing approval or that approval will be granted within any particular timeframe. We may not experience a faster development or regulatory review or approval process with Fast Track designation compared to conventional FDA procedures. In addition, the FDA may withdraw Fast Track designation if it believes that the designation is no longer supported by data from our clinical development program. Fast Track designation alone does not guarantee qualification for the FDA’s priority review procedures.
Risks Related to Commercialization of Our Drug Candidates
Even if we are successful in completing all preclinical studies and clinical trials, we may not be successful in commercializing one or more of our drug candidates.
Even if we complete the necessary preclinical studies and clinical trials, the marketing approval process is expensive, time-consuming and uncertain and may prevent us from obtaining approvals for the commercialization of some or all of our drug candidates. If we are not able to obtain, or if there are delays in obtaining, required regulatory approvals, we will not be able to commercialize our drug candidates, and our ability to generate revenue will be materially impaired.
Our drug candidates and the activities associated with their development and commercialization, including their design, testing, manufacture, safety, efficacy, recordkeeping, labeling, storage, approval, advertising, promotion, sale and distribution, export and import are subject to comprehensive regulation by the FDA and other regulatory agencies in the United States and by the EMA and similar regulatory authorities outside of the United States. Failure to obtain marketing approval for a drug candidate will prevent us from commercializing the drug candidate. We have not submitted an application for or received marketing approval for any of our drug candidates in the United States or in any other jurisdiction.
We have only limited experience in filing and supporting the applications necessary to gain marketing approvals and expect to rely on third-party clinical research organizations or other third-party consultants or vendors to assist us in this process. Securing marketing approval requires the submission of extensive preclinical and clinical data and supporting information to regulatory authorities for each therapeutic indication to establish the drug candidate’s safety and efficacy. Securing marketing approval also requires the submission of information about the drug manufacturing process to, and inspection of manufacturing facilities by, the regulatory authorities. Our drug candidates may not be effective, may be only moderately effective or may prove to have undesirable or unintended side effects, toxicities or other characteristics that may preclude our obtaining marketing approval or prevent or limit commercial use. New cancer drugs frequently are indicated only for patient populations that have not responded to an existing therapy or have relapsed. If any of our drug candidates receives marketing approval, the accompanying label may limit the approved use of our drug in this way, which could limit sales of the drug.
The process of obtaining marketing approvals, both in the United States and abroad, is expensive, may take many years, if approval is obtained at all, and can vary substantially based upon a variety of factors, including the type, complexity and novelty of the drug candidates involved. Changes in marketing approval policies during the development period, changes in or the enactment of additional statutes or regulations, or changes in regulatory review for each submitted drug application, may cause delays in the approval or rejection of an application. Regulatory authorities have substantial discretion in the approval process and may refuse to accept any application or may decide that our data is insufficient for approval and require additional preclinical, clinical or other studies. In addition, varying interpretations of the data obtained from preclinical studies and clinical trials could delay, limit or prevent marketing approval of a drug candidate. Any marketing approval we ultimately obtain may be limited or subject to restrictions or post-approval commitments that render the approved drug not commercially viable.
79
If our drugs do not gain market acceptance, our business will suffer because we might not be able to fund future operations.
A number of factors may affect the market acceptance of our drugs or any other products we develop or acquire, including, among others:
| ● | the price of our drugs relative to other products for the same or similar treatments; |
| ● | the perception by patients, physicians and other members of the health care community of the effectiveness and safety of our drugs for their indicated applications and treatments; |
| ● | our ability to fund our sales and marketing efforts; and |
| ● | the effectiveness of our sales and marketing efforts. |
If our drugs do not gain market acceptance, we may not be able to fund future operations, including developing, testing and obtaining regulatory approval for new drug candidates and expanding our sales and marketing efforts for our approved drugs, which would cause our business to suffer.
We may rely on orphan drug status to commercialize some of our drug candidates, and even if orphan drug status is approved, such approval may not confer marketing exclusivity or other commercial advantages or expected commercial benefits.
We may rely on orphan drug exclusivity for our drug candidates. In the United States, orphan drug designation entitles a party to financial incentives such as opportunities for grant funding towards clinical trial costs, tax advantages and user-fee waivers. In addition, if a drug that has orphan drug designation subsequently receives the first FDA marketing approval for the disease for which it has such designation, the drug is entitled to orphan drug exclusivity. Orphan drug exclusivity in the United States provides that the FDA may not approve any other applications, including a full NDA, to market the same drug for the same indication for seven years, and except in limited circumstances the applicable exclusivity period is ten years in Europe. The European exclusivity period can be reduced to six years if a drug no longer meets the criteria for orphan drug designation or if the drug is sufficiently profitable so that market exclusivity is no longer justified.
Even if we, or any future collaborators, obtain orphan drug designation for a drug candidate, we, or they, may not be able to obtain or maintain orphan drug exclusivity for that drug candidate. We may not be the first to obtain marketing approval of any drug candidate for which we have obtained orphan drug designation for the orphan-designated indication due to the uncertainties associated with developing pharmaceutical products, and it is possible that another company also holding orphan drug designation for the same drug candidate will receive marketing approval for the same indication before we do. If that were to happen, our applications for that indication may not be approved until the competing company’s period of exclusivity expires. In addition, exclusive marketing rights in the United States may be limited if we seek approval for an indication broader than the orphan-designated indication or may be lost if the FDA later determines that the request for designation was materially defective or if we are unable to assure sufficient quantities of the drug to meet the needs of patients with the rare disease or condition. Further, even if we, or any future collaborators, obtain orphan drug exclusivity for a drug, that exclusivity may not effectively protect the drug from competition because different drugs with different active moieties may be approved for the same condition. Even after an orphan drug is approved, the FDA can subsequently approve the same drug with the same active moiety for the same condition if the FDA concludes that the later drug is clinically superior in that it is shown to be safer, more effective or makes a major contribution to patient care or the manufacturer of the drug with orphan exclusivity is unable to maintain sufficient drug quantity. Orphan drug designation neither shortens the development time or regulatory review time of a drug nor gives the drug any advantage in the regulatory review or approval process, nor does it prevent competitors from obtaining approval of the same drug candidate as ours for indications other than those in which we have been granted orphan drug designation.
On August 3, 2017, the U.S. Congress passed the FDA Reauthorization Act of 2017, or FDARA. FDARA, among other things, codified the FDA’s preexisting regulatory interpretation, to require that a drug sponsor demonstrate the clinical superiority of an orphan drug that is otherwise the same as a previously approved drug for the same rare disease in order to receive orphan drug exclusivity. The new legislation reverses prior precedent holding that the Orphan Drug Act unambiguously requires that the FDA recognize the orphan exclusivity period regardless of a showing of clinical superiority. The FDA may further reevaluate the Orphan Drug Act and its regulations and policies. We do not know if, when or how the FDA may change the orphan drug regulations and policies in the future, and it is uncertain how any changes might affect our business. Depending on what changes the FDA may make to its orphan drug regulations and policies, our business could be adversely impacted.
80
A Breakthrough Therapy designation by the FDA for our drug candidates may not lead to a faster development or regulatory review or approval process, and it does not increase the likelihood that our drug candidates will receive marketing approval.
We may seek a breakthrough therapy designation for some of our drug candidates. A breakthrough therapy is defined as a drug that is intended, alone or in combination with one or more other drugs, to treat a serious or life-threatening disease or condition, and preliminary clinical evidence indicates that the drug may demonstrate substantial improvement over existing therapies on one or more clinically significant endpoints, such as substantial treatment effects observed early in clinical development. For drugs and biologics that have been designated as breakthrough therapies, interaction and communication between the FDA and the sponsor of the trial can help to identify the most efficient path for clinical development while minimizing the number of patients placed in ineffective control regimens. Drugs designated as breakthrough therapies by the FDA are also eligible for accelerated approval.
Designation as a breakthrough therapy is within the discretion of the FDA. Accordingly, even if we believe one of our drug candidates meets the criteria for designation as a breakthrough therapy, the FDA may disagree and instead determine not to make such designation. Even if we receive Breakthrough Therapy designation, the receipt of such designation for a drug candidate may not result in a faster development process, review or approval compared to drugs considered for approval under conventional FDA procedures and does not assure ultimate approval by the FDA. In addition, even if one or more of our drug candidates qualify as breakthrough therapies, the FDA may later decide that the drugs no longer meet the conditions for qualification or decide that the time period for FDA review or approval will not be shortened.
A Fast Track designation by the FDA may not lead to a faster development or regulatory review or approval process.
We may seek Fast Track designation for some of our drug candidates. If a drug is intended for the treatment of a serious or life-threatening condition and the drug demonstrates the potential to address unmet medical needs for this condition, the drug sponsor may apply for FDA Fast Track designation. The FDA has broad discretion whether or not to grant this designation, so even if we believe a particular drug candidate is eligible for this designation, we cannot assure you that the FDA would decide to grant it. Even if we do receive Fast Track designation, we may not experience a faster development process, review or approval compared to conventional FDA procedures. The FDA may withdraw Fast Track designation if it believes that the designation is no longer supported by data from our clinical development program.
Failure to obtain marketing approval in foreign jurisdictions would prevent our drug candidates from being marketed abroad.
In order to market and sell our drugs in the European Union and many other foreign jurisdictions, we or our potential third-party collaborators must obtain separate marketing approvals and comply with numerous and varying regulatory requirements. The approval procedure varies among countries and can involve additional testing. The time required to obtain approval may differ substantially from that required to obtain FDA marketing approval. The regulatory approval process outside of the United States generally includes all of the risks associated with obtaining FDA approval. In addition, in many countries outside of the United States, it is required that the drug be approved for reimbursement before the drug can be approved for sale in that country. We or our potential third-party collaborators may not obtain approvals from regulatory authorities outside of the United States on a timely basis, if at all. Approval by the FDA does not ensure approval by regulatory authorities in other countries or jurisdictions, and approval by one regulatory authority outside of the United States does not ensure approval by regulatory authorities in other countries or jurisdictions or by the FDA. However, a failure or delay in obtaining regulatory approval in one country may have a negative effect on the regulatory process in other countries. We may not be able to file for marketing approvals and may not receive necessary approvals to commercialize our drugs in any market.
81
If we are required by the FDA to obtain approval of a companion diagnostic in connection with approval of a therapeutic drug candidate, and we do not obtain or face delays in obtaining FDA approval of a diagnostic device, we will not be able to commercialize the drug candidate and our ability to generate revenue will be materially impaired.
According to FDA guidance, if the FDA determines that a companion diagnostic device is essential to the safe and effective use of a novel therapeutic drug or indication, the FDA generally will not approve the therapeutic drug or new therapeutic drug indication if the companion diagnostic is not also approved or cleared for that indication. Under the Federal Food, Drug, and Cosmetic Act, or FDCA, companion diagnostics are regulated as medical devices, and the FDA has generally required companion diagnostics intended to select the patients who will respond to cancer treatment to obtain Premarket Approval, or a PMA, for the diagnostic. The PMA process, including the gathering of clinical and preclinical data and the submission to and review by the FDA, involves a rigorous premarket review during which the applicant must prepare and provide the FDA with reasonable assurance of the device’s safety and effectiveness and information about the device and its components regarding, among other things, device design, manufacturing and labeling. A PMA is not guaranteed and may take considerable time, and the FDA may ultimately respond to a PMA submission with a “not approvable” determination based on deficiencies in the application and require additional clinical trial or other data that may be expensive and time-consuming to generate and that can substantially delay approval. As a result, if we are required by the FDA to obtain approval of a companion diagnostic for a therapeutic drug candidate, and we do not obtain or there are delays in obtaining FDA approval of a diagnostic device, we may not be able to commercialize the drug candidate on a timely basis or at all and our ability to generate revenue will be materially impaired.
While it is possible that one or more of our drug candidates may require a companion diagnostic to select the patients who will likely respond to a cancer therapy involving one of our drug candidates that would require a PMA for the companion diagnostic as a condition to obtaining marketing approval from the FDA, it is too early in our drug candidates development to identify which drug candidate, if any, would require a PMA.
Any drug candidate that we obtain marketing approval for could be subject to post-marketing restrictions or withdrawal from the market and we may be subject to substantial penalties if we fail to comply with regulatory requirements or if we experience unanticipated problems with our drugs, when and if any of them are approved.
Any drug candidate for which we obtain marketing approval, along with the manufacturing processes, post-approval clinical data, labeling, advertising and promotional activities for such drug, will be subject to continual requirements of and review by the FDA and other regulatory authorities. These requirements include submissions of safety and other post-marketing information and reports, registration and listing requirements, cGMP requirements relating to manufacturing, quality control, quality assurance and corresponding maintenance of records and documents, requirements regarding the distribution of samples to physicians and recordkeeping. Even if marketing approval of a drug candidate is granted, the approval may be subject to limitations on the indicated uses for which the drug may be marketed or to the conditions of approval, including the requirement to implement a REMS. New cancer drugs frequently are indicated only for patient populations that have not responded to an existing therapy or have relapsed. If any of our drug candidates receives marketing approval, the accompanying label may limit the approved use of our drug in this way, which could limit sales of the drug.
The FDA may also impose requirements for costly post-marketing studies or clinical trials and surveillance to monitor the safety or efficacy of the drug, including the adoption and implementation of REMS. The FDA and other agencies, including the Department of Justice, or the DOJ, closely regulate and monitor the post-approval marketing and promotion of drugs to ensure they are marketed and distributed only for the approved indications and in accordance with the provisions of the approved labeling. The FDA and DOJ impose stringent restrictions on manufacturers’ communications regarding off-label use, and if we do not market our drugs for their approved indications, we may be subject to enforcement action for off-label marketing. Violations of the FDCA and other statutes, including the False Claims Act, relating to the promotion and advertising of prescription drugs may lead to investigations and enforcement actions alleging violations of federal and state healthcare fraud and abuse laws, as well as state consumer protection laws.
82
In addition, later discovery of previously unknown adverse events or other problems with our drugs, manufacturers or manufacturing processes, or failure to comply with regulatory requirements, may have various consequences, including:
| ● | restrictions on such drugs, manufacturers or manufacturing processes; |
| ● | restrictions and warnings on the labeling or marketing of a drug; |
| ● | restrictions on drug distribution or use; |
| ● | requirements to conduct post-marketing studies or clinical trials; |
| ● | warning letters or untitled letters; |
| ● | withdrawal of the drugs from the market; |
| ● | refusal to approve pending applications or supplements to approved applications that we submit; |
| ● | recall of drugs; |
| ● | fines, restitution or disgorgement of profits or revenues; |
| ● | suspension or withdrawal of marketing approvals; |
| ● | damage to relationships with any potential collaborators; |
| ● | unfavorable press coverage and damage to our reputation; |
| ● | refusal to permit the import or export of our drugs; |
| ● | drug seizure; |
| ● | injunctions or the imposition of civil or criminal penalties; or |
| ● | litigation involving patients using our drugs. |
Non-compliance with European Union requirements regarding safety monitoring or pharmacovigilance, and with requirements related to the development of drugs for the pediatric population, can also result in significant financial penalties. Similarly, failure to comply with the European Union’s requirements regarding the protection of personal information can also lead to significant penalties and sanctions.
In addition, manufacturers of approved drugs and those manufacturers’ facilities are required to comply with extensive FDA requirements, including ensuring that quality control and manufacturing procedures conform to cGMPs applicable to drug manufacturers or quality assurance standards applicable to medical device manufacturers, which include requirements relating to quality control and quality assurance as well as the corresponding maintenance of records and documentation and reporting requirements. We, any contract manufacturers we may engage in the future, our future collaborators and their contract manufacturers will also be subject to other regulatory requirements, including submissions of safety and other post-marketing information and reports, registration and listing requirements, requirements regarding the distribution of samples to clinicians, recordkeeping, and costly post-marketing studies or clinical trials and surveillance to monitor the safety or efficacy of the drug such as the requirement to implement a REMS.
83
We operate in a highly competitive and rapidly changing industry.
Biotechnological and pharmaceutical drug development is highly competitive and subject to rapid and significant technological advancements. Our success is highly dependent upon our ability to in-license, acquire, develop and obtain regulatory approval for new and innovative drugs on a cost-effective basis and to market them successfully. In doing so, we face and will continue to face intense competition from a variety of businesses, including large, fully integrated, well-established pharmaceutical companies who already possess a large share of the market, specialty pharmaceutical and biopharmaceutical companies, academic institutions, government agencies and other private and public research institutions in the United States, the European Union and other jurisdictions.
Many of the companies against which we are competing or against which we may compete in the future have significantly greater financial resources and expertise in research and development, manufacturing, preclinical testing, conducting clinical trials, obtaining regulatory approvals and marketing approved drugs than we do. These third parties compete with us in recruiting and retaining qualified scientific and management personnel, establishing clinical trial sites and patient registration for clinical trials, as well as in acquiring technologies complementary to, or necessary for, our programs. Mergers and acquisitions in the pharmaceutical and biotechnology industries could result in even more resources being concentrated among a small number of our competitors.
Competition may further increase as a result of advances in the commercial applicability of technologies and greater availability of capital for investment in these industries. Our competitors may succeed in developing, acquiring or licensing, on an exclusive basis, drugs that are more effective or less costly than any drug candidate that we may develop.
Established pharmaceutical and biotechnology companies may invest heavily to accelerate discovery and development of novel compounds or to in-license novel compounds that could make our drug candidates less competitive. In addition, any new drug that competes with an approved drug must demonstrate compelling advantages in efficacy, convenience, tolerability and safety in order to overcome price competition and to be commercially successful. Accordingly, our competitors may succeed in obtaining patent protection, discovering, developing, receiving FDA approval for or commercializing drugs before we do, which would have an adverse impact on our business and results of operations.
The availability of our competitors’ drugs could limit the demand and the price we are able to charge for any drug candidate we commercialize, if any. The inability to compete with existing or subsequently introduced drugs would harm our business, financial condition and results of operations.
If we are unable to develop satisfactory sales and marketing capabilities, we may not succeed in commercializing LP-184 and LP-300 or any other drug candidate.
We have no experience in marketing and selling drug products. We have not entered into arrangements for the sale and marketing of LP-184 and LP-300 or any other drug candidate. Typically, pharmaceutical companies would employ groups of sales representatives and associated sales and marketing staff numbering in the hundreds to thousands of individuals to call on this large number of physicians and hospitals. We may seek to collaborate with a third party to market our drugs or may seek to market and sell our drugs by ourselves. If we seek to collaborate with a third party, we cannot be sure that a collaborative agreement can be reached on terms acceptable to us. If we seek to market and sell our drugs directly, we will need to hire additional personnel skilled in marketing and sales. We cannot be sure that we will be able to acquire, or establish third party relationships to provide, any or all of these marketing and sales capabilities. The establishment of a direct sales force or a contract sales force or a combination direct and contract sales force to market our drugs will be expensive and time-consuming and could delay any drug launch. Further, we can give no assurances that we may be able to maintain a direct and/or contract sales force for any period of time or that our sales efforts will be sufficient to generate or to grow our revenues or that our sales efforts will ever lead to profits.
84
Even if we obtain regulatory approvals to commercialize LP-184 and LP-300 or our other drug candidates, our drug candidates may not be accepted by physicians or the medical community in general.
There can be no assurance that LP-184 and LP-300 and our other drug candidates or any other drug candidate successfully developed by us, independently or with partners, will be accepted by physicians, hospitals and other health care facilities. LP-184 and LP-300 and any future drug candidates we develop will compete with a number of drugs manufactured and marketed by major pharmaceutical and biotech companies. The degree of market acceptance of any drugs we develop depends on a number of factors, including:
| ● | our demonstration of the clinical efficacy and safety of LP-184 and LP-300 and our other drug candidates; |
| ● | timing of market approval and commercial launch of LP-184 and LP-300 and our other drug candidates; |
| ● | the clinical indication(s) for which LP-184 and LP-300 and our other drug candidates are approved; |
| ● | drug label and package insert requirements; |
| ● | advantages and disadvantages of our drug candidates compared to existing |
| ● | continued interest in and growth of the market for anticancer or anti-agitation drugs; |
| ● | strength of sales, marketing, and distribution support; |
| ● | drug pricing in absolute terms and relative to alternative treatments; |
| ● | future changes in health care laws, regulations, and medical policies; and |
| ● | availability of reimbursement codes and coverage in select jurisdictions, and future changes to reimbursement policies of government and third-party payors. |
Significant uncertainty exists as to the coverage and reimbursement status of any drug candidate for which we obtain regulatory approval. In the United States and markets in other countries, sales of any drugs for which we receive regulatory approval for commercial sale will depend in part on the availability of reimbursement from third-party payors. Third-party payors include government health administrative authorities, managed care providers, private health insurers and other organizations.
Healthcare reform measures could hinder or prevent our drug candidates’ commercial success.
The U.S. government and other governments have shown significant interest in pursuing healthcare reform. Any government-adopted reform measures could adversely impact the pricing of healthcare drugs and services in the United States or internationally and the amount of reimbursement available from governmental agencies or other third-party payors. The continuing efforts of the U.S. and foreign governments, insurance companies, managed care organizations and other payors of health care services to contain or reduce health care costs may adversely affect our ability to set prices for our drugs which we believe are fair, and our ability to generate revenues and achieve and maintain profitability.
In the United States, some states have implemented, and other states are considering, pharmaceutical price controls or patient access constraints under their Medicaid program. There have also been recent state legislative efforts that have generally focused on increasing transparency around drug costs or limiting drug prices. In addition, the growth of large managed care organizations and prescription benefit managers, as well as the prevalence of generic substitution, has hindered price increases for prescription drugs. Continued intense public scrutiny of the price of drugs, together with government and payor dynamics, may limit the ability of producers and marketers to set or adjust the price of products based on their value. Outside the United States, numerous major markets, including the EU, Japan and China, have pervasive government involvement in funding healthcare, and, in that regard, fix the pricing and reimbursement of pharmaceutical products. Consequently, our products generating will be subject to increasing government decision-making and budgetary actions. There can be no assurance that new or proposed products will be considered cost-effective or that adequate third-party reimbursement will be available to enable the producer or marketer of such product to maintain price levels sufficient to realize an appropriate return.
85
New laws, regulations and judicial decisions, or new interpretations of existing laws, regulations and decisions, that relate to healthcare availability, methods of delivery or payment for products and services, or sales, marketing or pricing, may limit our potential revenue, and we may need to revise our research and development programs. The pricing and reimbursement environment may change in the future and become more challenging due to several reasons, including policies advanced by the current executive administration in the United States, new healthcare legislation or fiscal challenges faced by government health administration authorities. Specifically, in both the United States and some foreign jurisdictions, there have been a number of legislative and regulatory proposals to change the health care system in ways that could affect our ability to sell our drugs profitably.
For example, the Patient Protection and Affordable Care Act, as amended by the Health Care and Education Reconciliation Act, or the PPACA has substantially changed the way healthcare is financed by both government health plans and private insurers, and significantly impacts the pharmaceutical industry. The PPACA contains a number of provisions that are expected to impact our business and operations in ways that may negatively affect our potential revenues in the future. For example, the PPACA imposes a non-deductible excise tax on pharmaceutical manufacturers or importers that sell branded prescription drugs to government programs which we believe will increase the cost of our drugs. In addition, as part of the PPACA’s provisions closing a funding gap that currently exists in the Medicare Part D prescription drug program, we will be required to provide a discount on branded prescription drugs equal to 50% of the government-negotiated price, for drugs provided to certain beneficiaries who fall within the donut hole. Similarly, PPACA increases the level of Medicaid rebates payable by manufacturers of brand-name drugs from 15.1% to 23.1% and requires collection of rebates for drugs paid by Medicaid managed care organizations. The PPACA also includes significant changes to the 340B drug discount program including expansion of the list of eligible covered entities that may purchase drugs under the program. At the same time, the expansion in eligibility for health insurance benefits created under PPACA is expected to increase the number of patients with insurance coverage who may receive our drugs. While it is too early to predict all the specific effects the PPACA or any future healthcare reform legislation will have on our business, they could have a material adverse effect on our business and financial condition.
Congress periodically adopts legislation like the PPACA and the Medicare Prescription Drug, Improvement and Modernization Act of 2003, that modifies Medicare reimbursement and coverage policies pertaining to prescription drugs. Implementation of these laws is subject to ongoing revision through regulatory and sub regulatory policies. Congress also may consider additional changes to Medicare policies, potentially including Medicare prescription drug policies, as part of ongoing budget negotiations. While the scope of any such legislation is uncertain at this time, there can be no assurances that future legislation or regulations will not decrease the coverage and price that we may receive for our proposed drugs. Other third-party payors are increasingly challenging the prices charged for medical products and services. It will be time consuming and expensive for us to go through the process of seeking coverage and reimbursement from Medicare and private payors. Our proposed drugs may not be considered cost-effective, and coverage and reimbursement may not be available or sufficient to allow us to sell our proposed drugs on a profitable basis. Further federal and state proposals and health care reforms are likely which could limit the prices that can be charged for the drug candidates that we develop and may further limit our commercial opportunities. Our results of operations could be materially adversely affected by proposed healthcare reforms, by the Medicare prescription drug coverage legislation, by the possible effect of such current or future legislation on amounts that private insurers will pay and by other health care reforms that may be enacted or adopted in the future.
In September 2007, the Food and Drug Administration Amendments Act of 2007 was enacted, giving the FDA enhanced post-marketing authority, including the authority to require post-marketing studies and clinical trials, labeling changes based on new safety information, and compliance with risk evaluations and mitigation strategies approved by the FDA. The FDA’s exercise of this authority could result in delays or increased costs during drug development, clinical trials and regulatory review, increased costs to assure compliance with post-approval regulatory requirements, and potential restrictions on the sale and/or distribution of approved drugs.
86
Our relationships with healthcare providers, physicians and third-party payors will be subject to applicable anti-kickback, fraud and abuse, false claims, transparency, health information privacy and security, and other healthcare laws and regulations, which, in the event of a violation, could expose us to criminal sanctions, civil penalties, contractual damages, reputational harm, administrative burdens and diminished profits and future earnings.
Healthcare providers, physicians and third-party payors will play a primary role in the recommendation and prescription of any drug candidates for which we obtain marketing approval. Our future arrangements with healthcare providers, physicians and third-party payors may expose us to broadly applicable fraud and abuse and other healthcare laws and regulations that may constrain the business or financial arrangements and relationships through which we market, sell and distribute any drugs for which we obtain marketing approval. In addition, we may be subject to transparency laws and patient privacy regulation by U.S. federal and state governments and by governments in foreign jurisdictions in which we conduct our business. Restrictions under applicable federal and state healthcare laws and regulations include the following:
| ● | the federal Anti-Kickback Statute prohibits, among other things, persons from knowingly and willfully soliciting, offering, receiving or providing remuneration, directly or indirectly, in cash or in kind, to induce or reward, or in return for, either the referral of an individual for, or the purchase, order or recommendation or arranging of, any good or service, for which payment may be made under a federal healthcare program such as Medicare and Medicaid; |
| ● | the federal False Claims Act imposes criminal and civil penalties, including through civil whistleblower or qui tam actions, against individuals or entities for, among other things, knowingly presenting, or causing to be presented, false or fraudulent claims for payment by a federal healthcare program or making a false statement or record material to payment of a false claim or avoiding, decreasing or concealing an obligation to pay money to the federal government, with potential liability including mandatory treble damages and significant per-claim penalties, currently set at $5,500 to $11,000 per false claim; |
| ● | the federal Health Insurance Portability and Accountability Act of 1996, or HIPAA, imposes criminal and civil liability for executing a scheme to defraud any healthcare benefit program or making false statements relating to healthcare matters; |
| ● | HIPAA, as amended by the Health Information Technology for Economic and Clinical Health Act of 2009, and their respective implementing regulations, also imposes obligations, including mandatory contractual terms, with respect to safeguarding the privacy, security and transmission of individually identifiable health information; |
| ● | the federal Physician Payments Sunshine Act requires applicable manufacturers of covered drugs to report payments and other transfers of value to physicians and teaching hospitals; and |
| ● | analogous state and foreign laws and regulations, such as state anti-kickback and false claims laws and transparency statutes, may apply to sales or marketing arrangements and claims involving healthcare items or services reimbursed by non-governmental third-party payors, including private insurers. |
87
Some state laws require pharmaceutical companies to comply with the pharmaceutical industry’s voluntary compliance guidelines and the relevant compliance guidance promulgated by the federal government and may require drug manufacturers to report information related to payments and other transfers of value to physicians and other healthcare providers or marketing expenditures. Additionally, some state and local laws require the registration of pharmaceutical sales representatives in the jurisdiction. State and foreign laws also govern the privacy and security of health information in some circumstances, many of which differ from each other in significant ways and often are not preempted by HIPAA, thus complicating compliance efforts.
Efforts to ensure that our business arrangements with third parties will comply with applicable healthcare laws and regulations will involve substantial costs. It is possible that governmental authorities will conclude that our business practices may not comply with current or future statutes, regulations or case law involving applicable fraud and abuse or other healthcare laws and regulations. If our operations are found to be in violation of any of these laws or any other governmental regulations that may apply to us, we may be subject to significant civil, criminal and administrative penalties, damages, fines, imprisonment, exclusion of drugs from government funded healthcare programs, such as Medicare and Medicaid, and the curtailment or restructuring of our operations. If any of the physicians or other healthcare providers or entities with whom we expect to do business is found to be not in compliance with applicable laws, they may be subject to criminal, civil or administrative sanctions, including exclusions from participation in government funded healthcare programs.
Recently enacted and future legislation may increase the difficulty and cost for us to obtain marketing approval of and commercialize our drug candidates and affect the prices we may obtain for any drugs that are approved in the United States or foreign jurisdictions.
In the United States and some foreign jurisdictions, there have been a number of legislative and regulatory changes and proposed changes regarding the healthcare system that could prevent or delay marketing approval of our drug candidates, restrict or regulate post-approval activities and affect our ability to profitably sell any drug candidates for which we obtain marketing approval. The pharmaceutical industry has been a particular focus of these efforts and has been significantly affected by legislative initiatives. Current laws, as well as other healthcare reform measures that may be adopted in the future, may result in more rigorous coverage criteria and in additional downward pressure on the price that we receive for any FDA approved drug.
In the United States, the Medicare Prescription Drug, Improvement, and Modernization Act of 2003, or the MMA, changed the way Medicare covers and pays for pharmaceutical products. The legislation expanded Medicare coverage for drug purchases by the elderly and introduced a new reimbursement methodology based on average sales prices for physician-administered drugs. In addition, this legislation provided authority for limiting the number of drugs that will be covered in any therapeutic class. Cost reduction initiatives and other provisions of this legislation could decrease the coverage and price that we receive for any approved drugs. While the MMA applies only to drug benefits for Medicare beneficiaries, private payors often follow Medicare coverage policy and payment limitations in setting their own reimbursement rates. Therefore, any reduction in reimbursement that results from the MMA may result in a similar reduction in payments from private payors.
In March 2010, President Obama signed into law the Patient Protection and Affordable Care Act, as amended by the Health Care and Education Reconciliation Act of 2010, or collectively the ACA. Among the provisions of the ACA of potential importance to our business, including, without limitation, our ability to commercialize and the prices we may obtain for any of our drug candidates that are approved for sale, are the following:
| ● | an annual, non-deductible fee on any entity that manufactures or imports specified branded prescription drugs and biologic agents; |
| ● | an increase in the statutory minimum rebates a manufacturer must pay under the Medicaid Drug Rebate Program; |
| ● | expansion of healthcare fraud and abuse laws, including the civil False Claims Act and the federal Anti-Kickback Statute, new government investigative powers and enhanced penalties for noncompliance; |
88
| ● | a new Medicare Part D coverage gap discount program, in which manufacturers must agree to offer 50% (and 70% starting January 1, 2019) point-of-sale discounts off negotiated prices; |
| ● | extension of manufacturers’ Medicaid rebate liability; |
| ● | expansion of eligibility criteria for Medicaid programs; |
| ● | expansion of the entities eligible for discounts under the Public Health Service pharmaceutical pricing program; |
| ● | new requirements to report certain financial arrangements with physicians and teaching hospitals; |
| ● | a new requirement to annually report drug samples that manufacturers and distributors provide to physicians; and |
| ● | a new Patient-Centered Outcomes Research Institute to oversee, identify priorities in, and conduct comparative clinical effectiveness research, along with funding for such research. |
In addition, other legislative changes have been proposed and adopted since the ACA was enacted. These changes include the Budget Control Act of 2011, which, among other things, led to aggregate reductions to Medicare payments to providers of up to 2% per fiscal year that started in 2013 and, due to subsequent legislative amendments to the statute, will stay in effect through 2027 unless additional congressional action is taken, and the American Taxpayer Relief Act of 2012, which, among other things, reduced Medicare payments to several types of providers and increased the statute of limitations period for the government to recover overpayments to providers from three to five years. These new laws may result in additional reductions in Medicare and other healthcare funding and otherwise affect the prices we may obtain for any of our drug candidates for which we may obtain regulatory approval or the frequency with which any such drug candidate is prescribed or used. Further, there have been several recent U.S. congressional inquiries and proposed state and federal legislation designed to, among other things, bring more transparency to drug pricing, review the relationship between pricing and manufacturer patient programs, reduce the costs of drugs under Medicare and reform government program reimbursement methodologies for drug products.
We expect that these healthcare reforms, as well as other healthcare reform measures that may be adopted in the future, may result in additional reductions in Medicare and other healthcare funding, more rigorous coverage criteria, new payment methodologies and additional downward pressure on the price that we receive for any approved drug and/or the level of reimbursement physicians receive for administering any approved drug we might bring to market. Reductions in reimbursement levels may negatively impact the prices we receive or the frequency with which our drugs are prescribed or administered. Any reduction in reimbursement from Medicare or other government programs may result in a similar reduction in payments from private payors.
89
The costs of prescription pharmaceuticals have also been the subject of considerable discussion in the United States, and members of Congress have stated that they will address such costs through new legislative and administrative measures. To date, there have been several recent U.S. congressional inquiries and proposed and enacted state and federal legislation designed to, among other things, bring more transparency to drug pricing, review the relationship between pricing and manufacturer patient programs, reduce the costs of drugs under Medicare and reform government program reimbursement methodologies for drug products. While any proposed measures will require authorization through additional legislation to become effective, Congress has indicated that it will continue to seek new legislative and/or administrative measures to control drug costs. At the state level, legislatures are increasingly passing legislation and implementing regulations designed to control pharmaceutical and biological product pricing, including price or patient reimbursement constraints, discounts, restrictions on certain product access and marketing cost disclosure and transparency measures, and, in some cases, designed to encourage importation from other countries and bulk purchasing.
Legislative and regulatory proposals have been made to expand post-approval requirements and restrict sales and promotional activities for pharmaceutical products. We cannot be sure whether additional legislative changes will be enacted, or whether FDA regulations, guidance or interpretations will be changed, or what the impact of such changes on the marketing approvals of our drug candidates, if any, may be. Increased scrutiny by the U.S. Congress of the FDA’s approval process may significantly delay or prevent marketing approval, as well as subject us to more stringent product labeling and post-marketing testing and other requirements.
Governments outside of the United States tend to impose strict price controls, which may adversely affect our revenues, if any.
In some countries, particularly the countries of the European Union and Canada, the pricing of prescription pharmaceuticals is subject to governmental control. In these countries, pricing negotiations with governmental authorities can take considerable time after the receipt of marketing approval for a drug. To obtain reimbursement or pricing approval in some countries, we may be required to conduct a clinical trial that compares the cost-effectiveness of our drug candidate to other available therapies. In the European Union, a member state may approve a specific price for the medicinal product or it may instead adopt a system of direct or indirect controls on the profitability of the company placing the medicinal product on the market. If reimbursement of our drugs is unavailable or limited in scope or amount, or if pricing is set at unsatisfactory levels, our business could be harmed, possibly materially. Historically, products launched in the European Union do not follow price structures of the United States and generally prices tend to be significantly lower.
90
If we or any third-party manufacturers or contractors we engage now or in the future fail to comply with environmental, health and safety laws and regulations, we could become subject to fines or penalties or incur costs or liabilities that could harm our business.
We and third-party manufacturers we engage now are, and any third-party manufacturers we may engage in the future will be, subject to numerous environmental, health and safety laws and regulations, including those governing laboratory procedures and the handling, use, storage, treatment and disposal of hazardous materials and wastes. Our operations, including work conducted through third-party manufacturers or contractors, involve the use of hazardous and flammable materials, including chemicals and biological materials. Our operations also produce hazardous waste products. We generally contract with third parties for the disposal of these materials and wastes. We cannot eliminate the risk of contamination or injury from these materials. In the event of contamination or injury resulting from our use of hazardous materials, we could be held liable for any resulting damages, and any liability could exceed our resources. Liability under certain environmental laws governing the release and cleanup of hazardous materials is joint and several and could be imposed without regard to fault. We also could incur significant costs associated with civil or criminal fines and penalties or become subject to injunctions limiting or prohibiting our activities for failure to comply with such laws and regulations.
Although we maintain general liability insurance as well as workers’ compensation insurance to cover us for costs and expenses we may incur due to injuries to our employees resulting from the use of hazardous materials, this insurance may not provide adequate coverage against potential liabilities. We do not maintain insurance for environmental liability or toxic tort claims that may be asserted against us in connection with our, or our contractors, storage or disposal of biological, hazardous or radioactive materials.
In addition, we may incur substantial costs in order to comply with current or future environmental, health and safety laws and regulations. These current or future laws and regulations may impair our research, development or production efforts. Our failure to comply with these laws and regulations also may result in substantial fines, penalties or other sanctions.
Further, with respect to the operations of our current and any future third-party contract manufacturers or other contractors, it is possible that if they fail to operate in compliance with applicable environmental, health and safety laws and regulations or properly dispose of wastes associated with our drugs, we could be held liable for any resulting damages, suffer reputational harm or experience a disruption in the manufacture and supply of our drug candidates or drugs. In addition, our supply chain may be adversely impacted if any of our third-party contract manufacturers become subject to injunctions or other sanctions as a result of their non-compliance with environmental, health and safety laws and regulations.
We may experience challenges with the acquisition, development, enhancement or deployment of technology necessary for our RADR® platform.
We operate in businesses that require sophisticated computer systems and software for data collection, data processing, cloud-based platforms, analytics, statistical projections and forecasting, mobile computing, social media analytics and other applications and technologies. We seek, in part, to address our technology risks by increasing our reliance on the use of innovations by cross-industry technology leaders and adapting these for our applicable needs and applications. Some of the technologies supporting our industry are changing rapidly and we must continue to adapt to these changes in a timely and effective manner at an acceptable cost. We also must continue to obtain and utilize data to in forms that are easy to use while simultaneously providing clear answers to complex questions. There can be no guarantee that we will be able to develop, acquire or integrate new technologies, that these new technologies will meet our needs or achieve our expected goals, or that we will be able to do so as quickly or cost-effectively as our competitors. Significant technological change could render our RADR® platform obsolete. Our continued success will depend on our ability to adapt to changing technologies, manage and process ever-increasing amounts of data and information and improve the performance, features and reliability of our platform and capabilities in response to changing internal and industry demands. We may experience difficulties that could delay or prevent the successful design, development, testing, and introduction of advanced versions of our RADR®platform, limiting our ability to identify new drug candidates. New services, or enhancements to existing services using our RADR® platform, may not adequately meet our requirements. Any of these failures could have a material adverse effect on our operating results and financial condition.
91
Risks Related to Our Reliance on Third Parties
We rely on third parties to conduct our preclinical studies and clinical trials. If these third parties do not successfully perform their contractual legal and regulatory duties or meet expected deadlines, we may not be able to obtain regulatory approval for or commercialize our drug candidates and our business could be substantially harmed.
We have relied upon and plan to continue to rely upon third-party medical institutions, clinical investigators, contract laboratories and other third party CROs to monitor and manage data for our ongoing preclinical and clinical programs. We also rely on these parties for execution of our preclinical studies and clinical trials, and control only certain aspects of their activities. Nevertheless, we are responsible for ensuring that each of our studies is conducted in accordance with the applicable protocol, legal, regulatory and scientific standards, and our reliance on the CROs does not relieve us of our regulatory responsibilities. We and our CROs are required to comply with cGCPs, which are regulations and guidelines enforced by the FDA, the Competent Authorities of the Member States of the European Economic Area, or EEA, and comparable foreign regulatory authorities for all of our drugs in clinical development.
Regulatory authorities enforce these cGCPs through periodic inspections of trial sponsors, principal investigators and trial sites. If we or any of our CROs fail to comply with applicable cGCPs, the clinical data generated in our clinical trials may be deemed unreliable and the FDA, the EMA or comparable foreign regulatory authorities may require us to perform additional clinical trials before approving our marketing applications. We cannot assure you that upon inspection by a given regulatory authority, such regulatory authority will determine that any of our clinical trials comply with cGCP regulations. In addition, our clinical trials must be conducted with product produced under current good manufacturing practices, or cGMP, regulations. Our failure to comply with these regulations may require us to repeat clinical trials, which would delay the regulatory approval process.
If any of our relationships with these third-party CROs terminate, we may not be able to enter into arrangements with alternative CROs or to do so on commercially reasonable terms. In addition, our CROs are not our employees, and except for remedies available to us under our agreements with such CROs, we cannot control whether or not they devote sufficient time and resources to our on-going clinical, nonclinical and preclinical programs. If CROs do not successfully carry out their contractual duties or obligations or meet expected deadlines, if they need to be replaced or if the quality or accuracy of the clinical data they obtain is compromised due to the failure to adhere to our clinical protocols, regulatory requirements or for other reasons, our clinical trials may be extended, delayed or terminated and we may not be able to obtain regulatory approval for or successfully commercialize our drug candidates. As a result, our results of operations and the commercial prospects for our drug candidates would be harmed, our costs could increase and our ability to generate revenues could be delayed.
Many of the third parties with whom we contract may also have relationships with other commercial entities, including our competitors, for whom they may also be conducting clinical trials or other drug development activities that could harm our competitive position. If the third parties conducting our GLP preclinical studies or our clinical trials do not perform their contractual duties or obligations, experience work stoppages, do not meet expected deadlines, terminate their agreements with us or need to be replaced, or if the quality or accuracy of the clinical data they obtain is compromised due to their failure to adhere to our clinical trial protocols or to GCPs, or for any other reason, we may need to enter into new arrangements with alternative third parties. Switching or adding additional CROs involves additional cost and requires management time and focus. In addition, there is a natural transition period when a new CRO commences work. As a result, delays occur, which can materially impact our ability to meet our desired clinical development timelines. Though we carefully manage our relationships with our CROs, there can be no assurance that we will not encounter similar challenges or delays in the future or that these delays or challenges will not have a material adverse impact on our business, financial condition and prospects.
92
We are substantially dependent on third parties for the manufacture of our clinical supplies of our drug candidates, and we intend to rely on third parties to produce commercial supplies of any approved drug candidate. Therefore, our development of our drugs could be stopped or delayed, and our commercialization of any future drug could be stopped or delayed or made less profitable if third party manufacturers fail to obtain approval of the FDA or comparable regulatory authorities or fail to provide us with drug products in sufficient quantities or at acceptable prices.
The manufacture of pharmaceutical products is complex and requires significant expertise, capital investment, process controls and know-how. Common difficulties in pharmaceutical manufacturing may include: sourcing and producing raw materials, transferring technology from chemistry and development activities to production activities, validating initial production designs, scaling manufacturing techniques, improving costs and yields, establishing and maintaining quality controls and stability requirements, eliminating contaminations and operator errors, and maintaining compliance with regulatory requirements. We do not currently have nor do we plan to acquire the infrastructure or capability internally in accordance with cGMP prescribed by the FDA or to produce an adequate supply of compounds to meet future requirements for clinical trials and commercialization of our drugs. Drug manufacturing facilities are subject to inspection before the FDA will issue an approval to market a new drug product, and all of the manufacturers that we intend to use must adhere to the cGMP regulations prescribed by the FDA.
We expect therefore to rely on third-party manufacturers for clinical supplies of our drug candidates that we may develop. These third-party manufacturers will be required to comply with current good manufacturing practices, or GMPs, and other applicable laws and regulations. We will have no control over the ability of these third parties to comply with these requirements, or to maintain adequate quality control, quality assurance and qualified personnel. If the FDA or any other applicable regulatory authorities do not approve the facilities of these third parties for the manufacture of our other drug candidates or any drugs that we may successfully develop, or if it withdraws any such approval, or if our suppliers or contract manufacturers decide they no longer want to supply or manufacture for us, we may need to find alternative manufacturing facilities, in which case we might not be able to identify manufacturers for clinical or commercial supply on acceptable terms, or at all. Any of these factors would significantly impact our ability to develop, obtain regulatory approval for or market our drug candidates and adversely affect our business.
We and/or our third-party manufacturers may be adversely affected by developments outside of our control, and these developments may delay or prevent further manufacturing of our drugs. Adverse developments may include labor disputes, resource constraints, shipment delays, inventory shortages, lot failures, unexpected sources of contamination, lawsuits related to our manufacturing techniques, equipment used during manufacturing, or composition of matter, unstable political environments, acts of terrorism, war, natural disasters, and other natural and man-made disasters. If we or our third-party manufacturers were to encounter any of the above difficulties, or otherwise fail to comply with contractual obligations, our ability to provide any drug for clinical trial or commercial purposes would be jeopardized. This may increase the costs associated with completing our clinical trials and commercial production. Further, production disruptions may cause us to terminate ongoing clinical trials and/or commence new clinical trials at additional expense. We may also have to take inventory write-offs and incur other charges and expenses for drugs that fail to meet specifications or pass safety inspections. If production difficulties cannot be solved with acceptable costs, expenses, and timeframes, we may be forced to abandon our clinical development and commercialization plans, which could have a material adverse effect on our business, prospects, financial condition, and the value of our securities.
We, or third-party manufacturers on whom we rely, may be unable to successfully scale-up manufacturing of our drug candidates in sufficient quality and quantity, which would delay or prevent us from developing our drug candidates and commercializing approved drugs, if any.
In order to conduct clinical trials of our drug candidates and commercialize any approved drug candidates, we, or our manufacturers, will need to manufacture them in large quantities. We, or our manufacturers, may be unable to successfully increase the manufacturing capacity for any of our drug candidates in a timely or cost-effective manner, or at all. In addition, quality issues may arise during scale-up activities. If we, or any of our manufacturers, are unable to successfully scale up the manufacture of our drug candidates in sufficient quality and quantity, the development, testing, and clinical trials of that drug candidate may be delayed or infeasible, and regulatory approval or commercial launch of any resulting drug may be delayed or not obtained, which could significantly harm our business. If we are unable to obtain or maintain third-party manufacturing for commercial supply of our drug candidates, or to do so on commercially reasonable terms, we may not be able to develop and commercialize our drug candidates successfully.
93
Our failure to find third party collaborators to assist or share in the costs of drug development could materially harm our business, financial condition and results of operations.
Our strategy for the development and commercialization of our proprietary drug candidates may include the formation of collaborative arrangements with third parties. Existing and future collaborators have significant discretion in determining the efforts and resources they apply and may not perform their obligations as expected. Potential third-party collaborators include biopharmaceutical, pharmaceutical and biotechnology companies, academic institutions and other entities. Third-party collaborators may assist us in:
| ● | funding research, preclinical development, clinical trials and manufacturing; |
| ● | seeking and obtaining regulatory approvals; and |
| ● | successfully commercializing any future drug candidates. |
If we are not able to establish further collaboration agreements, we may be required to undertake drug development and commercialization at our own expense. Such an undertaking may limit the number of drug candidates that we will be able to develop, significantly increase our capital requirements and place additional strain on our internal resources. Our failure to enter into additional collaborations could materially harm our business, financial condition and results of operations.
In addition, our dependence on licensing, collaboration and other agreements with third parties may subject us to a number of risks. These agreements may not be on terms that prove favorable to us and may require us to relinquish certain rights in our drug candidates. To the extent we agree to work exclusively with one collaborator in a given area, our opportunities to collaborate with other entities could be curtailed. Lengthy negotiations with potential new collaborators may lead to delays in the research, development or commercialization of drug candidates. The decision by our collaborators to pursue alternative technologies or the failure of our collaborators to develop or commercialize successfully any drug candidate to which they have obtained rights from us could materially harm our business, financial condition and results of operations.
Risks Related to Our Business and Industry
We may face future business disruption and related risks resulting from the outbreak of the novel coronavirus 2019 (COVID-19) or from another pandemic, epidemic or outbreak of an infectious disease, any of which could have a material adverse effect on our business.
The development of our drug candidates could be disrupted and materially adversely affected in the future by a pandemic, epidemic or outbreak of an infectious disease like the outbreak of COVID-19. The spread of COVID-19 from China to other countries has resulted in the Director General of the World Health Organization declaring the outbreak of COVID-19 as a global pandemic. In response, national, state and local governments around the world, including in the U.S., Canada and Europe, have implemented measures to reduce the spread of COVID-19, including international travel restrictions. Additionally, numerous national, state and local jurisdictions have imposed, and in the future may impose, shelter-in-place orders, quarantines, shut-downs of non-essential businesses, and similar government orders and restrictions on their residents all of varying durations to control the spread of COVID-19.
Measures adopted to slow the spread of COVID-19 have adversely affected workforces, customers, supply chains, consumer sentiment, economies, and financial markets, and, along with decreased consumer spending, have led to an economic downturn across many global economies. In particular, the measures may result in the inability of our suppliers to deliver components or raw materials on a timely basis or materially and adversely affect our collaborators and out-license partners’ ability to perform and advance preclinical studies and clinical trials. For example, Allarity Therapeutics has informed us that continuing enrollment for the Phase II clinical trial for LP-100 (Irofulven) has slowed during the pandemic. The timing of non-clinical research studies for our drug candidates by collaborators and service providers also slowed during 2020 in connection with the pandemic. In addition, hospitals may reduce staffing and reduce or postpone certain treatments in response to the spread of an infectious disease. Such events may result in a period of business and manufacturing disruption, and in reduced operations, any of which could materially affect our business, financial condition and results of operations. The extent to which COVID-19 impacts our business will depend on future developments, which are highly uncertain and cannot be predicted, including new information which may emerge concerning the severity of the coronavirus and the actions to contain the coronavirus or treat its impact, among others. While some of the measures were allowed to lapse in many parts of the world with the fall in cases during the summer season in the Northern Hemisphere, the return of colder weather in the Northern Hemisphere has resulted in an increase in cases in that region, which has increased forecasts of a “second wave” of infections that could result in the reimposition of many governmental measures to stem the spread of COVID-19.
94
International stock markets continue to reflect the uncertainty associated with the slow-down in the worldwide economy and the reduced levels of international travel which has resulted. Domestic and international stock indices initially suffered large declines in the Spring of 2020. While stock indexes have since recovered, the return of additional waves and infections and new virus variants could result in further disruption in domestic and international capital markets. Disruption in the capital markets could adversely impact our ability to raise the capital we need to further our business on favorable terms.
We are still assessing our business plans and the impact COVID-19 may have on our ability to advance the development of our drug candidates or to raise financing to support the development of our drug candidates, but no assurances can be given that this analysis will enable us to avoid part or all of any impact from the spread of COVID-19 or its consequences, including downturns in business sentiment generally or in our sector in particular.
We will need to increase the size of our organization and the scope of our outside vendor relationships, and we may experience difficulties in managing growth.
As of the date of this report, we employed a total of 11 full-time and four part-time employees. Our current internal departments include research and development, finance and administration. We intend to expand our management team to include an operation ramp up of additional scientific development and technical staff required to achieve our business objectives. We will need to expand our managerial, operational, technical and scientific, financial and other resources in order to manage our operations and clinical trials, establish independent manufacturing, continue our research and development activities, and commercialize our drug candidate. Our management and scientific personnel, systems and facilities currently in place may not be adequate to support our future growth.
Our need to effectively manage our operations, growth and various projects requires that we:
| ● | manage our clinical trials effectively, including our planned clinical trials of LP-184 and LP-300 and our other drug candidates; |
| ● | manage our internal development efforts effectively while carrying out our contractual obligations to licensors, contractors and other third parties; |
| ● | continue to improve our operational, financial and management controls and reporting systems and procedures; and |
| ● | attract and retain sufficient numbers of talented employees. |
We may utilize the services of vendors and research partners or collaborators to perform tasks including preclinical studies and clinical trial management, statistics and analysis, regulatory affairs, medical advisory, market research, formulation development, chemistry, manufacturing and control activities, other drug development functions, legal, auditing, financial advisory, and investor relations. Our growth strategy may also entail expanding our group of contractors or consultants to implement these and other tasks going forward. Because we rely on numerous consultants to outsource many key functions of our business, we will need to be able to effectively manage these consultants to ensure that they successfully carry out their contractual obligations and meet expected deadlines. However, if we are unable to effectively manage our outsourced activities or if the quality or accuracy of the services provided by consultants is compromised for any reason, our clinical trials may be extended, delayed or terminated, and we may not be able to obtain regulatory approval for our drug candidate or otherwise advance our business. There can be no assurance that we will be able to manage our existing consultants or find other competent outside contractors and consultants on economically reasonable terms, or at all. If we are not able to effectively expand our organization by hiring new employees and expanding our groups of consultants and contractors, we may be unable to successfully implement the tasks necessary to further develop and commercialize our drug candidates and, accordingly, may not achieve our research, development and commercialization goals.
95
We depend on our senior management team, and the loss of one or more of our executive officers or key employees or an inability to attract and retain highly skilled employees could adversely affect our business.
Our success depends largely upon the continued services of Panna Sharma, our Chief Executive Officer, President and Director. We do not maintain “key person” insurance for Mr. Sharma or any of our other key employees. We also rely on employees in the areas of research and development, artificial intelligence and machine learning services and general and administrative functions, some of which are in the US on H-1B work visas. From time to time, there may be changes in our executive management and employees resulting from the hiring or departure of executives or other key employees or the expiration or termination of H-1B work visas, which could disrupt our business. The replacement of one or more of our executive officers or other key employees would likely involve significant time and costs and may significantly delay or prevent the achievement of our business objectives.
To continue to execute our growth strategy, we also must attract and retain highly skilled personnel. We might not be successful in maintaining our unique culture and continuing to attract and retain qualified personnel. We have from time to time in the past experienced, and we expect to continue to experience in the future, difficulty in hiring and retaining highly skilled personnel with appropriate qualifications. The pool of qualified personnel with experience in artificial intelligence, machine learning, and genomics, or experience working with the pharma market is limited overall. In addition, many of the companies with which we compete for experienced personnel have greater resources than we have.
In addition, in making employment decisions, particularly in the biotechnology and pharmaceutical industries, job candidates often consider the value of the stock options or other equity instruments they are to receive in connection with their employment. Volatility in the price of our stock might, therefore, adversely affect our ability to attract or retain highly skilled personnel. Furthermore, the requirement to expense stock options and other equity instruments might discourage us from granting the size or type of stock option or equity awards that job candidates require to join our company. If we fail to attract new personnel or fail to retain and motivate our current personnel, our business and future growth prospects could be severely harmed.
Our employees may engage in misconduct or other improper activities, including noncompliance with regulatory standards and requirements and insider trading.
We are exposed to the risk of employee fraud or other misconduct. Misconduct by employees could include intentional failures to comply with any regulations applicable to us, to provide accurate information to regulatory authorities, to comply with manufacturing standards we have established, to comply with federal and state healthcare fraud and abuse laws and regulations, or to report financial information or data accurately or disclose unauthorized activities to us. In particular, sales, marketing and business arrangements in the healthcare industry are subject to extensive laws and regulations intended to prevent fraud, misconduct, kickbacks, self-dealing and other abusive practices. These laws and regulations may restrict or prohibit a wide range of pricing, discounting, marketing and promotion, sales commission, customer incentive programs and other business arrangements. Employee misconduct could also involve the improper use of information obtained in the course of clinical trials, which could result in regulatory sanctions and serious harm to our reputation. We have adopted a Code of Business Conduct, but it is not always possible to identify and deter employee misconduct, and the precautions we take to detect and prevent this activity may not be effective in controlling unknown or unmanaged risk. If our employees engage in any such misconduct, we could face criminal penalties, fines, revocation of regulatory approvals and harm to our reputation, any of which could form a material adverse effect on our business.
96
Business interruptions could adversely affect future operations, revenues, and financial conditions, and may increase our costs and expenses.
Our operations, and those of our directors, advisors, contractors, consultants, CROs, and collaborators, could be adversely affected by earthquakes, floods, hurricanes, typhoons, extreme weather conditions, fires, water shortages, power failures, business systems failures, medical epidemics and other natural and man-made disaster or business interruptions. Our phones, electronic devices and computer systems and those of our directors, advisors, contractors, consultants, CROs, and collaborators are vulnerable to damages, theft and accidental loss, negligence, unauthorized access, terrorism, war, electronic and telecommunications failures, and other natural and man-made disasters. Operating as a virtual company, our employees conduct business outside of our headquarters and leased or owned facilities. These locations may be subject to additional security and other risk factors due to the limited control of our employees. If such an event as described above were to occur in the future, it may cause interruptions in our operations, delay research and development programs, clinical trials, regulatory activities, manufacturing and quality assurance activities, sales and marketing activities, hiring, training of employees and persons within associated third parties, and other business activities. For example, the loss of clinical trial data from completed or future clinical trials could result in delays in our regulatory approval efforts and significantly increase our costs to recover or reproduce the data.
Likewise, we will rely on third parties to manufacture LP-100, LP-184 and LP-300 and conduct clinical trials, and similar events as those described in the prior paragraph relating to their business systems, equipment and facilities could also have a material adverse effect on our business. To the extent that any disruption or security breach were to result in a loss of, or damage to, our data or applications, or inappropriate disclosure of confidential or proprietary information, we could incur liability and the further development and commercialization of our drug candidates could be delayed or altogether terminated.
Disruptions to our information technology systems, including future cyber-attacks and security breaches, and the costs of maintaining secure and effective information technology systems could negatively affect our business and results of operations.
The efficient operation of our businesses is highly dependent on computer hardware and software systems, including our customized information technology systems that form our RADR® platform. Information systems are vulnerable to security breaches by computer hackers and cyber terrorists. We rely on industry accepted security measures and technology to securely maintain confidential and proprietary information maintained on our information systems, and continue to invest in maintaining and upgrading these systems and applications to ensure risk is controlled. Regardless of our efforts to maintain and upgrade our cyber security systems, there can be no assurance that we will not suffer an intrusion, that unauthorized parties will not gain access to confidential or personal information, or that any such incident will be discovered promptly. The techniques used by criminals to obtain unauthorized access to sensitive data change frequently and often are not recognized until launched against a target, and we may be unable to anticipate these techniques or implement adequate preventative measures. The failure to promptly detect, determine the extent of and appropriately respond to a significant data security breach could have a material adverse impact on our business, financial condition and results of operations. In addition, the unavailability of the information systems or failure of these systems to perform as anticipated for any reason, including a major disaster or business interruption resulting in an inability to access data stored in these systems or sustain the data center systems necessary to support functions to meet our needs, and any inability to respond to, or recover from, such an event, could disrupt our business and could result in decreased performance and increased overhead costs, causing our business and results of operations to suffer.
Additionally, our operations involve the receipt and storage of sensitive data, including personal information about our employees and proprietary business information of ours and our vendors. We may also share information with vendors that assist us in conducting our business, as required by law, with the permission of the individual or as permitted under applicable privacy policies.
Despite the utilization of information security measures, we cannot be certain that all of our IT systems or the IT systems of our vendors are or will be able to prevent, contain or detect any future cyber-attacks or security breaches from known malware, malware that may be developed in the future or otherwise. Cyber-attacks are rapidly evolving and becoming increasingly sophisticated and difficult to detect, and therefore, we may be unable to anticipate these attacks or implement adequate preventive measures. Additionally, unauthorized parties may attempt to gain access to our or a vendor’s systems or facilities through fraud, trickery or other forms of deception involving our employees or vendors. To the extent that any attack or breach results in the loss, damage or misappropriation of information, we may be adversely affected by claims from persons participating in our clinical trials, stockholders and others and by costly inquiries or enforcement actions on the part of regulatory authorities. Our operations could also be significantly disrupted by these claims, as well as by the need to spend significant time and expense to upgrade, fix or replace our systems. We could also lose credibility with persons participating in our clinical trials and suffer damage to our reputation and future sales, if any. In addition, the cost of complying with stricter privacy and information security laws and standards and developing, maintaining and upgrading technology systems to address future advances in technology, could be significant and we could experience problems and interruptions associated with the implementation of new or upgraded systems and technology or with maintenance or adequate support of existing systems.
97
Our failure to successfully acquire, develop and market additional drug candidates could impair our ability to grow.
As part of our growth strategy, we may evaluate, acquire, license, develop and/or market additional drug candidates and technologies. Our internal research capabilities are limited and we may be dependent upon pharmaceutical and biopharmaceutical companies, academic scientists and other researchers to sell or license drug candidates or technologies to us. The success of this strategy depends partly upon our ability to identify, select and acquire promising pharmaceutical drug candidates and technologies. The process of proposing, negotiating and implementing a license or acquisition of a drug candidate is lengthy and complex. Other companies, including some with substantially greater financial, marketing and sales resources, may compete with us for the license or acquisition of drug candidates and technologies. We have limited resources to identify and execute the acquisition or in-licensing of potential drug candidates and technologies and to integrate them into our current infrastructure. Moreover, we may devote resources to potential acquisitions or in-licensing opportunities that are never completed, or we may fail to realize the anticipated benefits of such efforts. Furthermore, we may not be able to acquire the rights to additional drug candidates on terms that we find acceptable, or at all.
In addition, future acquisitions of intellectual property rights may entail numerous operational and financial risks, including:
| ● | exposure to unknown liabilities; |
| ● | disruption of our business and diversion of our management’s and technical personnel’s time and attention to develop acquired drug candidates or technologies; |
| ● | incurrence of substantial debt or dilutive issuances of securities to pay for acquisition costs; |
| ● | higher than expected acquisition costs; and |
| ● | increased amortization expenses. |
Any drug candidate that we acquire may require additional development efforts prior to commercial sale or out-licensing, including extensive clinical testing and approval by the FDA and applicable foreign regulatory authorities. All drug candidates are prone to risks of failure typical of pharmaceutical drug development, including the possibility that a drug candidate will not be shown to be sufficiently safe and effective for approval by regulatory authorities. In addition, we cannot provide assurance that any drugs that we may develop or approved drugs that we may acquire will be manufactured profitably or achieve market acceptance.
We have obtained statistical data, market data and other industry data and forecasts used throughout this report from market research, publicly available information and industry publications which we believe are reliable but have not been verified by any third party.
This report contains estimates, projections and other information concerning our industry, our business and the markets for our drug candidates, including data regarding the estimated size of such markets and the incidence of certain medical conditions. We obtained the industry, market and similar data set forth in this report from our internal estimates and research and from academic and industry research, publications, surveys and studies conducted by third parties, including governmental agencies. In some cases, we do not expressly refer to the sources from which this data is derived. Information that is based on estimates, forecasts, projections, market research or similar methodologies is inherently subject to uncertainties and actual events or circumstances may differ materially from events and circumstances that are assumed in this information. While we believe our internal research is reliable, such research has not been verified by any third party.
98
Risks Related to Our Intellectual Property
If we do not obtain patent term extension for any drug candidates we may develop, our business may be materially harmed.
In the United States, depending upon the timing, duration, and specifics of any FDA marketing approval of a drug candidate, the patent term of a patent that covers an FDA-approved drug may be eligible for limited patent term extension, which permits patent term restoration as compensation for the patent term lost during the FDA regulatory review process. The Drug Price Competition and Patent Term Restoration Act of 1984, also known as the Hatch-Waxman Act, permits a patent term extension of up to five years beyond the expiration of the patent. The length of the patent term extension is related to the length of time the drug is under regulatory review. Patent term extension cannot extend the remaining term of a patent beyond a total of 14 years from the date of drug approval, and only one patent applicable to an approved drug may be extended and only those claims covering the approved drug, a method for using it, or a method for manufacturing it may be extended. Similar provisions are available in Europe and other non-United States jurisdictions to extend the term of a patent that covers an approved drug. While, in the future, if and when our drug candidates receive FDA approval, we expect to apply for patent term extensions on patents directed to those drug candidates, there is no guarantee that the applicable authorities will agree with our assessment of whether such extensions should be granted, and even if granted, the length of such extensions. We may not be granted an extension because of, for example, failing to exercise due diligence during the testing phase or regulatory review process, failing to apply within applicable deadlines, failing to apply prior to expiration of the relevant patents, or otherwise failing to satisfy applicable requirements. If we are unable to obtain any patent term extension or the term of any such extension is less than we request, our competitors may obtain approval of competing drugs following the expiration of our patent rights, and our business, financial condition, results of operations, and prospects could be materially harmed.
Changes to patent laws in the United States and other jurisdictions could diminish the value of patents in general, thereby impairing our ability to protect our drugs.
Changes in either the patent laws or interpretation of patent laws in the United States, including patent reform legislation such as the Leahy-Smith America Invents Act, or the Leahy-Smith Act, could increase the uncertainties and costs surrounding the prosecution of our owned and in-licensed patent applications and the maintenance, enforcement or defense of our owned and in-licensed issued patents. The Leahy-Smith Act includes a number of significant changes to United States patent law. These changes include provisions that affect the way patent applications are prosecuted, redefine prior art, provide more efficient and cost-effective avenues for competitors to challenge the validity of patents, and enable third-party submission of prior art to the USPTO during patent prosecution and additional procedures to attack the validity of a patent at USPTO-administered post-grant proceedings, including post-grant review, inter parties review, and derivation proceedings. Assuming that other requirements for patentability are met, prior to March 2013, in the United States, the first to invent the claimed invention was entitled to the patent, while outside the United States, the first to file a patent application was entitled to the patent.
After March 2013, under the Leahy-Smith Act, the United States transitioned to a first-to-file system in which, assuming that the other statutory requirements for patentability are met, the first inventor to file a patent application will be entitled to the patent on an invention regardless of whether a third party was the first to invent the claimed invention. As such, the Leahy-Smith Act and its implementation could increase the uncertainties and costs surrounding the prosecution of our patent applications and the enforcement or defense of our issued patents, all of which could have a material adverse effect on our business, financial condition, results of operations, and prospects.
In addition, the patent positions of companies in the development and commercialization of biologics and pharmaceuticals are particularly uncertain. Recent U.S. Supreme Court rulings have narrowed the scope of patent protection available in certain circumstances and weakened the rights of patent owners in certain situations. This combination of events has created uncertainty with respect to the validity and enforceability of patents once obtained. Depending on future actions by the U.S. Congress, the federal courts, and the USPTO, the laws and regulations governing patents could change in unpredictable ways that could have a material adverse effect on our patent rights and our ability to protect, defend and enforce our patent rights in the future.
99
We or our licensors may become involved in lawsuits to protect or enforce our patent or other intellectual property rights, which could be expensive, time-consuming and unsuccessful.
Competitors and other third parties may infringe, misappropriate or otherwise violate our or our licensor’s issued patents or other intellectual property. As a result, we or our licensors may need to file infringement, misappropriation or other intellectual property related claims, which can be expensive and time-consuming. Any claims we assert against perceived infringers could provoke such parties to assert counterclaims against us alleging that we infringe, misappropriate or otherwise violate their intellectual property. In addition, in a patent infringement proceeding, such parties could counterclaim that the patents we or our licensors have asserted are invalid or unenforceable. In patent litigation in the United States, defendant counterclaims alleging invalidity or unenforceability are commonplace. Grounds for a validity challenge could be an alleged failure to meet any of several statutory requirements, including lack of novelty, obviousness, or non-enablement. Grounds for an unenforceability assertion could be an allegation that someone connected with prosecution of the patent withheld relevant information from the USPTO, or made a misleading statement, during prosecution. Third parties may institute such claims before administrative bodies in the United States or abroad, even outside the context of litigation. Such mechanisms include re-examination, post-grant review, inter parties review, interference proceedings, derivation proceedings, and equivalent proceedings in foreign jurisdictions (e.g., opposition proceedings).
An adverse result in any such proceeding could put one or more of our owned or in-licensed patents at risk of being invalidated or interpreted narrowly, and could put any of our owned or in-licensed patent applications at risk of not yielding an issued patent. A court may also refuse to stop the third party from using the technology at issue in a proceeding on the grounds that our owned or in-licensed patents do not cover such technology. Furthermore, because of the substantial amount of discovery required in connection with intellectual property litigation, there is a risk that some of our confidential information or trade secrets could be compromised by disclosure during this type of litigation. Any of the foregoing could allow such third parties to develop and commercialize competing technologies and products and have a material adverse impact on our business, financial condition, results of operations, and prospects.
Third parties may initiate legal proceedings alleging that we are infringing, misappropriating or otherwise violating their intellectual property rights, the outcome of which would be uncertain and could have a material adverse effect on the success of our business.
Our commercial success depends upon our ability, and the ability of our collaborators, to develop, manufacture, market and sell our drug candidates and use our proprietary technologies without infringing, misappropriating or otherwise violating the intellectual property and proprietary rights of third parties. There is considerable patent and other intellectual property litigation in the pharmaceutical and biotechnology industries. We may become party to, or threatened with, adversarial proceedings or litigation regarding intellectual property rights with respect to our technology and drug candidates, including interference proceedings, post grant review, inter parties review, and derivation proceedings before the USPTO and similar proceedings in foreign jurisdictions such as oppositions before the European Patent Office.
The legal threshold for initiating litigation or contested proceedings is low, so that even lawsuits or proceedings with a low probability of success might be initiated and require significant resources to defend. Litigation and contested proceedings can also be expensive and time-consuming, and our adversaries in these proceedings may have the ability to dedicate substantially greater resources to prosecuting these legal actions than we can. The risks of being involved in such litigation and proceedings may increase if and as our drug candidates near commercialization and as we gain the greater visibility associated with being a public company. Third parties may assert infringement claims against us based on existing patents or patents that may be granted in the future, regardless of merit. We may not be aware of all such intellectual property rights potentially relating to our technology and drug candidates and their uses. Thus, we do not know with certainty that our technology and drug candidates, or our development and commercialization thereof, do not and will not infringe, misappropriate or otherwise violate any third party’s intellectual property.
Even if we believe that third party intellectual property claims are without merit, there is no assurance that a court would find in our favor on questions of misappropriation, infringement, validity, enforceability, or priority. A court of competent jurisdiction could hold these third-party patents are valid, enforceable, and infringed, which could materially and adversely affect our ability to commercialize any technology or drug candidate covered by the asserted third-party patents. In order to successfully challenge the validity of any such U.S. patent in federal court, we would need to overcome a presumption of validity. As this burden is a high one requiring us to present clear and convincing evidence as to the invalidity of any such U.S. patent claim, there is no assurance that a court of competent jurisdiction would invalidate the claims of any such U.S. patent.
100
If we are found to infringe, misappropriate or otherwise violate a third party’s intellectual property rights, we could be required to obtain a license from such third party to continue developing, manufacturing and marketing our technology and drug candidates. However, we may not be able to obtain any required license on commercially reasonable terms or at all. Even if we were able to obtain a license, it could be non-exclusive; thereby giving our competitors and other third parties access to the same technologies licensed to us and could require us to make substantial licensing and royalty payments. We could be forced, including by court order, to cease developing, manufacturing and commercializing the infringing technology or drug. In addition, we could be found liable for significant monetary damages, including treble damages and attorneys’ fees, if we are found to have willfully infringed a patent or other intellectual property right and could be forced to indemnify our collaborators or others. A finding of infringement could prevent us from commercializing our drug candidates or force us to cease some of our business operations, which could materially harm our business. In addition, we may be forced to redesign our drug candidates, seek new regulatory approvals and indemnify third parties pursuant to contractual agreements. Claims that we have misappropriated the confidential information or trade secrets of third parties could have a similar material adverse effect on our business, financial condition, results of operations, and prospects.
Intellectual property litigation or other legal proceedings relating to intellectual property could cause us to spend substantial resources and distract our personnel from their normal responsibilities.
Even if resolved in our favor, litigation or other legal proceedings relating to intellectual property claims may cause us to incur significant expenses, and could distract our technical and management personnel from their normal responsibilities. In addition, there could be public announcements of the results of hearings, motions or other interim proceedings or developments and if securities analysts or investors perceive these results to be negative, it could have a substantial adverse effect on the price of our common stock. Such litigation or proceedings could substantially increase our operating losses and reduce the resources available for development activities or any future sales, marketing or distribution activities. We may not have sufficient financial or other resources to conduct such litigation or proceedings adequately. Some of our competitors may be able to sustain the costs of such litigation or proceedings more effectively than we can because of their greater financial resources and may also have an advantage in such proceedings due to their more mature and developed intellectual property portfolios. Uncertainties resulting from the initiation and continuation of intellectual property litigation or other proceedings could compromise our ability to compete in the marketplace.
Obtaining and maintaining patent protection depends on compliance with various procedural, document submission, fee payment and other requirements imposed by governmental patent agencies, and our patent protection could be reduced or eliminated for non-compliance with these requirements.
Periodic maintenance, renewal and annuity fees and various other government fees on any issued patent and pending patent application must be paid to the USPTO and foreign patent agencies in several stages or annually over the lifetime of our owned and in-licensed patents and patent applications. The USPTO and various foreign governmental patent agencies require compliance with a number of procedural, documentary, fee payment and other similar provisions during the patent application process. In certain circumstances, we rely on our licensing partners to pay these fees to, or comply with the procedural and documentary rules of, the relevant patent agency. With respect to our patents, we rely on an annuity service to remind us of the due dates and to make payment after we instruct them to do so. While an inadvertent lapse can in many cases be cured by payment of a late fee or by other means in accordance with the applicable rules, there are situations in which noncompliance can result in abandonment or lapse of the patent or patent application, resulting in partial or complete loss of patent rights in the relevant jurisdiction. Non-compliance events that could result in abandonment or lapse of a patent or patent application include failure to respond to official actions within prescribed time limits, non-payment of fees and failure to properly legalize and submit formal documents. In such an event, potential competitors might be able to enter the market with similar or identical products or technology. If we or our licensors fail to maintain the patents and patent applications directed to our drug candidates, it would have a material adverse effect on our business, financial condition, results of operations, and prospects.
101
If we fail to comply with our obligations in our intellectual property licenses and funding arrangements with third parties, we could lose rights that are important to our business.
We are party to license and funding agreements that impose, and we may enter into additional licensing and funding arrangements with third parties that may impose, diligence, development and commercialization timelines, milestone payment, royalty, insurance and other obligations on us. Under our existing licensing and funding agreements, we are obligated to pay certain specified milestone payments and royalties on net drug sales of drug candidates or related technologies to the extent they are covered by the agreements. If we fail to comply with such obligations under current or future license and funding agreements, our counterparties may have the right to terminate these agreements or require us to grant them certain rights. Such an occurrence could materially adversely affect the value of any drug candidate being developed under any such agreement. For example, under the AF Agreement, we are required to use commercially reasonable efforts to research, develop and commercialize LP-184. If we fail to meet the foregoing obligation, then, under certain circumstances, AF may terminate the AF Agreement and may exercise the exclusive, sub-licensable and worldwide license we granted AF in and to certain of our intellectual property to develop and commercialize LP-184. Termination of these agreements or reduction or elimination of our rights under these agreements may result in our having to negotiate new or reinstated agreements with less favorable terms, or cause us to lose our rights under these agreements, including our rights to important intellectual property or technology, which would have a material adverse effect on our business, financial condition, results of operations, and prospects.
Additionally, these and other license agreements may not provide exclusive rights to use the licensed intellectual property and technology in all relevant fields of use and in all territories in which we may wish to develop or commercialize our technology and drugs in the future. As a result, we may not be able to prevent competitors from developing and commercializing competitive products and technology in fields of use and territories not included in such agreements. In addition, we may not have the right to control the preparation, filing, prosecution, maintenance, enforcement, and defense of patents and patent applications directed to the technology that we license from third parties. Therefore, we cannot be certain that these patents and patent applications will be prepared, filed, prosecuted, maintained, and defended in a manner consistent with the best interests of our business. If our licensors fail to prosecute, maintain, enforce, and defend such patents, or lose rights to those patents or patent applications, the rights we have licensed may be reduced or eliminated, and our right to develop and commercialize any of our drugs that are the subject of such licensed rights could be adversely affected.
We may need to obtain additional licenses from others to advance our research or allow commercialization of our drug candidates. It is possible that we may be unable to obtain additional licenses at a reasonable cost or on reasonable terms, if at all, or such licenses may be non-exclusive. The licensing or acquisition of third-party intellectual property rights is a competitive area, and several more established companies may pursue strategies to license or acquire third-party intellectual property rights that we may consider attractive or necessary. These established companies may have a competitive advantage over us due to their size, capital resources and greater clinical development and commercialization capabilities. In addition, companies that perceive us to be a competitor may be unwilling to assign or license rights to us. We also may be unable to license or acquire third-party intellectual property rights on terms that would allow us to make an appropriate return on our investment or at all.
If we are unable to obtain rights to required third-party intellectual property rights or maintain the existing intellectual property rights we have, we may be required to expend significant time and resources to redesign our technology, drug candidates, or the methods for manufacturing them or to develop or license replacement technology, all of which may not be feasible on a technical or commercial basis. If we are unable to do so, we may be unable to develop or commercialize the affected technology and drug candidates, which could harm our business, financial condition, results of operations, and prospects significantly.
Disputes may arise regarding intellectual property subject to a licensing agreement, including:
| ● | the scope of rights granted under the license agreement and other interpretation related issues; |
| ● | the extent to which our technology and processes infringe on intellectual property of the licensor that is not subject to the licensing agreement; |
102
| ● | the sublicensing of patent and other rights under our collaborative development relationships; |
| ● | our diligence obligations under the license agreement and what activities satisfy those diligence obligations; |
| ● | the inventorship and ownership of inventions and know-how resulting from the joint creation or use of intellectual property by our licensors and us and our partners; and |
| ● | the priority of invention of patented technology. |
In addition, the agreements under which we currently license intellectual property or technology from third parties are complex, and certain provisions in such agreements may be susceptible to multiple interpretations. The resolution of any contract interpretation disagreement that may arise could narrow what we believe to be the scope of our rights to the relevant intellectual property or technology, or increase what we believe to be our financial or other obligations under the relevant agreement, either of which could have a material adverse effect on our business, financial condition, results of operations, and prospects. Moreover, if disputes over intellectual property that we have licensed prevent or impair our ability to maintain our current licensing arrangements on commercially acceptable terms, we may be unable to successfully develop and commercialize the affected technology and drug candidates, which could have a material adverse effect on our business, financial conditions, results of operations, and prospects.
Our licensors may have relied on third-party consultants or collaborators or on funds from third parties such that our licensors are not the sole and exclusive owners of the patents and patent applications we in-licensed. If other third parties have ownership rights to our in-licensed patents, they may be able to license such patents to our competitors, and our competitors could market competing products and technology. This could have a material adverse effect on our competitive position, business, financial conditions, results of operations, and prospects.
In spite of our best efforts, our licensors might conclude that we have materially breached our license agreements and might therefore terminate the license agreements, thereby removing our ability to develop and commercialize drug candidates and technology covered by these license agreements. If these in-licenses are terminated, or if the underlying intellectual property fails to provide the intended exclusivity, competitors would have the freedom to seek regulatory approval of, and to market, products and technologies identical to ours. This could have a material adverse effect on our competitive position, business, financial conditions, results of operations, and prospects.
We may not be able to protect our intellectual property and proprietary rights throughout the world.
Filing, prosecuting, and defending patents on drug candidates in all countries throughout the world would be prohibitively expensive, and the laws of foreign countries may not protect our rights to the same extent as the laws of the United States. Consequently, we may not be able to prevent third parties from practicing our inventions in all countries outside the United States, or from selling or importing products made using our inventions in and into the United States or other jurisdictions. Competitors may use our technologies in jurisdictions where we have not obtained patent protection to develop their own products and, further, may export otherwise infringing products to territories where we have patent protection or licenses but enforcement is not as strong as that in the United States. These products may compete with our products, and our patents or other intellectual property rights may not be effective or sufficient to prevent them from competing.
Many companies have encountered significant problems in protecting and defending intellectual property rights in foreign jurisdictions. The legal systems of certain countries, particularly certain developing countries, do not favor the enforcement of patents, trade secrets, and other intellectual property protection, particularly those relating to pharmaceutical products, which could make it difficult for us to stop the infringement of our patents or marketing of competing products in violation of our intellectual property and proprietary rights generally. Proceedings to enforce our intellectual property and proprietary rights in foreign jurisdictions could result in substantial costs and divert our efforts and attention from other aspects of our business, could put our patents at risk of being invalidated or interpreted narrowly, could put our patent applications at risk of not issuing, and could provoke third parties to assert claims against us. We may not prevail in any lawsuits that we initiate, and the damages or other remedies awarded, if any, may not be commercially meaningful. Accordingly, our efforts to enforce our intellectual property and proprietary rights around the world may be inadequate to obtain a significant commercial advantage from the intellectual property that we develop or license.
103
Many countries have compulsory licensing laws under which a patent owner may be compelled to grant licenses to third parties. In addition, many countries limit the enforceability of patents against government agencies or government contractors. In these countries, the patent owner may have limited remedies, which could materially diminish the value of such patent. If we or any of our licensors are forced to grant a license to third parties with respect to any patents relevant to our business, our competitive position may be impaired, and our business, financial condition, results of operations, and prospects may be adversely affected.
We may be subject to claims by third parties asserting that our employees, consultants, contractors or advisors have wrongfully used or disclosed alleged trade secrets of their current or former employers or claims asserting we have misappropriated their intellectual property, or claiming ownership of what we regard as our own intellectual property.
Many of our employees, consultants, contractors and advisors were previously employed, or may currently be employed, at universities or other pharmaceutical or biotechnology companies, including our competitors or potential competitors. Although we try to ensure that our employees, contractors and advisors do not use the proprietary information or know-how of others in their work for us, we may be subject to claims that these individuals or we have used or disclosed intellectual property, including trade secrets or other proprietary information, of any such individual’s current or former employer. Litigation may be necessary to defend against these claims.
In addition, while it is our policy to require our employees, consultants, contractors and advisors who may be involved in the development of intellectual property to execute agreements assigning such intellectual property to us, we may be unsuccessful in executing such an agreement with each party who in fact develops intellectual property that we regard as our own. Our intellectual property assignment agreements with them may not be self-executing or may be breached, and we may be forced to bring claims against third parties, or defend claims they may bring against us, to determine the ownership of what we regard as our intellectual property. Such claims could have a material adverse effect on our business, financial conditions, results of operations, and prospects.
If we fail in prosecuting or defending any such claims, in addition to paying monetary damages, we may lose valuable intellectual property rights or personnel, which could have a material adverse effect on our competitive business position and prospects. Such intellectual property rights could be awarded to a third party, and we could be required to obtain a license from such third party to commercialize our technology or products, which license may not be available on commercially reasonable terms, or at all, or such license may be non-exclusive. Even if we are successful in prosecuting or defending against such claims, litigation could result in substantial costs and be a distraction to our management and employees.
In addition to seeking patents for some of our technology and drug candidates, we also rely on trade secrets and confidentiality agreements relating to the development of our RADR® platform to protect our unpatented know-how, technology and other proprietary information, in order to maintain our competitive position. We seek to protect our trade secrets and other proprietary technology, in part, by entering into non-disclosure and confidentiality agreements with parties who have access to them, such as our employees, corporate collaborators, outside scientific collaborators, contract research organizations, contract manufacturers, consultants, advisors and other third parties. We also enter into confidentiality and invention or patent assignment agreements with our employees and consultants. We cannot guarantee that we have entered into such agreements with each party that may have or has had access to our trade secrets or proprietary technology. Despite these efforts, any of these parties may breach the agreements and disclose our proprietary information, including our trade secrets, and we may not be able to obtain adequate remedies for such breaches. Detecting the disclosure or misappropriation of a trade secret and enforcing a claim that a party illegally disclosed or misappropriated a trade secret is difficult, expensive and time-consuming, and the outcome is unpredictable. In addition, some courts inside and outside of the United States are less willing or unwilling to protect trade secrets. If any of our trade secrets were to be lawfully obtained or independently developed by a competitor or other third party, we would have no right to prevent them, or those to whom they communicate it, from using that technology or information to compete with us. If any of our trade secrets were to be disclosed to or independently developed by a competitor or other third party, our competitive position would be materially and adversely harmed.
104
Intellectual property rights do not necessarily address all potential threats.
The degree of future protection afforded by our intellectual property rights is uncertain because intellectual property rights have limitations and may not adequately protect our business or permit us to maintain our competitive advantage. For example:
| ● | our RADR® platform is not protected by any issued patents, and we may not be able to obtain, develop, acquire or in-license any patentable technologies or other intellectual property related to such platform; |
| ● | we, or our license partners or current or future collaborators, might not have been the first to make the inventions covered by the issued patent or pending patent applications that we license or may own in the future; |
| ● | we, or our license partners or current or future collaborators, might not have been the first to file patent applications covering certain of our or their inventions; |
| ● | others may independently develop similar or alternative technologies or duplicate any of our technologies without infringing our owned or in-licensed intellectual property rights; |
| ● | it is possible that our owned and in-licensed pending patent applications or those we may own or in-license in the future will not lead to issued patents; |
| ● | issued patents that we hold rights to may be held invalid or unenforceable, including as a result of legal challenges by our competitors; |
| ● | our competitors might conduct research and development activities in countries where we do not have patent rights and then use the information learned from such activities to develop competitive products for sale in our major commercial markets; |
| ● | we may not develop additional proprietary technologies that are patentable; |
| ● | the patents of others may harm our business; and |
| ● | we may choose not to file a patent in order to maintain certain trade secrets or know-how, and a third party may subsequently file a patent covering such intellectual property. |
Should any of these events occur, they could have a material adverse effect on our business, financial condition, results of operations, and prospects.
Risks Related to Owning our Common Stock
Our stock price has been volatile and thinly traded which may impair your ability to sell your shares.
Our common stock has traded on the Nasdaq Capital Market since June 11, 2020. Since then, our common stock has been relatively thinly traded, with an average daily trading volume of approximately 96,000 shares and prices ranging from a low of $10.40 to a high of $24.84 per share. There can be no assurance that the market for our common shares will become more liquid. The stock market in general, and early stage public companies in particular, has experienced extreme price and volume fluctuations that have often been unrelated or disproportionate to the operating performance of such companies. If we are unable to increase the trading volume for our common shares, you may not be able to sell your common shares at prices you consider to be fair or at times that are convenient for you, or at all.
105
Shares eligible for future sale may adversely affect the market for our common stock.
Of the 11,169,665 shares of our common stock outstanding as of the date of this report, approximately 7,750,558 shares are held by “non-affiliates” and are freely tradable without restriction pursuant to Rule 144 under the Securities Act. The market price of our common stock could decline as a result of sales of a large number of shares of our common stock in the market or the perception that these sales could occur. Such sales or offerings could lower the market price for our common stock and may make it more difficult for us to sell equity securities in the future at a time and at a price that we deem appropriate. We may in the future sell additional shares of our common stock or equity-linked securities to raise capital. A substantial number of shares of our common stock could be registered and issued. Furthermore, there are substantial amounts of vested stock options which are “in the money” which could be exercised and sold in public markets. We continue to expect to issue stock options as part of compensation. There may be further effect on our stock price upon the vesting and settlement of restricted stock units and performance units. We cannot predict the size of future issuances or the effect, if any, that they may have on the market price for our common stock. The issuance and sale of substantial amounts of common stock or equity-linked securities, or the perception that such issuances and sales may occur, could adversely affect the trading price of our common stock and impair our ability to raise capital through the sale of additional equity or equity-linked securities. Additional dilution may also result as a consequence of shares of common stock sold pursuant to potential future offerings as well as if outstanding options to acquire shares of our common stock are exercised.
In addition, holders of up to approximately 3,192,345 shares of our common stock, including shares of common stock issuable under outstanding options and warrants, have the right to require us to register these shares under the Securities Act pursuant to an Amended and Restated Investors’ Rights Agreement and the terms of warrants issued to the underwriters in connection with our IPO. If our existing stockholders sell substantial amounts of our common stock in the public market, or if the public perceives that such sales could occur, this could have an adverse impact on the market price of our common stock, even if there is no relationship between such sales and the performance of our business.
The price of our common stock may fluctuate substantially.
You should consider an investment in our common stock to be risky, and you should invest in our common stock only if you can withstand a significant loss and wide fluctuations in the market value of your investment. Some factors that may cause the market price of our common stock to fluctuate, in addition to the other risks mentioned in this “Risk Factors” section and elsewhere in this report, are:
| ● | sale of our common stock by our stockholders, executives, and directors; |
| ● | volatility and limitations in trading volumes of our shares of common stock; |
| ● | our ability to obtain financings to conduct and complete research and development activities including, but not limited to, our proposed clinical trials, and other business activities; |
| ● | possible delays in the expected recognition of revenue due to lengthy and sometimes unpredictable product development and sales timelines; |
| ● | the timing and success of introductions of new technologies, therapeutic approaches, product candidates and product marketing applications by us or our competitors or any other change in the competitive dynamics of our industry, including consolidation among competitors, customers or strategic partners; |
| ● | network outages or security breaches; |
| ● | the lack of market acceptance and sales growth for our drug candidates, if any, that receive marketing approval; |
| ● | our ability to secure resources and the necessary personnel to conduct clinical trials on our desired schedule; |
| ● | commencement, enrollment or results of our clinical trials for our drug candidates or any future clinical trials we may conduct; |
| ● | changes in the development status of our drug candidates; |
106
| ● | any delays or adverse developments or perceived adverse developments with respect to the FDA’s review of our planned preclinical studies and clinical trials; |
| ● | any delay in our submission for studies or drug approvals or adverse regulatory decisions, including failure to receive regulatory approval for our drug candidates; |
| ● | unanticipated safety concerns related to the use of our drug candidates; |
| ● | failures to meet external expectations or management guidance; |
| ● | changes in our capital structure or dividend policy, future issuances of securities, sales of large blocks of common stock by our stockholders; |
| ● | our cash position; |
| ● | announcements and events surrounding financing efforts, including debt and equity securities; |
| ● | our inability to enter into new markets or develop new drugs; |
| ● | reputational issues; |
| ● | competition from existing technologies and drugs or new technologies and drugs that may emerge; |
| ● | announcements of acquisitions, partnerships, collaborations, joint ventures, new drugs, capital commitments, or other events by us or our competitors; |
| ● | changes in general economic, political and market conditions in or any of the regions in which we conduct our business; |
| ● | changes in industry conditions or perceptions; |
| ● | changes in valuations of similar companies or groups of companies; |
| ● | analyst research reports, recommendations and changes in recommendations, price targets, and withdrawals of coverage; |
| ● | departures and additions of key personnel; |
| ● | disputes and litigations related to intellectual properties, proprietary rights, and contractual obligations; |
| ● | changes in applicable laws, rules, regulations, or accounting practices and other dynamics; and |
| ● | other events or factors, many of which may be out of our control. |
In addition, if the market for stocks in our industry or industries related to our industry, or the stock market in general, experiences a loss of investor confidence, the trading price of our common stock could decline for reasons unrelated to our business, financial condition and results of operations. If any of the foregoing occurs, it could cause our stock price to fall and may expose us to lawsuits that, even if unsuccessful, could be costly to defend and a distraction to management.
107
We have broad discretion in the use of our financial resources and may not use them effectively.
Our management will have broad discretion in the application of our financial resources. Because of the number and variability of factors that will determine our use of our financial resources, their ultimate use may vary substantially from their currently intended use. Our management may not apply our financial resources in ways that ultimately increase the value of any investment in our securities or enhance stockholder value. The failure by our management to apply these funds effectively could harm our business. We have invested and may in the future invest our cash in short-term, interest-bearing securities. These investments may not yield a favorable return to our stockholders. If we do not invest or apply our cash in ways that enhance stockholder value, we may fail to achieve expected financial results, which may result in a decline in the price of our shares of common stock, and, therefore, may negatively impact our ability to raise capital, invest in or expand our business, acquire additional drugs or licenses, commercialize our drugs, or continue our operations.
We may acquire other companies or technologies, which could divert our management’s attention, result in dilution to our stockholders and otherwise disrupt our operations and adversely affect our operating results.
We may in the future seek to acquire or invest in businesses, product applications and services or technologies that we believe could complement or expand our existing product candidates and business, enhance our technical capabilities or otherwise offer growth opportunities. The pursuit of potential acquisitions may divert the attention of management and cause us to incur various expenses in identifying, investigating and pursuing suitable acquisitions, whether or not they are consummated.
In addition, we do not have any experience in acquiring other businesses. If we acquire additional businesses, we may not be able to integrate the acquired personnel, operations and technologies successfully or effectively manage the combined business following the acquisition. We also may not achieve the anticipated benefits from the acquired business due to a number of factors, including:
| ● | inability to integrate or benefit from acquired businesses, products, technologies or services in a profitable manner; |
| ● | unanticipated costs or liabilities associated with the acquisition; |
| ● | difficulty integrating the accounting systems, operations and personnel of the acquired business; |
| ● | difficulties and additional expenses associated with supporting legacy drugs and hosting infrastructure of the acquired business; |
| ● | difficulty maintaining the customers, if any, of the acquired business, including disparities in the revenue, licensing, support or business model of the acquired company; |
| ● | diversion of management’s attention from other business concerns; |
| ● | adverse effects to our existing business relationships with business partners and customers, if any, as a result of the acquisition; |
| ● | the potential loss of key employees; |
| ● | use of resources that are needed in other parts of our business; and |
| ● | use of substantial portions of our available cash to consummate the acquisition. |
In addition, a significant portion of the purchase price of companies we acquire may be allocated to acquired goodwill and other intangible assets, which must be assessed for impairment at least annually. In the future, if our acquisitions do not yield expected returns, we may be required to take charges to our operating results based on this impairment assessment process, which could adversely affect our results of operations.
Acquisitions could also result in dilutive issuances of equity securities or the incurrence of debt, which could adversely affect our operating results. In addition, if an acquired business fails to meet our expectations, our operating results, business and financial position may suffer.
108
Market and economic conditions may negatively impact our business, financial condition and share price.
Concerns over inflation, energy costs, geopolitical issues, the U.S. mortgage market and a declining real estate market, unstable global credit markets and financial conditions, and volatile oil prices have led to periods of significant economic instability, diminished liquidity and credit availability, declines in consumer confidence and discretionary spending, diminished expectations for the global economy and expectations of slower global economic growth going forward, increased unemployment rates, and increased credit defaults in recent years. Our general business strategy may be adversely affected by any such economic downturns, volatile business environments and continued unstable or unpredictable economic and market conditions. If these conditions continue to deteriorate or do not improve, it may make any necessary debt or equity financing more difficult to complete, more costly, and more dilutive. Failure to secure any necessary financing in a timely manner and on favorable terms could have a material adverse effect on our growth strategy, financial performance, and share price and could require us to delay or abandon development or commercialization plans.
If securities or industry analysts do not publish research or reports, or publish unfavorable research or reports about our business, our stock price and trading volume may decline.
The trading market for our common stock will rely in part on the research and reports that industry or financial analysts publish about us, our business, our markets and our competitors. We do not control these analysts. If securities analysts do not cover our common stock, the lack of research coverage may adversely affect the market price of our common stock. Furthermore, if one or more of the analysts who do cover us downgrade our stock or if those analysts issue other unfavorable commentary about us or our business, our stock price would likely decline. If one or more of these analysts cease coverage of us or fails to regularly publish reports on us, we could lose visibility in the market and interest in our stock could decrease, which in turn could cause our stock price or trading volume to decline and may also impair our ability to expand our business with existing customers and attract new customers.
Because certain of our stockholders control a significant number of shares of our common stock, they may have effective control over actions requiring stockholder approval.
Our directors, executive officers, and their respective affiliates, beneficially own approximately 30.3% of our outstanding shares of common stock. As a result, these stockholders, acting together, would have the ability to control the outcome of matters submitted to our stockholders for approval, including the election of directors and any merger, consolidation or sale of all or substantially all of our assets. In addition, these stockholders, acting together, would have the ability to control the management and affairs of our company. Accordingly, this concentration of ownership might harm the market price of our common stock by:
| ● | delaying, deferring or preventing a change in corporate control; |
| ● | impeding a merger, consolidation, takeover or other business combination involving us; or |
| ● | discouraging a potential acquirer from making a tender offer or otherwise attempting to obtain control of us. |
Future sales and issuances of our common stock could result in additional dilution of the percentage ownership of our stockholders and could cause our share price to fall.
We expect that significant additional capital will be needed in the future to continue our planned operations, including increased marketing, hiring new personnel, commercializing our drugs, and continuing activities as an operating public company. To the extent we raise additional capital by issuing equity securities; our stockholders may experience substantial dilution. We may sell common stock, convertible securities or other equity securities in one or more transactions at prices and in a manner we determine from time to time. If we sell common stock, convertible securities or other equity securities in more than one transaction, investors may be materially diluted by subsequent sales. Such sales may also result in material dilution to our existing stockholders, and new investors could gain rights superior to our existing stockholders.
109
We do not intend to pay cash dividends on our shares of common stock so any returns will be limited to the value of our shares.
We currently anticipate that we will retain future earnings for the development, operation and expansion of our business and do not anticipate declaring or paying any cash dividends for the foreseeable future. Any return to stockholders will therefore be limited to the increase, if any, of our share price.
We are an “emerging growth company” and will be able to avail ourselves of reduced disclosure requirements applicable to emerging growth companies, which could make our common stock less attractive to investors.
We are an “emerging growth company,” as defined in the Jumpstart Our Business Startups Act of 2012, or the JOBS Act, and we intend to take advantage of certain exemptions from various reporting requirements that are applicable to other public companies that are not “emerging growth companies” including not being required to comply with the auditor attestation requirements of Section 404(b) of the Sarbanes-Oxley Act, reduced disclosure obligations regarding executive compensation in our periodic reports and proxy statements, and exemptions from the requirements of holding a nonbinding advisory vote on executive compensation and stockholder approval of any golden parachute payments not previously approved. In addition, Section 107 of the JOBS Act also provides that an “emerging growth company” can take advantage of the extended transition period provided in Section 7(a)(2)(B) of the Securities Act, for complying with new or revised accounting standards. In other words, an “emerging growth company” can delay the adoption of certain accounting standards until those standards would otherwise apply to private companies. We are not electing to delay such adoption of new or revised accounting standards, and as a result, we will comply with new or revised accounting standards on the relevant dates on which adoption of such standards is required for non-emerging growth companies. We cannot predict if investors will find our common stock less attractive because we may rely on these exemptions. If some investors find our common stock less attractive as a result, there may be a less active trading market for our common stock and our stock price may be more volatile. We may take advantage of these reporting exemptions until we are no longer an “emerging growth company.” We will remain an “emerging growth company” until the earliest of (i) the last day of the fiscal year in which we have total annual gross revenues of $1.07 billion or more; (ii) the last day of our fiscal year following the fifth anniversary of the date of the completion of our initial public offering, or December 31, 2025; (iii) the date on which we have issued more than $1 billion in nonconvertible debt during the previous three years; or (iv) the date on which we are deemed to be a large accelerated filer under the rules of the SEC.
We may be at risk of securities class action litigation.
We may be at risk of securities class action litigation. In the past, biotechnology and pharmaceutical companies have experienced significant stock price volatility, particularly when associated with binary events such as clinical trials and drug approvals. If we face such litigation, it could result in substantial costs and a diversion of management’s attention and resources, which could harm our business and result in a decline in the market price of our common stock.
Our certificate of incorporation and our by-laws, and Delaware law may have anti-takeover effects that could discourage, delay or prevent a change in control, which may cause our stock price to decline.
Our certificate of incorporation, and our by-laws, and Delaware law could make it more difficult for a third party to acquire us, even if closing such a transaction would be beneficial to our stockholders. We are authorized to issue up to 1,000,000 shares of preferred stock. This preferred stock may be issued in one or more series, the terms of which may be determined at the time of issuance by our board of directors without further action by stockholders. The terms of any series of preferred stock may include voting rights (including the right to vote as a series on particular matters), preferences as to dividend, liquidation, conversion and redemption rights and sinking fund provisions. None of our preferred stock is currently outstanding. The issuance of any preferred stock could materially adversely affect the rights of the holders of our common stock, and therefore, reduce the value of our common stock. In particular, specific rights granted to future holders of preferred stock could be used to restrict our ability to merge with, or sell our assets to, a third party and thereby preserve control by the present management.
110
Provisions of our certificate of incorporation, by-laws and Delaware law also could have the effect of discouraging potential acquisition proposals or making a tender offer or delaying or preventing a change in control, including changes a stockholder might consider favorable. Such provisions may also prevent or frustrate attempts by our stockholders to replace or remove our management. In particular, our certificate of incorporation and by-laws and Delaware law, as applicable, among other things:
| ● | provide the board of directors with the ability to alter the by-laws without stockholder approval; |
| ● | establishing advance notice requirements for nominations for election to the board of directors or for proposing matters that can be acted upon at stockholder meetings; and |
| ● | provide that vacancies on the board of directors may be filled by a majority of directors in office, although less than a quorum. |
Our by-laws designate the Court of Chancery of the State of Delaware (or, if the Court of Chancery does not have jurisdiction, the federal district court for the District of Delaware) as the exclusive forum for certain types of claims, which may limit a stockholder’s ability to bring a claim in a judicial forum that it finds favorable.
Section 7.06 of our by-laws specifies that unless we consent in writing to the selection of an alternative forum, the court of Chancery of the State of Delaware (or, if the Court of Chancery does not have jurisdiction, the federal district court for the District of Delaware) shall, to the fullest extent permitted by law, be the sole and exclusive forum for: (a) any derivative action or proceeding brought on our behalf; any action asserting a claim of breach of fiduciary duty owed by any of our directors, officers or other employees to us or to our stockholders; (b) any action asserting a claim against us arising pursuant to the Delaware General Corporation Law (“DGCL”) or certificate of incorporation or our by-laws; or (c) or any action asserting a claim against us that is governed by the internal affairs doctrine. There is uncertainty as to whether a court would enforce this provision with respect to claims under the Securities Act and our stockholders cannot waive compliance with the federal securities laws and the rules and regulations thereunder. The exclusive forum provision may limit a stockholder’s ability to bring a claim in a judicial forum that it finds favorable for disputes against us and our directors, officers and other employees, which may discourage such lawsuits, or may require increased costs to bring a claim.
Financial reporting obligations of being a public company in the United States require well defined disclosure and financial controls and procedures that are expensive and time-consuming requiring our management to devote substantial time to compliance matters.
As a publicly traded company, we incur significant additional legal, accounting and other expenses that a privately held company is not required to incur. For example, a privately held company is not required to have well defined disclosure and financial controls and procedures or systems of internal controls over financial reporting that are generally required of publicly held companies. In connection with our review of our previously existing internal controls as part of our preparations for becoming a publicly traded company, we determined that our internal controls over financial reporting for prior periods were inadequate and included material weaknesses that needed to be remedied. Although we have taken, and are continuing to take, additional steps to remedy these material weaknesses in order to assure compliance with our future financial reporting obligations, there can be no assurance that we will be able to do so in a timely manner or at all.
These reporting obligations associated with being a public company in the United States require significant expenditures and will place significant demands on our management and other personnel, including costs resulting from our reporting obligations under the Securities Exchange Act of 1934, as amended, (the “Exchange Act”), and the rules and regulations regarding corporate governance practices, including those under the Sarbanes-Oxley Act of 2002, as amended, (the “Sarbanes-Oxley Act”), the Dodd-Frank Wall Street Reform and Consumer Protection Act, as amended, (the “Dodd-Frank Act”), and the listing requirements of the stock exchange on which our securities are to be listed. These rules require the establishment and maintenance of effective disclosure and financial controls and procedures, internal control over financial reporting and changes in corporate governance practices, among many other complex rules that are often difficult to implement, monitor and maintain compliance with. Moreover, despite recent reforms made possible by the JOBS Act, the reporting requirements, rules, and regulations make some activities more time-consuming and costly, which will be particularly true after we are no longer an “emerging growth company.” In addition, we expect these rules and regulations will make it more difficult and more expensive for us to obtain director and officer liability insurance. Our management and other personnel have to devote a substantial amount of time to ensure that we comply with all of these requirements and to keep pace with new regulations, otherwise we may fall out of compliance and risk becoming subject to litigation or being delisted, among other potential problems.
111
If we fail to comply with the rules under the Sarbanes-Oxley Act related to accounting controls and procedures in the future, or, if we discover additional material weaknesses and other deficiencies in our internal control and accounting procedures, our stock price could decline significantly and raising capital could be more difficult.
Section 404 of the Sarbanes-Oxley Act requires annual management assessments of the effectiveness of our internal control over financial reporting after a transition period ending with our second annual report on Form 10-K filed under Section 13(a) of the Exchange Act. If we fail to comply with the rules under the Sarbanes-Oxley Act related to disclosure controls and procedures in the future, or, if in the future we discover additional material weaknesses and other deficiencies in our internal control and accounting procedures, our stock price could decline significantly and raising capital could be more difficult.
Comprehensive tax reform bills could adversely affect our business and financial condition.
The U.S. government recently enacted comprehensive federal income tax legislation that includes significant changes to the taxation of business entities. These changes include, among others, a permanent reduction to the corporate income tax rate. Notwithstanding the reduction in the corporate income tax rate, the overall impact of this tax reform is uncertain, and our business and financial condition could be adversely affected. This report does not discuss any such tax legislation or the manner in which it might affect purchasers of our common stock. We urge our stockholders to consult with their legal and tax advisors with respect to any such legislation and the potential tax consequences of investing in our common stock.
Item 1B. Unresolved Staff Comments.
None.
Our principal executive office is located at 1920 McKinney Avenue, 7th Floor, Dallas, Texas 75201. During 2020, we leased office space and access to meeting facilities at this location under month-to-month lease arrangements. In connection with our employees working remotely due to COVID-19, in August 2020 we reduced our monthly lease commitment and costs to minimal levels. We are continuing to monitor the COVID-19 conditions and intend to increase our lease of office space following an improvement in the COVID-19 situation. We intend to add new facilities, add to existing space, or replace with larger facilities, as needed, as we add employees and expand operations. We believe that suitable additional or substitute space will be available in the future on commercially reasonable terms to support this expansion.
From time to time in the future, we may become involved in litigation or other legal proceedings that arise in the ordinary course of business. We are not currently a party to any legal proceedings, and we are not aware of any pending or threatened litigation against us that we believe could have a material adverse effect on our business, operating results or financial condition. In the event we are subject to a legal proceeding, it could have a material adverse impact on us because of litigation costs and diversion of management resources.
Item 4. Mine Safety Disclosures.
Not applicable.
112
Item 5. Market for Registrant’s Common Equity, Related Stockholder Matters and Issuer Purchases of Equity Securities.
Market Information
Our common stock began trading on the Nasdaq Capital Market under the symbol “LTRN” on June 11, 2020. Prior to that date, there was no public trading market for our common stock.
Stockholders
As of March 8, 2021, there were 26 stockholders of record of our common stock. The actual number of holders of our common stock is greater than this number of record holders, and includes stockholders who are beneficial owners, but whose shares are held in street name by brokers or held by other nominees.
Dividend Policy
We have never paid or declared any cash dividends on our common stock, and we do not anticipate declaring or paying, in the foreseeable future, any cash dividends on our capital stock. We intend to retain all available funds and future earnings, if any, to fund the development and expansion of our business, and we do not anticipate paying any cash dividends in the foreseeable future. Any future determination regarding the declaration and payment of dividends, if any, will be at the discretion of our board of directors and will depend on then-existing conditions, including our financial condition, operating results, contractual restrictions, capital requirements, business prospects and other factors our board of directors may deem relevant.
Unregistered Sales of Securities
Options
In January 2020, an option holder exercised options to purchase 50,460 shares of common stock in cash at an exercise price of $1.03 per share of common stock for an aggregate purchase price of $51,910.
Exercise of Warrants
In October 2020, a warrant holder acquired 3,350 shares of common stock pursuant to the cashless exercise of a warrant to purchase 4,022 shares. In January 2021, a warrant holder acquired 800 shares of common stock pursuant to the cashless exercise of a warrant to purchase 957 shares. In January 2021, three warrant holders acquired an aggregate of 19,367 shares pursuant to the cash exercise of warrants. All of such warrants were exercisable at an exercise price of $3.13 per share of common stock. The aggregate cash proceeds received by the Company from the exercise of such warrants was $60,619.
None of the foregoing transactions involved any underwriters, underwriting discounts or commissions, or any public offering. We believe the offers, sales and issuances of the above securities were exempt from registration under the Securities Act (or Regulation D promulgated thereunder) by virtue of Section 4(a)(2) of the Securities Act because the issuance of securities to the recipients did not involve a public offering. The recipients of the securities in each of these transactions represented their intentions to acquire the securities for investment only and not with a view to or for sale in connection with any distribution thereof, and appropriate legends were placed upon the stock certificates issued in these transactions. The sales of these securities were made without any general solicitation or advertising.
113
Securities Authorized for Issuance under Equity Compensation Plans
The table below contains information as of December 31, 2020 regarding the Amended and Restated Lantern Pharma Inc. 2018 Equity Incentive Plan (the “Plan”). Additional information regarding the Plan is contained in Note 6 to our consolidated financial statements included as part of this report. The Company does not have any equity compensation plans that have not been approved by stockholders.
|
Plan category |
Number of securities to be issued upon exercise of outstanding options, warrants and rights |
Weighted-average exercise price of outstanding options, warrants and rights |
Number of securities remaining available for future issuance under equity compensation plans (excluding securities reflected in column (a)) |
| (a) | (b) | (c) | |
| Equity compensation plans approved by security holders |
835,608 shares of Common Stock |
$6.41 per share |
535,099 shares of Common Stock |
| Equity compensation plans not approved by security holders |
N/A |
N/A |
N/A |
| Total: | 835,608 shares of Common Stock | $6.41 per share |
535,099 shares of Common Stock |
Use of proceeds from our initial public offering of common stock
On June 10, 2020, our registration statement on Form S-1, as amended (File No. 333-237714) was declared effective by the SEC in connection with our initial public offering of common stock, pursuant to which we issued and sold, on June 15, 2020, 1,750,000 shares of common stock at a public offering price of $15.00 per share for total gross proceeds of $26,250,000. On June 15, 2020 we received net proceeds of $23,419,721, after deducting underwriting discounts and commissions of $1,968,750 and other offering expenses of $861,529 borne by us.
As of December 31, 2020, we estimate that we have used approximately $4,569,000 of the net proceeds from our IPO for advancing and developing our drug candidates and RADR® platform, and for working capital and other general corporate purposes, including payment of director and officer liability insurance premium amounts of approximately $1,810,000, approximately $1,009,000 of which have been expensed through December 31, 2020 and approximately $801,000 of which are included as part of prepaid expenses and other current assets on the Company’s condensed consolidated balance sheet at December 31, 2020. Substantially all of the unused net proceeds from the offering are held in interest bearing accounts. There has been no material change in our use of the net proceeds from the IPO as described in our final prospectus filed pursuant to Rule 424(b)(4) under the Securities Act with the SEC on June 10, 2020. Other than payments in the ordinary course of business for compensation of officers and to non-employee directors as compensation for board or board committee service, none of the net proceeds from our IPO used by us were direct or indirect payments to any of (i) our directors or officers or their associates, (ii) persons owning 10 percent or more of our common stock, or (iii) our affiliates.
Item 6. Selected Financial Data.
As a Smaller Reporting Company we are exempt from the requirements of Item 6.
114
Item 7. Management’s Discussion and Analysis of Financial Condition and Results of Operations.
You should read the following discussion and analysis of our financial condition and plan of operations together with our financial statements and the related notes appearing elsewhere in this Annual Report on Form 10-K. In addition to historical information, this discussion and analysis contains forward-looking statements that involve risks, uncertainties and assumptions. Our actual results may differ materially from those discussed below. Factors that could cause or contribute to such differences include, but are not limited to, those identified below, and those discussed in Item 1A titled “Risk Factors” included elsewhere in this Annual Report on Form 10-K.
Overview
We are a clinical stage biotechnology company, focused on leveraging artificial intelligence (“A.I.”), machine learning and genomic data to streamline the drug development process and to identify the patients that will benefit from our targeted oncology therapies. Our portfolio of therapies consists of small molecules that others have tried, but failed, to develop into an approved commercialized drug, as well as new compounds that we are developing with the assistance of our proprietary A.I. platform and our biomarker driven approach. Our A.I. platform, known as RADR® , currently includes more than 1.2 billion data points, and uses big data analytics (combining molecular data, drug efficacy data, data from historical studies, data from scientific literature, phenotypic data from trials and publications, and mechanistic pathway data) and machine learning to rapidly uncover biologically relevant genomic signatures correlated to drug response, and then identify the cancer patients that we believe may benefit most from our compounds. This data-driven, genomically-targeted and biomarker-driven approach allows us to pursue a transformational drug development strategy that identifies, rescues or develops, and advances potential small molecule drug candidates at what we believe is a fraction of the time and cost associated with traditional cancer drug development.
Our strategy is to both develop new drug candidates using our RADR® platform, and other machine learning driven methodologies, and to pursue the development of drug candidates that have undergone previous clinical trial testing or that may have been halted in development or deprioritized because of insufficient clinical trial efficacy (i.e., a meaningful treatment benefit relevant for the disease or condition under study as measured against the comparator treatment used in the relevant clinical testing) or for strategic reasons by the owner or development team responsible for the compound. Importantly, these historical drug candidates appear to have been well-tolerated in many instances, and often have considerable data from previous toxicity, tolerability and ADME (absorption, distribution, metabolism, and excretion) studies that have been completed. Additionally, these drug candidates may also have a body of existing data supporting the potential mechanism(s) by which they achieve their intended biologic effect, but often require more targeted trials in a stratified group of patients to demonstrate statistically meaningful results. Our dual approach to both develop de-novo, biomarker-guided drug candidates and “rescue” historical drug-candidates by leveraging A.I., recent advances in genomics, computational biology and cloud computing is emblematic of a new era in drug development that is being driven by data-intensive approaches meant to de-risk development and accelerate the clinical trial process. In this context, we intend to create a diverse portfolio of oncology drug candidates for further development towards regulatory and marketing approval with the objective of establishing a leading A.I.-driven, methodology for treating the right patient with the right oncology therapy.
A key component of our strategy is to target specific cancer patient populations and treatment indications identified by leveraging our RADR®platform, a proprietary A.I. enabled engine created and owned by us. We believe the combination of our therapeutic area expertise, our A.I. expertise, and our ability to identify and develop promising drug candidates through our collaborative relationships with research institutions in selected areas of oncology gives us a significant competitive advantage. Our RADR® platform was developed and refined over the last four years and integrates millions of data points immediately relevant for oncology drug development and patient response prediction using artificial intelligence and proprietary machine learning algorithms. By identifying clinical candidates, together with relevant genomic and phenotypic data, we believe our approach will help us design more efficient pre-clinical studies, and more targeted clinical trials, thereby accelerating our drug candidates’ time to approval and eventually to market. Although we have not yet applied for or received regulatory or marketing approval for any of our drug candidates, we believe our RADR® platform has the ability to reduce the cost and time to bring drug candidates to specifically targeted patient groups. We believe we have developed a sustainable and scalable biopharma business model by combining a unique, oncology-focused big-data platform that leverages artificial intelligence along with active clinical and preclinical programs that are being advanced in targeted cancer therapeutic areas to address today’s treatment needs.
115
Our current portfolio consists of four compounds in active development: two drug candidates in clinical phases, one in preclinical studies and one in research optimization. All of these drug candidates are leveraging precision oncology, A.I. and genomic driven approaches to accelerate and direct development efforts. We currently have two drug candidates in clinical development, LP-100 and LP-300, where we are leveraging data from prior preclinical studies and clinical trials, along with insights generated from our A.I. platform, to target the types of tumors and patient groups that would be most responsive to the drug. Both LP-100 and LP-300 showed promise in important patient subgroups, but failed pivotal Phase III trials when the overall results did not meet the predefined clinical endpoints. We believe that this was due to a lack of biomarker-driven patient stratification. Additionally, we have one new drug candidate, LP-184, in preclinical development for two potentially distinct indications where we are leveraging machine learning and genomic data to streamline the drug development process and to identify the patients and cancer subtypes that will best benefit from the drug, if approved. As part of our antibody drug conjugate (ADC) program commenced in early 2021, we have initiated the optimization and evaluation of an antibody drug conjugate aimed at leveraging our LP-184 molecule in combination with an antibody for select solid tumors.
Our development strategy is to pursue an increasing number of oncology focused, molecularly targeted therapies where artificial intelligence and genomic data can help us provide biological insights, reduce the risk associated with development efforts and help clarify potential patient response. We plan on strategically evaluating these on a program-by-program basis as they advance into clinical development, either to be done entirely by us or with our licensing partners to maximize the commercial opportunity and reduce the time it takes to bring the right drug to the right patient
To date, except for a research grant in 2017, we have not generated any revenue, we have incurred net losses and our operations have been financed primarily by sales of our equity securities. Our net losses were approximately $5,908,000 and $2,428,000 for the years ended December 31, 2020 and 2019, respectively.
Our net losses have primarily resulted from costs incurred in licensing and developing the drug candidates in our pipeline, planning, preparing and conducting preclinical studies, early stage clinical testing and general and administrative activities associated with our operations. We expect to continue to incur significant expenses and corresponding increased operating losses for the foreseeable future as we continue to develop our pipeline. Our costs may further increase as we conduct preclinical studies and clinical trials and potentially seek regulatory clearance for and prepare to commercialize our drug candidates. We expect to incur significant expenses to continue to build the infrastructure necessary to support our expanded operations, preclinical studies, clinical trials, commercialization, including manufacturing, marketing, sales and distribution functions. We have experienced and will continue to experience increased costs associated with operating as a public company.
Our operations, including the development of our drug candidates, could be disrupted and materially adversely affected in the future by a pandemic, epidemic or outbreak of an infectious disease like the outbreak of COVID-19. For example, as a result of measures imposed by the governments in regions affected by COVID-19, businesses and schools have been suspended due to quarantines or “stay at home” orders intended to contain this outbreak. The spread of COVID-19 from China to other countries has resulted in the Director General of the World Health Organization declaring the outbreak of COVID-19 as a Public Health Emergency of International Concern (PHEIC), based on the advice of the Emergency Committee under the International Health Regulations (2005). On March 12, 2020, the President of the United States imposed international travel restrictions between the U.S. and Europe to supplement the existing international travel restrictions between the US and certain Asian countries and, on March 13, 2020, declared a national emergency in response to the likely spread of COVID-19. COVID-19 continues to spread globally and, as of December 31, 2020, has spread to over 150 countries, including the United States. U.S. and international stock markets continue to experience fluctuations and to be impacted from time to time by uncertainty associated with the impact of COVID-19 on the U.S., Chinese, European and other economies and the reduced levels of international travel experienced since early 2020. The Dow Industrial Average and other domestic and international stock indices experienced substantial fluctuations during 2020 largely attributed to assessments and expectations regarding the adverse effects of the pandemic on the world’s economies. We are continuing to assess our business plans and the impact COVID-19 may have on our operations and plans, including the ability to advance the development of our drug candidates, but no assurances can be given that this analysis will enable us to avoid part or all of any impact from the spread of COVID-19 or its consequences, including downturns in business sentiment generally or in our sector in particular. The extent to which COVID-19 impacts our operations and plans will depend on future developments, which are highly uncertain and cannot be predicted with confidence, including the duration of the outbreak, new information which may emerge concerning the severity and treatment of COVID-19, and preventative or protective actions that governments, businesses, and organizations performing research and clinical trials may take in respect of COVID-19, among others. The existence and spread of an infectious disease, including COVID-19, may also result in the inability of our suppliers to deliver components or raw materials on a timely basis or materially and adversely affect our collaborators and out-license partner’s ability to perform and advance preclinical and nonclinical studies and clinical trials. For example, Allarity Therapeutics (formerly known as Oncology Venture) has informed us that continuing enrollment in the Phase II clinical trial for LP-100 (Irofulven) has slowed during the pandemic. The timing of non-clinical research studies for our drug candidates by collaborators and service providers also slowed during the second and third quarters of 2020 in connection with the pandemic.
116
Components of Our Results of Operations
Revenues
We did not recognize revenues for the years ended December 31, 2020 and 2019.
General and Administrative
General and administrative expenses consist of our operating expenses that are not included in the direct costs of production or cost of goods sold which include:
| ● | corporate office overhead expenses such as salaries of administrative staff and corporate officers; |
| ● | legal expenses; |
| ● | accounting expenses; and |
| ● | rent, utilities and supplies. |
Research and Development
Research and development expenses consist primarily of costs incurred for the research and development of our preclinical and clinical candidates, which include:
| ● | expenses incurred towards consultants, laboratories and investigators that conduct our preclinical or clinical research activities; and |
| ● | the cost of acquiring and developing preclinical study materials and lab supplies. We expense research and development costs to operations as incurred. |
For the years ended December 31, 2020 and 2019, we incurred an aggregate of approximately $2,243,000 and $953,000, respectively, in research and development expenses related to the development of LP-100, LP- 184, LP 300 and our RADR®platform. We expect that our research and development expenses will increase as we plan for and commence our clinical trials of LP-184 and LP-300.
117
Our research and development costs by project category for the year ended December 31, 2020 are as follows:
| Year ended December 31, 2020 | ||||
| LP-300 | $ | 455,914 | ||
| LP-184 | 939,093 | |||
| RADR®platform | 443,152 | |||
| Other | 267,962 | |||
| Unallocated* | 137,104 | |||
| Total Research & Development Expenses | $ | 2,243,225 | ||
*As a private company, we did not track our research and development costs by project category primarily because research and development salary expenses were not further allocated to each project. As a result, our tracking of research and development costs by project category commenced during the three months ended June 30, 2020 in connection with the Company’s IPO.
We expect that our research and development expenses will increase as we plan for and commence our clinical trials of LP-184 and LP-300.
Because of the numerous risks and uncertainties associated with product development, we cannot determine with certainty the duration and completion costs of these or other current or future clinical trials of LP-184 and LP-300 or our other therapeutic candidates. We may never succeed in achieving regulatory approval for LP-184 and LP-300 or any of our other drug candidates. The duration, costs and timing of clinical trials and development of our therapeutic candidates will depend on a variety of factors, including the uncertainties of future clinical and preclinical studies, uncertainties in clinical trial enrollment rate and significant and changing government regulation. In addition, the probability of success for each drug candidate will depend on numerous factors, including competition, manufacturing capability and commercial viability.
General and Administrative
General and administrative expenses consist primarily of salaries and related costs for employees in executive, finance and administration, corporate development and administrative support functions, including stock-based compensation expenses and benefits. Other significant general and administrative expenses include accounting and legal services, the cost of various consultants, occupancy costs and information systems costs.
We expect that our general and administrative expenses will increase as we continue to operate as a public company. We expect increased administrative costs resulting from our anticipated clinical trials and the potential commercialization of our drug candidates. We believe that these increases will likely include increased costs for director and officer liability insurance, hiring additional personnel to support future market research and future product commercialization efforts and increased fees for outside consultants, attorneys and accountants. We also expect to continue to incur increased costs to comply with corporate governance, internal controls, investor relations and disclosures and similar requirements applicable to a public company.
118
Financial Operations Overview and Analysis for the Years Ended December 31, 2020 and 2019
| Year Ended | ||||||||
| December 31, | ||||||||
| 2020 | 2019 | |||||||
| Revenue | - | - | ||||||
| Expenses | ||||||||
| General and administrative | $ | 3,664,965 | $ | 1,475,000 | ||||
| Research and development | 2,243,225 | 953,185 | ||||||
Total operating expenses | 5,908,190 | 2,428,185 | ||||||
| Net loss | $ | (5,908,190 | ) | $ | (2,428,185 | ) | ||
Revenues
To date, except for a research grant in 2017, we have not generated any revenue since our inception.
General and Administrative Expenses
General and administrative expenses increased $2,189,965 or 149%, from $1,475,000 for the year ended December 31, 2019 to $3,664,965 for the year ended December 31, 2020. The increase was primarily attributable to an increase in corporate insurance expense of approximately $1,077,000, an increase in general and administrative related stock option compensation expense of approximately $604,000, an increase in general and administrative labor expense of $512,000, an increase in business development expense of $128,000, increases in NASDAQ and othering filing fees of $73,000, and an increase in other professional services of $70,000. These increases were partially offset by a decrease in travel and relocation expense of approximately $147,000 and a decrease in legal and patent fees of approximately $146,000.
Research and Development Expenses
Research and development expenses increased $1,290,040, or 135%, from $953,185 for the year ended December 31, 2019 to $2,243,225 for the year ended December 31, 2020. The increase was primarily attributable to an increase in research and development labor expense of approximately $489,000, an increase in research and development related stock option compensation expense of approximately $470,000, an increase in research study expenses of approximately $194,000, an increase in product candidate manufacturing expense of approximately $70,000, and an increase in non-manufacturing consulting expense of approximately $43,000.
On September 3, 2018, Lantern Pharma Limited, our wholly owned subsidiary, was awarded a grant by the UK government in the form of state aid under the Commission Regulations (EU) No. 651/2014 of 17 June 2014 (the “General Block Exemption”), Article 25 Aid for research and development projects, state aid notification no. SA.40154. The grant was awarded to conduct research and development activities for the prostate cancer biomarker analysis of our LP-184 drug candidate. Following our research and development activities in Northern Ireland, the grant will reimburse 50% of our research and development expenses not exceeding GBP 24,215 of vouched and approved expenditures within specific categories and will remain in force for a period of five years. No revenue has been recognized from this grant through December 31, 2020.
119
Liquidity and Capital Resources
Since our inception, our operations have been financed primarily through the sale of equity securities, and, to a lesser extent, a grant received by us from Massachusetts Life Sciences Center in 2017. We have not yet generated any revenues from operations, other than revenues from a research grant in 2017, and we have not yet achieved profitability. We expect that general and administrative expenses and our research and development expenses will continue to increase and, as a result, we will need to generate significant product revenues to achieve profitability.
We incurred net losses of $5,908,190 and $2,428,185 for the years ended December 31, 2020 and 2019, respectively. As of December 31, 2020 and 2019, we had working capital of approximately $19,685,000 and $744,000, respectively.
On May 1, 2020 (the “Origination Date”), we received $108,500 in aggregate loan proceeds (the “PPP Loan”) from JPMorgan Chase Bank (the “Lender”) pursuant to the Paycheck Protection Program under the Coronavirus Aid, Relief, and Economic Security (CARES) Act. As of December 31, 2020, we expect to meet the requirements of loan forgiveness under the stipulations of the program. We plan to file for forgiveness under this loan within the first half of 2021. In the event we do not meet the requirements of loan forgiveness, the PPP Loan bears interest at a fixed rate of 1.0% per annum. Payments of principal and interest were deferred for the first six months following the Origination Date, with the PPP Loan to mature two years after the Origination Date. The guidance under the Paycheck Protection Program was later updated so that deferral of payments of principal and interest were extended to ten months after completion of the covered period of 24 weeks and maturity was extended past two years. We continue to monitor further development and guidance related to the Paycheck Protection Program terms.
On June 15, 2020, we completed an initial public offering of 1,750,000 shares of our common stock at $15.00 per share, for gross proceeds of $26,250,000, before deducting underwriting discounts, commissions and offering expenses, which substantially contributed to our liquidity.
As of the years ended December 31, 2020 and 2019, we had cash and cash equivalents of approximately $19,229,000 and $1,232,000, respectively. In January of 2021, we completed an additional offering with gross proceeds of approximately $69,000,000. We believe that proceeds from this offering, based on the sale of 4,928,571 shares of common stock at the public offering price of $14.00 per share, together with our existing cash and cash equivalents as of December 31, 2020, and our anticipated expenditures and capital commitments for the calendar year 2021 and the first half of 2022, will enable us to fund our operating expenses and capital expenditure requirements for at least 12 months from the date of this report.
120
Cash Flows
The following table summarizes our cash flow for the periods indicated:
| Year
Ended December 31, | ||||||||
| 2020 | 2019 | |||||||
| Net cash flows used in operating activities | $ | (5,651,621 | ) | $ | (2,127,923 | ) | ||
| Net cash flows (used in) provided by investing activities | (16,137 | ) | (5,717 | ) | ||||
| Net cash flows provided by financing activities | 23,664,960 | 2,920,507 | ||||||
| Net increase in cash and cash equivalents | $ | 17,997,202 | $ | 786,867 | ||||
Operating Activities
For the year ended December 31, 2020, net cash used in operating activities was $5,651,621 compared to $2,127,923 for the year ended December 31, 2019. The increase in net cash used in operating activities was primarily the result of the increase in the net loss together with increases in prepaid expenses.
Investing Activities
For the year ended December 31, 2020, net cash used in investing activities was $16,137, compared to $5,717 used in investing activities during the year ended December 31, 2019.
Financing Activities
Net cash provided by financing activities was $23,664,960 during the year ended December 31, 2020, attributable primarily to net proceeds from our initial public offering. Net cash provided by financing activities during the year ended December 31, 2019 was $2,920,507, attributable to the sale of 658,571 shares of Series A preferred stock and warrants to purchase Series A preferred stock for proceeds of approximately $3,455,000, of which approximately $2,920,000 consisted of cash and $535,000 consisted of the conversion of Simple Agreement for Future Equity (“SAFE”) agreements to Series A Preferred Stock.
Operating Capital and Capital Expenditure Requirements
We expect to continue to incur significant and increasing operating losses at least for the next several years as we commence our clinical trials of LP-184 and LP-300, pursue development of our other drug candidates, and seek potential future marketing approval for our drug candidates which could be several years in the future, if at all. We do not expect to generate revenue, other than possible license revenue, unless and until we successfully complete development and obtain regulatory approval for our therapeutic candidates. Our net losses may fluctuate significantly from quarter-to-quarter and year-to-year, depending on the timing of our planned clinical trials and our expenditures on other research and development activities.
We have based our projections of operating capital requirements on assumptions that may prove to be incorrect and we may use all of our available capital resources sooner than we expect. Because of the numerous risks and uncertainties associated with research, development and commercialization of pharmaceutical products, we are unable to estimate the exact amount of our operating capital requirements. We anticipate that our expenses will increase substantially as we:
| ● | continue the development of our drug candidates; |
| ● | initiate preclinical studies and clinical trials for any additional indications for our current drug candidates and any future drug candidates that we may pursue; |
121
| ● | continue to build our portfolio of drug candidates through the acquisition or in-license of additional drug candidates or technologies; |
| ● | continue to develop, maintain, expand and protect our intellectual property portfolio; |
| ● | pursue regulatory approvals for those of our current and future drug candidates that successfully complete clinical trials; |
| ● | ultimately establish a sales, marketing, distribution and other commercial infrastructure to commercialize any drug candidate for which we may obtain marketing approval; |
| ● | hire additional clinical, regulatory, scientific and accounting personnel; |
| ● | incur additional legal, accounting and other expenses in operating as a public company; and |
| ● | continue to develop, maintain, and expand our RADR® platform. |
We expect that we will need to obtain substantial additional funding in order to complete our clinical trials. To the extent that we raise additional capital through the sale of common stock, convertible securities or other equity securities, the ownership interests of our existing stockholders may be materially diluted and the terms of these securities could include liquidation or other preferences that could adversely affect the rights of our existing stockholders. In addition, debt financing, if available, would result in increased fixed payment obligations and may involve agreements that include restrictive covenants that limit our ability to take specific actions, such as incurring additional debt, making capital expenditures or declaring dividends, that could adversely impact our ability to conduct our business. If we are unable to raise capital when needed or on attractive terms, we could be forced to significantly delay, scale back or discontinue the development or commercialization of LP-184 and LP-300 and/or other drug candidates, seek collaborators at an earlier stage than otherwise would be desirable or on terms that are less favorable than might otherwise be available, and relinquish or license, potentially on unfavorable terms, our rights to LP-184 and LP-300 or other drug candidates that we otherwise would seek to develop or commercialize ourselves.
Off-Balance Sheet Arrangements
We did not have during the periods presented, and we do not currently have, any off-balance sheet arrangements as defined under SEC rules.
Critical Accounting Policies
We prepare our consolidated financial statements in accordance with generally accepted accounting standards in the United States of America. Our significant accounting policies are described in Note 3 to our consolidated financial statements included as part of this report. We believe the following critical accounting policies involve the most significant judgments and estimates used in the preparation of the consolidated financial statements.
Use of Estimates
The preparation of financial statements in conformity with accounting principles generally accepted in the United States of America requires management to make estimates and assumptions that affect the reported amounts of assets and liabilities and disclosures of contingent liabilities at the dates of the financial statements and the reported amounts of revenues and expenses during the reporting periods. Significant areas of estimation include determining the deferred tax asset valuation allowance and the inputs in determining the fair value of equity-based awards and warrants issued. Actual results could differ from these estimates.
122
Research and Development
Research and development expenses are expensed as incurred. Costs to acquire technologies, including licenses, that are utilized in research and development and that have no alternative future use are expensed when incurred.
Stock-based Compensation
We have granted stock options to our employees under our equity incentive plan. Stock-based compensation expense from awards granted under our plan is allocated over the required service period over which those stock option awards vest.
The stock option awards are valued at fair value on the date of grant and that fair value is recognized over the requisite service period. The estimated fair value of these stock option awards was determined using the Black Scholes option pricing model on the date of grant. Some of these grants occurred at a time when we were not a public company. Significant judgment and estimates were used to estimate the fair value of these awards, as they occurred when our stock was not publicly traded.
Our estimation of fair value of the awards considered our recent transactions, relevant industry and comparable public company data. Since, at the time of many of the grants, we were a non-public entity, the majority of the inputs used to estimate the fair value of the common stock option awards are considered level 3 due to their unobservable nature. Each option award is subject to specified vesting schedules and requirements. Compensation expense is charged to us over the required service period to earn the award which is expected to be up to four years, subject to the achievement of time and event-based vesting requirements. For the years ended December 31, 2020 and 2019, we have incurred share-based compensation expense related to equity awards totaling approximately $1,192,000 and $118,000, respectively.
Accounting Pronouncements
New Accounting Pronouncements Not Yet Adopted
Current Expected Credit Loss
In June 2016 the FASB issued Accounting Standard Update (ASU) 2016-13, Measurement of Credit Losses on Financial Instruments (Topic 326). This introduces new methodology for recognition of credit losses - the current expected credit loss (“CECL”) method. The CECL method requires the recognition of all losses expected over the life of a financial instrument upon origination or purchase of the instrument, unless the company elects to recognize such instruments at fair value with changes in profit and loss. CECL is effective for the Company on January 1, 2023. The Company does not anticipate a material impact from the adoption of this new standard on its financial statements.
Income Taxes
In December 2019, the FASB issued ASU 2019-12: Income Taxes (Topic 740) – Simplifying the Accounting for Income Taxes. This ASU simplifies accounting for income taxes by removing the exception to the incremental approach for intraperiod tax allocation when there is a loss from continuing operations and income or gain for other items, the exception to the requirement to recognize a deferred tax liability for equity method investments when a foreign subsidiary becomes an equity method investment, exception to the ability not to recognize a deferred tax liability for a foreign subsidiary when a foreign equity method investment becomes a subsidiary, and the exception to the general methodology for calculating income taxes in an interim period when a year-to-date loss exceeds the anticipated loss for the year. This ASU also includes other requirements related to franchise tax, goodwill as part of a business combination, consolidations, changes in tax laws, and affordable housing projects. ASU 2019-12 is effective for fiscal years beginning after December 15, 2020, including interim periods within that fiscal year. Early adoption is permitted for periods in which financial statements have not yet been issued. We do not anticipate a material impact from the adoption of this new standard on our financial statements.
123
Recently Adopted Accounting Standards
Leases
In February 2016 the FASB issued ASU 2016-02: Leases. The ASU introduces a lessee model that results in most leases impacting the balance sheet. The ASU addresses other concerns related to the current lease model. Under ASU 2016-02, lessees will be required to recognize for all leases with terms longer than 12 months, at the commencement date of the lease, a lease liability, which is a lessee’s obligation to make lease payments arising from a lease measured on a discounted basis, and a right-to-use (ROU) asset, which is an asset that represents the lessee’s right to use or control the use of a specified asset for the lease term. Leases will be classified as either finance or operating, with classification affecting the pattern of expense recognition.
In July 2018, the FASB issued ASU 2018-10 “Codification Improvements to Topic 842, Leases.” This ASU affects narrow aspects of the guidance issued in the amendments in ASU 2016-02 including those regarding residual value guarantees, rate implicit in the lease, lessee reassessment of lease classification, lessor reassessment of lease term and purchase option, variable lease payments that depend on an index or a rate, investment tax credits, lease term and purchase option, transition guidance for amounts previously recognized in business combinations, certain transition adjustments, transition guidance for leases previously classified as capital leases under Topic 840, transition guidance for modifications to leases previously classified as direct financing or sales-type leases under Topic 840, transition guidance for sale and leaseback transactions, impairment of net investment in the lease, unguaranteed residual asset, effect of initial direct costs on rate implicit in the lease, and failed sale and leaseback transactions.
We adopted ASC 2018-10 Topic 842 effective January 1, 2019 and elected the short-term lease recognition exemption for all leases that qualify. For those leases that qualify, the Company will not recognize ROU assets or lease liabilities, and this includes not recognizing ROU assets or lease liabilities for existing short-term leases of those assets in transition. This practical expedient was elected to not separate lease and non-lease components for its office space leases. The adoption of this new standard did not have a material impact on the Company’s financial statements as the Company did not have any leases that have terms of longer than 12 months.
Compensation – Stock Compensation
In June 2018, the FASB issued ASU 2018-07: Compensation – Stock Compensation (Topic 718): Improvements to Nonemployee Share- Based Payment Accounting. This ASU expands the scope of Topic 718 to include share-based payment transactions for acquiring goods and services from non-employees, and as a result, the accounting for share-based payments to non-employees will be substantially aligned. ASU 2018-07 is effective for fiscal years beginning after December 15, 2018, including interim periods within that fiscal year, early adoption is permitted but no earlier than an entity’s adoption date of Topic 606. We do not believe there has been a material impact from the adoption of this new accounting guidance on our consolidated financial statements and related footnote disclosures.
Quantitative and Qualitative Disclosure About Market Risk
Our primary exposure to market risk is interest expense sensitivity, which is affected by changes in the general level of U.S. interest rates. Historically, we have raised capital through the issuance of equity securities. As of December 31, 2020 and 2019, we had no long-term debt outstanding, other than our PPP Loan Agreement entered into in May 2020.
We do not believe that our cash has significant risk of default or illiquidity. While we believe our cash does not contain excessive risk, we cannot provide absolute assurance that in the future our investments will not be subject to adverse changes in market value. In addition, we maintain significant amounts of cash at one or more financial institutions that are in excess of federally insured limits.
124
We do not participate in any foreign currency hedging activities and we do not have any other derivative financial instruments.
Inflation generally affects us by increasing our cost of labor and clinical trial costs. We do not believe that inflation has had a material effect on our results of operations during the periods presented.
JOBS Act
On April 5, 2012, the Jumpstart Our Business Startups Act of 2012, or the JOBS Act, was enacted. Section 107 of the JOBS Act provides that an “emerging growth company” can take advantage of the extended transition period provided in Section 7(a)(2)(B) of the Securities Act of 1933, as amended, or the Securities Act, for complying with new or revised accounting standards. In other words, an “emerging growth company” can delay the adoption of certain accounting standards until those standards would otherwise apply to private companies.
We have chosen to opt out of the extended transition periods available to emerging growth companies under the JOBS Act for complying with new or revised accounting standards. Section 107 of the JOBS Act provides that our decision to opt out of the extended transition periods for complying with new or revised accounting standards is irrevocable.
Subject to certain conditions set forth in the JOBS Act, as an “emerging growth company,” we have elected to rely on the other exemptions available under the JOBS Act, including without limitation, (i) providing an auditor’s attestation report on our system of internal controls over financial reporting pursuant to Section 404(b) of the Sarbanes-Oxley Act and (ii) complying with any requirement that may be adopted by the PCAOB regarding mandatory audit firm rotation or a supplement to the auditor’s report providing additional information about the audit and the financial statements, known as the auditor discussion and analysis. We will remain an “emerging growth company” until the earliest of (i) the last day of the fiscal year in which we have total annual gross revenues of $1.07 billion or more; (ii) the last day of our fiscal year following the fifth anniversary of the date of the completion of our initial public offering, or December 31, 2025; (iii) the date on which we have issued more than $1 billion in nonconvertible debt during the previous three years; or (iv) the date on which we are deemed to be a large accelerated filer under the rules of the SEC.
Item 7A. Quantitative and Qualitative Disclosures About Market Risk.
As a Smaller Reporting Company we are exempt from the requirements of Item 7A.
125
Item 8. Financial Statements and Supplementary Data.
LANTERN PHARMA INC.
INDEX TO FINANCIAL STATEMENTS
F-1
REPORT OF INDEPENDENT REGISTERED PUBLIC ACCOUNTING FIRM
To the Board of Directors and Stockholders of
Lantern Pharma Inc. and Subsidiary
Opinion on the Financial Statements
We have audited the accompanying consolidated balance sheets of Lantern Pharma Inc. and Subsidiary (the “Company”) as of December 31, 2020 and 2019, and the related consolidated statements of operations, stockholders’ equity, and cash flows for each of the years then ended, and the related notes (collectively referred to as the “financial statements”). In our opinion, the financial statements present fairly, in all material respects, the consolidated financial position of the Company as of December 31, 2020 and 2019 and the consolidated results of its operations and its cash flows for each of the years then ended, in conformity with accounting principles generally accepted in the United States of America.
Basis for Opinion
These financial statements are the responsibility of the Company’s management. Our responsibility is to express an opinion on the Company’s financial statements based on our audits. We are a public accounting firm registered with the Public Company Accounting Oversight Board (United States) (“PCAOB”) and are required to be independent with respect to the Company in accordance with the U.S. federal securities laws and the applicable rules and regulations of the Securities and Exchange Commission and the PCAOB.
We conducted our audits in accordance with the standards of the PCAOB. Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the financial statements are free of material misstatement, whether due to error or fraud. The Company is not required to have, nor were we engaged to perform, an audit of its internal control over financial reporting. As part of our audits we are required to obtain an understanding of internal control over financial reporting but not for the purpose of expressing an opinion on the effectiveness of the Company’s internal control over financial reporting. Accordingly, we express no such opinion.
Our audits included performing procedures to assess the risks of material misstatement of the financial statements, whether due to error or fraud, and performing procedures that respond to those risks. Such procedures included examining, on a test basis, evidence regarding the amounts and disclosures in the financial statements. Our audits also included evaluating the accounting principles used and significant estimates made by management, as well as evaluating the overall presentation of the financial statements. We believe that our audits provide a reasonable basis for our opinion.
/s/ EisnerAmper LLP
We have served as the Company’s auditor since 2019.
EISNERAMPER LLP
Iselin, New Jersey
March 10, 2021
F-2
Lantern Pharma Inc. and Subsidiary
Consolidated Balance Sheets
| December 31, | ||||||||
| 2020 | 2019 | |||||||
| CURRENT ASSETS | ||||||||
| Cash | $ | 19,229,232 | $ | 1,232,030 | ||||
| Prepaid expenses & other current assets | 1,007,690 | 788 | ||||||
| Total current assets | 20,236,922 | 1,232,818 | ||||||
| Property and equipment, net | 21,507 | 8,758 | ||||||
| Deferred offering costs | 101,205 | 191,000 | ||||||
| TOTAL ASSETS | $ | 20,359,634 | $ | 1,432,576 | ||||
| CURRENT LIABILITIES | ||||||||
| Accounts payable and accrued expenses | $ | 552,339 | $ | 489,292 | ||||
| Total Current Liabilities | 552,339 | 489,292 | ||||||
| PPP loan payable | 108,500 | - | ||||||
| TOTAL LIABILITIES | 660,839 | 489,292 | ||||||
| COMMITMENTS AND CONTINGENCIES (NOTE 5) | ||||||||
| STOCKHOLDERS’ EQUITY | ||||||||
| Series A Preferred Stock (1,000,000 authorized at December 31, 2020; 3,480,000 authorized at December 31, 2019; $.0001 par value) (Zero shares issued and outstanding at December 31, 2020; 2,438,866 shares issued and outstanding at December 31, 2019) | - | 244 | ||||||
| Common Stock (25,000,000 authorized at December 31, 2020; 12,180,000 authorized at December 31, 2019; $.0001 par value) (6,220,927 shares issued and outstanding at December 31, 2020; 1,978,269 shares issued and outstanding at December 31, 2019) | 622 | 198 | ||||||
| Additional paid-in capital | 32,358,068 | 7,694,547 | ||||||
| Accumulated deficit | (12,659,895 | ) | (6,751,705 | ) | ||||
| Total stockholders’ equity | 19,698,795 | 943,284 | ||||||
| TOTAL LIABILITIES AND STOCKHOLDERS’ EQUITY | $ | 20,359,634 | $ | 1,432,576 | ||||
See accompanying Notes to Consolidated Financial Statements
F-3
Lantern Pharma Inc. and Subsidiary
Consolidated Statements of Operations
| For the Year
Ended December 31, | ||||||||
| 2020 | 2019 | |||||||
| Operating expenses: | ||||||||
| General and administrative | $ | 3,664,965 | $ | 1,475,000 | ||||
| Research and development | 2,243,225 | 953,185 | ||||||
| Total operating expenses | 5,908,190 | 2,428,185 | ||||||
| NET LOSS | $ | (5,908,190 | ) | $ | (2,428,185 | ) | ||
| Net loss per share of common shares, basic and diluted | (1.37 | ) | (1.23 | ) | ||||
| Weighted-average number of common shares outstanding, basic and diluted | 4,304,918 | 1,978,269 | ||||||
See accompanying Notes to Consolidated Financial Statements
F-4
Lantern Pharma Inc. and Subsidiary
Consolidated Statements of Stockholders’ Equity (Deficit)
| Preferred
Stock Number of Shares | Preferred
Stock Amount | Common
Stock Number of Shares | Common
Stock Amount | Additional
Paid-in Capital | Accumulated
Deficit | Total
Stockholders’ Equity (Deficit) | ||||||||||||||||||||||
| Balance, January 1, 2019 | 1,292,952 | $ | 129 | 1,978,269 | $ | 198 | $ | 4,121,395 | $ | (4,323,520 | ) | $ | (201,798 | ) | ||||||||||||||
| Preferred stock and warrants issued | 1,145,914 | 115 | - | - | 3,455,392 | - | 3,455,507 | |||||||||||||||||||||
| Stock-based compensation | - | - | - | - | 117,760 | - | 117,760 | |||||||||||||||||||||
| Net Loss | - | - | - | - | - | (2,428,185 | ) | (2,428,185 | ) | |||||||||||||||||||
| Balance, December 31, 2019 | 2,438,866 | 244 | 1,978,269 | 198 | 7,694,547 | (6,751,705 | ) | 943,284 | ||||||||||||||||||||
| Common stock issued from offering, net of issuance costs | - | - | 1,750,000 | 175 | 23,419,546 | - | 23,419,721 | |||||||||||||||||||||
| Preferred Stock Converted to Common, net of fractional shares adjustment | (2,438,866 | ) | (244 | ) | 2,438,848 | 244 | (261 | ) | - | (261 | ) | |||||||||||||||||
| Common stock issued from option exercise | - | - | 50,460 | 5 | 51,995 | - | 52,000 | |||||||||||||||||||||
| Cashless exercise of warrant | - | - | 3,350 | - | - | - | - | |||||||||||||||||||||
| Stock-based compensation | - | - | - | - | 1,192,241 | - | 1,192,241 | |||||||||||||||||||||
| Net Loss | - | - | - | - | - | (5,908,190 | ) | (5,908,190 | ) | |||||||||||||||||||
| Balance, December 31, 2020 | - | $ | - | 6,220,927 | $ | 622 | $ | 32,358,068 | $ | (12,659,895 | ) | $ | 19,698,795 | |||||||||||||||
See accompanying Notes to Consolidated Financial Statements
F-5
Lantern Pharma Inc. and Subsidiary
Consolidated Statements of Cash Flows
| 2020 | 2019 | |||||||
| CASH FLOWS FROM OPERATING ACTIVITIES | ||||||||
| Net loss | $ | (5,908,190 | ) | $ | (2,428,185 | ) | ||
| Adjustments to reconcile net loss to cash used in operating activities: | ||||||||
| Depreciation and amortization | 3,388 | 1,627 | ||||||
| Stock based compensation | 1,192,241 | 117,760 | ||||||
| Changes in assets and liabilities: | ||||||||
| Accounts receivable | - | - | ||||||
| Prepaid expenses & other current assets | (1,006,902 | ) | (788 | ) | ||||
| Deferred offering costs | (49,325 | ) | (191,000 | ) | ||||
| Accounts payable and accrued expenses | 117,167 | 372,663 | ||||||
| Net cash flows used in operating activities | (5,651,621 | ) | (2,127,923 | ) | ||||
| INVESTING ACTIVITIES | ||||||||
| (Purchase) sale of property and equipment | (16,137 | ) | (5,717 | ) | ||||
| Net cash flows (used in) provided by investing activities | (16,137 | ) | (5,717 | ) | ||||
| FINANCING ACTIVITIES | ||||||||
| Proceeds from issuance of common and preferred stock | 26,250,000 | 2,920,507 | ||||||
| Issuance costs | (2,745,279 | ) | - | |||||
| Proceeds from stock option exercise | 52,000 | - | ||||||
| Preferred stock converted to common stock net of fractional shares adjustment | (261 | ) | - | |||||
| Borrowings on notes payable | 169,049 | - | ||||||
| Payments on notes payable | (169,049 | ) | - | |||||
| Borrowings on PPP loan payable | 108,500 | - | ||||||
| Net cash flows provided by financing activities | 23,664,960 | 2,920,507 | ||||||
| CHANGE IN CASH FOR THE YEAR | 17,997,202 | 786,867 | ||||||
| CASH, BEGINNING OF YEAR | 1,232,030 | 445,163 | ||||||
| CASH, END OF YEAR | $ | 19,229,232 | $ | 1,232,030 | ||||
| Non-cash financing activities | ||||||||
| Conversion of SAFE agreements to Series A preferred stock | $ | - | $ | 535,000 | ||||
| Deferred offering costs applied to net offering proceeds | $ | (85,000 | ) | $ | - | |||
| Deferred offering costs recorded in AP and accrued expenses | $ | 51,880 | ||||||
See accompanying Notes to Consolidated Financial Statements
F-6
Note 1. Organization, Principal Activities, and Basis of Presentation
Lantern Pharma Inc., and Subsidiary (the “Company”) is a clinical stage biopharmaceutical company, focused on leveraging artificial intelligence (“A.I.”), machine learning and genomic data to streamline the drug development process and to identify the patients that will benefit from its targeted oncology therapies. The Company’s portfolio of therapies consists of small molecule drug candidates that others have tried, but failed, to develop into an approved commercialized drug, as well as new compounds that it is developing with the assistance of its A.I. platform and its biomarker driven approach. The Company’s A.I. platform, known as RADR®, uses big data analytics (combining molecular data, drug efficacy data, data from historical studies, data from scientific literature, phenotypic data from trials and publications, and mechanistic pathway data) and machine learning. The Company’s data-driven, genomically-targeted and biomarker-driven approach allows it to pursue a transformational drug development strategy that identifies, rescues or develops, and advances potential small molecule drug candidates.
Lantern Pharma Inc. was incorporated under the laws of the state of Texas on November 7, 2013, and thereafter reincorporated in the state of Delaware on January 15, 2020. The Company’s principal operations are located in Texas. The Company formed a wholly owned subsidiary, Lantern Pharma Limited, in the United Kingdom in July 2017.
Since inception, the Company has devoted substantially all its activity to advancing research and development, including efforts in connection with preclinical studies, clinical trials and development of its RADR platform. This includes research and development for three drug candidates in development in targeted areas identified with the assistance of the RADR platform:
| ● | LP-100 (irofulven), out-licensed to Allarity Therapeutics (formerly known as Oncology Venture), in a phase II trial for the treatment of prostate cancer; |
| ● | LP-300 (Tavocept) in planning stages for phase II trial for the treatment of non-small cell lung cancer; and |
| ● | LP-184 in preclinical studies for treatment of solid tumors including prostate, liver and pancreatic cancers and glioblastoma. |
In connection with the Company’s reincorporation in the state of Delaware on January 15, 2020, the par value of the Company’s Common Stock and Series A Preferred Stock was changed from $0.01 per share to $0.0001 per share. The change in the par value has been retroactively reflected in the accompanying consolidated financial statements. Additional funds have been reclassified from Common Stock and Series A Preferred Stock to additional paid-in capital to reflect the change in par value associated with the reincorporation.
The accompanying consolidated financial statements have been prepared in accordance with accounting principles generally accepted in the United States of America (“GAAP”) and include all adjustments necessary for the fair presentation of the Company’s financial position, results of operations, and cash flows for each period presented. The preparation of financial statements in conformity with GAAP requires management to make estimates and assumptions that affect the reported amounts of assets and liabilities and disclosure of contingent assets and liabilities at the date of the consolidated financial statements and the reported amounts of expenses during the reporting periods. Actual results could differ from these estimates.
Any reference in these notes to applicable guidance refers to Accounting Standards Codification (“ASC”) and Accounting Standards Update (“ASU”) of the Financial Accounting Standards Board (“FASB”). To date, the Company has operated its business as one segment. The Company’s consolidated financial statements include the accounts of the Company and its wholly owned subsidiary, Lantern Pharma Limited. All intercompany balances and transactions have been eliminated in consolidation.
F-7
Effective June 11, 2020, in connection with the Company’s initial public offering (“IPO”), the Company completed a forward stock split of its common stock at a ratio of 1.74 for 1 shares. In addition, all of the Company’s preferred stock converted into common stock effective June 15, 2020 in connection with the IPO. All data on common stock and equivalents in the accompanying consolidated financial statements and in these notes are shown herein reflective of this stock split and the conversion of the preferred stock. In addition, the number of shares of preferred stock in the accompanying consolidated financial statements and in these notes is presented to reflect the number of shares into which the preferred stock would convert as a result of the forward stock split.
Note 2. Liquidity
The Company incurred a net loss of approximately $5,908,000 and $2,428,000 during the years ended December 31, 2020 and 2019, respectively. As of December 31, 2020, the Company had working capital of approximately $19,685,000, primarily as a result of the net proceeds raised in the IPO of approximately $23,420,000 (see Note 6). As of December 31, 2019, the Company had working capital of approximately $744,000.
On January 20, 2021, the Company closed a public offering of 4,928,571 shares of its common stock at a public offering price of $14.00 per share, which amount included 642,856 shares sold upon full exercise of the underwriter’s over-allotment option. Total gross proceeds from the offering were $68,999,994, and net proceeds from the offering were approximately $64,200,000.
The Company has received funding in the form of periodic capital raises and also plans to apply for grant funding in the future to assist in supporting its capital needs. We may also explore the possibility of entering into commercial credit facilities as an additional source of liquidity.
We believe that our existing cash and cash equivalents as of December 31, 2020, and our anticipated expenditures and capital commitments for the calendar year 2021 and the first half of 2022, will enable us to fund our operating expenses and capital expenditure requirements for at least 12 months from the date of filing this Form 10-K for the year ended December 31, 2020.
Note 3. Summary of Significant Accounting Policies
Use of Estimates and Assumptions
The preparation of financial statements in conformity with GAAP requires management to make estimates and assumptions that affect the reported amounts of assets and liabilities and disclosure of contingent assets and liabilities at the date of the financial statements and the reported amounts of revenues and expenses during the reporting period. The significant areas of estimation include determining deferred tax asset valuation allowance and the inputs in determining the fair value of equity-based awards and warrants issued. Actual results could differ from those estimates.
Risks and Uncertainties
The Company operates in an industry that is subject to intense competition, government regulation and rapid technological change. Operations are subject to significant risk and uncertainties including financial, operational, technological, regulatory, and other risks, including the potential risk of business failure.
The extent of the impact and effects of the coronavirus (COVID-19) on the operation and financial performance of the Company’s business will depend on future developments, including the duration and spread of the outbreak, related travel advisories and restrictions, the recovery time of disrupted research services, the consequential staff shortages, and research and development delays, or the uncertainty with respect to the accessibility of additional liquidity or capital markets, all of which are highly uncertain and cannot be predicted. If the Company’s operations are impacted by this outbreak for an extended period, the Company’s results of operations or liquidity may be materially adversely affected.
Deferred Offering Costs
Costs incurred related to equity offerings are capitalized as deferred equity issuance costs in other non-current assets until the offering is completed or abandoned. If the Company completes an offering, these costs will be offset against proceeds received; or if the offering does not occur, they will be expensed. Offering costs include direct and incremental costs related to the offering such as legal fees and related costs.
F-8
The Company recorded deferred offering costs of $101,205 and $191,000 as of December 31, 2020 and 2019, respectively. During the year ended December 31, 2020, the Company has applied deferred offering costs of $456,437 as a reduction to additional paid-in capital upon completion of the Company’s initial public offering (“IPO”) on June 15, 2020.
Research and Development
Research and development costs are expensed as incurred. These expenses primarily consist of payroll, contractor expenses, research study expenses, costs for manufacturing and supplies, and technical infrastructure on the cloud for the purposes of developing the Company’s RADR platform and identifying, developing, and testing drug candidates. Development costs incurred by third parties are expensed as the work is performed. Costs to acquire technologies, including licenses, that are utilized in research and development and that have no alternative future use are expensed when incurred.
Cash and Cash Equivalents
Highly liquid investments with original maturities of three months or less when purchased are considered to be cash equivalents. Financial instruments which potentially subject the Company to concentrations of credit risk consist primarily of cash and cash equivalents. The Company maintains cash and cash equivalents with high-credit quality financial institutions. At times, such amounts may exceed insured limits. The Company has not experienced any losses in such accounts.
Prepaid Expenses and Other Current Assets
Prepaid expenses and other current assets as of December 31, 2020 totaled approximately $1,008,000 and included approximately $187,000 of upfront payments for contractor and academic research studies and services, approximately $15,000 of licensing and other fees, and approximately $806,000 of prepaid annual insurance fees.
Loan Pursuant to Paycheck Protection Program
On May 1, 2020, the Company received $108,500 in aggregate loan proceeds (the “PPP Loan”) from JPMorgan Chase Bank (the “Lender”) pursuant to the Paycheck Protection Program under the Coronavirus Aid, Relief, and Economic Security (CARES) Act. The PPP Loan is evidenced by a loan application and payment agreement (the “PPP Loan Agreement”) by and between the Company and the Lender. This amount is recorded as a loan payable on the Company’s consolidated balance sheet at December 31, 2020.
Income Taxes
Deferred tax assets and liabilities are determined based on the differences between the financial reporting and tax basis of assets and liabilities using enacted tax rates which will be in effect when the differences reverse. The Company provides a full valuation allowance against net deferred tax assets unless, based upon the available evidence, it is more likely than not that the deferred tax asset will be realized.
Stock-based Compensation
Stock-based awards have been accounted for as required by ASC 718 “Compensation - Stock Compensation.” Under ASC 718, awards are valued at fair value on the date of grant, and that fair value is recognized over the requisite service period.
F-9
Reclassification
Certain prior period information has been reclassified to conform to the current period presentation.
Note 4. New Accounting Pronouncements
New Accounting Pronouncements, Not Yet Adopted
Current Expected Credit Loss
In June 2016 the FASB issued Accounting Standard Update (ASU) 2016-13, Measurement of Credit Losses on Financial Instruments (Topic 326). This introduces new methodology for recognition of credit losses - the current expected credit loss (“CECL”) method. The CECL method requires the recognition of all losses expected over the life of a financial instrument upon origination or purchase of the instrument, unless the company elects to recognize such instruments at fair value with changes in profit and loss. CECL is effective for the Company on January 1, 2023. The Company does not anticipate a material impact from the adoption of this new standard on its financial statements.
Income Taxes
In December 2019, the FASB issued ASU 2019-12: Income Taxes (Topic 740) – Simplifying the Accounting for Income Taxes. This ASU simplifies accounting for income taxes by removing the exception to the incremental approach for intraperiod tax allocation when there is a loss from continuing operations and income or gain for other items, the exception to the requirement to recognize a deferred tax liability for equity method investments when a foreign subsidiary becomes an equity method investment, the exception to the ability not to recognize a deferred tax liability for a foreign subsidiary when a foreign equity method investment becomes a subsidiary, and the exception to the general methodology for calculating income taxes in an interim period when a year-to-date loss exceeds the anticipated loss for the year. This ASU also includes other requirements related to franchise tax, goodwill as part of a business combination, consolidations, changes in tax laws, and affordable housing projects. ASU 2019-12 is effective for fiscal years beginning after December 15, 2020, including interim periods within that fiscal year. Early adoption is permitted for periods in which financial statements have not yet been issued. The Company does not anticipate a material impact from the adoption of this new standard on its financial statements.
Recently Adopted Accounting Standards
Leases
In February 2016 the FASB issued ASU 2016-02: Leases. The ASU introduces a lessee model that results in most leases impacting the balance sheet. The ASU addresses other concerns related to the current lease model. Under ASU 2016-02, lessees will be required to recognize for all leases with terms longer than 12 months, at the commencement date of the lease, a lease liability, which is a lessee’s obligation to make lease payments arising from a lease measured on a discounted basis, and a right-to-use (ROU) asset, which is an asset that represents the lessee’s right to use or control the use of a specified asset for the lease term. Leases will be classified as either finance or operating, with classification affecting the pattern of expense recognition.
In July 2018, the FASB issued ASU 2018-10 “Codification Improvements to Topic 842, Leases.” This ASU affects narrow aspects of the guidance issued in the amendments in ASU 2016-02 including those regarding residual value guarantees, rate implicit in the lease, lessee reassessment of lease classification, lessor reassessment of lease term and purchase option, variable lease payments that depend on an index or a rate, investment tax credits, lease term and purchase option, transition guidance for amounts previously recognized in business combinations, certain transition adjustments, transition guidance for leases previously classified as capital leases under Topic 840, transition guidance for modifications to leases previously classified as direct financing or sales-type leases under Topic 840, transition guidance for sale and leaseback transactions, impairment of net investment in the lease, unguaranteed residual asset, effect of initial direct costs on rate implicit in the lease, and failed sale and leaseback transactions.
F-10
The Company adopted ASC 2018-10 Topic 842 effective January 1, 2019 and elected the short-term lease recognition exemption for all leases that qualify. For those leases that qualify, the Company will not recognize ROU assets or lease liabilities, and this includes not recognizing ROU assets or lease liabilities for existing short-term leases of those assets in transition. This practical expedient was elected to not separate lease and non-lease components for its office space leases. The adoption of this new standard did not have a material impact on the Company’s financial statements as the Company did not have any leases that have terms of longer than 12 months.
Compensation – Stock Compensation
In June 2018, the FASB issued ASU 2018-07: Compensation – Stock Compensation (Topic 718): Improvements to Nonemployee Share-Based Payment Accounting. This ASU expands the scope of Topic 718 to include share-based payment transactions for acquiring goods and services from non-employees, and as a result, the accounting for share-based payments to non-employees will be substantially aligned. ASU 2018-07 is effective for fiscal years beginning after December 15, 2018, including interim periods within that fiscal year. Early adoption is permitted but no earlier than an entity’s adoption date of Topic 606. The Company adopted ASU Topic 718 effective January 1, 2019. The adoption of this new accounting guidance did not have a material impact on the Company’s consolidated financial statements and related footnote disclosures.
Note 5: Commitments and Contingencies
General.
The Company has entered into, and expects to enter into from time to time in the future, license agreements, strategic alliance agreements, assignment agreements, and similar agreements related to the advancement of its product candidates and research and development efforts (collectively, “License and Strategic Alliance Agreements”). As of the date of filing this report on Form 10-K, the Company has obligations relating to License and Strategic Alliance Agreements that are expected to result in total payments of approximately $600,000 for 2021.
BioNumerik Pharmaceuticals.
In January 2018, the Company entered into an Assignment Agreement (the “Assignment Agreement”) with BioNumerik Pharmaceuticals, Inc. (“BioNumerik”), pursuant to which the Company acquired rights to domestic and international patents, trademarks and related technology and data relating to LP-300 (Tavocept) for human therapeutic treatment indications. The Assignment Agreement replaced a License Agreement that was entered into between the Company and BioNumerik in May 2016. The Company made upfront payments totaling $25,000 in connection with entry into the Assignment Agreement.
In the event the Company develops and commercializes LP-300 internally, the Company is required to pay to the BioNumerik-related payment recipients designated in the Assignment Agreement a percentage royalty in the low double digits on cumulative net revenue up to $100 million, with incremental increases in the percentage royalty for net cumulative revenue between $100 million and $250 million, $250 million and $500 million, and $500 million and $1 billion, with a percentage royalty payment that could exceed $200 million for net cumulative revenue in excess of $1 billion. The Company has the right to first recover certain designated portions of patent costs and development and regulatory costs before the payment of royalties described above.
If the Company enters into a third party transaction for LP-300, the Company is required to pay the BioNumerik-related payment recipients a specified percentage of any upfront, milestone, and royalty amounts received by the Company from the transaction, after first recovering specified direct costs incurred by the Company for the development of LP-300 that are not otherwise reimbursed from such third party transaction.
In addition, the Assignment Agreement provides that the Company will use commercially diligent efforts to develop LP-300 and make specified regulatory filings and pay specified development and regulatory costs related to LP-300. The Assignment Agreement also provides that the Company will provide TriviumVet DAC (“TriviumVet”) with (i) specified data and information generated by the Company with respect to LP-300, and (ii) an exclusive license to use specified LP-300-related patent rights, trademark rights and related intellectual property to support LP-300 development in non-human (animal) treatment indications.
F-11
The Company is also required to pay all patent costs on covered patents related to LP-300. Patent costs paid by the Company to BioNumerik with respect to LP-300 related patents amounted to $0 and approximately $74,000 for the years ended December 31, 2020 and 2019, respectively. These patent costs are included in general and administrative expenses in the accompanying consolidated statement of operations. These patent costs are fully recoverable at the time of any net revenue from LP-300, with up to 50% of net revenue amounts to be applied towards repayment of patent costs until such costs are fully recovered.
In addition to the recovery of patent costs, the Company has the right to recover the $25,000 upfront payments made in connection with entry into the Assignment Agreement, which payments are recoverable prior to making any royalty or third party transaction sharing payments. The Company also has the right to recover previously incurred LP-300 development and regulatory costs, with up to a mid-single digit percentage of net revenue amounts to be applied towards repayment of development and regulatory costs until such costs are fully recovered.
No amounts are owed to BioNumerik as of December 31, 2020. Approximately $11,000 is owed and recorded in accounts payable to BioNumerik as of December 31, 2019.
AF Chemicals.
In January 2015, the Company entered into a Technology License Agreement to exclusively license domestic and international patent rights from AF Chemicals, LLC (“AF Chemicals”) for the treatment of cancer in humans for the compounds LP-100 (Irofulven) and LP-184. In February 2016, the Company and AF Chemicals entered into an Addendum (the “Addendum”) providing for additions and amendments to the Technology License Agreement. In December 2020, the Company and AF Chemicals entered into a Second Addendum (the “Second Addendum”) providing for further additions and amendments to the Technology License Agreement. The Technology License Agreement, Addendum and Second Addendum are collectively referred to as the “AFC License Agreement”.
The Second Addendum provides for us to make specified payments to AF Chemicals within 10 days after signing and by March 31, 2021. The Second Addendum also provides that, from December 30, 2020 until January 15, 2025, we will have no obligation to pay annual licensing fees, development diligence extension payments, or patent maintenance fee payments to AFC under the AFC License Agreement. Nothing was expensed in the year ended December 31, 2020 relating to entering into the Second Addendum.
As part of the Second Addendum, we have agreed to apply for specified orphan drug designations for LP-184 in the US and EU. The Second Addendum also amends and clarifies other provisions of the Technology License Agreement, and provides us with the ability to recover a portion of initial payments made under the Second Addendum from sublicense fees or royalty payments that may be made to AFC by us or third parties prior to January 15, 2025.
Pursuant to the AFC License Agreement the Company made annual licensing fee payments to AF Chemicals in the amount of $30,000 during each of the years ended December 31, 2020 and 2019 relating to LP-184. Such amounts are included in research and development expenses in the accompanying consolidated statement of operations. In addition, the Company is obligated to make milestone payments to AF Chemicals at the time of an Investigational New Drug Application (“IND”) filing relating to LP-184 and also upon reaching additional specified milestones in connection with the development and potential marketing approval of LP-184 in the United States, specified countries in Europe, and other countries.
F-12
The AFC License Agreement also provides that the Company will pay AF Chemicals a royalty of at least a very small single digit percentage of specified net sales of LP-184 and other analogs. In addition, the AFC License Agreement contains specified time requirements for the Company to file an IND, enroll patients in clinical trials, and file a potential NDA with respect to LP-184, with the ability for the Company to pay AF Chemicals additional amounts ranging up to an amount in the low hundreds of thousands of dollars for each one, two, three and four year extension to such development time requirements, with additional extensions beyond four years to be negotiated by the Company and AF Chemicals. The Company paid $50,000 and $37,500 during the years ended December 31, 2020 and 2019, respectively in connection with the extension of the IND filing milestone for LP-184, which amounts are included under research and development in the accompanying consolidated statements of operations. Pursuant to the Second Addendum, no additional payments of annual licensing fees or development diligence extension payments are required to be made by the Company until January 15, 2025, at which time these obligations will resume. The Company will also be obligated to make annual licensing fee payments to AF Chemicals relating to LP-100 beginning January 15, 2025, as described below under Allarity Therapeutics.
In the event of a sublicense of the LP-184 rights, the Company is obligated to pay AF Chemicals (a) a low double digit percentage of the gross income and fees received by the Company with respect to the United States in connection with such sublicense, and (b) a lower double digit percentage of the gross income and fees received by the Company with respect to Europe and Japan in connection with such sublicense.
No amounts are payable to AF Chemicals as of December 31, 2020 and 2019.
Allarity Therapeutics (formerly known as Oncology Venture)
In May 2015, the Company licensed various rights to LP-100 to Oncology Venture (now known as Allarity Therapeutics) pursuant to a Drug License and Development Agreement. In February 2016, the Company and Allarity Therapeutics entered into an addendum and an amendment providing for additions and amendments to the Drug License and Development Agreement. In connection with the Drug License and Development Agreement, as amended (collectively, the “Allarity License and Development Agreement”), Allarity Therapeutics agreed to directly pay to AF Chemicals on behalf of the Company certain amounts to satisfy the Company’s milestone obligations to AF Chemicals with respect to LP-100 under the AFC License Agreement. Amounts paid by Allarity Therapeutics to AF Chemicals on behalf of the Company are then deducted from amounts owed by Allarity Therapeutics to the Company.
The amounts to be paid to AF Chemicals with respect to LP-100 under the AFC License Agreement are in many ways similar to the amounts to be paid with respect to LP-184 as described above under “AF Chemicals”. In the event any such amounts relating to LP-100 are not paid to AF Chemicals by Allarity Therapeutics, the Company is obligated to pay such unpaid amounts. In addition to the payments to be made by Allarity Therapeutics, the Company is obligated to make annual licensing fee payments to AF Chemicals relating to LP-100. The Company paid $30,000 to AF Chemicals during each of the years ended December 31, 2020 and 2019 relating to LP-100. Such amounts are included in research and development expenses in the accompanying consolidated statement of operations.
In addition, the AFC License Agreement contains specified time requirements for the Company to file an IND, enroll patients in clinical trials, and file a potential NDA with respect to LP-100. During the year ended December 31, 2020, the Company paid AF Chemicals $25,000 relating to a one-year milestone extension fee for LP-100 commencing in August 2020, approximately $10,000 of which was expensed during the year ended December 31, 2020 and included under research and development expenses in the accompanying consolidated statements of operations.
No amounts are payable under the Allarity License and Development Agreement as of December 31, 2020 and 2019.
EU Grant
In September 2018, Lantern Pharma Limited, a wholly owned subsidiary of Lantern Pharma Inc., was awarded a grant by the UK government in the form of state aid under the Commission Regulations (EU) No. 651/2014 of 17 June 2014 (the “General Block Exemption”), Article 25 Aid for research and development projects, state aid notification no. SA.40154. The grant was awarded to conduct research and development activities for the prostate cancer biomarker analysis of the LP-184 drug candidate. Following the Company’s research and development activities in Northern Ireland, the grant will reimburse the Company 50% of its research and development expenses not exceeding GBP 24,215 of vouched and approved expenditures within specific categories. The grant contains some reporting and consent requirements. The grant will remain in force for a period of five years. No payments to the Company have been made under the grant as of December 31, 2020 and December 31, 2019. No revenue has been recognized from this grant through December 31, 2020.
F-13
Patheon API Services
In July 2020, the Company entered into an agreement with Patheon API Services, Inc. (“Patheon”) for the manufacture and supply of cGMP material to support the Company’s planned Phase II clinical trial for its product candidate LP-300. In addition to producing LP-300 API (active pharmaceutical ingredient) under cGMP (current Good Manufacturing Practices) conditions, Patheon will transfer previously validated manufacturing processes and analytical methods for LP-300 and will produce non-GMP material that can be used to support non-clinical studies for LP-300. The agreement provides for payments in stages as specified process and manufacturing milestones are achieved. Patheon, a part of Thermo Fisher Scientific, has previously developed and/or manufactured more than 700 pharmaceuticals for biopharma clients and has more than 55 locations around the world, providing access to a fully integrated global network of facilities.
The Company paid approximately $203,000 to Patheon during the twelve months ended December 31, 2020 pursuant to the Patheon agreement. Approximately $227,000 was expensed with respect to the Patheon agreement during the twelve months ended December 31, 2020, which relates to the services received by the Company through December 31, 2020. This amount is included in research and development expenses in the accompanying consolidated statements of operations. Approximately $24,000 relating to the Patheon agreement is included under accounts payable and accrued expenses on the Company’s consolidated balance sheet for the period ended December 31, 2020. The Company expects to pay additional amounts to Patheon in future periods in accordance with specified process and manufacturing milestones under the Patheon agreement.
Southwest Research Institute
As part of the Company’s research and development activities, the Company has engaged Southwest Research Institute (“SwRI”) from time to time to assist with compound synthesis and manufacturing related activities for the Company’s product candidates. Approximately $71,000 and $234,000 was expensed with respect to SwRI during the twelve months ended December 31, 2020 and December 31, 2019, respectively. All of such expensed amounts are included in research and development expenses in the accompanying consolidated statements of operations. Approximately $82,000 was payable to SwRI as of December 31, 2020, and approximately $13,000 was payable to SwRI as of December 31, 2019. In September 2020, the Company entered into an agreement with SwRI for the non-GMP synthesis of LP-184 material and related analytical development to assist with preclinical studies. Approximately $97,000 relating to the SwRI agreement is included under prepaid expenses on the Company’s consolidated balance sheet for the period ended December 31, 2020. There were no prepaid expenses relating to SwRI as of December 31, 2019. The Company expects to pay additional amounts to SwRI in future periods as synthesis and analytical work is conducted by SwRI under the agreement.
The Research Institute of Fox Chase Cancer Center
In September 2020, the Company entered into a research agreement with the Research Institute of Fox Chase Cancer Center (“FCCC”) as part of the Company’s research and development activities, with a focus on advancing the targeted use of LP-184 in molecularly-defined sub-types of pancreatic cancer. Approximately $85,000 was expensed with respect to the FCCC agreement during the twelve months ended December 31, 2020, which amount is included in research and development expenses in the accompanying consolidated statements of operations. As of December 31, 2020, approximately $14,000 was recorded as accrued with respect to FCCC. The Company expects to pay additional amounts to FCCC in future periods in accordance with the payment schedule specified under the FCCC agreement.
Other Research and Service Provider Agreements
In addition to the agreements described above, the Company has entered into other research and service provider agreements for the advancement of its product candidates and research and development efforts. The Company expects to pay additional amounts in future periods in connection with existing and future research and service provider agreements.
F-14
Operating Leases
The Company leased office space in Dallas, Texas under month-to-month lease arrangements during the years ended December 31, 2020 and 2019. In connection with the Company’s employees working remotely due to COVID-19, the Company in August 2020 reduced its monthly lease commitment and costs to minimal levels. The Company is continuing to monitor the COVID-19 conditions and intends to increase its lease of office space following an improvement in the COVID-19 pandemic.
In August 2019, the Company entered into a leasing agreement for office space in New Jersey. Monthly rent was $2,106, plus electrical utilities. The lease expired on July 31, 2020 and was not renewed.
Note 6. Shareholders’ Equity
Preferred Stock
As of December 31, 2019, the Company had 3,480,000 authorized shares of preferred stock, of which 2,438,866 shares designated as Series A Preferred Stock (the “Series A Preferred Stock”) were issued and outstanding.
Upon the Company’s IPO, all shares of the Company’s Series A preferred stock were converted into 2,438,851 shares of common stock effective June 15, 2020, with fractional share adjustments made in connection with the conversion as discussed below. As of December 31, 2020, the Company had 1,000,000 authorized shares of preferred stock, with zero shares of preferred stock issued and outstanding.
The holders of Series A Preferred Stock were entitled to receive dividends when, as and if declared by the Company’s Board of Directors, payable in preference and priority to any declaration or payment of dividends on Common Stock. No dividends on any Series A Preferred Stock were declared and no dividends on Common Stock have been declared to date.
In March 2019, the Company sold 590,643 shares of Series A preferred stock for aggregate proceeds of approximately $1,850,000. The Company also issued 213,510 shares of Series A preferred stock in March 2019, in connection with the conversion of the Simple Agreement for Future Equity (SAFE) agreements. See Note 7. In connection with the sale and issuance of the Series A preferred stock in March 2019, the Company issued warrants to purchase an aggregate of 96,499 shares of Series A preferred stock at an initial exercise price of $3.13 per share.
In July 2019, the Company sold 341,761 shares of Series A preferred stock for aggregate proceeds of approximately $1,070,000. In connection with the issuance of the Series A preferred stock, the Company issued warrants to purchase an aggregate of 41,015 shares of Series A preferred stock at an initial exercise price of $3.13 per share.
Each share of Series A Preferred Stock was convertible into one share of Common Stock, subject to adjustments for anti-dilution. In addition, the terms of the Series A Preferred Stock provided that it would automatically convert into Common Stock upon the closing of an initial public offering meeting certain specified conditions, and also that it would convert into Common Stock in the event holders of at least 75% of the Series A Preferred Stock approved a mandatory conversion.
The holders of the Series A Preferred Stock, exclusively and as a separate class, had the right to elect two directors of the Company, and two directors of the Company were elected by the holders of Series A Preferred Stock in accordance with such provision. The Series A Preferred Stock also had the right to vote together with holders of Common Stock on any matter presented to the shareholders of the Company for their action or consideration. In addition, the separate approval of a majority of the Series A Preferred Stock was required in connection with specified Company activities and transactions, including a merger or consolidation of the Company, and the liquidation, dissolution or winding-up the business and affairs of the Company.
F-15
In the event of a voluntary or involuntary liquidation, dissolution or winding up of the Company or a deemed liquidation event, the terms of the Series A Preferred Stock provided that holders of Series A Preferred Stock would be entitled to be paid, out of the assets of the Company available for distribution, an amount equal to $3.13 per share, plus any dividends declared but unpaid thereon, before any payment was made to the holders of Common Stock. The liquidation preference of the Series A Preferred Stock was approximately $7,639,000 at December 31, 2019. The terms of the Series A Preferred Stock provided that, if upon any liquidation, dissolution or winding up of the Company or deemed liquidation event, the assets of the Company available for distribution to its shareholders should be insufficient to pay holders of Series A Preferred Stock the full amount to which they would otherwise be entitled, the holders of Series A Preferred Stock would share ratably in any distribution of the assets available for distribution in proportion to the respective amounts which would otherwise be payable in respect of the shares held by them upon such distribution if all amounts payable on or with respect to such shares were paid in full.
Effective January 15, 2020, as a result of the Company’s reincorporation in the state of Delaware, the par value of the Company’s preferred stock was changed from $0.01 to $0.0001 per share, and all data on preferred stock was retroactively adjusted to be shown herein as reflective of this change.
Common Stock
On June 15, 2020, the Company received net proceeds of $23,419,721 in its IPO, after deducting underwriting discounts and commissions of $1,968,750 and other offering expenses of $861,529 borne by the Company. The Company issued and sold 1,750,000 shares of common stock in its IPO at a price of $15.00 per share. In connection with the IPO, all shares of the Company’s Series A Preferred Stock were converted into 2,438,851 shares of common stock, after giving effect to the 1.74 for 1 forward stock split of the common stock and net of the fractional shares adjustments that occurred in connection with the IPO.
The Company made payments of approximately $261 in the aggregate in connection with fractional shares resulting from the stock split and the conversion of the preferred stock that took place in connection with the IPO.
During the year ended December 31, 2020, the Company issued 50,460 shares of common stock, relating to the exercise of stock options. The shares were issued at a purchase price of $1.03 for total proceeds of $52,000.
During the year ended December 31, 2020, the Company issued 3,350 shares of common stock related to a cashless exercise of a warrant to purchase 4,022 shares.
As of December 31, 2020, the Company had 25,000,000 authorized shares of Common Stock, of which 6,220,927 shares were issued and outstanding. As of December 31, 2019, the Company had 12,180,000 authorized shares of Common Stock, of which 1,978,269 shares were issued and outstanding.
Options
On August 29, 2018, the Board of Directors of the Company adopted the Lantern Pharma Inc. 2018 Equity Incentive Plan, which was subsequently amended on December 17, 2018 and February 26, 2020. The Lantern Pharma Inc. 2018 Equity Incentive Plan, as amended and restated, is referred to herein as the “Plan”. The Company reserved 1,489,680 shares of its common stock for issuance under the Plan. The Plan is designed to provide additional incentives to employees, directors and consultants to remain in the service of the Company as well as to encourage stock acquisition by members of these targeted groups, which in the opinion of the management will support the alignment of the interests of the members of these groups and stockholders. Options granted under the Plan are generally exercisable for up to 10 years from grant date. 535,099 shares remain available for future awards under the Plan at December 31, 2020, following the grant of options and the award of restricted stock grants through December 31, 2020. The Company recorded stock-based compensation of approximately $1,192,000 and $118,000 related to stock options during the years ended December 31, 2020 and 2019, respectively. Total remaining unrecognized compensation expense for non-vested options is $2,480,912 as of December 31, 2020, and is expected to be recognized over a weighted average period of 1.3 years. The weighted average remaining contractual term of outstanding options at December 31, 2020 is 8.5 years.
F-16
A summary of stock option activity under the Plan during the years ended December 31, 2020 and 2019 is presented below:
| Options Outstanding | Options Exercisable | |||||||||||||||||
| Number
of Shares | Weighted-Average Exercise Price | Number
of Options | Weighted-Average Exercise Price | |||||||||||||||
| Outstanding December 31, 2018 | 629,060 | $ | 1.03 | 194,479 | $ | 1.03 | ||||||||||||
| Granted | 1,342 | $ | 1.03 | - | - | |||||||||||||
| Exercised | - | - | - | - | ||||||||||||||
| Cancelled or expired | (22,911 | ) | $ | 1.03 | - | - | ||||||||||||
| Outstanding December 31, 2019 | 607,491 | $ | 1.03 | 393,413 | $ | 1.03 | ||||||||||||
| Granted | 321,743 | $ | 15.01 | - | - | |||||||||||||
| Exercised | (50,460 | ) | $ | 1.03 | - | - | ||||||||||||
| Cancelled or expired | (43,166 | ) | $ | 1.03 | - | - | ||||||||||||
| Outstanding December 31, 2020 | 835,608 | $ | 6.41 | 610,633 | $ | 3.24 | ||||||||||||
For 2020 and 2019, the fair value of each option granted was estimated using the Black-Scholes option-pricing model, using the following weighted average assumptions:
| 2020 | 2019 | |||||||
| Term (in years) | 7.00 | 5.94 | ||||||
| Risk Free Rate | 0.54% - 0.67 | % | 2.79 | % | ||||
| Volatility | 83.2% - 84.37% | 60.1 | % | |||||
| Dividend Yield | 0.0 | % | 0.0 | % | ||||
| Grant Date Fair Value | $ | 11.01 – 11.28 | $ | 0.59 | ||||
The fair value of options is recognized as an expense over the vesting period and forfeitures are accounted for as they occur.
The total intrinsic value of options outstanding at December 31, 2020 was $10,726,878, and the total intrinsic value of options exercisable at December 31, 2020 was $9,773,797. The total intrinsic value of options exercised during the year ended December 31, 2020 was $20,590. The intrinsic value of options outstanding at December 31, 2019 was $0. No options were exercised during the year ended December 31, 2019.
| Expected Term - | The Company used a weighted average of time to vesting and maturity date. |
| Expected Volatility- | Due to the Company’s limited operating history and a lack of company-specific historical and implied volatility data, the Company has based its estimate of expected volatility on the historical volatility of a group of similar companies that are publicly traded commensurate with expected term as of grant date. The historical volatility data was computed using the daily closing prices for the selected comparable companies’ shares. |
| Risk-Free Interest Rate- | The Company used the U.S. treasury bill rate commensurate with the expected term as of grant date. |
| Expected Dividend- | As the Company has not issued any dividends and does not expect to issue dividends over the life of the options, the Company has estimated the dividend yield to be zero. |
Warrants
The Company had warrants to purchase 325,618 shares of common stock outstanding and exercisable as of December 31, 2020 at a weighted average exercise price of $6.49 per share. The Company had warrants to purchase 262,003 shares of Series A Preferred Stock outstanding and exercisable as of December 31, 2019 at a weighted average exercise price of $3.13 per share.
F-17
In connection with the Series A Preferred Stock financing transactions discussed above, in 2019 the Company issued warrants to purchase an aggregate of 137,513 shares of Series A Preferred Stock.
In connection with the IPO and the conversion of the Series A Preferred Stock into common stock, all outstanding warrants to purchase Series A Preferred Stock converted into warrants to purchase common stock.
In connection with the IPO, the Company granted the underwriters warrants (the “Underwriters’ Warrants”) to purchase an aggregate of 70,000 shares of common stock at an exercise price of $18.75 per share, which is 125% of the initial public offering price. The Underwriters’ Warrants have a five-year term and were not exercisable prior to December 7, 2020. All of the Underwriters’ Warrants were outstanding at December 31, 2020.
In 2020, the Company issued 3,350 shares of common stock related to a cashless exercise of a warrant to purchase 4,022 shares.
In 2019, warrants to purchase an aggregate of 39,651 shares of Series A Preferred Stock were modified to become warrants to purchase an aggregate of 27,754 shares of Series A Preferred Stock. As part of the modification, the term of these warrants was extended from .02 to 1.02 years. The fair value of the modified warrants was approximately $21,000 and is recorded in additional paid in capital.
In 2020, a warrant to purchase an aggregate of 23,734 shares of Common Stock was modified to become a warrant to purchase an aggregate of 21,360 shares of Common Stock. As part of the modification, the term of the warrant was extended from .003 to 1.003 years. The fair value of the modified warrant was approximately $36,000 and is recorded in additional paid in capital.
Note 7. SAFE Agreements
In December 2018, the Company entered into Simple Agreement for Future Equity (SAFE) agreements (the “SAFE Financing”) with five investors pursuant to which the Company received funding of $535,000 in exchange for agreement to issue the investors shares of preferred stock upon occurrence of a subsequent financing of preferred stock.
The number of shares to be received by the SAFE agreement investors was based on 80% of the pricing in the triggering equity financing. In a liquidity or dissolution event, the investors’ right to receive cash out was junior to payment of outstanding indebtedness and creditor claims, on par for other SAFEs and preferred stock, and senior to common stock. The SAFE agreements had no interest rate or maturity date, and the SAFE investors had no voting right prior to conversion.
As of December 31, 2018, the Company had received $535,000 of proceeds related to the SAFE agreements. The SAFE agreements had not yet converted as a qualifying financing had not yet occurred as of December 31, 2018. Pursuant to the guidance under ASC 480, the Company determined that the Purchase Amount (a term defined in the SAFE agreements denoting the amount in exchange for which an investor received the rights to receive the shares) should be recorded as a liability on the Company’s balance sheet. Due to a short period where the Company expected these to be converted, the Company recorded the entire amount of $535,000 as a short-term liability. The SAFE agreements were converted to equity in March 2019 and the Company issued 213,510 shares of Series A Preferred Stock in full satisfaction of these agreements.
Note 8. Notes and Loan Payable
In January 2020, the Company entered into a financing arrangement for commercial insurance with First Insurance Funding. The total amount financed was approximately $66,000 with an annual interest rate of 6.64%, to be paid over a period of ten months. In June 2020, the insurance policy was canceled, and the remaining loan balance was repaid. As of December 31, 2020, there is no remaining loan balance on the Company’s consolidated balance sheet related to the First Insurance financing arrangement.
F-18
On May 1, 2020 (the “Origination Date”), the Company received $108,500 in aggregate loan proceeds (the “PPP Loan”) from JPMorgan Chase Bank (the “Lender”) pursuant to the Paycheck Protection Program under the Coronavirus Aid, Relief, and Economic Security (CARES) Act. The PPP Loan is evidenced by a loan application and payment agreement (the “PPP Loan Agreement”) by and between the Company and the Lender. Subject to the terms of the PPP Loan Agreement, the PPP Loan bears interest at a fixed rate of one percent (1.0%) per annum. Payments of principal and interest are deferred for the first six months following the Origination Date, and the PPP Loan will mature two years after the Origination Date. The guidance under the Paycheck Protection Program was later updated so that deferral of payments of principal and interest were extended to ten months after completion of the covered period of 24 weeks and maturity was extended past two years. The Company is continuing to monitor further development and guidance related to the Paycheck Protection Program terms.
Following the deferral period, unless the loan is forgiven, the Company will be required to make payments of principal plus interest accrued under the PPP Loan to the Lender in monthly installments based upon an amortization schedule to be determined by the Lender based on the principal balance of the PPP Loan outstanding following the deferral period and taking into consideration any portion of the PPP Loan that may be forgiven prior to that time. The PPP Loan is unsecured and guaranteed by the U.S. Small Business Administration. The Company plans to file for forgiveness under this loan within the first half of 2021.
During the twelve months ended December 31, 2020, the Company received approximately $103,000 in funding resulting from a loan that was funded incorrectly. All of the funds from the loan were repaid by the Company in July 2020, and no loan funds were expended prior to the repayment. There are no amounts outstanding under this loan as of December 31, 2020.
Note 9. Related Party Transactions
The Company has obtained preclinical services from Biological Mimetics, Inc., which is also a stockholder in the Company. No expenses related to Biological Mimetics, Inc. were recorded during the year ended December 31, 2020 and nothing was owed to Biological Mimetics, Inc. at December 31, 2020. The Company recorded expenses of approximately $23,000 related to Biological Mimetics, Inc. during the year ended December 31, 2019, all of which is included in research and development. Approximately $2,000 was owed to Biological Mimetics, Inc. at December 31, 2019.
The Company has previously engaged Intuition Systems (“Intuition”) to provide services relating to development of the Company’s technology infrastructure and artificial intelligence platform, cloud computing, and computational biology. The chief executive officer of Intuition is the brother of Arun Asaithambi, the Company’s former Chief Executive Officer, President and Director. Nothing was expensed related to Intuition during the years ended December 31, 2020 and 2019. At December 31, 2020 and 2019, approximately $9,000 remained unpaid relating to Intuition and is included in accounts payable and accrued expenses in the accompanying consolidated balance sheet.
In January 2018, the Company entered into an Assignment Agreement (the “Assignment Agreement”) with BioNumerik Pharmaceuticals, Inc. (“BioNumerik”), pursuant to which the Company acquired rights to domestic and international patents, trademarks and related technology and data relating to LP-300 for human therapeutic treatment indications. Mr. Margrave, the Company’s Chief Financial Officer and Secretary, formerly served as the President, Chief Administrative Officer, General Counsel and Secretary of BioNumerik and has a minority ownership interest in BioNumerik. Nothing was expensed related to BioNumerik during the year ended December 31, 2020. The Company expensed less than $1,000 related to BioNumerik during the year ended December 31, 2019, which amount is included in general and administrative expenses in the accompanying consolidated statement of operations. No amounts are owed to BioNumerik as of December 31, 2020. Approximately $11,000 was owed and recorded in accounts payable to BioNumerik as of December 31, 2019.
Note 10. Loss Per Share of Common Shares
Basic loss per share is derived by dividing net loss applicable to common stockholders by the weighted average number of shares of common stock outstanding during each period. Diluted loss per share includes the effect, if any, from the potential exercise or conversion of securities, such as warrants, and stock options, which would result in the issuance of incremental shares of common stock unless such effect is anti-dilutive. In calculating the basic and diluted net loss per share applicable to common stockholders, the weighted average number of shares remained the same for both calculations due to the fact that when a net loss exists, dilutive shares are not included in the calculation. Potentially dilutive securities outstanding that have been excluded from diluted loss per share due to being anti-dilutive include the following:
| For the year ended December 31, | ||||||||
| 2020 | 2019 | |||||||
| Warrants | 325,618 | 262,003 | ||||||
| Stock options | 835,608 | 607,491 | ||||||
| Series A preferred stock | - | 2,438,866 | ||||||
| 1,161,226 | 3,308,360 | |||||||
F-19
Note 11. Income Taxes
Our effective tax rate differs from the statutory federal tax rate as presented in the following table:
| 2020 | 2019 | |||||||
| U.S. federal statutory tax rate | 21 | % | 21 | % | ||||
| Permanent differences | 1 | % | (1 | )% | ||||
| Valuation allowance | (22 | )% | (20 | )% | ||||
| Total: | - | % | - | % | ||||
As of December 31, 2020 and 2019, the Company was domiciled in Texas, and due to the losses generated and no revenues, it incurred no federal or state tax.
The tax effect of the temporary differences that give rise to the significant portions of the deferred tax assets and liabilities is presented below.
| December 31, | ||||||||
| 2020 | 2019 | |||||||
| Deferred tax assets | ||||||||
| Depreciation | $ | - | $ | 502 | ||||
| Research and development credits | 180,889 | 93,102 | ||||||
| Stock-based compensation | 257,941 | 24,695 | ||||||
| Net operating loss carryforwards | 2,417,169 | 1,366,040 | ||||||
| Deferred tax asset | 2,855,999 | 1,484,340 | ||||||
| Less: valuation allowance | (2,849,762 | ) | (1,484,340 | ) | ||||
| Net deferred tax asset | 6,237 | - | ||||||
| Deferred tax liabilities | ||||||||
| Fixed assets | (6,237 | ) | - | |||||
| Net deferred tax assets | $ | - | $ | - | ||||
Due to a history of losses we have generated since inception, we believe it is more-likely-than-not that all of the deferred tax assets will not be realized as of December 31, 2020 and 2019. Therefore, we have recorded a full valuation allowance on our deferred tax assets. At December 31, 2020 and 2019, we have net operating loss (“NOL”) carryforwards for federal income tax purposes of approximately $11.5 million and $6.5 million, respectively. The NOL carryforwards generated prior to 2018 of approximately $3.1 million could expire over time beginning in 2035, if not used. The NOL carryforwards generated in 2018 to 2020 of $8.4 million do not expire and are carried forward indefinitely. We also have state NOLs of approximately $71,000 at December 31, 2020. The Company also has approximately $181,000 of research and development tax credit carryforwards for federal purposes. These credits begin expiring in 2034. Due to the change in ownership provisions of the Internal Revenue Code, the availability of the Company’s NOL carryforwards and research and development credit carryforwards may be subject to annual limitations under Section 382 of the Internal Revenue Code against taxable income in the future period, which could substantially limit the eventual utilization of such carryforwards.
Entities are also required to evaluate, measure, recognize and disclose any uncertain income tax provisions taken on their income tax returns. The Company has analyzed its tax positions and has concluded that as of December 31, 2020, there were no uncertain positions. In addition, interest and penalties, if any, as they relate to income taxes assessed, are included in the income tax provision, for which there were none. The Company’s U.S. federal operating losses have occurred since its inception and as such, tax years subject to potential tax examination could apply from that date because the utilization of net operating losses from prior years opens the relevant year to audit by the IRS and/or state taxing authorities.
Note 12. Subsequent Events
On January 20, 2021, the Company closed a public offering of 4,928,571 shares of its common stock at a public offering price of $14.00 per share, which amount included 642,856 shares sold upon full exercise of the underwriter’s over-allotment option. Total gross proceeds from the offering were $68,999,994, and net proceeds from the offering were approximately $64,200,000.
F-20
Item 9. Changes in and Disagreements with Accountants on Accounting and Financial Disclosure.
None.
Item 9A. Controls and Procedures.
Our management, with the participation of our Chief Executive Officer and Chief Financial Officer (our principal executive officer and principal financial officer, respectively), evaluated the effectiveness of our disclosure controls and procedures as of December 31, 2020. The term “disclosure controls and procedures,” as defined in Rules 13a-15(e) and 15d-15(e) under the Securities Exchange Act of 1934, as amended, or the Exchange Act, means controls and other procedures of a company that are designed to ensure that information required to be disclosed by a company in the reports that it files or submits under the Exchange Act is recorded, processed, summarized and reported, within the time periods specified in the SEC’s rules and forms. Disclosure controls and procedures include, without limitation, controls and procedures designed to ensure that information required to be disclosed by a company in the reports that it files or submits under the Exchange Act is accumulated and communicated to the company’s management, including its principal executive and principal financial officers, as appropriate to allow timely decisions regarding required disclosure. Management recognizes that any controls and procedures, no matter how well designed and operated, can provide only reasonable assurance of achieving their objectives and management necessarily applies its judgment in evaluating the cost-benefit relationship of possible controls and procedures.
The closing of our initial public offering occurred on June 15, 2020. Consequently, as a newly reporting company under the Exchange Act, we are not required to evaluate the effectiveness of our internal controls over financial reporting until the end of the fiscal year after we file our first annual report on Form 10-K, which will occur on December 31, 2021. However, in connection with the audit of our financial statements for the years ended December 31, 2019 and 2018, prior to our initial public offering, we observed material weaknesses in our internal controls over financial reporting during those periods because we did not have a formal process for period end financial closing and reporting, and also because we historically had insufficient resources to conduct an effective monitoring and oversight function independent from our operations.
During 2020, we have taking several measures to address these weaknesses, including implementation of additional internal control processes and procedures regarding the financial close and reporting process, the recruitment of a full time Chief Financial Officer, the allocation of additional personnel and resources to support our finance function, and the conduct of additional monitoring and evaluation processes. Following the implementation of these remedial actions, and based on the monitoring and evaluation we have conducted, our management has determined that, as of December 31, 2020, the previously identified material weaknesses have been remediated.
Based on the evaluation of our disclosure controls and procedures as of December 31, 2020, our Chief Executive Officer and Chief Financial Officer have concluded that, as of such date, our disclosure controls and procedures, as defined above, are effective.
This Annual Report on Form 10-K does not include a report of management’s assessment regarding internal control over financial reporting or an attestation report of the Company’s registered public accounting firm due to a transition period established by rules of the Securities and Exchange Commission for newly public companies. In accordance with such rules, the report of management’s assessment and the attestation report will be included as part of our Annual Report on Form 10-K for the year ending December 31, 2021.
None.
126
Item 10. Directors, Executive Officers and Corporate Governance.
The information required by this Item is incorporated herein by reference to the information that will be contained in our proxy statement related to our annual meeting of stockholders to be held in 2021 (the “2021 Annual Meeting of Stockholders”), which we intend to file with the SEC within 120 days of the year ended December 31, 2020.
Item 11. Executive Compensation.
The information required by this Item is incorporated herein by reference to the information that will be contained in our proxy statement related to the 2021 Annual Meeting of Stockholders, which we intend to file with the SEC within 120 days of the year ended December 31, 2020.
Item 12. Security Ownership of Certain Beneficial Owners and Management and Related Stockholder Matters.
The information required by this Item is incorporated herein by reference to the information that will be contained in our proxy statement related to the 2021 Annual Meeting of Stockholders, which we intend to file with the SEC within 120 days of the year ended December 31, 2020.
Item 13. Certain Relationships and Related Transactions, and Director Independence.
The information required by this Item is incorporated herein by reference to the information that will be contained in our proxy statement related to the 2021 Annual Meeting of Stockholders, which we intend to file with the SEC within 120 days of the year ended December 31, 2020.
Item 14. Principal Accountant Fees and Services.
The information required by this Item is incorporated herein by reference to the information that will be contained in our proxy statement related to the 2021 Annual Meeting of Stockholders, which we intend to file with the SEC within 120 days of the year ended December 31, 2020.
127
Item 15. Exhibit and Financial Statement Schedules.
(a) The following documents are filed as part of this report:
| (1) | Financial Statements |
| (2) | Financial Statement Schedules |
All financial statement schedules are omitted because the information called for is not required or is shown either in the consolidated financial statements or in the notes thereto.
| (3) | Exhibits |
The following exhibits are filed herewith or incorporated by reference herein:
128
| 101.INS* | XBRL Instance Document |
| 101.SCH* | XBRL Taxonomy Extension Schema |
| 101.CAL* | XBRL Taxonomy Extension Calculation Linkbase |
| 101.DEF* | XBRL Taxonomy Extension Definition Linkbase |
| 101.LAB* | XBRL Taxonomy Extension Label Linkbase |
| 101.PRE* | XBRL Taxonomy Extension Presentation Linkbase |
| (a) | Incorporated by reference from the Registration Statement on Form S-1 filed April 16, 2020. |
| (b) | Incorporated by reference from Current Report on Form 8-K filed June 17, 2020. |
| (c) | Incorporated by reference from the Registration Statement on Form S-1/A filed May 19, 2020. |
| (d) | Incorporated by reference from the Registration Statement on Form S-1/A filed May 12, 2020. |
| (e) | Incorporated by reference from Current Report on Form 8-K filed August 21, 2020. |
| (f) | Incorporated by reference from the Registration Statement on Form S-1/A filed June 8, 2020. |
| (g) | Incorporated by reference from Quarterly Report on Form 10-Q for the period ending September 30, 2020. |
| (h) | Incorporated by reference from the Registration Statement on Form S-1 filed January 8, 2021. |
| (i) | Incorporated by reference from Exhibit 1.1 of the Registration Statement on Form S-1/A filed May 19, 2020. |
| + | Indicates a management control or any compensatory plan, contract or arrangement. |
| # | Certain confidential portions of this Exhibit were omitted by means of marking such portions with an asterisk (the Mark) because the identified confidential portions (i) are not material and (ii) are of the type that the Registrant treats as private and confidential. |
| * | Filed herewith. |
| ** | Furnished with this report |
Not applicable.
129
SIGNATURES
Pursuant to the requirements of Section 13 or 15(d) of the Securities Exchange Act of 1934, the registrant has duly caused this report to be signed on its behalf by the undersigned, thereunto duly authorized.
| Lantern Pharma Inc., | ||
| A Delaware Corporation | ||
| Dated: March 10, 2021 | By: | /s/ Panna Sharma |
| Panna Sharma, Chief Executive Officer | ||
| Dated: March 10, 2021 | By: | /s/ David R. Margrave |
| David R. Margrave, Chief Financial Officer | ||
Pursuant to the requirements of the Securities Exchange Act of 1934, this report has been signed below by the following persons on behalf of the registrant and in the capacities and on the dates indicated.
| Name | Title | Date | ||
| /s/ Panna Sharma | President, Chief Executive Officer and Director | March 10, 2021 | ||
| Panna Sharma | (Principal Executive Officer) | |||
| /s/ David R. Margrave | Chief Financial Officer | March 10, 2021 | ||
| David R. Margrave | (Principal Financial and Principal Accounting Officer) | |||
| /s/ Donald J. Keyser | ||||
| Donald J. Keyser | Chairman of the Board | March 10, 2021 | ||
| /s/ Leslie W. Kreis, Jr. | ||||
| Leslie W. Kreis, Jr. | Director | March 10, 2021 | ||
| /s/ David S. Silberstein | ||||
| David S. Silberstein | Director | March 10, 2021 | ||
| /s/ Vijay Chandru | ||||
| Vijay Chandru | Director | March 10, 2021 | ||
| /s/ Franklyn Prendergast | ||||
| Franklyn Prendergast | Director | March 10, 2021 |
130